A pelvic pleomorphic hyalinizing angiectatic tumor: a rare case report
Meriem Braiki, Mohamed Azzaza, Moncef Mokni, Khaled Sakly, Dorra Daly, Fethi Derbe
Corresponding author: Meriem Braiki, Department of Surgery, Sidi Bouzid Regional Hospital, Sidi Bouzid, Tunisia 
Received: 03 Nov 2019 - Accepted: 15 Nov 2019 - Published: 18 Nov 2019
Domain: General surgery
Keywords: Pleomorphic, tumor, pelvis, hyalinizing, surgery, immunohistochesmistry
©Meriem Braiki et al. PAMJ Clinical Medicine (ISSN: 2707-2797). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Meriem Braiki et al. A pelvic pleomorphic hyalinizing angiectatic tumor: a rare case report. PAMJ Clinical Medicine. 2019;1:14. [doi: 10.11604/pamj-cm.2019.1.14.20876]
Available online at: https://www.clinical-medicine.panafrican-med-journal.com//content/article/1/14/full
A pelvic pleomorphic hyalinizing angiectatic tumor: a rare case report
Meriem Braiki1,&, Mohamed Azzaza2, Moncef Mokni3, Khaled Sakly3, Dorra Daly4, Fethi Derbe5
1Department of Surgery, Sidi Bouzid Regional Hospital, Sidi Bouzid, Tunisia, 2Department of Surgery, Sahloul University Hospital, Sousse, Tunisia, 3Department of Pathology, Farhat Hached Hospital, Sousse, Tunisia, 4Basic Center Health, Sidi Bouzid, Tunisia, 5Department of Surgery, Clinique Les Oliviers, Sousse, Tunisia
&Corresponding author
Meriem Braiki, Department of Surgery, Sidi Bouzid Regional Hospital, Sidi Bouzid, Tunisia
Pleomorphic hyalinizing angiectatic tumor (PHAT) is a particular rare entity corresponding to soft tissue neoplasm with low malignant potential. The exact etiopathology responsible for the tumor occurrence is not exactly identified. Knowledge of this condition is necessary to avoid misdiagnosis of the lesion and subsequently, to adopt the proper management. Here we report a case of PHAT originating from soft tissue in the pelvic retroperitoneum. According to the litterature, few articles deal with such pathology and such location. This work illustrates features of the tumor, its characteristics, and the adequate management with the histopathological findings.
Pleomorphic hyalinizing angiectatic tumors (PHATs) were first described in 1996 by Smith et al. [1], and are rare mesenchymal tumors of uncertain origin and low potiential of malignancy [2,3]. PHATs are characterized by the presence of amorphus materiel including various clusters of thin-walled characteristic angiectasic vessels that are infiltrated and surrounded by spindle-shaped, round and plump pleomorphic cells. These cells are frequently arranged in sheets or, less commonly in fascicles. The pleomorphic cellular component is constituted of large single and multinucleate cells with enlarged irregular nuclei and abundant cytoplasm. The mitotic activity is rarely found [1,2].
A 40-year-old woman was referred to the surgery department for evaluation of a pelvic mass. The lesion was incidentally discovered by her gynecologist on ultrasonographic imaging required for 4-month-history of pelvic reccurent pain. Her past medical and surgical history was unremarkable. The physical examination found slight pelvic palpatory tenderness. Laboratory tests were within normal limits. Radiological investigations including ultrasonography (US) and magnetic resonance imaging (MRI) of the pelvic cavity revealed a large irregular and lobulating heterogenous soft tissue lesion measuring 10*7*5 cm and located in the pelvic retroperitoneum (Figure 1). The mass had close contact with pelvic right ureter and right iliac vessels. The patient underwent a surgical complete excision of the lesion. Intraoperatively (Figure 2), the process was irregular with multiple vessels on its surface, the mass was adherent to adjacent tissues and vessels. The tumor was carefully dissected and then completely removed with no bleeding during operation. The specimen (Figure 3) was sent for an histopathological examination. Microscopically (Figure 4), numerous dilated thin-walled vessels with an evident hyalinization of the vessel walls were found. Pleomorphic neoplastic cells were distributed among dilated vessels. Cellularity was variable with hyper and hypo cellular areas and sparse mitotic activity was noted. Furthermore on Immunohistochemistry, the tumor shows a strong positivity for CD34, CD99, CD117 and vimentin. Whereas, S-100 protein, CD56, smooth muscle actin (SMA), Desmin, DOG-1, ALK-1 and actin were negative. Basing on these findings, the definitive diagnosis was consistant with pleomorphic hyalinizing angiectatic tumor (PHAT) of the soft parts. The post operative course was uneventful, the patient was discharged the 4th day post operatively. The follow-up period was of 6 months with no evidence of local recurrence on follow-up imaging.
