Prevalence and correlates of sleep-disordered breathing in patients with heart failure at a tertiary hospital in South-west Nigeria: a cross-sectional study
Folasade Adeola Daniel, Atinuke Kalada Richards, Phillip Alaba Adebola, Oyenike Rashidat Opaleye
Corresponding author: Folasade Adeola Daniel, Department of Medicine, Lagos State University College of Medicine, Ikeja, Nigeria 
Received: 16 Jul 2022 - Accepted: 09 Jun 2023 - Published: 22 Jun 2023
Domain: Cardiology
Keywords: Sleep, disordered breathing, heart failure, oxygen desaturation index, STOPBANG, overnight oximetry
©Folasade Adeola Daniel et al. PAMJ Clinical Medicine (ISSN: 2707-2797). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Folasade Adeola Daniel et al. Prevalence and correlates of sleep-disordered breathing in patients with heart failure at a tertiary hospital in South-west Nigeria: a cross-sectional study. PAMJ Clinical Medicine. 2023;12:19. [doi: 10.11604/pamj-cm.2023.12.19.36346]
Available online at: https://www.clinical-medicine.panafrican-med-journal.com//content/article/12/19/full
Research 
Prevalence and correlates of sleep-disordered breathing in patients with heart failure at a tertiary hospital in South-west Nigeria: a cross-sectional study
Prevalence and correlates of sleep-disordered breathing in patients with heart failure at a tertiary hospital in South-west Nigeria: a cross-sectional study
![]() Folasade Adeola Daniel1,2,&, Atinuke Kalada Richards3,
Folasade Adeola Daniel1,2,&, Atinuke Kalada Richards3, ![]() Phillip Alaba Adebola1,2, Oyenike Rashidat Opaleye2
Phillip Alaba Adebola1,2, Oyenike Rashidat Opaleye2
&Corresponding author
Introduction: sleep-disordered breathing is a phenomenon known to occur among patients with heart failure and has the potential to worsen an already grave prognosis. It has however not been well studied in sub-Saharan Africa, probably due to the expense and technicality of equipment needed to do so. The objective of this study was to establish the prevalence of sleep-disordered breathing in heart failure using a simple monitor and to determine clinical and demographic correlates of the phenomenon.
Methods: the study was a cross-sectional research of patients with heart failure; they had a full history and clinical examination and echocardiograms. Overnight pulse oximetry was carried out using an ambulatory pulse oximeter and the 3% oxygen desaturation index was determined digitally. sleep-disordered breathing was defined as oxygen desaturation index of ≥12.5/hour. The STOPBANG questionnaire was also administered to the subjects. Clinical features were correlated with ODI using student´s T-test, and a multivariate regression analysis was carried out with the significant features.
Results: forty-four (48.8%) of the patients had sleep-disordered breathing: 18.8% (17) of these had central sleep apnea, 30% (27) had obstructive sleep apnea. sleep-disordered breathing was more prevalent among males (p-value=0.008), heavier persons (p-value=0.033) and those with a higher Body mass index (p-value =0.032). The STOPBANG correlated well with oxygen desaturation index X2=4.403; p-value =0.036). The odds of having sleep-disordered breathing are higher with males OR:2.588, 95%CI=1.031-7.954, p=0.034 and with a high risk STOPBANG score (OR: 0.361, 95% CI=0.133-0.967; p=0.045.
Conclusion: sleep-disordered breathing is common among male patients with heart failure, and the STOPBANG score is valuable as a simple screening tool for sleep-disordered breathing in heart failure.
sleep-disordered breathing is an often unrecognized feature of patients with heart failure, yet it worsens the already poor prognosis of heart failure. Heart failure is a frequent diagnosis among patients admitted into medical wards and the incidence is on the rise with ageing of the populace approaching 5/1000 person/years in adults with a prevalence of 1-2% of adults [1,2]. Sleep-disordered breathing consists of central sleep apnea (CSA) usually with Cheyne-Stokes respiration (CSR), obstructive sleep apnea (OSA) [3,4] or a mixture of the two; these occur with a combined prevalence of between 71-76% as found in some European studies [5-7]. In Cheyne-Stokes respiration, there is abnormal feedback to and from the respiratory center with an excessive sympathetic response to arterial carbon dioxide resulting in an inappropriate hyperventilation during sleep [8] leading to apnea and hypopnea cycles with variation in heart rate, blood pressure, oxygen concentration, endothelial, function and elevation of C-reactive protein [9]. These worsen the clinical state of heart failure, and the two conditions have a perpetuating effect on each other [10]. Obstructive sleep apnea (OSA) may also accelerate progression of heart failure by causing a rise in venous return to the right heart and preload, thus compromising left ventricular function due to the negative intrathoracic pressure which is generated when respiration proceeds against a closed airway [11]. The hypopnea and apnea which occur in obstructive sleep apnea also activate the sympathetic nervous system [8].
