Management of a type 2 DM patient with cardio-cerebral infarction in a resource-limited environment: a case report
Okechukwu Obumneme Ezekpo, Oladiipo Olanipekun, Opeyemi Ezekiel Ojo, Oluwafemi Andrew Ogunniyi, Gbadebo Oladimeji Ajani, Adedayo Hakeem Oyebanji, Habib Olatunji Alagbo, Mayowa Sodiq Akinpelu
Corresponding author: Okechukwu Obumneme Ezekpo, Department of Medicine, Afe Babalola University, Ado Ekiti and Multi-System Hospital, Ado Ekiti, Nigeria 
Received: 12 Jan 2023 - Accepted: 19 May 2023 - Published: 27 Jun 2023
Domain: Cardiology,Diabetes care,Neurology (general)
Keywords: Cardio-cerebral infarction, resource-limited environment, case report
©Okechukwu Obumneme Ezekpo et al. PAMJ Clinical Medicine (ISSN: 2707-2797). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Okechukwu Obumneme Ezekpo et al. Management of a type 2 DM patient with cardio-cerebral infarction in a resource-limited environment: a case report. PAMJ Clinical Medicine. 2023;12:21. [doi: 10.11604/pamj-cm.2023.12.21.38871]
Available online at: https://www.clinical-medicine.panafrican-med-journal.com//content/article/12/21/full
Case report 
Management of a type 2 DM patient with cardio-cerebral infarction in a resource-limited environment: a case report
Management of a type 2 DM patient with cardio-cerebral infarction in a resource-limited environment: a case report
![]() Okechukwu Obumneme Ezekpo1,&,
Okechukwu Obumneme Ezekpo1,&, ![]() Oladiipo Olanipekun1,
Oladiipo Olanipekun1, ![]() Opeyemi Ezekiel Ojo2, Oluwafemi Andrew Ogunniyi1, Gbadebo Oladimeji Ajani3,
Opeyemi Ezekiel Ojo2, Oluwafemi Andrew Ogunniyi1, Gbadebo Oladimeji Ajani3, ![]() Adedayo Hakeem Oyebanji4,
Adedayo Hakeem Oyebanji4, ![]() Habib Olatunji Alagbo5,
Habib Olatunji Alagbo5, ![]() Mayowa Sodiq Akinpelu1
Mayowa Sodiq Akinpelu1
&Corresponding author
A "cardio-cerebral infarction" is described as a concomitant occurring acute myocardial infarction and an ischemic cerebrovascular accident. It is a very rare condition, which currently has no local or national guidelines in Nigeria on its management and with the co-existence of Type 2 Diabetes Mellitus (DM) as another co-morbidity, an equally challenging condition in itself in resource-limited countries, further complicates its management. We present a 67-year-old recently diagnosed Type 2 DM patient referred to the Cardiology clinic of our hospital for percutaneous coronary intervention (PCI) following a diagnosis of ST segment elevation myocardial infarction (STEMI). The patient presented with a-day history of retrosternal pain associated with two episodes of vomiting, a positive history of abdominal pain, and a low-grade fever. There was associated obesity, dyslipidemia and a positive family history of diabetic mellitus, however with no history of hypertension or peptic ulcer disease. A 12-lead electrocardiography showed atrial fibrillation, a left axis deviation and ST segment elevation in the antero-inferior leads. Subsequently, the patient´s level of consciousness and higher cortical function deteriorated with an observed right-sided flaccid hemiparesis, from an acute ischemic stroke. A brain Magnetic Resonance Imaging (MRI) showed an acute left temporo-parietal lobe infarct in the vascular territory of the left middle cerebral artery (MCA), a subacute right parietal lobe infarct in the vascular territory of the right MCA, and chronic periventricular, deep white matter, pontine, and medullary infarcts. The Glycated hemoglobin (HbA1C) at presentation was 8.6%. The patient was successfully managed conservatively with no thrombolysis or revascularization technique, despite the challenges of managing such a condition in a resource-limited environment.
A stroke, according to the World Health Organization, is a clinical syndrome consisting of rapidly developing clinical signs of focal or global disturbance of cerebral function attributable to a vascular cause which persists for more than 24 hours [1]. A "cardio-cerebral infarction" is described as a concomitant occurring acute myocardial infarction (AMI) and an ischemic stroke either at the same time (simultaneous or synchronous) or one after the other (metachronous) [2].
