Meckel´s diverticulum located at the mesenteric edge of the ileum in an adult male: case report
Prince Kasongo Mwila, Baudouin Kongolo Kakudji, Ntabiseng Mosimanyane, Peter de Hill
Corresponding author: Prince Kasongo Mwila, Department of Surgery, Potchefstroom Hospital, Potchefstroom, South Africa 
Received: 20 Nov 2019 - Accepted: 25 Nov 2019 - Published: 30 Nov 2019
Domain: General surgery
Keywords: Ileum, mesentery, Meckel´s diverticulum
©Prince Kasongo Mwila et al. PAMJ Clinical Medicine (ISSN: 2707-2797). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Prince Kasongo Mwila et al. Meckel´s diverticulum located at the mesenteric edge of the ileum in an adult male: case report. PAMJ Clinical Medicine. 2019;1:36. [doi: 10.11604/pamj-cm.2019.1.36.21040]
Available online at: https://www.clinical-medicine.panafrican-med-journal.com//content/article/1/36/full
Case report 
Meckel´s diverticulum located at the mesenteric edge of the ileum in an adult male: case report
Meckel´s diverticulum located at the mesenteric edge of the ileum in an adult male: case report
Prince Kasongo Mwila1,&, Baudouin Kongolo Kakudji1,2, Ntabiseng Mosimanyane1, Peter de Hill1
1Department of Surgery, Potchefstroom Hospital, Potchefstroom, South Africa, 2School of Clinical Medicine, Faculty of Health Sciences, University of the Witwatersrand, Johannesburg, South Africa
&Corresponding author
Prince Kasongo Mwila, Department of Surgery, Potchefstroom Hospital, Potchefstroom, South Africa
Meckel’s diverticulum (MD) is the most common congenital malformation of the gastrointestinal tract and occurs in 2-3% of the population. It is a true intestinal diverticulum that results from failure of the vitelline duct to obliterate during the fifth week of fetal development. Very few cases of ileal mesenteric edge location have been reported in the literature. We report a case of a 33 year old male, who presented with clinical signs of localised peritonitis. At laparotomy we found a perforated appendix with localised peritonitis. An incidental finding of a MD was discovered at about 70cms from the ileocecal valve. Macroscopic examination revealed an out pouching growth of 32mm in length, 12mm in diameter with the distal end being slightly bulbous. A segmental resection of the MD with primary anastomosis was performed. The ileal mesenteric edge locations of MD have been reported by a few other authors. The fact that the condition is not reported in large series could contribute to its consideration as bowel duplication. Because there is a high risk of ileal mesenteric MD to erode the mesenteric vasculature and cause devastating consequences, we advocate for systematic resection of ileal mesenteric MD in absence of other contraindications. We believe the ileal mesenteric location is a variant of the classical antimesenteric location. Finding a MD on the ileal mesenteric edge is exceptionally rare.
Meckel's diverticulum (MD) is the most common congenital malformation of the gastrointestinal tract and occurs in 2-3% of the population, 60% of patients come to medical attention before the age of ten years with the remainder of cases presenting in adolescence and adulthood [1]. MD was first described in a paper published in 1809 by the German anatomist, Johann Friedrich Meckel, who described it as a remnant of the omphalo-mesenteric duct [2], although such an abnormality had been mentioned quite a lot earlier by Fabricius Hildamus in 1598 and in 1671 by Laveter who did not recognize its embryological origin [3]. Several characteristics facilitate the identification of MD including location within two feet (60 cms) of the ileocecal valve, the presence of an independent vessel supplying the structure, its antimesenteric location, five layers of small intestine, and ectopic mucosa of either gastric, pancreatic or of other origin [4]. Despite the fact that the antimesenteric location has been described as one of the cardinal findings in defining the MD, few cases of location at the mesenteric edge have been described in the literature [5-9]. We describe a case of an incidental finding of Meckel´s diverticulum located at ileal mesenteric edge during a laparotomy for localised peritonitis secondary to a perforated appendix.
A 33 years old male was transferred from a local clinic for an acute appendicitis. Symptoms started 3 days prior with epigastric pains. The following day the patient was nauseous, started vomiting and had worsening pain. He had no previous surgery, no chronic diseases, and no change of bowel habits or gastro intestinal bleed. He occasionally drinks alcohol and doesn´t smoke. His family history was unremarkable. On physical examination, he was febrile; temperature 38.2 degree celcius; BP 115/75 mmHg; heart rate 113 beats per minute; respiratory rate 24 cycles per minute, Sp02 93% on room air. The abdomen was not distended, there were no scars, no peristaltic waves or hernias. There was localised tenderness on the abdomen, mainly in the right fossa iliaca with rebound tenderness and guarding. On plain abdominal and chest radiographs, there was no free air under the diaphragm and no air fluid levels. Laboratory testing revealed a leukocytosis with a neutrophilia white cells count 18.2 per cubic millimeter, C-reactive protein 276 mg/l. A clinical diagnosis of perforated appendicitis with localised peritonitis was made. At explorative laparotomy we found a perforated grade IV appendicitis. At about 70 cms from the ileocecal valve we then incidentally found what we believed to be a MD despite its location on the ileal mesenteric edge (Figure 1, Figure 2, Figure 3). Segmental intestinal resection with primary end to end anastomosis was then performed, after the appendectomy. The abdomen was washed out with a copious amount of saline and closed. The post-operative period was characterized by a paralytic ileus on day one which completely resolved with conservative management on day 3. The patient was discharged on day 5 without any other complications being reported thus far.
