Neurosurgical approach in intra-conical orbital dermoid cyst: a case report
Yassine Moursli, Younesse Hidan, Mohamed Reda Bentouhami, Adil Mchachi, Leila Benhmidoune, Rayad Rachid, Mohamed El Belhadji
Corresponding author: Yassine Moursli, University of Hassan II, Adults Ophthalmology Department, 20 August Hospital, Casablanca, Morocco 
Received: 28 Aug 2023 - Accepted: 07 Oct 2023 - Published: 24 Oct 2023
Domain: Ophthalmology
Keywords: Dermoid cyst, orbit, neurosurgical approaches, case report
©Yassine Moursli et al. PAMJ Clinical Medicine (ISSN: 2707-2797). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Yassine Moursli et al. Neurosurgical approach in intra-conical orbital dermoid cyst: a case report. PAMJ Clinical Medicine. 2023;13:23. [doi: 10.11604/pamj-cm.2023.13.23.41551]
Available online at: https://www.clinical-medicine.panafrican-med-journal.com//content/article/13/23/full
Neurosurgical approach in intra-conical orbital dermoid cyst: a case report
Yassine Moursli1,&, ![]() Younesse Hidan1, Mohamed Reda Bentouhami1, Adil Mchachi1, Leila Benhmidoune1, Rayad Rachid1, Mohamed El Belhadji1
Younesse Hidan1, Mohamed Reda Bentouhami1, Adil Mchachi1, Leila Benhmidoune1, Rayad Rachid1, Mohamed El Belhadji1
&Corresponding author
Dermoid cysts are benign congenital tumors whose clinical expression varies according to location and size. Two forms are to be individualized: the superficial forms and the deep retro- or peri-bulbar forms. The intra-conical location is exceptional, and the diagnosis is often made at the stage of compression of the neighboring elements. Surgical access to these tumors remains difficult, hence the need for more elaborate approaches. We describe the observation of an intra-conical orbital dermoid cyst that underwent neurosurgical ablation by subfrontal approach.
Dermoid cysts are benign congenital tumours, having a dual ectodermal and mesodermal origin, and whose wall delimits a cavity with a complex content made of keratin, sebum, hair, etc. [1]. The clinical expression of these tumors varies according to their location and size. The preferential orbital location is the tail of the eyebrow. The posterior orbital location is rare, and the diagnosis is often made at the stage of compression of the neighboring elements [2]. Such a location has the disadvantage of being difficult to access, requiring special approaches. We report the case of an intra-conical orbital dermoid cyst that underwent neurosurgical ablation.
Patient information: an 8-year-old boy who presented with a progressive decrease in visual acuity of the right eye, evolving for 2 months.
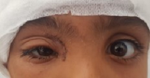
Clinical finding: best corrected visual acuity was limited to 2/10 with minimal axile, irreducible, and non-pulsatile exophthalmos, without associated oculomotor disorder (Figure 1) as well as a relative afferent pupillary reflex and temporal papillary hyperaemia. Examination of the left eye was normal.
Timeline of the current episode: July 2022: the exophthalmos was noted by the parents. August 2022: orbital MRI was performed. August 2022: patient referral to the healthcare unit. September 2022: surgery was performed.
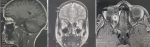
Diagnostic assessment: an orbital MRI was performed showing the presence at the right intra-orbital level, at the supero-internal angle, of a well-limited formation, in T1 hypersignal, heterogeneous T2 hypersignal, partly disappearing after fat saturation and partly enhancing after injection of gadolinium. It comes into intimate contact with the internal rectus muscle and spreads the superior rectus. It measures 12 x 10 mm (Figure 2).
Diagnostic: the results were consistent with an intra-conical dermoid cyst.
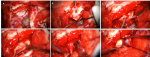
Therapeutic interventions: an attempted surgical extraction by lynch incision ended in failure (Figure 3). A sub frontal approach without removal of the upper orbital rim was performed and allowed extraction of the tumor (Figure 4).
Follow-up and outcome of interventions: histological examination confirmed diagnosis of a dermoid cyst by finding a cystic formation bordered by a regular focally ciliated squamous lining, resting on a fibrous wall. Follow-up after one week found an improvement in visual acuity which rose to 7/10 with the persistence of sequelae abnormalities in papillary OCT (Figure 5). The patient is still seen in consultation and shows no signs of recurrence.
Patient perspective: “I am relieved that the surgery went well, and I am very glad I got my vision back ”.
