A case of male breast cancer relapsing with pleural effusion
Zakaria El Ouali, Najat Id El Haj, Souheil Boubia, Asmaa Elkebir, Mehdi Karkouri, Mohammed Ridai
Corresponding author: El Ouali Zakaria, Department of Thoracic Surgery, University Hospital of Ibn Rochd, Casablanca, Morocco 
Received: 25 Oct 2019 - Accepted: 28 Oct 2019 - Published: 30 Oct 2019
Domain: Oncology,Pulmonology,Thoracic surgery
Keywords: Breast Cancer, Male, Pleural effusion, Pleurodesis, Talc
©Zakaria El Ouali et al. PAMJ Clinical Medicine (ISSN: 2707-2797). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Zakaria El Ouali et al. A case of male breast cancer relapsing with pleural effusion. PAMJ Clinical Medicine. 2019;1:3. [doi: 10.11604/pamj-cm.2019.1.3.20808]
Available online at: https://www.clinical-medicine.panafrican-med-journal.com//content/article/1/3/full
A case of male breast cancer relapsing with pleural effusion
Zakaria El Ouali1,&, Najat Id El Haj1, Souheil Boubia1, Asmaa Elkebir2, Mehdi Karkouri2, Mohammed Ridai1
1Department of Thoracic Surgery, University Hospital of Ibn Rochd, Casablanca, Morocco, 2Department of Anatomical Pathology, University Hospital of Ibn Rochd, Casablanca, Morocco
&Corresponding author
Zakaria El Ouali, Department of Thoracic Surgery, University Hospital of Ibn Rochd, Casablanca, Morocco
Male breast cancer (MBC) is a rare entity, accounting only for 0.6% of all breast cancers. Its causes are incompletely understood. Pleural effusion is usually known as a metastasis of advanced breast cancer in women. However, it has never been described as a recurrence of MBC. We report the case of a 84 year-old man diagnosed with a breast cancer in 2014, initially treated with a mastectomy followed by chemotherapy, radiotherapy, and hormonotherapy regimen. He has been under remission for 4 years until he consulted for respiratory distress. Chest X-ray revealed a large right-sided pleural effusion. He was admitted for a pleural biopsy that concluded in tumor proliferation, leading to pleurodesis. Pathological examination confirmed the breast origin of his pleural effusion.
Male breast cancer (MBC) is an uncommon entity, accounting only for 0.6% of all breast cancers [1]. Its causes are incompletely characterized and understood [2]. Pleural effusion is usually known as a metastasis of women’s advanced breast cancer. However, it has never been reported as recurrence of MBC. We report the case of an 84-year-old man who presented a secondary pleural effusion to his breast cancer.
An 84-year-old man was diagnosed with a breast cancer in 2014, initially revealed by a nodule of the upper lateral quadrant, and a bloody nipple discharge. He never smoked and has no other toxic habits nor professional exposition, but type II diabetes mellitus. He had a mastectomy whose pathological examination showed an invasive ductal carcinoma moderately differentiated, grade I of Scarff-Bloom et Richardson, measuring 3,5 centimeters long, with nipple skin infiltration, and without embolus nor Paget's lesion. Resection margins were clean. A lymph node dissection was performed and showed a unique lymph node metastasis (1N+/14N) with no capsular effraction. The pTNM classification, following the AJCC TNM 7th edition due December 2009, was pT2N1aMx, R0. The study of hormonal receptors showed 100% positive cells to estrogen receptors (ER), and 30% positive cells to progesterone receptors (PR). 80% of the cells were overexpressing the HER2 oncogene, with a 3+ score. The Ki67 proliferation index showed a nuclear staining of 30% of the tumor cells. Work-up of extension consisted in a thoraco-abdominopelvic computed tomography (CT) and bone scintigraphy, that were both normal and the staging was IIB. He received a chemotherapy regimen made of 6 cycles of docetaxel, carboplatin, and trastuzumab (TCH), followed by 16 sessions of radiotherapy to the chest wall and sus-clavicular region. He was then taking tamoxifen (20 mg/day). After completing his chemotherapy and radiotherapy sessions, he performed a control thoraco-abdominopelvic CT scan that showed calcified mediastinal lymph nodes and peripheral ground-glass pulmonary contusion areas that were linked to his radiotherapy. Hence there was no evidence of disease.