Histology: Meckel´s Diverticulum: Macroscopic description: an unopened portion of small bowel with attached congested fatty tissue, 140mm in length. 70mm from one margin a diverticulum is present, 32mm in length, with a diameter of 12mm. The distal end is slightly bulbous. Height to diameter ratio (HDR) of 2.7
Microscopic examination: sections taken of the diverticulum show full thickness small bowel with normal intestinal mucosa, and in the lamina propria occasional lymphoid follicles. There is no evidence of inflammation, metaplasia or ulceration. There is mild fibrosis on the serosa surface and mesenterial fat. Sections taken of the rest of the terminal ileum also show mild fibrosis on the serosal surface.
Macroscopic description: an appendix vermiformis with a length of 50mm. A fibrino-purulent exudate is present on the serosa.
Microscopic examination: shows an acute inflammatory cell infiltrate consisting of neutrophilic leukocytes in the mucosa, muscularis propria and on the serosa. The histological appearance is that of an acute necrotizing appendicitis with peritonitis.
Ethical approval: this is a case report study which is not revealing any patient details and is file based. Still, we got the approval from the hospital patient's safety group.
The location of MD on the antimesenteric ileal edge has been accepted for a long time to be part of the diagnostic criteria [10]. However, some cases of location on the mesenteric ileal edge have been reported since 1941, and were suggestive of possible ileal duplication [11]. In their case-series, Donellan et al. described that the etiology of mesenteric location is due to congenital and inflammatory adhesions [12]. Another possibility considered by them was a meso-diverticular band (due to a persistent short vitelline artery), which might have diverted the diverticulum away from the anti-mesenteric border during rapid growth. In our case, and studies of other authors such as Mohanty PK et al; pathological examination revealed neither a meso-diverticular band nor a vitelline artery, and there were no features of inflammation [8]. This confirms that mesenteric location of MD is a distinct variant of MD and would just be a forgotten entity. For Segal et al and Akile et al this unfamiliar location could have been due to a short vitelline artery that disappeared without leaving a remnant or due to an intrauterine adhesion between the mesentery of the ileum and the omphalomesenteric canal [5,7]. Thus, during the process of elongation and growth, the “stuck” diverticulum might have been diverted from the antimesenteric border of the ileum. Other authors who reported cases of MD made it a differential of an intestinal duplication cyst [13]. In our case there was a communication with the lumen without any vitelline artery or heterotopic tissue. According to Ajaz et al. Charles Mayo stated "MD is frequently suspected, often looked for, and seldom found” [14]. This statement reveals how MD is a rare surgical condition. The diagnosis of a symptomatic MD in adults can be difficult. It requires a high index of suspicion, and despite the use of diverse diagnostic modalities such as endoscopy, angiography, contrast studies and scintigraphy, most adult patients are diagnosed intraoperatively [15]. If there is suspicion of a symptomatic MD laparoscopy is the investigation of choice. It is safe, cost effective and efficient for the diagnosis and definitive treatment of MD [16]. Surgical resection of symptomatic MD is the standard of care. There is ongoing controversy about the management of an asymptomatic MD. Surgical options include simple diverticulectomy, wedge excision or segmental resection by classical laparotomy or laparoscopy [17]. MD is a rare cause of mortality, and it is primarily a disease of young patients. In our case the Meckel´s diverticulum was found incidentally during an explorative laparotomy for a localised peritonitis secondary to a perforated appendix. Despite an ileus that developed on day one, and was treated conservatively, the postoperative period was uneventful. Robjin J et al and Park JJ et al have reported managing a MD based on a scoring system which predicts the risk for future complications of a non-resected MD [18,19]. This risk score is based on 4 risk factors: male sex, patients younger than 45 years, diverticulitis longer than 2cms and the presence of a fibrous band. They suggest resection of an asymptomatic MD with a risk score of six or more. For Sagar J et al, it is impossible intraoperatively to determine by inspection or palpation whether an incidentally found Meckel´s diverticulum is at increased risk of complications or not [3].