Pleomorphic hyalinizing angiectatic tumor (PHAT) are defined as rare soft tissue tumors categorized under benign neoplasm with uncertain differentiation and uncertain origin [4,5]. The most common site of such tumors is the subcutaneous tissue and muscles, located mainly in low extremities, less commonly these tumors may have a deep location as the pelvis [6-8]. In the present case, the soft tissue in the pelvic retroperitoneum is affected. The clinical presentation is non specific with no significant manifestations. It could be incidentally discovered when the mass is relatively large with a local slow growing course [6]. According to the literature, there are few published reports related to the imaging features of PHATs. Typically, PHATs are shown as soft tissue lesions without calcifications (8 10). On MRI, PHATs appear hypointense isointense on T1 weighted sequences, heterogeneously isointense hyperintense on T2 weighted sequences, and show significant heterogenous enhancement following intravenous contrast administration [2]. Microscopally, PHATs have polymorphotic appearance with characterized thin-walled, ecstatic vessels lined with a layer of hyaline substance mostly composed of fibrin. These pleomorphic neoplastic cells are immersed in an amorphus materiel of proliferating spindle and inflammatory cells containing hyperchromatic, pleomorphic nuclei and inter-nuclear cytoplasmic inclusions. Furthermore, few mitotic activity is rarely found [9,10]. Immuno-histochemical stains are useful for better tumor characterization because this kind of neoplasm has several histologic similarities with other soft tissue tumors and could be easily misdiagnosed. Differential diagnosis include; solitary fibrous tumors, fibrous histiocytoma, cellular angiofibroma and schwannoma. Thus, PHATs are characteristically strongly positive for CD34 and vimentin but show negative staining for desmin and S-100 [9]. Complete surgical excision of the tumor with macroscopic healthy soft tissue margins avoid the local recurrence. However, metastases have not been recorded till date.
We report a rare case of PHAT with an unusual deep location, which is accidentally discovered. The diagnosis is established basing on microscopic and immunohistochemical analysis. The prognosis related to such tumors is relatively good except a low risk of local recurrence when the excision is not complete.
The authors declare no competing interests.
All the authors have read and agreed to the final manuscript.
Figure 1: radiological
findings on MRI of the pelvis showing a well defined lobulated
soft tissue mass (white arrow), measuring 10x7x5 cm and located
in the pelvic retroperitoneum.