The evaluation of sleep-disordered breathing includes an apnea/hypopnea index (AHI); being the ratio of events of apnea and hypopnea occurring overnight obtained by a polysomnogram [12,13] or a respiratory polygraph. Overnight pulse oximetry has been used in comparison with conventional polysomnography in patients with heart failure and other cohorts and found comparable [14,15]. The oxygen desaturation index (ODI) as obtained by overnight oximetry is a good predictor of AHI, which is measured by polysomnography. An oxygen desaturation index more than 12.5 times in an hour is 93% sensitive and 72% specific for diagnosing moderate to severe sleep-disordered breathing [10,12-15]. The prevalence of sleep-disordered breathing is not well known among patients with heart failure in our environment; this knowledge would afford treatment to be made available for sleep-disordered breathing (SDB) depending on the prominent type and this could improve symptoms and overall survival. The purpose of this study is to establish the prevalence of sleep-disordered breathing among patients with heart failure in Lagos State University Teaching Hospital; the prevalent type and also to determine the physical and laboratory features which would correlate to an oxygen desaturation index of 3% in ≥12.5/hour determined by overnight pulse oximetry. In addition, we aimed to compare the oxygen desaturation index determined by overnight pulse oximetry with the STOPBANG score for obstructive sleep apnea.
Study design and setting: this was a cross-sectional observational study carried out at the out-patient medical department and medical wards of a Nigerian Hospital between September 2017 and July 2020. The study was carried out at the Lagos State University Teaching Hospital (LASUTH), located in the metropolis of Ikeja, in South-West Nigeria. It is a tertiary health care institution which caters for the over 20 million inhabitants of Lagos State and many others from other states of the federation and sometimes from neighboring countries.
Study population: we recruited one hundred patients who met the criteria of the European Society of Cardiology Guidelines criteria for heart failure. These patients were recruited consecutively as they presented to the cardiology outpatient clinics or on admission into the medical wards. Inclusion criteria were age of 18 years and above, willingness to participate and meeting the criteria of the European Society of Cardiology for Heart failure. We excluded patients who had chronic obstructive airway disease and others who refused to give consent. All the participants gave informed written consent. The sample size was calculated using the formula;
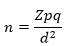
N= estimated sample size, Z= confidence level =1.96, P- estimated prevalence of heart failure in Nigeria (10%), Q= 1-P, D=margin of acceptable error or measure of precision=0.05. Calculated sample size was 70 and due to attrition a further twenty was added= 90 participants.
Data collection variables: the patients were recruited into the study by the research assistant and the resident doctors in the unit after they had given written informed consent to participate. The bio-data and medical history of the patients were obtained in addition to a full physical examination. Information about co-morbidities were also obtained. Patients were observed for Cheyne-Stokes respiration and the STOPBANG questionnaire [16] was used to categorize the patients into low or high risk for obstructive sleep apnea using the criteria of neck circumference, waist circumference, body mass index>30�kg/m2, snoring and hypertension; including history of snoring, loudness of snoring and whether they wake up tired or not (Annex 1). Echocardiograms were carried out on all patients in accordance with the American Society of Echocardiography guidelines; the equipment used was Sonoscape S40 Echocardiograph. Basic measurements were taken including left ventricular chamber size, left ventricular ejection fraction, atrial diameters, right ventricular systolic function determined by tricuspid annular posterior systolic excursion and right atrial systolic pressure.
