Cardiac tamponade revealing systemic lupus in an elderly subject: a rare case report
Yassine Ettagmouti, Khawla Chawki, Khadija Essafi, Rachida Habbal
Corresponding author: Yassine Ettagmouti, Ibn Rochd Hospital University, Casablanca, Morocco 
Received: 27 Aug 2022 - Accepted: 01 Feb 2023 - Published: 02 Feb 2023
Domain: Cardiology
Keywords: Systemic lupus, elderly subject, cardiac tamponade, case report
©Yassine Ettagmouti et al. PAMJ Clinical Medicine (ISSN: 2707-2797). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Yassine Ettagmouti et al. Cardiac tamponade revealing systemic lupus in an elderly subject: a rare case report. PAMJ Clinical Medicine. 2023;11:30. [doi: 10.11604/pamj-cm.2023.11.30.37050]
Available online at: https://www.clinical-medicine.panafrican-med-journal.com//content/article/11/30/full
Cardiac tamponade revealing systemic lupus in an elderly subject: a rare case report
![]() Yassine Ettagmouti1,&, Khawla Chawki1, Khadija Essafi1, Rachida Habbal1
Yassine Ettagmouti1,&, Khawla Chawki1, Khadija Essafi1, Rachida Habbal1
&Corresponding author
Systemic lupus erythematous (SLE) is a chronic autoimmune disease with a polymorphic clinical presentation that occurs mainly in young women. The particularity of this case report is that pericardial tamponade as the first manifestation of SLE and its late discovery in an elderly subject are rare. Few similar cases are reported in the literature. We report the case of a 60-year-old woman admitted to the cardiology department for dyspnoea evolving for 15 days, with a sensation of chest pressure. On admission, the patient was haemodynamically unstable. Echocardiography showed abundant circumferential pericardial effusion with variations in respiratory flow. A pericardiocentesis was performed with a sample of 900 ml of blood fluid. We started a symptomatic treatment of the pericardial effusion and an etiological assessment was carried out. The diagnosis of SLE was made according to the Systemic Lupus International Collaborating Clinics (SLICC) criteria for SLE. In our case, emergency pericardial puncture showed hematic-like pericardial effusion. Using the lab results and other investigations, we were able to make a diagnosis of SLE. The diagnosis of lupus allowed a curative treatment of the etiology of the pericardial effusion, to avoid the recurrence as well as to improve the prognosis. This case is interesting because lupus is rarely the cause of a very abundant pericardial effusion, even less so in an elderly subject. Cardiac tamponade is a life-threatening condition. Therefore, pericardiocentesis should be performed as soon as possible to avoid death. It should be kept in mind that SLE can be complicated by pericardial tamponade and know how to look for it after hemodynamic stabilization of the patient.
Systemic lupus erythematosus (SLE) is a multisystem disease with a variety of presentations and clinical manifestations [1]. It is a connective tissue disorder that can include mucocutaneous, joint, renal, hematological, neurological but also cardiac involvement. Cardiac involvement usually consists of diffuse pericardial effusion or pericarditis, but can also cause pulmonary hypertension, myocarditis, thromboembolic manifestations, conduction disturbances, and valvulopathy [1,2]. Cardiac involvement as the initial presentation of SLE has been reported in only a few patients, but cardiac tamponade is rarely the first manifestation [3]. In this report, we describe the case of a 60-year-old woman in whom cardiac tamponade secondary to pericardial effusion was the initial manifestation of SLE. This case is reported for the rarity of cardiac tamponade as the first manifestation of SLE as well as for the advanced age of the discovery of this pathology.
Patient information: we report the case of a 60-year-old female with blood hypertension under amlodipine 5 mg/day, self-treated for 3 years for arthralgia of the wrists and right ankle by nonsteroidal anti-inflammatory drugs. Reporting no recent viral infection or tuberculosis contagion and no history of neoplasia. She had no abnormalities in the previous pregnancies. The patient was admitted in the cardiology department for shortness of breath evolving for 15 days, with an exacerbated pain on inspiration.
