A malignant and idiopathic pyoderma gangrenosum : case report
Ibtissam Al Faker, Meriem El Bahloul, Farah Marraha, Soukayna Kabbou, Salim Gallouj
Corresponding author: Ibtissam Al Faker, Department of Dermatology, University Hospital Center Tangier, Tetouan Al Hoceima, Faculty of Medicine and Pharmacy Tangier Abdelmalek Essaadi University, Tangier, Morocco 
Received: 13 Aug 2021 - Accepted: 11 Dec 2022 - Published: 15 Dec 2022
Domain: Dermatology
Keywords: Ulcers, pyoderma gangrenosum, anterior nodular scleritis, corticosteroids, case report
©Ibtissam Al Faker et al. PAMJ Clinical Medicine (ISSN: 2707-2797). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Ibtissam Al Faker et al. A malignant and idiopathic pyoderma gangrenosum : case report. PAMJ Clinical Medicine. 2022;10:34. [doi: 10.11604/pamj-cm.2022.10.34.31229]
Available online at: https://www.clinical-medicine.panafrican-med-journal.com//content/article/10/34/full
A malignant and idiopathic pyoderma gangrenosum : case report
Ibtissam Al Faker1,&, Meriem El bahloul2, ![]() Farah Marraha1, Soukayna Kabbou1, Salim Gallouj1
Farah Marraha1, Soukayna Kabbou1, Salim Gallouj1
&Corresponding author
Malignant pyoderma gangrenosum (MPG) is a rare and aggressive form of pyoderma gangrenosum of unknown origin; the diagnosis is made after exclusion of other diseases. This case report describes a unique and particular case of MPG: generalized and aggressive form, nodular scleritis as a relapse and satisfactory outcome after treatment. A 55-year-old woman suffering for the last two weeks from painful and diffuse ulcerations, paraclinical investigations were normal, and the histological examination recalls a pyoderma gangrenosum. We encourage early aggressive treatment to expect well prognosis, especially since this form is malignant.
Malignant pyoderma gangrenosum (MPG) is a rare ulcerative variety of pyoderma gangrenosum (PG), first described by Perry et al. [1], it´s a rapidly evolving and severe skin disease on the head -and upper trunk, and not associated with systemic disease [2]. Its association with ophthalmic involvement, corneal and scleral, is also rare [3]. We report a case of MPG with a good evolution under treatment and a relapse once this last one is degreased.
Patient information: a 55-year-old Moroccan woman was admitted to our hospital ward, with very painful and rapidly evolved ulcers, the initial lesion was ulceration in the right leg of 10 cm, which quickly became widespread on the limbs and the back; she had no past medical history or similar episode in the past.
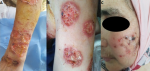
Clinical findings and timeline: the patient developed over the course of two weeks multiple ulcers of varying sizes involving her entire body (Figure 1), with erythematous fibrinous fundus, hypertrophic jagged borders and non-follicular pustules on the cheeks. She had no mucosal phanereal involvement; there was no palpable lymphadenopathy, and the rest of the somatic examination was normal.
Diagnostic assessment: a skin biopsy showed an important neutrophil inflammatory infiltrate (Figure 2). The contribution of histology here consists mainly of eliminating infections, other inflammatory diseases (thrombotic vasculitis) or tumor (carcinoma, lymphoma). A look for secondary causes was negative for malignancy and inflammatory bowel diseases (IBD). There were no signs of any inflammatory or rheumatologic conditions. We carried out a group of tests including hepatitis B, C and HIV serologies-, electrophoresis of serum proteins with protein immunofixation, rheumatoid factor, a liver test, a blood count with smear, a ferritinemia, a myelogram, C reactive protein, lactate dehydrogenase, 3 culture of Koch´s bacillus in sputum, chest x-ray, mammogram, abdominopelvic ultrasound, cervical smear and an esophagogastroduodenoscopy (EGD) endoscopy, and they were all normal except for inflammatory anemia and-gastritis due to Helicobacter pylori.
Diagnosis: the diagnosis of MPG has retained in front of the clinical aspect, the evolution, the generalized and facial involvement, the histology and exclusion of other aetiology of spread ulcerations.
Therapeutic intervention: methylprednisolone pulse therapy (15�mg/kg) has administered during three days with oral relay prednisolone (1.5�mg/kg/d) and topical corticosteroid (CS), after three weeks, the patient started Azathioprine (2.5 mg/kg/d) with CS reduction.
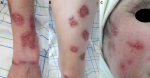
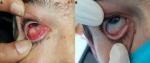
Follow-up and outcome of interventions: the ulcers have completely healed with cribriform scars (Figure 3) within two months, with a vertebral fracture as side effects of corticosteroid therapy. Ten months later, the patient presented red-eye with pain, ophtalmic examination revealed an anterior nodular scleritis (Figure 4 (A)) in her right eye; she has been treated successfully (Figure 4 (B) with corticosteroid eye drops and subconjunctival injection of corticosteroids once a day for three days.
Patient perspective: patient affirmed that the treatment protocol allowed obtaining acceptable results.
Informed consent: was obtained from the patient.