An ambulatory wrist pulse oximeter (Prince-100H) was administered to every consenting patient in heart failure within 24 hours of the echocardiogram. The gadget gives a continuous reading of oxygen saturation and heart rate. The equipment was attached to the wrist of the non-dominant hand of the patient with the sensor on a finger when the subject went to bed and was disconnected in the morning on waking. Patients were instructed and shown how to ensure that the device was recording. Only recordings that lasted at least six hours were utilized; others less than six hours were discarded. The results of the overnight pulse oximetry which had been stored digitally were uploaded to a computer system via a universal serial bus (USB) interface and the results were analyzed by use of the oximeter data manager 5.0. The diagnosis of sleep-disordered breathing was made based on the number of 3% oxygen desaturation that each patient experienced in an hour overnight. An oxygen desaturation index (ODI) of ≥12.5 desaturations/hour was the benchmark for sleep-disordered breathing and central sleep apnea was determined by presence of Cheyne-Stokes respiration. Obstructive sleep apnea was defined as ODI ≥12.5/hour without the presence of CSR.
Quantitative variables: the quantitative variables obtained are age, weight, height, oxygen desaturation index (ODI), left ventricular ejection fraction, pulmonary artery systolic pressure, tricuspid annular systolic excursion. Categorical data such as sex, patient status, occupation, snoring and co-morbidities were also obtained. Descriptive statistics such as means, medians, ranges and standard deviations were used to summarize quantitative variables while categorical variables were summarized with frequencies, proportions and percentages and were expressed as means and percentages.
Statistical methods: data entry, cleaning, validation and analyses were done using Statistical Packages for Social Sciences (SPSS) version 23.0 Univariate analyses such as Chi-square test and Independent t-test were used to investigate the association between Oxygen desaturation index and potential predictor variables. Variables that were found to be significantly associated in bivariate analysis were harvested and subjected to Binary Logistic Regression to explore factors that were significantly associated with ODI. Model fit was assessed using the Hosmer Lemeshow goodness of fit test. All tests were carried out at 5% level of significance.
Ethical consideration: the study was reviewed and approved by the Health Research and Ethics Committee of Lagos State University Teaching Hospital REF.NO:LREC.06/10/800 and written informed consent was obtained from all willing participants.
General characteristics of the study population: there were 100 participants in the study, but only 90 had utilizable data; twenty-two (24.4%) of them were patients on out-patient follow-up in the clinic and (68) 75.6% who were patients recruited from the wards. The mean age was 51.8±13.8 years the number of male patients were fifty-five (61.1%) while females were thirty-five (38.9%). Eighteen (20%) of the patients were either serving public servants or retired, while 65 (72.2%) worked in the private sector; owned a business or were artisans. The mean weight of the patients was 69.1±13.9�kg the mean body mass index was 24.74±5.2�kg/m2 with about half the patients 46 (51.1%) having normal body mass index, while 5 (5.6%) were underweight. The mean systolic and diastolic blood pressures were 117.8±23.8 and 80.3±15.46 mmHg respectively. The median pulse rate was 89 beats per minute. A little over half of the patients had a history of hypertension 49 (54.4%) while only 12 (13.3%) had diabetes mellitus. The most prevalent heart disease was dilated cardiomyopathy followed by hypertensive heart disease found in 55 (61.6%) and 26 (28.9%) patients respectively (Table 1). Less than 10% (7) of the patients were smokers and 18.9% (17) drank alcohol. The number of patients who had suffered from strokes was eight (8.9%). The median New York Heart Association (NYHA) functional status grading was class 3 with 52% of the subjects falling under that category, in this respect there were missing data on the NYHA grading in more than half of the participants (Table 1). The mean left ventricular end-diastolic diameter was 65.34±10.13�mm, the mean left ventricular ejection fraction was 32.3±10.9%. The tricuspid annulus posterior systolic excursion which indicated right ventricular function was 15.14±4.18 mm and the mean pulmonary artery systolic pressure was 52.19±23.94 mmHg (Table 1).
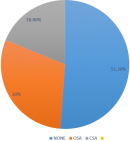
Prevalence of sleep-disordered breathing: a total of forty-four patients (48.8%) had sleep-disordered breathing based on a 3% oxygen desaturation index of ≥12.5/hour, comprised of seventeen patients with central sleep apnoea (18.8%) and twenty-seven patients with obstructive sleep apnoea (30%) Figure 1. Forty-one subjects (45.6%) had a high risk for obstructive sleep apnea using the STOPBANG score.
