Ectopic deciduosis with gigantic nodules: an uncommon case during pregnancy
Abderrahim Siati, Mohammed Boukhechba, Abdelaziz Baidada, Aicha Kharbach
Corresponding author: Abderrahim Siati, Department of Gynecology and Obstetrics, Maternity Souissi Hospital, University Hospital Center IBN SINA, University Mohammed V, Rabat, Morocco 
Received: 07 Oct 2019 - Accepted: 05 Nov 2019 - Published: 07 Nov 2019
Domain: Obstetrics and gynecology,Surgical oncology
Keywords: Ectopic deciduosis, gigantic nodules, pregnancy
©Abderrahim Siati et al. PAMJ Clinical Medicine (ISSN: 2707-2797). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Abderrahim Siati et al. Ectopic deciduosis with gigantic nodules: an uncommon case during pregnancy. PAMJ Clinical Medicine. 2019;1:7. [doi: 10.11604/pamj-cm.2019.1.7.20579]
Available online at: https://www.clinical-medicine.panafrican-med-journal.com//content/article/1/7/full
Ectopic deciduosis with gigantic nodules: an uncommon case during pregnancy
Abderrahim Siati1,&, Mohammed Boukhechba2, Abdelaziz Baidada1, Aicha Kharbach1
1Department of Gynecology and Obstetrics, Maternity Souissi Hospital, University Hospital Center Ibn Sina, University Mohammed V, Rabat, Morocco, 2Department of Pathology, Mohamed V Military Hospital, University Hospital Center Ibn Sina, University Mohammed V, Rabat, Morocco
&Corresponding author
Abderrahim Siati, Department of Gynecology and Obstetrics, Maternity Souissi
Hospital, University Hospital Center Ibn Sina, University Mohammed V, Rabat,
Morocco
Ectopic deciduosis is a common phenomenon during pregnancy, most often benign and corresponds to the presence of decidual tissue outside the endometrium. However, ectopic deciduous of the peritoneum and omentum remains a rare entity. In the literature, this is a physiological phenomenon that can complicate a mass syndrome or haemorrhage. We report here a case of ectopic peritoneal and omental deciduosis, discovered incidentally during caesarian section. This is a very rare case because we have found gigantic nodules and the largest measuring 75 mm in diameter. Pathological examination remains essential in order to differentiate it from peritoneal carcinomatosis or from an infectious disease such as tuberculosis. The prognosis is excellent. Surgical excisions of nodules with biopsies were performed. The patient was discharged from the hospital on the 5th postoperative day. Few months later, a laparoscopy was performed and showed the complete regression of the lesions.
Ectopic deciduosis was described for the first time once in 1887 by Walker et al. [1]. She was found in numerous sites such as the vagina, ovaries, fallopian tubes, peritoneum, omentum, lymph nodes and even the kidneys or lungs [2]. Ectopic decidualization is caused by pregnancy, although cases have been described even outside pregnancy, following a significant and abnormal impregnation of hormones of origin iatrogenic [3]. For some, this is a physiological phenomenon that can nevertheless complicate a mass syndrome or haemorrhage and whose great variability in clinical presentation makes diagnosis difficult.