Informed consent: the patient gave informed consent.
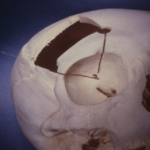
Dermoid cysts are benign congenital tumors belonging to the group of choristomas. They represent 14% of all orbital tumors. These tumors affect preferentially young subjects: 50% of cases are diagnosed before the age of 15 [3]. Two forms are to be individualized: the superficial forms, which most often sit at the level of the tail of the eyebrow and whose diagnosis is easy. They appear as a firm, painless swelling. The deep orbital forms are rarer (0.5% of dermoid cysts), they most often sit extra-conically, near the bone. They are generally asymptomatic at first and are diagnosed late, when they increase in size, in adolescence or adulthood, at the stage of exophthalmos or compression of neighboring elements (optic nerve, etc.) [4]. The intra-conical localization is exceptional. In our case, it had the disadvantage of being difficult to access, hence the need for a neurosurgical approach. Neurosurgical routes allow access to the posterior two-thirds of the orbit and sometimes require more or less extensive bone removal. They can be summarized into three types: superior routes, lateral routes, and superolateral mixed routes [5]. The superior or subfrontal route, which was adopted in our case, can be driven according to classical schemes or be widened at the orbital rim, thus offering optimal exposure to the orbit and its contents, including the eyeball (Figure 6) [6]. Indications for the upper transcranial pathways include tumors developing intracranially, or extending into the optic canal, such as meningiomas of the optic nerve sheath, or gliomas of the optic nerve; tumors in the apical region; tumors of the internal quadrants and large tumors extending from the globe to the apex, such as lymphangiomas or schwannomas and bone tumors of the orbital roof [5]. Postoperative complications include epilepsy, post-operative infections, cerebral edemas or hematomas related to cerebral retraction, subcutaneous cerebrospinal fluid fistula, and transient post-operative ptosis in case of mobilization of the levator muscle of the upper eyelid [5].
The intraconical localization of orbital dermoid cysts remains exceptional. They are often revealed by signs of compression of neighboring elements, namely the optic nerve, and must benefit from urgent surgical treatment. The use of more elaborate routes is sometimes necessary for the surgical extraction of these tumors. The subfrontal neurosurgical approach represents an interesting access route to these locations.
The authors declare no competing interests.
Yassine Moursli: study concept, data curation, formal analysis, methodology, project management, and writing (original draft, review, and editing). Younesse Hidan, Mohamed Reda Bentouhami, Adil Mchachi, Leila Benhmidoune, Rayad Rachid, Mohamed El Belhadji : study concept, data curation, formal analysis, methodology, project management, and writing (review and editing). All authors have read and approved the final manuscript
Figure 1: (A,B,C) absence of oculomotor disorder
Figure 2: orbital magnetic resonance imaging (MRI) in T1 (A), T2 (B) and T1 with injection of gadolinium (C) sequences
Figure 3: lynch incision
Figure 4: (A,B,C,D,E,F) intraoperative photographs of the surgery
Figure 5: papillary optical coherence tomography (OCT) showing sequelae thinning of the temporal optic fiber layers
Figure 6: superior orbital removal
- Civit T, Joud A, Klein O. Congenital orbital tumors in adults (dermoid cysts). Neurochirurgie. 2010 Apr-Jun;56(2-3):183-6. PubMed | Google Scholar
- El Afrit MA, Trojet S, Kammoun H, Sdiri N, Abid BS, Bromdhane F et al. Dermoid cysts: epidemiological, clinical and pathological studies. J Fr Ophtalmol. 2003 Jun;26(6):618-21. PubMed | Google Scholar
- Gotzamanis A, Desphieux JL, Pluot M, Ducasse A. Dermoid cysts. Epidemiology, clinical and anatomo-pathologic aspects, therapeutic management. J Fr Ophtalmol. 1999 May;22(5):549-53. PubMed | Google Scholar
- Ruban JM. Kystes dermoïdes. Pathologie orbito-palpébrale. Paris: Masson. 1998;550-62.
- Civit T, Cophignonb J. Les voies d´abord neurochirurgicales de l´orbite. Neurochirurgie. 2010 Apr 1;56(2-3):218-29. Google Scholar
- Cophignon J, Clay C, Marchac D, Rey A. Abord sous-frontal élargi des tumeurs de l´orbite. Neurochirurgie. 1974:20;161-167.