Correlates of sleep-disordered breathing: sleep-disordered breathing was more prevalent among the male patients and the difference was statistically significant (p=0.008. The patients with SDB had larger weight and the difference made statistical significance (p=0.033). There was also a significant difference in the body mass index (BMI) when those with SDB were compared with those who had no SDB (p= 0.032) (Table 2). There was a significant higher prevalence of smoking among the subjects with sleep-disordered breathing (p value = 0.047). The systolic and diastolic blood pressures were higher in the patients with SDB, but the difference was not statistically significant. There were more individuals with hypertension among those who did not have SDB than those found to have sleep-disordered breathing (53.1% vs 46.9%), but there was no statistical difference. Conversely, there was a higher prevalence of diabetes mellitus among those with sleep-disordered breathing (p value= 0.186) (Table 2). There was also a higher prevalence of previous strokes among those with SDB (p value= 0.420). However, these did not meet statistical significance. The left ventricular end diastolic diameter was larger in those with SDB than in those without SDB. There was a negative correlation between left ventricular ejection fraction (LVEF) and ODI 29.88±6.1 vs 34.65±13.3) X2= -1.914, p value = 0.060. The pulse rates of the subjects with SDB were slower than those who did not have sleep-disordered breathing (88.63±16 beats/minute vs 91.61±15 beats/minute) p= 0.38. The tricuspid annular posterior systolic excursion (TAPSE) which is an indicator of right ventricular systolic function was lower in patients with sleep-disordered breathing, but the difference was not statistically significant (14.63�mm vs15.63 mm) p value = 0.342 (Table 2). The STOPBANG score was used to stratify the patients into low risk and high risk for OSA, and a total of forty-one patients had a high risk for OSA using the STOPBANG score. The patients with the highest STOPBANG score were those with the highest ODI and there was a significant correlation between level of STOPBANG score and presence of sleep-disordered breathing using ODI of ≥12.5 ;X2 = 4.403, p value= 0.036. (Table 2). Multivariate logistic regression using the male sex; odds ratio: 2.588, 95%CI=1.031-7.954, p=0.034. Body weight which was also statistically different among those with SDB had odds ratio: 1.026,95% CI 0.958-1.098; p=0.464. The odds ratio for body mass index was 1.087, 95% CI 0.915-1.291; p=0.343; for smoking the odds ratio was 3.114,95%CI 0.290-33.442; p=0.348 while STOPBANG score gave the following odds ratio: 0.361, 95% CI=0.133-0.967; p=0.045 (Table 3). The sensitivity of STOPBANG to predict SDB is 56.8% and the specificity is 65.2% (Table 4).
This study set out to determine the prevalence of sleep-disordered breathing among patients with heart failure and evaluate the performance of STOPBANG score in the diagnosis of sleep-disordered breathing. We found the prevalence of sleep-disordered breathing in this cohort to be 48.8%, there was a significant correlation of sleep-disordered breathing with males, smoking, larger weight and BMI and STOPBANG score. The multivariate logistic regression showed that the male gender increased the odds of SDB by 2.5 and the STOPBANG low risk reduced the probability of SDB by 0.33. The prevalence derived by this study is similar to that of studies done outside the sub-Saharan region [3-7] where SDB prevalence ranged from 41 to 81%. This is of significance since we employed only the overnight pulse oximetry for diagnosis of SDB, whereas the quoted studies used either unattended cardiorespiratory polygraphy or overnight attended polysomnography. It further establishes overnight pulse oximetry as a useful tool for screening sleep-disordered breathing [13-15]. There is also a cost advantage in utilizing overnight pulse oximetry, which can be harnessed in sub-Saharan Africa to improve diagnosis and possibly recommend treatment for those affected. The risk of sleep-disordered breathing assessed by presence of snoring and daytime sleepiness scores has been evaluated in several studies in Nigeria both in patients with heart failure and in patients on medical wards by Akintunde and Desalu [17,18]. The risk of OSA among heart failure patients was estimated as 51.6% and 18% among patients admitted for other medical conditions. A lot more can be done to actually diagnose sleep-disordered breathing in this part of the world because risk of a condition does not necessarily confirm the diagnosis and the treatment would only be beneficial and applicable if the condition is confirmed.