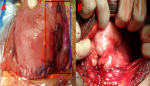
A 30-year-old Moroccan woman, G3P3 (2 alive children) with a previous caesarean section, was admitted in birth room at 38 weeks of amenorrhea. Her pregnancy was normal without any medical history. An emergency caesarean section was performed for suspicion of acute fetal distress. It allowed the extraction of a girl weighing 3520 g, which had an Apgar score of 07/10/10 at respectively 3/5/10 minutes of life. During cesarean section, the appearance of the uterus was unusual; its surface was dotted with small brownish and oval nodules (Figure 1). Haemostasis was difficult, due to spontaneous detachment of friable nodules on the uterine surface. In addition, the omentum appeared suspicious. It was edematous, with two gigantic oval nodules; the largest was measured 75mm in length (Figure 1). An identical appearance was found in the parietal peritoneum of the abdominal cavity with three oval formations of 4 to 40 mm compatible with peritoneal carcinomatosis. The exploration of the abdominal cavity did not find any hepatic or intestinal lesions. The left fallopian tube showed marked vascular turgidity and appeared to have also small nodules. A surgical excision of nodules with biopsies, and partial omentectomy were performed for diagnostic purposes. Pathological examination eliminated peritoneal carcinomatosis and confirmed an ectopic peritoneal and omental deciduosis. Histologically, these nodular formations were presented a decidual aspect with a mucoid content, sometimes alkaline, contained bulky eosinophilic cells, but which also lacked excessive mitotic activity, to the detriment of carcinomatosis diagnosis (Figure 2). In immunohistology, lesions were vimentin positive, progesterone receptors positive, smooth negative actin and PS 100 negative. The patient was discharged from the hospital on the 5th postoperative day. Four months later, a tubal sterilization by laparoscopy was performed at the request of the patient. Any abdominal or pelvic lesion was visible. The appearance of the peritoneum and the omentum was normal.
The process of decidualization is a physiological phenomenon resulting from the influence of steroid hormones secreted by the ovary and then the placenta. Its physiopathology remains poorly known. The ectopic deciduosis seems to locate preferentially on tissues derived from the coelomic epithelium. This is even less surprising when we know the common embryological origin, namely mesenchymal tissue via the coelomic epithelium, Muller's ducts and organs that are derived. The theory of caelomic metaplasia is evoked by authors. Decidual metaplasia occurs by independent and diffuse reaction of the peritoneum associated with the totipotency of subcoelomic mesenchyme cells by mechanical or hormonal factors [4]. There is indeed a sub-mesothelial zone, usually difficult to visualize under the microscope, which can give rise to different cell types such as fibroblasts, myofibroblasts and leiomyocytes [5]. Estrogens, when they are alone, induce nodular proliferation of fibroblasts and with progesterone they favor the differentiation of these fibroblasts into leiomyocytes and decidual cells [6]. The ectopic development of this phenomenon of decidualization, especially in a giant form poses the problem of differential diagnosis with carcinological lesions or tuberculosis [7]. Macroscopically, these lesions appear most often in the form of small white nodules whose localizations during pregnancy are most frequently the ovaries, the anterior and posterior surfaces of the uterus, the omentum, the cervical stroma, the cervical mucosa, but also the pelvic and lumbar ganglia-aortic and sometimes the appendix [8,9]. Masses of 60 mm could be described [10]. Morphologically, our case had the same characteristics as peritoneal carcinomatosis with a vegetating aspect of lesions.
Specifically, we had a gigantic white nodule measuring 75 mm in diameter. The ectopic decidosis is generally asymptomatic, and is usually discovered by chance during a caesarean section. It can induce complications during pregnancy or in the immediate postpartum. Hemorrhagic complications can be occured like massive hemoperitoneum in relation to erosion of this friable tissue by trauma related to pregnancy and delivery [11]. However, metrorrhagia, hematuria, hydronephrosis, occlusions on bridles, appendicular syndromes and even hemothorax have been described [5,12,13]. In our case, haemostasis was difficult on the uterine surface with multiple friable nodules. The pathological examination helped to correct the diagnosis. It was a regular epithelium with cells showing normal mitotic activity, different from the histological features of the cancer. Conventional pathology by identifying the presence of large submesothelial eosinophilic cells that corresponded to endometrial stromal cells was indeed effective in guiding the diagnosis to an ectopic deciduosis. An extemporaneous examination could have been discussed but was not done as part of the emergency. The interest of the immunohistology is to confirm the deciduous nature of the tissue process. Indeed, the antibodies directed against the vimentin were positive, demonstrating the existence of smooth muscle, always present during the decidualization of the endometrium. The immunohistological examination also showed the presence of progesterone receptors, a hormone necessary for the deciduous development of the endometrium, and usually absent in the omentum or peritoneum. Regarding other tissue markers, smooth actin and PS100 are classically absent in decidualized tissues. The prognosis of ectopic deciduosis is excellent. Generally, this tissue transformation is spontaneously resolving with a complete cure after the pregnancy [10]. Laparoscopy performed in our case a few months later, confirms this hypothesis.