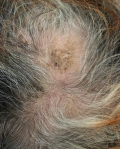
Clinical findings: the medical examination revealed a conscious patient with a blood pressure of 95/60 mmHg, respiratory rate of 27 breaths/min, oxygen saturation of 96%, heart rate of 105 bpm, apyretic. The cardiovascular and pulmonary examination showed a decreased heart sounds with no crackling rales and jugular distension. The scalp examination revealed a non-scarring alopecia (Figure 1), no skin stain, no palpable lymph nodes.
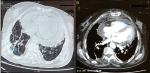
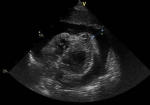
Diagnostic assessment: the EKG revealed a sinus tachycardia (Figure 2). Injected thoracic CT (Figure 3 A,B) showed a cardiomegaly related to pericardial effusion, left low abundance pleural effusion and interstitial lung disease. Echocardiography assessed a massive circumferential pericardial effusion (Figure 4) with respiratory variations of the mitral flow (45%) and tricuspid flow (60%), an IVC dilated to 26�mm non-complying.
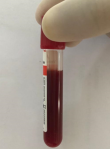
Therapeutic intervention: the initial emergency behavior was to admit the patient in our intensive care unit, half-seated position, saline infusion and pericardiocentesis withdrawal of 900 ml of hematic fluid (Figure 5). We have started symptomatic treatment of the pericardial effusion of colchicine 0.5 mg per day, aspirin 3g a day with a proton pump inhibitor. The laboratory work on the pericardial fluid showed an exudative liquid, predominantly of neutrophils, the culture was sterile and tuberculosis PCR was negative. Complete blood count showed a normochromic normocytic anemia (hemoglobin 10.1 gr/dl), white blood cell count of 6820/mm3 neutrophils 6450/mm3, lymphocytes 370/mm3, platelets 113 000/mm3, the C-Reactive Protein was elevated at 168 mg/dl, the erythrocyte sedimentation rate was 55�mm while the fibrinogen was 5.14, GFR 67ml/min with a negative 24h proteinuria. Tumor markers and coronavirus testing were negative, while direct combs test was positive. Concerning the immunologic testing: rheumatoid factor was increased, complement C3 fraction was low, antinuclear antibodies were high (1280) anti cardiolipin IgM/G and anti B2 glycoprotein IgG/M antibodies were positive. The diagnosis of SLE was established according to the Systemic Lupus International Collaborating Clinics (SLICC) SLE criteria.
Follow-up and outcomes: after the pericardiocentesis, we noted the resolution of dyspnea and normalization of hemodynamic and respiratory parameters, the echocardiographic control noticed a low abundance pericardial effusion facing the right cavities. The patient's condition improved following treatment with prednisone and hydroxychloroquine with a significant decrease of the pericardial effusion after 2 months.
Patient perspective: our patient was satisfied with the therapeutic management administered and declared no undesirable post-treatment effects.
Informed consent: all medical and paramedical acts as well as the details of its therapeutic management have been carried out with the written consent of the patient.
Systemic lupus erythematosus (SLE) is classified as a systemic autoimmune disease, in which deposits of immune complexes often lead to an inflammatory response that involves many internal organs of the body, with unpredictable flare and remission patterns. The cardiac manifestation of SLE includes pericarditis, myocarditis, pulmonary hypertension, valvular heart disease, and conduction system abnormalities. In 1949, Curtis and Horne described the first confirmed cases of lupus erythematosus with pericardial effusion as the main manifestation [4]. Sudden onset pericardial effusion has been noted less frequently, with an incidence of 8 to 18% [5]. However, cardiac tamponade is rarely the initial symptom of the disease. A large study of 1300 patients showed hemodynamic instability secondary to pericardial effusion compressing the heart chambers in less than 1% of patients [6]. It has been observed more in the female sex, in case of anemia, nephropathy, pleurisy, biological inflammation: higher ESR, C-reactive protein and fibrinogen values and lower complement levels [7,8].