Both AMI, especially STEMI and Acute Ischaemic stroke have a narrow therapeutic time-window, and a delayed intervention of one infarcted territory for the other may result in permanent irreversible morbidity or disability and even death. In addition to the dilemma of the sequence of management, the agents of management for each territory may complicate the extent of the other infarcted territory [3]. Conservative management of patients with this condition, also with type 2 DM in the picture and which inadvertently remains the most viable option in a resource-setting, will always pose a challenge.
Patient information: a 67-year-old right-handed female patient was referred to us with a diagnosis of ST segment elevation myocardial infarction (STEMI) for Percutaneous Coronary Intervention (PCI) from a Federal Medical Center. The patient had presented with a three-day history of retrosternal pain described as being compressing in nature, with associated vomiting of two episodes and a low-grade fever. Prior to referral, the patient had investigations done and was given drugs including aspirin and isosorbide dinitrate at the referring facility. She was newly diagnosed to have type 2 diabetes mellitus (DM) with a positive family history of DM in a first-degree relative, but no known family history of heart disease or hypertension. No history of smoking or alcohol use.
Clinical findings: clinical examination revealed a confused patient with a Glasgow Coma Score (GCS) of 14/15 (eye-opening = 4, best verbal response = 4, best motor response = 6), normal tone globally, full power (5/5) in all limbs. On cardiovascular examination, she was tachycardic with a pulse rate of 104 beats per minute (bpm) which was irregularly irregular and blood pressure of 121/80 mmHg. No raised jugular venous pressure, apex beat was located at the 5th left intercostal space, lateral to the mid-clavicular line and heaving. Heart sound was chaotic with a rate of 142bpm and pulse deficit of 38. Other systemic examinations revealed no abnormal findings.
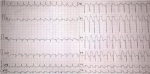
Diagnostic assessment: investigations performed included an electrocardiogram (ECG), which (Figure 1) revealed extensive ST segment elevation in the antero-inferior leads (V1-V6, I, II and avF), pathological Q wave in V2-V4, atrial fibrillation with rapid ventricular response at a rate of 148bpm, and a left axis deviation. Other investigations revealed an HbA1c of 8.6%, a raised level of Aspartate Transaminase (AST) (80IU/L), a deranged lipid profile, a prolonged prothrombin time (19.2 secs), and a normal international normalized ratio (INR) and normal renal function test. Echocardiogram revealed moderate pericardial effusion, left ventricular hypertrophy, akinesis of the antero-septal and infero-septal wall and a dilated left atrium. No intra-cardiac clot was seen. The initial diagnosis made was that of an Acute (ST segment elevation) Myocardial Infarction in a known Type 2 DM patient complicated by arrythmias (atrial fibrillation).
Therapeutic interventions: the patient was admitted to the intensive care unit and was conservatively treated with dual antiplatelets, anticoagulant therapy, nitrate, beta blocker, Angiotensin-converting enzyme (ACE) inhibitor and a basal-bolus insulin regimen. Thrombolysis was not considered because of the late presentation of the patient; however, she was being prepared for percutaneous coronary intervention after stabilization.
Timeline: the above presentation was witnessed on day one of this patients´ presentation. On the second day of admission, the patient's consciousness level suddenly deteriorated with a decline of the GCS to 10 (eye opening = 3, best verbal response = 1, best motor response = 6) and had expressive aphasia. A right-sided flaccid hemiparesis with a power of 4/5 was also noticed.
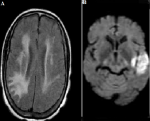
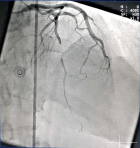
Diagnostic assessment: a brain MRI showed an acute left temporo-parietal lobe infarct in the vascular territory of the left Middle Cerebral Artery (MCA) (Alberta stroke programme early computerized tomography {ASPECT} score of 6), a subacute right parietal lobe infarct in the vascular territory of the right MCA, and chronic periventricular, deep white matter, pontine, and medullary infarcts (Figure 2). A coronary angiogram revealed a 99% occlusion of the left anterior descending (LAD) midsegment and diffuse disease of the distal LAD (Figure 3). A further diagnosis of a Left Hemispheric Ischaemic stroke in MCA territory was made; risk factors being - advanced age, black race, post - menopausal state, type 2 DM & dyslipidaemia. At this juncture, and with the two earlier diagnoses made; an ´Acute cardio-cerebral infarction in a known Type 2 DM patient´ was entertained as the final diagnosis.