The signal intensity was inhomogenous. The lesion has significant
heterogenous enhancement with fat saturation following intravenous
contrast administration
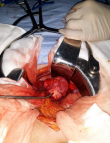
Figure 2: intraoperative photo demonstrating the tumor during dissection. The mass was carefully separated from adjacent tissues and vessels
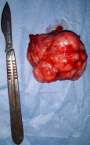
Figure 3: the specimen corresponding to a white-yellow lobulated mass
Figure 4: numerous ectatic thin-walled vessels with an evident hyalinization of the vessel walls. Pleomorphic neoplastic cells were distributed among dilated vessels and are immersed in an amorphus materiel of proliferating spindle and inflammatory cells. Cellularity was variable with hyper and hypo cellular areas
- Smith Mark E, Fisher Cyril, Weiss Sharon. Pleomorphic hyalinizing angiectatic tumor of soft parts: a low grade neoplasm resem�bling neurilemoma. Am J Surg Pathol. 1996;20(1):21-29. Google Scholar
- Couger Jimenez Jaramillo, John Wojcik, Kristy Weber, Ronnie Sebro. Imaging and histological appearance of pleomorphic hyalinizing angiectatic tumors: a case series and literature review.Oncol Lett. 2018; 15(4): 4720-4730. PubMed | Google Scholar
- Wei S, Pan Z, Siegal GP, Winokur TS, Carroll AJ, Jhala D. Complex analysis of a recurrent pleomorphic hyalinizing angiectatic tumor of soft parts. Hum Pathol. 2012;43(1):121-6. Google Scholar
- Chalmeti A, Arakeri SU, Javalgi AP, Goyal S. Pleomorphic hyalinizing angiectatic tumour; a rare case report and discussion of differential diagnosis. Journal of Clinical and Diagnostic Research. 2017;11(8):ED15-ED16. PubMed | Google Scholar
- Suzuki K, Yasuda T, Hori T, Oya T, Watanabe K, Kanamori M et al. Pleomorhic hyalinizing angiectatic tumour arising in thigh: a case report. Oncology Letters. 2014;7(4):1249-1252. PubMed | Google Scholar
- Zhi-gang Chu, Meng-qi Liu, Zhi-yu Zhu, Fa-jin Lv, Yu Ouyang. Pelvic retroperitoneal pleomorphic hyalinizing angiectatic tumor (PHAT) of soft tissue: a case report. BMC Medical Imaging. 2016;16:28. Google Scholar
- Ke Q, Erbolat, Zhang HY, Bu H, Li S, Shi DN et al. Clinicopathologic features of pleomorphic hyalinizing angiectatic tumor of soft parts. Chin Med J. 2007;120(10):876-81. PubMed | Google Scholar
- Subhawong TK, Subhawong AP, Montgomery EA, Fayad LM. Pleomorphic hyalinizing angiectatic tumor: imaging findings. Skeletal Radiol. 2012;41(12):1621-1626. PubMed | Google Scholar
- Chibueze Onyemkpa, Tolutope Oyasiji. Pleomorphic hyalinizing angiectatic tumor arising in the groin: a case report. International Journal of Surgery Case Reports. 2016;28: 227-230. Google Scholar
- Folpe AL, Weiss SW. Pleomorphic hyalinizing angiectatic tumor analysis of 41 cases supporting evolution from a distinctive precursor lesion. Am J Surg Pathol. 2004;28(11):1417-25. PubMed | Google Scholar
Search
This article authors
On Pubmed
On Google Scholar
Citation [Download]
Navigate this article
Similar articles in
Key words
Tables and figures
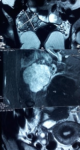 Figure 1: radiological findings on MRI of the pelvis showing a well defined lobulated soft tissue mass (white arrow), measuring 10x7x5 cm and located in the pelvic retroperitoneum. The signal intensity was inhomogenous. The lesion has significant heterogenous enhancement with fat saturation following intravenous contrast administration
Figure 1: radiological findings on MRI of the pelvis showing a well defined lobulated soft tissue mass (white arrow), measuring 10x7x5 cm and located in the pelvic retroperitoneum. The signal intensity was inhomogenous. The lesion has significant heterogenous enhancement with fat saturation following intravenous contrast administration
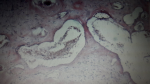 Figure 4: numerous ectatic thin-walled vessels with an evident hyalinization of the vessel walls. Pleomorphic neoplastic cells were distributed among dilated vessels and are immersed in an amorphus materiel of proliferating spindle and inflammatory cells. Cellularity was variable with hyper and hypo cellular areas
Figure 4: numerous ectatic thin-walled vessels with an evident hyalinization of the vessel walls. Pleomorphic neoplastic cells were distributed among dilated vessels and are immersed in an amorphus materiel of proliferating spindle and inflammatory cells. Cellularity was variable with hyper and hypo cellular areas