In 1968, Perry et al. were the first to use the term MP to describe a rare form of PG. Many authors have retained the adjective malignant to highlight the rapid evolution of ulcers involving large areas [4], our patient presented with painful and rapidly progressive ulcers all over her body with pustules and erosions on her face. The incidence of PG is estimated at 6 cases/million/year [5] with a median age of 59 years [6]. The majority of cases (75%) have underlying diseases such as inflammatory bowel disease, malignant hemopathies, rheumatoid arthritis, spondyloarthritis, systemic lupus erythematosus, vasculitis, Sjogren´s syndrome and neoplasia [7,8,9]; in our case, the patient had no associated disease. Erdi H et al. reported for the first time the generalized character in a 43-year-old woman, to our knowledge, our patient represents an original case of both idiopathic and generalized MP. The diagnosis is essentially based on histology, which shows a dense inflammatory infiltrate of the dermis that is very rich in neutrophils with intra-epidermal abscesses and an infiltration of the vascular wall.
Nodular scleritis in PG is very rare; it has been reported only four times [3,10,11,12]; and we assume that its occurrence may be a form of relapse of the disease, especially that it happened after reduction of corticosteroid therapy. Various therapeutic modalities have been tried in patients with MP, including systemic CS, methylprednisolone bolus, thalidomide, dapsone, clofazimine, azathioprine and cyclosporine [4,13,14]; the management of idiopathic PG is more problematic than the cases associated with systemic diseases, in our study, the bolus then oral relay, topical CS class I, optimized wound care and azathioprine resulted in complete healing. Given that it is a chronic disease, a long-term follow-up is essential and crucial to detect a paraneoplastic form.
The concomitant occurrence of a malignant and idiopathic form in our patient with a complication of nodular scleritis makes our case rare; to our knowledge, this association has never been described in the literature. Thus, it requires early, aggressive treatment in order to accelerate healing and prevent the onset of complications.
The authors declare no competing interests.
Patient management: Ibtissam Al Faker, Salim Gallouj and Meriem El bahloul. Data collection: Ibtissam Al Faker, Farah Marraha and Soukayna Kabbou. Manuscript drafting: Ibtissam Al Faker. Manuscript revision: Salim Gallouj . All the authors have read and agreed to the final manuscript.
Figure 1: (A,B,C) diffuse ulcers involving the body with an erosive lesion on the face
Figure 2: important neutrophil inflammatory infiltrate (A,B) with intra epidermal abscess (A,C)
Figure 3: ulcers have healed leaving hypertrophic and cribriform scars
Figure 4: anterior nodular scleritis on right eye (A), and treatment outcome (B)
- Perry HO, Winkelmann RK, Muller SA, Kierland RR. Malignant pyodermas. Archives of Dermatology. 1968;98(6):561-576. PubMed | Google Scholar
- Erdi H, Anadolu R, Piskin G, Gürgey E. Malignant pyoderma: a clinical variant of pyoderma gangrenosum. International Journal of Dermatology. 1996;35(11);811-813. PubMed | Google Scholar
- Maringe E, Gueudry J, Joly P, Muraine M. Nodular scleritis associated with pyoderma gangrenosum. Journal Francais d'Ophtalmologie. 2015;38(2):171-173. PubMed | Google Scholar
- Cardinali C, Giomi B, Caproni M, Fabbri P. Malignant pyoderma responding to cyclosporine. European Journal of Dermatology. 2001;11(6):595-6. PubMed | Google Scholar
- Weizman A, Huang B, Berel D, Targan SR, Dubinsky M, Fleshner P et al. Clinical, serologic, and genetic factors associated with pyoderma gangrenosum and erythema nodosum in inflammatory bowel disease patients. Inflammatory Bowel Diseases. 2014;20(3):525-533. PubMed | Google Scholar
- George C, Deroide F, Rustin M. Pyoderma gangrenosum-a guide to diagnosis and management. Clinical Medicine. 2019;19(3):224. PubMed | Google Scholar
- Cozzani E, Gasparini G, Parodi A. Pyoderma gangrenosum: a systematic review. G Ital Dermatol Venereol. 2014;149(5);587-600. PubMed | Google Scholar
- Klimusinaa J, Obersona M, Valentinoa MD. An unusual case of large vessel vasculitis associated with pyoderma gangrenosum. J Cardiovasc Med. 2011;14:185-188. Google Scholar
- Malek A, Saliba J, Choucair J, Irani C. Pyoderma gangrenosum as the first clinical manifestation of primary Sj�gren disease: a case report and review of literature. Clin Case Rep Rev. 2017;3(10.15761). Google Scholar
- Miserocchi E, Modorati G, Foster CS, Brancato R. Ocular and extracutaneous involvement in pyoderma gangrenosum. Ophthalmology. 2002;109(10):1941-1943. PubMed | Google Scholar
- Braun MM, Wong IG, Ta CN. Nodular scleritis in a patient with pyoderma gangrenosum. Archives of Ophthalmology. 2002;120(12):1763-1765. PubMed | Google Scholar
- Contreras-Verduzco FA, Espinosa-Padilla SE, Orozco-Covarrubias L, Alva-Chaire A, Rojas-Maruri CM, Sáez-de-Ocariz M. Pulmonary nodules and nodular scleritis in a teenager with superficial granulomatous pyoderma gangrenosum. Pediatric dermatology. 2018;35(1):e35-e38. PubMed | Google Scholar
- Mohanty J, Sharma A, Sharma MK. Malignant pyoderma. Indian Journal of Dermatology. 2002;47(04):251. Google Scholar
- Goihman-yaht M, Pari T, George S, Jacob M, Chandi SM, Pulimood S, Rajagopalan B. Malignant pyoderma responding to clofazimine. International Journal of Dermatology. 1996;35(10):757-758. PubMed | Google Scholar