Uncommon case report of an acephalic-acardiac twin and review of the literature
Abderrahim Siati, Maymouna El bouh, Aziz Slaoui, Sarah Talib, Imane Benmouna, Abdelaziz Baidada, Aicha Kharbach
Corresponding author: Abderrahim Siati, Department of Gynecology and Obstetrics, Maternity Souissi, University Hospital Center IBN SINA, University Mohammed V, Rabat, Morocco 
Received: 21 Oct 2019 - Accepted: 28 Oct 2019 - Published: 07 Nov 2019
Domain: Obstetrics and gynecology,Pediatrics (general),Reproductive Health
Keywords: Acardiac fetus, twin pregnancy, antenatal diagnosis
©Abderrahim Siati et al. PAMJ Clinical Medicine (ISSN: 2707-2797). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Abderrahim Siati et al. Uncommon case report of an acephalic-acardiac twin and review of the literature. PAMJ Clinical Medicine. 2019;1:6. [doi: 10.11604/pamj-cm.2019.1.6.20754]
Available online at: https://www.clinical-medicine.panafrican-med-journal.com//content/article/1/6/full
Uncommon case report of an acephalic-acardiac twin and review of the literature
Abderrahim Siati1,&, Maymouna El bouh1, Aziz Slaoui1, Sarah Talib1, Imane Benmouna1, Abdelaziz Baidada1, Aicha Kharbach1
1Department of Gynecology and Obstetrics, Maternity Souissi, University Hospital Center IBN SINA, University Mohammed V, Rabat, Morocco
&Corresponding author
Abderrahim Siati, Department of Gynecology and Obstetrics, Maternity Souissi, University Hospital Center IBN SINA, University Mohammed V, Rabat, Morocco
The TRAPS (Twin Reversed Arterial Perfusion Sequence) is an uncommon and specific complication of monozygotic genetic pregnancies. This anomaly is secondary to the presence of abnormal vascular connections between the twins, so it is a major form of the twin-to-twin transfusion syndrome. We present here a case of an acardiac-acephalic twin diagnosed during pregnancy at 27 weeks of amenorrhea. Thanks to advances in ultrasound, the antenatal diagnosis of the TRAP syndrome is made possible in the first trimester. This condition is associated with a high mortality rate in healthy twins caused by anemia and heart failure. Therapeutic resources involve in utero management such as the interruption of vascular anastomosis between the twins to perform a selective feticide.
In 1533, Benedetti for the first time describes an acardiac-acephalic twin. It is a rare condition, with an estimated frequency of 1/35 000 deliveries and about 1% of monozygotic twin pregnancies [1,2]. The TRAP sequence is an uncommon complication of monozygotic twin pregnancies. It is characterized by the existence of arteriovenous anastomoses between an acardiac fetus, recipient, and a healthy donor fetus. This syndrome is associated with a high mortality of healthy twin by anemia and heart failure.
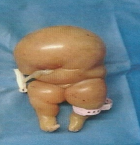
We hereby report the uncommon case of a 28-year-old woman with no medical history, gravida 3 para 2 having had 2 first vaginal deliveries without complication, current pregnancy not followed estimated at 6 months according to the patient, admitted to the emergency room for threat of premature delivery. The appearance the day before of close uterine contractions motivated her to consult in a rural health center that transferred her to us. The patient then immediately benefited an obstetrical ultrasound showing a monochoriale monoamniotic twin pregnancy, a "twin A" of normal morphology, biometry at 27 weeks of amenorrhea, with a "twin B" acephalic-acardiac. The umbilical cord of "twin A" had two arteries and a vein with normal doppler flow. In contrast, the umbilical cord of "twin B" had a single umbilical artery with Doppler flow reversal (Figure 1). During our surveillance, the "twin A" pump had presented a severe baradycardia. After consultation with the neonatal resuscitation team and preparation of its reception, a caesarean section is performed urgently. The patient gave birth to a daughter of 980g, pH 7.21, lactates 2.1mmol/L. The acephalic-acardiac twin weighing 1440g is extracted afterwards; it is composed of a trunk and two lower limbs (Figure 2). Althought efforts of neonatologists, the newborn were died at 4 hours of life. The placenta weighed 620g. The anatomo-pathological exam showing arterio-arterial anastomosis and the entire venous drainage was via the umbilical vein of the healthy twin.