The prevalence of OSA exceeded that of CSA following the pattern of occurrence in studies done by Bitter and Gupta, although those studies were done in patients with heart failure with preserved ejection fraction (HFpEF) in which the LVEF>50% [19,20]. The mean LVEF in our study was 32.15% and the studies with similar mean ejection fraction had higher prevalence of CSA than OSA and especially those in which the participants were all male. This is most probably linked to the poor circulation in the patients due to reduced cardiac output, which can initiate and sustain central sleep apnea. There was a significant male predominance in the cases with SDB compared to females in this study and this follows the trend seen in studies by Schulz, Ferrier and others [6,20-23]. Many of these studies included only male participants or had at least three quarters of the participants of the male gender. The odds of men having sleep-disordered breathing according to the multivariate analysis is 2.5: more than double the chances of same in a female patient. This could be explained by a higher risk of cardiovascular disease which most men have; with higher rates of smoking and alcohol consumption and moreover there is a higher incidence of snoring in men [17,18].
The weight and body mass index of the subjects were significantly higher among those with SDB compared with those without it: weight was a defining factor and the larger the BMI the higher the chances of SDB. This pattern was seen in a review by Khattak [24] who observed that in patients with heart failure with reduced ejection fraction (HFrEF), higher BMI was a risk factor for OSA. Gupta and Bitter also found that for those with heart failure with preserved ejection fraction(HFpEF), having a higher BMI increased the risk of having OSA [19,20] which is not surprising seeing that obesity and an increased neck circumference are risk factors for OSA. More of those with SDB were smokers: smoking has the effect of increasing the rate of oxidative stress which impacts obstructive sleep apnea, and it is believed that there is a synergy between tobacco smoke and OSA, though the mechanisms are not very clear [25]. A lower left ventricular ejection fraction (LVEF) is one of the independent risk predictors for sleep-disordered breathing [21-24] and in this study the mean LVEF was lower among those with SDB than those without SDB despite not reaching statistical significance; the degree of dysfunction of the myocardium as indicated by LVEF and tricuspid annular posterior systolic excursion (TAPSE) which is a measure of right ventricular contractile function are likely to enhance neurohormonal abnormalities which would definitely worsen the physical state of patients with heart failure and contribute to sleep-disordered breathing.
A significant correlation was found to exist between the STOPBANG score and ODI showing that STOPBANG is useful in determining OSA in heart failure as it has been found to be in the general population. The Epworth sleepiness score which is used in the general population to screen for OSA has not been found to be useful in the detection of OSA among heart failure patients because daytime sleepiness is not often reported [21,22,26]. Massongo et al. [27] screened a population of Cameroonians for SDB using STOPBANG questionnaire and cardiorespiratory polygraph, their findings were that the score has 75% negative predictive value and 82% sensitivity for OSA. In our study the specificity and sensitivity calculated is also nearer to a hundred which would imply the reliability of the overnight oximetry in diagnosing SDB in heart failure. This shows that STOPBANG can be used in sub-Saharan Africa in both the general population to screen for SDB and in heart failure. Therapy for sleep-disordered breathing in heart failure requires optimal guideline mediated medical treatment in all cases with the addition of continuous positive airway pressure ventilation, although this has only shown evidence of improvement in cardiac function and central apnea but not for reduction in mortality and morbidity [6,10]. There were limitations to the study because the study was a cross-sectional hospital based study and the findings may need to be interpreted with some caution. Also, the sample size was small. The strength of the study is however in the attempt to study prevalence of sleep-disordered breathing as against merely the risk of SDB, which other local studies were unable to do. It is therefore recommended that larger population based studies be carried out in sub-Saharan Africa to determine accurately prevalence of sleep-disordered breathing in heart failure.
Sleep-disordered breathing is common in Nigerian patients with heart failure in Lagos State University Teaching Hospital as detected by overnight pulse oximetry and it´s also more likely to occur in male patients who have a high risk STOPBANG score.
What is known about this topic
- Sleep-disordered breathing occurs in more than half of patients with heart failure;
- Overnight oximetry has been used to evaluate chronic heart failure patients for sleep-disordered breathing in a Caucasian cohort;
- STOPBANG score is a better screening tool for sleep-disordered breathing than Epworth sleepiness score among heart failure patients.