Given the history of recurrent arthralgia of the wrists and right ankle of our patient self-treated with nonsteroidal anti-inflammatory drugs, the initial diagnostic theory included an autoimmune process. Autoimmune work revealed positive ANA and low C3 levels. Using the lab results and other investigations, we were able to make a diagnosis of SLE based on the 2015 revised criteria from the Systemic Lupus International Collaborative Clinics (SLICC) and the American College of Rheumatology (ACR) for LED diagnosis [9]. Our patient had a total of 7 criteria out of 17: non-scarring alopecia, pericarditis, low C3 level, immunological disorders, hematological disorder and a positive direct Coombs test. Typically, SLE-related pericardial effusions are predominantly citrine yellow, exudative, and usually reflect a neutrophil-dominated inflammatory response. They are of progressive installation and are only slightly complicated by arterial hypotension. Only a few hemorrhagic-looking effusions have been reported in the literature [9]. In our case, the pericardial puncture performed urgently, given the hemodynamic context, showed a pericardial effusion of a hematic nature that could wrongly point to neoplasia. Although the evolution after treatment is generally favorable, recurrences of effusion and chronic constrictive pericarditis have been reported in two patients in the series by Kahl et al [8].
Lessons to be learned from this case report are that: pericardial tamponade is a diagnostic and therapeutic emergency. Therefore, rapid evacuation of pericardial fluid must be performed. Systemic lupus erythematosus (SLE) can also affect elderly subjects with no history of lupus. Systemic lupus erythematosus (SLE) may be responsible for cardiac tamponade.
The authors declare no competing interests.
Yassine Ettagmouti: writing paper. Khawla Chawki: study concept literature. Khadija Essafi: care of the patient. Rachida Habbal Ettagmouti: Interpretation and analysis. All the authors have read and agreed to the final manuscript.
Figure 1: non-scarring alopecia of the scalp
Figure 2: sinus tachycardia
Figure 3: (A,B) cardiomegaly, pleural effusion and interstitial lung disease
Figure 4: circumferential pericardial effusion
Figure 5: hematic pericardial effusion fluid
- Updating the American College of Rheumatology revised criteria for the classification of systemic lupus erythematosus. Hochberg MC. Arthritis Rheum. 1997 Sep;40(9):1725. PubMed | Google Scholar
- Mandell BF. Cardiovascular involvement in systemic lupus erythematosus. Semin Arthritis Rheum. 1987 Nov;17(2):126-41. PubMed | Google Scholar
- López PD, Valvani R, Mushiyev S, Visco F, Pekler G. Cardiac tamponade: an unusual presentation of systemic lupus erythematosus. Am J Med. 2018 May;131(5):e189-e190. PubMed | Google Scholar
- Curtis AC, Horne SF. Disseminated lupus erythematosus with pericardial effusion. Ann Intern Med. 1949 Jan;30(1):209-17. PubMed | Google Scholar
- Shearn MA, Pirofsky B. Disseminated lupus erythematosus. Arch Int Med. 1952 Dec;90(6):790-807. PubMed | Google Scholar
- Cauduro SA, Moder KG, Tsang TS, Seward JB. Clinical and echocardiographic characteristics of hemodynamically significant pericardial effusions in patients with systemic lupus erythematosus. Am J Cardiol 2003;92:1370-2. PubMed | Google Scholar
- Rosenbaum E, Krebs E, Cohen M, Tiliakos A, Derk CT. The spectrum of clinical manifestations, outcome and treatment of pericardial tamponade in patients with systemic lupus erythematosus: a retrospective study and literature review. Lupus. 2009;18(7):608-612. PubMed | Google Scholar
- Kahl LE. The spectrum of pericardial tamponade in systemic lupus erythematosus: report of ten patients. Arthritis Rheum. 1992;35(11):1343-1349. PubMed | Google Scholar
- Salehi-Abari. ACR/SLICC revised criteria for diagnosis of systemic lupus erythematosus. Autoimmune Diseases and Therapeutic Approaches. 2015;2(1).