The acephalic-acardiac fetus is a twin from a mono or biamniotic monochorial pregnancy, whose vascularization is ensured by a double set of anastomoses allowing the normal twin to infuse him countercurrent by an umbilical artery. The acardiac twin is no longer vascularized by the placenta but only by the other twin [3]. In the TRAP sequence which seems to be a particular form of the TTTT syndrome (Twin-To-Twin Transfusion Symdrome), the donor being the normal fetus, supplies the blood for himself and for the acardiac fetus regarded as the recipient. Venous return is performed by the umbilical vein of the normal twin. Coming from the donor, deoxygenated blood and low pressure who should normally return to the placenta, go straight into the acardiac twin. This is at the origin of the abnormalities of the cephalic pole, limbs and abdominals organs by interruption of organogenesis [4]. The diagnosis is most often made in the antenatal period by the systematic ultrasound which finds a twin pregnancy with severe malformations of one of the twins. The abnormalities observed to suggest the diagnosis are: absence of skull, holoprosencephaly, anencephaly, absence of facial mass and absence of thorax and heart. These abnormalities are not specific but if one is diagnosed it is important to look for other anomalies in this twin. One must then look for signs of heart failures in the healthy twin such as ascites, pleural effusion, hydramnios or cutaneous edema [5,6]. Doppler provides a predictive value of the evolution of the donor fetus as shown by Dashe et al. [7]. In fact, it is the difference in the resistance indices between the twins that seems to be best correlated with the outcome of the pregnancy: a resistance difference greater than 0.20 between the donor twin and the acardiac twin is associated with good results, whereas a difference of less than 0.05 is associated with the appearance of complications [7,8].
The prognosis of these pregnancies is fatal for the acardiac twin. The mortality of the donor twin is of the order of 50 to 75%, most often by cardiac failure, which is our case [8,9]. Treatment of TRAP syndrome ranges from obstetric abstentionism to interventionism, which depends on the prognosis for the healthy twin, dominated by the risk of preterm birth and heart failure [10]. Interventionist treatments aim to interrupt vascular communication between the two twins [7,8, 11]. Seeds et al. [12] proposed a selective feticide but the injection of a terminal substance could also affect the healthy twin. Laser endoscopic coagulation echographic-control of umbilical cord blood vessels from the acardiac twin is an alternative for complete cessation of reverse arterial perfusion and removal of tricuspid regurgitation from normal twin within 2 weeks without any complications [13,14]. A selective reduction of the acardiac twin by radiofrequency at the level of cord insertion in the acardiac twin can be achieved. A needle is inserted percutaneously until the origin of the cord and the energy is sent until the blood flow is stopped in the acardiac [15]. Lewi et al. [14] recently conducted a study of 80 pregnancies that had undergone coagulation treatment with the umbilical cord clamp of the acardiac twin. For Wong and Sepulveda [15], when the acardiac twin is small, a simple echographic surveillance is recommended, with the search for complications in the healthy twin. On the other hand, it is necessary to consider an invasive treatment, by coagulation or radiofrequency interruption of the abdominal aorta or pelvic vessels of the acardiac, when the latter is large or if it grows quickly.
Thanks to advances in ultrasound, the antenatal diagnosis of the TRAP syndrome is made possible in the first trimester. This early diagnosis determines in utero management of the healthy co-twin. However, the rarity of the fetus-like complications does not allow definitive conclusions to be drawn regarding the prognostic factors of the fetus pump. Only regular surveillance by ultrasound and Doppler allows a possible early therapeutic indication whose sole purpose is to save the healthy twin.