What this study adds
- Sleep-disordered breathing occurs more in male patients with heart failure, who may be overweight;
- STOPBANG score correlates well with oxygen desaturation index obtained by overnight oximetry;
- Sleep-disordered breathing can be diagnosed with a simple, affordable gadget -the ambulatory pulse oximeter, used overnight.
The authors declare no competing interests.
Folasade Adeola Daniel: conceptualized the research, wrote first draft and final manuscript. Atinuke Kalada Richards: contributed to data collection and wrote methodology. Phillip Alaba Adebola: participated in writing of the final draft. Oyenike Rashidat Opaleye: contributed to data collection. All the authors have read and agreed to the final manuscript.
We wish to acknowledge the help and encouragement of Dr Olabimpe Lamai and Dr Ayodele Ogunsanya and Mr Clement Akinsola for his help in the statistical analysis of this work.
Table 1: summary of patients characteristics
Table 2: correlation between oxygen desaturation index and clinical characteristics
Table 3: multivariate logistic regression analysis of clinical and demographic features with oxygen desaturation index
Table 4: correlation between STOPBANG score and oxygen desaturation index
Figure 1: distribution of sleep-disordered breathing among patients with heart failure
j
Annex 1: STOPBANG questionnaire (PDF-319Kb)
- Conrad N, Judge A, Tran J, Mohseni H, Hedgecott D, Crespillo AP et al. Temporal trends and patterns in heart failure incidence: a population-based study of 4 million individuals. Lancet. 2018;391(10120):572-580. PubMed | Google Scholar
- Ziaeian B, Fonarow GC. Epidemiology and aetiology of heart failure. Nat Rev Cardiol. 2016:13(6)368-78. PubMed | Google Scholar
- Javaheri S, Parker TJ, Wexler L, Michaels SE, Stanberry E, Nishiyama H et al. Occult sleep -disordered breathing in stable congestive heart failure. Ann Intern Med. 1995;122(7):487-492. PubMed | Google Scholar
- Wilcox I, McNamara SG, Wessendorf T, Wilson GN, Piper AJ, Sullivan CE. Prognosis and sleep-disordered breathing in heart failure. Thorax. 1998;53(Suppl3): S33-36. PubMed | Google Scholar
- Oldenburg O, Lamp B, Faber L, Teschler H, Horstkotte D, Topfer V. sleep-disordered breathing in patients with symptomatic heart failure: a contemporary study of prevalence in and characteristics of 700 patients. Eur J Heart Fail. 2007;9(3):251-257. PubMed | Google Scholar
- Schulz R, Blau A, Borgel J, Duchna HW, Fietze I, Koper I et al. Sleep Apnoea in heart failure. Eur Resp J. 2007;29(6):1201-1205. PubMed | Google Scholar
- Paulino A, Damy L, Margarit L, StoÏca M, Deswart G, Khouri L et al. Prevalence of sleep-disordered breathing in a 316 -patient French cohort of stable congestive heart failure. Archives of Cardiovascular Disease. 2009;102(3):169-175. PubMed | Google Scholar
- Spaak J, Egri ZJ, Kubo T, Yu E, Ando SI, Kaeko Y et al. Muscle sympathetic nerve activity during wakefulness in heart failure patients with and without sleep apnea. Hypertension. 2005;46:1327-1332. PubMed | Google Scholar
- Dimsdale JE, Coy T, Ziegler MG, Ancoli-Israel S, Clausen J. The effect of sleep apnea on plasma and urinary catecholamines. Sleep. 1995;18:377-381. PubMed | Google Scholar
- Pearse SG, Cowie MR. sleep-disordered breathing in Heart failure. European Journal of Heart Failure. 2016 Apr;18(4):353-61. PubMed | Google Scholar
- Brinker JA, Weiss JL, Lappe DL, Rabson JL, Summer WR, Permutt S et al. Leftward septal displacement during right ventricular loading in man. Circulation. 1980;61(3):626-633. PubMed | Google Scholar