Meckel's diverticulum (MD) is the most common congenital malformation of the gastrointestinal tract. Even in major centres, individual surgeons are unlikely to encounter a MD on its antimesenteric location, finding a Meckel´s diverticulum on the ileal mesenteric edge is exceptionally rare. In the international literature we have encountered approximately ten case reports of a mesenteric Meckel´s diverticulum. We believe it´s a real variant of the classic antimesenteric location and should be systematically excised by segmental ileal resection because of its high risk of eroding into the mesentery and causing devastating consequences.
The author declare no competing interest.
All the authors have read and agreed to the final manuscript.
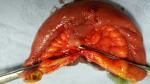
Figure 1: mesenteric edge location of Meckel´s diverticulum
Figure 2: segmental resection of the meckel´s diverticulum
Figure 3: intraoperative measurement of the Meckel´s diverticulum
Figure 4: superior view of the Meckel´s diverticulum
- Levy AD, Hobbs CM. Meckel´s diverticulum: Radiologic features with pathologic correlation. Radiographics. 2004;24:565-87. Google Scholar
- Meckel´s JF. Uber die divertikel am darmkanal. Arch physio. 1809;9:421-53. Google Scholar
- Sagar J. Meckel´s diverticulum: a systematic review. Jsoc med. 2006 Oct;99(10):501-5. PubMed | Google Scholar
- Walzak DA, Falek W, Zakszswski J. An uncommon location of Meckel´s diverticulum or small intestinal duplication? Case report and literature review. Polprzegl Chir. 2011;83(8):457-60. Google Scholar
- Akile Sarioglu-Buke, Cordu KN, Koltuksuz U, Karabul M, Savran B, Bagci S. An uncommon variant of Meckel´s diverticulum. Can J Surg. 2008 Apr;51(2):E46–E47. PubMed | Google Scholar
- Seitun S,Vito LD, Rossi UG, Panetta M, Cabiddu F, Tedechi U et al. Perforated Meckel´s diverticulum on the mesenteric side: Mdct findings. Abdom Imaging. 2012 Apr;37(2):288-91. PubMed | Google Scholar
- Segal SD, Albrecht DS, Belland KM, Elster EA. Rare mesenteric location of a forgotten entity: a case study aboard USS Kity Hawk. Am surg. 2004 Nov;70(11):985-8. PubMed | Google Scholar
- Mohanty PK, Panda SS, Das RR, Mallick S. Mesenteric location of Meckel´s diverticulum: Is it really uncommon. Saudi J Health sci. 2014; 3(3):166-167. Google Scholar
- Carpenter SG, McCullough AE, Pasha S, Harold KL. Mesenteric Meckel´s diverticulum: a real variant. IJAV. 2013;6:145-148. Google Scholar
- Blouhos K, Boulas KA, Tsali K, Barettas N, Paraskeva A, Kariotis I et al. A Meckel´s diverticulum in adults: surgical concerns. Front Surg. 2018;5:55. Google Scholar
- Wani I, Khan N, Nagash S, Choudri N, Wani K. Mesenteric Meckel´s diverticulum. Turk J gastroenterology. 2013;24(2):187-9. PubMed
- Donellan WL. Meckel´s Diverticulum and related anomalies. In Donellan WL, Burrington JD, Kimura K, Schafer JC, White JJ, Abdominal surgery of infancy and childhood. Luxemburg: Harwood Academic Publishers. 2001;12:1-4.
- Astrit RH, Besnik XB, Fisnik IK, Valon AZ, Fatas ES, Avdyl SK. Mesenteric Meckel´s diverticulum or intestinal duplication cyst: a case report with review of literature. Int J Surg case Rep. 2016;26:50-52. PubMed | Google Scholar
- Ajaz AM, Shams UB, Khurshid A, Abdul RK. Meckel´s Diverticulum revised. Saudi J. Gastroenterol 2010;16(1):3-7.
- Rivas H, Cacchione RN, Allen JW. Laparoscopic management of Meckel´s Diverticulum in adults. Surg Endosc 2003 Apr;17(4):620-2. PubMed | Google Scholar
- Shalaby RY, Soliman SM, Fawy M, Samaha A. Laparoscopic management of Meckel´s diverticulum in children. J Pediatric Surg. 2005;40(3):562-567. PubMed | Google Scholar
- Augusto Z, Simon E, Clare M, Agostino P. Incidentally detected Meckel´s Diverticulum to resect or not to resect. Annals of Surg. 2008;(2):276-281. Google Scholar
- Robijn J, Sebrechts E, Miserez M. Management of incidentally found Meckel´s Diverticulum: a new approach: resection based on a risk score. Acta Chir belg. 2006;106(4):467-470. PubMed | Google Scholar
- Park JJ, Wolff BG, Tollefson MK, Walsh EE, Larson DK. Meckel diverticulum the mayo clinic experience with 1476 patients(1950-2002). Ann Surg. 2005 Mar;241(3):529-33. PubMed | Google Scholar