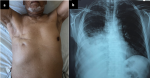
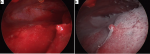
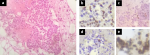
During his follow-up, he presented in November 2018 a symptomatology of exertional dyspnea and productive cough that were progressively increasing for 2 months. On physical examination, the temperature was 37°C, the body mass index was 25.1, and the mastectomy scar was clean (Figure 1a). Respiratory system examination revealed diminished breath sounds and decreased vocal resonance on the right side. Chest X-ray showed a right-sided pleural effusion (Figure 1b). Carcinoma Antigen 15-3 was 80.9 U/mL. CT scan showed an aspect of medium lobar condensation associated with non-septal thickenings related to radiotherapy, and right pleurisy of low abundance. A chest drainage was initially performed. The appearance of the pleural fluid was slightly cloudy, with a leucocyte count of 20/mm3 made of 10% of neutrophils and 90% of lymphocytes. The patient was then admitted in the operating room for a thoracoscopic pleural biopsy. During exploration, the pleura was very inflammatory and bloody to contact (Figure 2a). There were no lung nor pleural nodules. Frozen histological examination of the pleural biopsy concluded to a tumor proliferation and pleurodesis was performed using a talc to prevent any recurrence (Figure 2b). Pathology examination showed tumor cells arranged in clusters with chromatin nuclei sometimes dense and sometimes fine (Figure 3a). The immunohistochemical study confirmed the pleural origin of carcinomatous proliferation, hormonal-receptors-positive (Figure 3b, Figure 3c), a proliferative index of 15% (Figure 3d) and overexpressing HER2 (Figure 3e). Post-operative chest X-ray was normal. There were no post-operative complications. He was discharged 4 days after his intervention.
Breast cancer in men is a rare disease, accounting for 0.6% of all breast cancer cases and less than 1% of all malignancies in men [1]. Our patient was diagnosed with MBC at the age of 80, while occurrence of this disease peaks at the age of 71 [2]. The etiologies include hormonal, familial, genetic, and racial factors [2]. Presentation is usually a lump or nipple inversion [2]. The most common type of MBC is invasive ductal carcinoma (90%), like in our patient. Surgery is usually mastectomy with axillary clearance or sentinel node biopsy, followed by chemotherapy, radiotherapy and hormonotherapy depending on the stage [2]. Pleural effusion has been described as a presenting symptom of MBC, but has never been reported as a relapse of the disease [3]. Pleurodesis is the preferred palliative and supportive treatment option, targeting symptom relief. The timing for referral for pleurodesis is relevant: a prolonged time gap between a symptomatic pleurisy and pleurodesis was most strongly associated with the failure of pleurodesis due to the formation of adhesions in the pleural cavity, the thickening of the visceral pleura over time and hence the increased risk of trapped lung [4]. In our case, the time gap was about 1 month. Almost no adhesions were identified, and there was no trapped lung. Talc pleurodesis presents certain benefits over other pleurodesis agents: its main advantage is a shorter hospitalization, and biopsy specimens can be taken to determine more accurately the extent of disease spread [5], as it was done to our patient.
Although the epidemiologic, clinical, and therapeutic literature regarding female breast cancer is well documented, little is known about the features of MBC. The occurrence of a thoracic symptomatology mustn’t exclude a secondary pleurisy. Pleurodesis must be done as soon as possible after the confirmation for a better prognosis.
The authors declare no competing interest.
Zakaria El Ouali: conceptualization, data curation, investigation, writing original draft; Najat Id El Haj: data curation, supervision, validation, writing review & editing; Souheil Boubia, Mehdi Karkouri, Mohammed Ridai: supervision; Asmaa Elkebir: data curation. All the authors have read and agreed to the final manuscript.
Figure 1: (a) photography of the patient’s chest showing the mastectomy scar; (b) chest X-ray finding a large right-sided pleural effusion
Figure 2: (a) inflammatory and bleeding on contact pleural during exploration; (b) pleurodesis performance using talc
Figure 3: (a) frozen histological examination of the pleural biopsy with hematein and eosin stain; (b) immunohistochemical study with 70% of the cells expressing estrogen-receptors; (c) 5% progesterone-receptors; (d) Ki-67 of 15%; (e) HER2 score 3+
- Giordano SH, Cohen DS, Buzdar AU, Perkins G, Hortobagyi GN. Breast carcinoma in men: a population-based study. Cancer. 2004 Jul 1;101(1):51-7. PubMed | Google Scholar
- Fentiman IS, Fourquet A, Hortobagyi GN. Male breast cancer. Lancet. 2006 Feb 18;367(9510):595-604. PubMed | Google Scholar
- Karmakar S, Chaudhuri T, Nath A, Neyaz Z. Male breast cancer presenting with bilateral pleural effusion. North American Journal of Medical Sciences. 2013;5(1):72-4. PubMed | Google Scholar
- Leemans J, Dooms C, Ninane V, Yserbyt J. Success rate of medical thoracoscopy and talc pleurodesis in malignant pleurisy: a single-centre experience. Respirology. 2018;23(6):613-617. PubMed | Google Scholar
- Apffelstaedt JP, van Zyl JA, Muller AGS. Breast cancer complicated by pleural effusion: Patient characteristics and results of surgical management. Journal of Surgical Oncology. 1995;58(3):173-175. PubMed | Google Scholar