Ectopic deciduousis is a benign lesion associated to pregnancy. The prognosis is excellent outside rare serious complications that it can induce. The accidental discovery during pregnancy of diffuse peritoneal lesions such nodules should lead to the systematic realization of staged biopsies for pathological examination. The immunohistological examination complements the standard analysis and helps to correct the diagnosis.
The authors declare no competing interests.
All the authors have read and agreed to the final manuscript.
Figure 1: (A) representing
uterus and left fallopian tube with small oval brownish nodules; (B) showing
two gigantic nodules, the largest measuring 75 mm
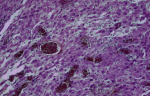
Figure 2: histological examination showing a decidual appearance, bulky eosinophilic cells lacked excessive mitotic activity with smooth muscle fibers in depth (HES)
- Piccinni DJ, Spitale LS, Cabalier LR, Dionisio de Cabalier ME. Decidua in the peritoneal surface mimicking metastatic nodules: findings during caesarean section. Rev Fac Cien Med Univ Nac Cordoba. 2002;59(1):113-6. PubMed | Google Scholar
- Castellv� Vives J, Garc�a Jim�nez A, Centeno Mediavilla C, Gil Moreno A, Hern�ndez de la Calle I, Gonz�lez-Bosquet J. Ectopic vaginal decidualization. An unusual finding that presents problems of differential diagnosis with carcinoma. Eur J Gynaecol Oncol. 1997;18(3):183-4. PubMed | Google Scholar
- Ober WB, Grady HG, Schoenbucher AK. Ectopic ovarian decidua without pregnancy. Am J Pathol. 1957 Mar-Apr;33(2):199-217. PubMed | Google Scholar
- Bassis ML. Pseudodeciduosis. Am J Obstet Gynecol. 1956;72(5):1029-37. PubMed | Google Scholar
- Buttner A, Bassler R, Theele C. Pregnancy-associated ectopic deciduas (deciduosis) of the greater omentum. An analysis of 60 biopsies with cases of fibrosing deciduosis and leiomyomatosis peritonealis disseminata. Pathol Res Pract. 1993;189(3):352-9. PubMed | Google Scholar
- Valente PT. Leiomyomatosis peritonealis disseminata. A report of two cases and review of the literature. Arch Pathol Lab Med. 1984;108(8):669-72. PubMed | Google Scholar
- Kondi-Pafiti A, Grapsa D, Kontogianni-Katsarou K, Papadias K, Kairi-Vassilatou E. Ectopic decidua mimicking metastatic lesions report of three cases and review of the literature. Eur J Gynaecol Oncol. 2005;26(4):459-61. PubMed | Google Scholar
- Wu DC, Hirschowitz S, Natarajan S. Ectopic decidua of pelvic lymph nodes: a potential diagnostic pitfall. Arch Pathol Lab Med. 2005;129(5):e117-20. PubMed | Google Scholar
- Lesaffer J, Feryn T, Proot L. Pregnancy-associated ectopic decidua of the appendix. Acta Chir Belg. 2009;109(1):93-4. PubMed | Google Scholar
- Malpica A, Deavers MT, Shahab I. Gross deciduosis peritonei obstructing labor: a case report and review of the literature. Int J Gynecol Pathol. 2002;21(3):273-5. PubMed | Google Scholar
- O�Leary SM. Ectopic decidualization causing massive postpartum intraperitoneal hemorrhage. Obstet Gynecol. 2006;108(3 Pt 2):776-9. PubMed | Google Scholar
- Suster S, Moran CA. Deciduosis of the appendix. Am J Gastroenterol. 1990 Jul;85(7):841-5. PubMed | Google Scholar
- Flieder DB, Moran CA, Travis WD, Koss MN, Mark EJ. Pleuro-pulmonary endometriosis and pulmonary ectopic deciduosis: a clinicopathologic and immunohistochemical study of 10 cases with emphasis on diagnostic pitfalls. Hum Pathol. 1998 Dec;29(12):1495-503. PubMed | Google Scholar