Therapeutic intervention: the patient was managed conservatively and monitored in the intensive care unit (ICU) for a period of 10 consecutive days, with concomitant complications, including hypokalemia, hyperglycemia, infections, and psychosis, requiring the intervention of other specialists.
Follow-up and outcome of interventions: the patient was discharged on the 12th day after admission with no further complaints, regained consciousness fully with improvement of paresis. She became euglycemic, was placed on continuous prophylaxis with antiplatelet therapy, anticoagulant therapy, oral hypoglycemic agents, basal insulin, nitrate, beta blocker, ACE inhibitor, statin, and physiotherapy.
Patient perspective: the patient stated that she was brought to this hospital to seek better care, as she was told there was something that needed to be done for her, to fix her heart problems, which could not be done at the referring hospital. She noted that she was quite satisfied with the level of care given to her and stated that she was grateful to God for making her well again. Furthermore, she further stated that she will permit the use of knowledge gained in the management of her case for the benefit of humanity.
Informed consent: the patient provided her full consent after oral explanation of our intention of publishing her case.
Cardio-cerebral infarction has no recommended guidelines for treatment due to the rarity of this pathology. It poses a challenge for physicians, as early diagnosis and management of these two medical emergencies are paramount. Development of one of these emergency conditions increases the risk of the other, and timely treatment of one of the conditions delays the other [4,5]. Unlike in individuals who are not diabetic, ischemic heart disease and dyslipidemia, both of which were present in our patient, have been established to be independently associated with ischemic stroke in patients with diabetes [6]. In this report, the patient was referred to our cardiology clinic, the only PCI-capable clinic in the region from a non-PCI-capable one, leading to an elapsed therapeutic window for thrombolysis. We assume that this delay resulted in the development of post-myocardial infarction (post-MI) complications such as post-MI carditis with pericardial effusion, septal wall akinesis and possibly cardiac/arterial thromboembolism due to atrial fibrillation. All the above factors as well as the baseline risk factors of type 2 diabetes mellitus and dyslipidemia could have resulted in the development of acute ischemic stroke as seen in this patient [4,5]. It is a common occurrence for patients in resource-limited countries to present late for appropriate standard care after acute MI and possible reasons are financial constraints, inadequate or inaccessibility to specialist clinic and the non-availability of trained personnel in procedures such as PCI.
This index patient was not offered therapy with alteplase or other intravenous recombinant-tissue plasminogen activators (IV rtPA) for the ischemic stroke because of a recent myocardial infarction, which amongst other factors is considered a relative contraindication for such therapy due to the risk of developing cardiac wall rupture and cardiac tamponade [7]. Other factors include older age, female sex, large anterior MI, longer time from symptom onset to thrombolysis, infarct size, transmural extent, and pericardial involvement - most of which were present in our patient [8,9]. Variable management approaches have been reported for the treatment of cardio-cerebral infarction. These treatments include PCI +/-drug therapy (or) ALTEPLASE/IV rtPA +/-drug therapy (or) both +/-drug therapy (or) drug therapy only [3,10]. Omar et al. reported the case of a 48-year-old male who developed a massive cerebral infarction with a GCS of 3/15 following admission to the emergency room for acute transmural infero-posterior and right ventricular infarction. A similar management approach to ours with no thrombolytic therapy nor PCI was used, however, that patient passed away the following day [2]. Ibekwe et al. reported the case of an 80-year-old female who presented similarly. The patient presented early and was treated with thrombolytic and antiplatelet therapy only, without PCI administration due to the risk of hemorrhagic conversion. The patient passed away on the third day [10]. Akinseye et al. described the case of a 53-year-old male who also presented similarly. Thrombolytic therapy was contraindicated by a refractory hypertension with a blood pressure of 230/130 mmHg; however, PCI was administered due to the availability of on-site interventional cardiologists. Endovascular embolectomy of the middle cerebral artery was also done. The patient was wheelchair bound after 3 months [3].