- Kapur VK, Aukley DH, Mehra R, Ramar K, Harrod CG. Clinical Practice Guidelines for Diagnostic Testing for Adult Obstructive Sleep Apnea. An American Academy of Sleep Medicine Clinical Practice Guideline. J Clin Sleep Med.2017;13(3):4709-504. Google Scholar
- Ramachandran SK, Josephs LA. A Meta-analysis of Clinical screening tests for obstructive sleep apnoea. Anesthesiology. 2009 Apr;110(4):928-39. PubMed | Google Scholar
- Ward NR, Cowie MR, Rosen SD, Roldao V, De Villa M, McDonagh TA et al. Utility of overnight pulse oximetery and heart rate variability analysis to screen for sleep-disordered breathing in chronic heart failure. Thorax. 2012 Nov;67(11):1000. PubMed | Google Scholar
- Chung F, Liao P, Elsaid H, Islam S, Shapiro CM, Sun Y. Oxygen desaturation index from nocturnal oximetry: a sensitive and specific tool to detect sleep-disordered breathing in surgical patients. Anaesth Analog. 2012;114(5):993-1000. PubMed | Google Scholar
- Chung F, Abdullah HR, Liao P. STOPBANG questionnaire: a practical approach to screen for obstructive sleep apnea. Chest. 2016;149(3),632-638. PubMed | Google Scholar
- Akintunde AA. Snoring and risk for obstructive sleep apnea among Nigerians with heart failure: prevalence and clinical correlates. Heart Views. 2013 Jan;14(1):17-21. PubMed | Google Scholar
- Desalu O, Onyedum C, Sanya E, Fadare J, Adeoti A, Salawu F et al. Prevalence Awareness and Reporting of Obstructive Sleep Apnoea among Hospitalized Adult Patients in Nigeria:A Multicenter Study. Ethiop J Health. Sci. 2016;26(4)321-330. PubMed | Google Scholar
- Bitter T, Faber L, Hering D, Langer C, Horstkotte D ,Oldenburg O. Sleep-disordered breathing in heart failure with normal ejection fraction. Eur J Heart Fail. 2009;11(6):602-8. PubMed | Google Scholar
- Gupta N, Agrawal S, Goel AD, Ish P, Chakrabarti S, Suri JC. Profile of sleep-disordered breathing in heart failure with preserved ejection fraction. Monaldi Archives for Chest Disease. 2020 Nov 9;90(4). PubMed | Google Scholar
- Ferrier K, Campbell A, Yee B, Richards M, O´Meeghan T, Weatherall M et al. Sleep-disordered breathing occurs frequently in stable outpatients with congestive heart failure. Chest. 2005;128(4):2116-22. PubMed | Google Scholar
- Arzt M, Young T, Finn L, Skatrud JB, Ryan CM,Newton GE et al. Sleepiness and sleep in patients with systolic heart failure and obstructive sleep apnea. Arch Intern Med. 2006;166(16):1716-22. PubMed | Google Scholar
- Javaheri S, Parker TJ, Liming JD, Corbett WS, Nishiyama H, Wexler L et al. Sleep apnea in 81 ambulatory male patients with stable heart failure. Types and their prevalences, consequences and presentations. Circulation. 1998;97(21):2154-9. PubMed | Google Scholar
- Khattak HK, Hayat F, Pamboukian SV, Hahn HS, Schwartz BP, Stein PK. Obstructive Sleep Apnea in Heart Failure: Review of Prevalence, Treatment with Continuous Positive Airway Pressure and Prognosis. Tex Heart Inst J. 2018;45(3):151-61. PubMed | Google Scholar
- Deleanu OC, Pocora D, Mihalcuta S, Ulmeanu R, Zaharie AM, Mihaltan F. Influence on smoking and obstructive sleep apnea. Pneumologica. 2016;65(1):28-35. PubMed | Google Scholar
- Taranto ML, Floras JS, Millar PJ, Kasai T, Gabriel JM, Spaak J et al. Inverse relationship of subjective daytime sleepiness to sympathetic activity in with heart failure and obstructive sleep apnea. Chest. 2012;142(5):1222-1228. PubMed | Google Scholar
- Massongo M, Balkissou AD, Kenyo CK, Sawa BN, Kanko N, Pefura EW. The STOPBANG score is effective for obstructive sleep apnea syndrome screening and correlates with its features, in a sub-Saharan African population. Pan African Medical Journal. Pan Afr Med J. 2020 Jun 15;36:93. PubMed | Google Scholar