The authors declare no competing interests.
All the authors have read and agreed to the final manuscript.
Figure 1: (A) ultrasound
scan of "twin A" with normal morphology and Doppler exam without particularity;
(B) representing "twin B" acephalic-acardiac with a reversal Doppler flow
Figure 2: representing physical appearance of "twin B" acephalic-acardiac
- Monnier JC, Wattecamps J, Lanciaux B. Le f�tus acardiaque: diagnostic et surveillance �chographique (� propos d�un cas). J GynecolObstet Biol Reprod. 1982;11:599-605.
- Seket B, Bennour F, Blibech S. F�tus acardiaque: revue de la litt�rature � propos d�une observation. Tunis Med. 1998;76:8-9.
- Coulam CB, Wright G. First trimester diagnosis of acardiac twins. Early Pregnancy. 2000;4(4):261-70. PubMed | Google Scholar
- Torres Borrego J, Guzman Cabanas J, Arjona Berral JE, Acosta Collado A, Romanos Lezcano A. Acardiusacephalus. Description of a case. An Esp Pediatr 2000;53(4):346-9. PubMed | Google Scholar
- Guigue V, Schwetterle F, Arbez-Gindre F. Un cas de jumeau acardiaque ac�phale et revue de la litt�rature. Journal de Gyn�cologie Obst�trique et Biologie de La Reproduction. 2007;36(3):293-297. PubMed | Google Scholar
- Kayalvizhi I, Dhall U, Magu S. Acardiusacephalus monster: a case report. J Anat Soc India. 2005;54(1):26-8. Google Scholar
- Dashe JS, Fernandez CO, Twickler DM. Utility of Doppler velocimetry in predicting outcome in twin reversed-arterial perfusion sequence. Am J Obstet Gynecol. 2001;185(1):135-9. PubMed | Google Scholar
- Rajesh B, Mahadhevan B, Rao S, Bhat VB. Acephalus acardiac foetus. Indian J Pediatr. 2004;71(10):948. PubMed | Google Scholar
- Brassard M, Fouron JC, Leduc L. Prognostic markers in twin pregnancies with an acardiac fetus. ObstetGynecol. 1999 Sep;94(3):409-14. PubMed | Google Scholar
- Moore TR, Gale S, Benirschke K. Perinatal outcome of fortynine pregnancies complicated by acardiac twinning. Am J Obstet Gynecol. 1990 Sep;163(3):907-12. PubMed| Google Scholar
- Seeds JW, Herbert WN, Richards DS. Prenatal sonographic diagnosis and management of a twin pregnancy with placenta previa and hemicardia. Am J Perinatol. 1987 Oct;4(4):313-6. PubMed | Google Scholar
- Tsao K, Feldstein VA, Albanese CT, Sandberg PL, Lee H, Harrison MR et al. Selective reduction of acardiac twin by radiofrequency ablation. Am J Obstet Gynecol. 2002;187(3):635-40. PubMed | Google Scholar
- Lewi L, Gratacos E, Ortibus E, Van Schoubroeck D, Carreras E, Higueras T et al. Pregnancy and infant outcome of 80 consecutive cord coagulations in complicated monochorionic multiple pregnancies. Am J ObstetGynecol 2006; 194(3): 782-9. Google Scholar
- Deprest JA, Audibert F, Van Schoubroeck D, Hecher K, MahieuCaputo D. Bipolar coagulation of the umbilical cord in complicated monochorionic twin pregnancy. Am J Obstet Gynecol. 2000;182(2):340-5. PubMed | Google Scholar
- Wong AE, Sepulveda W. Acardiac anomaly: current issues in prenatal assessment and treatment. Prenat Diagn. 2005;25(9):796-806. PubMed | Google Scholar