The 3 cases referenced above, with other published cases in literature, shows that variable approaches as deemed ideal by different managing teams have been employed in the management of cardio-cerebral infarction. The results have also been different, and despite being rare, the 3-month survival chance is increased with the use of PCI and endovascular embolectomy. However, to the best of our knowledge, the index case report, despite its increased management challenges in the face of multiple co-morbidity, is the first of its kind where a patient who received drug therapy only, survived up to 3 months post-cardio-cerebral infarction. This therefore provides a measure of hope to medical teams in resource-limited settings like ours, that a successful intervention in the treatment of this pathology using drug therapy alone is a possibility.
The success in this case reported is isolated, and more studies are required to determine the ideal management guidelines for cardio-cerebral infarction. Although the challenges faced in a developing country like ours played a role in the choice of treatment for our patient, it also highlights a possible consideration of conservative treatment when setting the guidelines for the treatment of cardio-cerebral infarction.
The authors declare no competing interests.
All the authors have read and agreed to the final manuscript.
Figure 1: an electrocardiogram (ECG), showing an anteroseptal and anterolateral wall myocardial infarction
Figure 2: a brain magnetic resonance imaging (MRI) showing acute, subacute and chronic infarcts
Figure 3: a coronary angiogram showing occlusions
- Chugh C. Acute Ischaemic Stroke: Management Approach. Indian Journal of Critical Care Medicine. 2019; 23(Suppl 2): S140-S146. PubMed | Google Scholar
- Omar HR, Fathy A, Rashad R, Helal E. Concomitant acute right ventricular infarction and ischemic cerebrovascular stroke; possible explanations. Int Arch Med. 2010;3:25. PubMed | Google Scholar
- Akinseye OA, Shahreyar M, Heckle MR, Khouzam RN. Simultaneous acute cardio-cerebral infarction: is there a consensus for management. Ann Transl Med. 2018 Jan;6(1):7. PubMed | Google Scholar
- Gunnoo T, Hassan N, Khan MS, Slark J, Bentley P, Sharma P. Quantifying the risk of heart disease following acute ischemic stroke: a meta-analysis of over 50,000 participants. BMJ Open. 2016 Jan 20;6(1):e009535. PubMed | Google Scholar
- Witt BJ, Ballman KV, Brown RD, Meverden RA, Jacobsen SJ, Roger VL. The incidence of stroke after myocardial infarction: a meta-analysis. Am J Med. 2006 Apr;119(4):354.e1-9. PubMed | Google Scholar
- Arboix A, Rivas A, García-Eroles L, De Marcos L, Massons J, Oliveres M. Cerebral Infarction in Diabetes: Clinical Pattern, Stroke Subtypes, and Predictors of In-Hospital Mortality. BMC Neurol. 2005 Apr 15;5(1):9. PubMed | Google Scholar
- De Silva DA, Manzano JJ, Chang HM, Wong MC. Reconsidering recent myocardial infarction as a contraindication for IV stroke thrombolysis. Neurology. 2011 May 24;76(21):1838-40. PubMed | Google Scholar
- Patel MR, Meine TJ, Lindblad L, Griffin J, Granger CB, Becker RC. Cardiac tamponade in the fibrinolytic era: analysis of >100,000 patients with ST-segment elevation myocardial infarction. Am Heart J. 2006 Feb;151(2):316-22. PubMed | Google Scholar
- Becker RC, Hochman JS, Cannon CP, Spencer FA, Ball SP, Rizzo MJ, Antman EM. Fatal cardiac rupture among patients treated with thrombolytic agents and adjunctive thrombin antagonists: observations from the Thrombolysis and Thrombin Inhibition in Myocardial Infarction 9 Study. J Am Coll Cardiol. 1999 Feb;33(2):479-87. PubMed | Google Scholar
- Ibekwe E, Kamdar HA, Strohm T. Cardio-cerebral infarction in left MCA strokes: a case series and literature review. Neurol Sci. 2022 Apr;43(4):2413-2422. PubMed | Google Scholar