Community-acquired bacterial meningitis due to Enterobacter cloacae in an infant: a case report and literature review
Houssam Rajad, Youssef Hadzine, Adel Elmekkaoui, Othmane Belenda, Hicham Nassik, Wiam Timsahi, Soukaina Wakrim
Corresponding author: Houssam Rajad, Resuscitation Department, Ibn Zohr University and Regional Hospital Center Hassan II, Agadir, Morocco 
Received: 30 Oct 2023 - Accepted: 05 Nov 2023 - Published: 20 Nov 2023
Domain: Emergency medicine,Infectious disease,Intensive care medicine
Keywords: Community-acquired bacterial meningitis, Enterobacter cloacae, infant, case report
©Houssam Rajad et al. PAMJ Clinical Medicine (ISSN: 2707-2797). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Houssam Rajad et al. Community-acquired bacterial meningitis due to Enterobacter cloacae in an infant: a case report and literature review. PAMJ Clinical Medicine. 2023;13:24. [doi: 10.11604/pamj-cm.2023.13.24.42082]
Available online at: https://www.clinical-medicine.panafrican-med-journal.com//content/article/13/24/full
Case report 
Community-acquired bacterial meningitis due to Enterobacter cloacae in an infant: a case report and literature review
Community-acquired bacterial meningitis due to Enterobacter cloacae in an infant: a case report and literature review
Houssam Rajad1,&, ![]() Youssef Hadzine1, Adel Elmekkaoui1, Othmane Belenda1,
Youssef Hadzine1, Adel Elmekkaoui1, Othmane Belenda1, ![]() Hicham Nassik1,
Hicham Nassik1, ![]() Wiam Timsahi2,
Wiam Timsahi2, ![]() Soukaina Wakrim2
Soukaina Wakrim2
&Corresponding author
Enterobacter cloacae meningitis represents a rare form of community-acquired bacterial meningitis. We report a case of a 9-month-old immunocompetent infant who was hospitalized for community-acquired meningitis caused by Enterobacter cloacae, with a computed tomography (CT) brain showing an ischemic stroke of the middle cerebral artery. The patient was treated with meropenem and amikacin. The clinical progression was favorable, although a residual mono paresis affecting the right lower limb persisted.
Bacterial meningitis in children is a significant concern due to its high mortality rate and the elevated rate of intensive-care hospitalizations. Commonly encountered pathogens include Streptococcus pneumoniae, Haemophilus influenzae, and Neisseria meningitidis. Whereas enterobacter infections are infrequently implicated.
In this case report, we present a case of community-acquired meningitis caused by Enterobacter cloacae in a 9-month-old immunocompetent infant who was admitted to the intensive care unit with a favorable clinical progression under meropenem and amikacin treatment.
Patient information: we present the case of a 9-month-old female infant with no significant medical history, exhibiting normal psychomotor development. The patient was admitted to the intensive care unit for management of a meningeal syndrome that had been progressing for 3 days, which was further complicated by a convulsive status epilepticus.
Clinical findings: clinical examination upon admission revealed a febrile infant with normal blood glucose levels, a Glasgow coma scale score of 10/15, and no hemodynamic or respiratory instability. Furthermore, neck stiffness and muscular hypertonia were detected during the clinical examination.
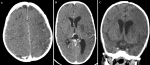
Diagnostic assessment: bain CT scan with and without contrast injection revealed an ischemic stroke involving both the superficial and deep territories of the middle cerebral artery, accompanied by moderate passive hydrocephalus (Figure 1).
The lumbar puncture revealed purulent cerebrospinal fluid. Cerebrospinal fluid examination revealed a cell count of 64,000 (80% polymorphonuclear), glycorrhachia concentration of 0.0g/l and proteinorachia of 7.23g/l. The results of the culture and sensitivity test of antibiotics were positive for Enterobacter cloacae which was resistant to fluoroquinolones, amoxicillin, ticarcillin, and cefoxitin, while being sensitive to ceftriaxone, cefepime, carbapenems, and aminoglycoside.
Therapeutic intervention: considering the admission presentation and the results from the cytobacteriological and biochemical analysis of the cerebrospinal fluid (CSF), a broad-spectrum empirical antibiotic therapy was initiated, including a third-generation cephalosporin (ceftriaxone) and an aminoglycoside (gentamicin). Upon receiving the results of culture and sensitivity test of antibiotics, the antibiotic protocol was changed to carbapenem (meropenem) and an aminoglycoside (amikacin). The convulsive seizures were managed with phenobarbital, and antipyretic measures were implemented.
Follow-up and outcomes: the clinical progression was favorable under treatment, the patient became afebrile and regained consciousness, although a residual monoparesis affecting the right lower limb persisted.
Patient perspective: the family was initially overwhelmed with fear and uncertainty. Their world had turned upside down as they watched their little one battle a life-threatening condition. They couldn�t help but feel a deep sense of helplessness and despair, especially when her condition worsened, leading to a convulsive status epilepticus. Upon seeing the positive changes in their daughter�s condition and she regained consciousness, the family was flooded with relief and gratitude. They were amazed by the resilience of their little one and the unwavering commitment of our hospital care and interventions, they were grateful for the excellent care their daughter received and for the chance to watch her grow and thrive once more.
Informed consent: an informed written consent was obtained from the patient�s family to publish this work.
Enterobacter cloacae is a gram-negative bacillus bacterium, belonging to the enterobacteriaceae family. It constitutes a part of the normal flora of the human gastrointestinal tract. Transmission primarily occurs through direct or indirect contact of mucous surfaces with the infectious agent. In the context of endogenous flora, transmission takes place through transfer to predisposed and sterile adjacent body regions. Additionally, it can also propagate through the fecal-oral route [1].
Meningitis caused by Enterobacter cloacae in adults and children represents a rare form of bacterial meningitis. It is frequently associated with nosocomial origins, with mortality rates ranging from 20% to 46%, and is rarely community-acquired. It usually occurs in the context of immunosuppression, following prolonged hospitalization, neurosurgical procedures, spinal anesthesia, lumbar punctures, or among patients with catheters [2].
In our case, no associated risk factors for E. cloacae were identified. Our patient was immunocompetent and had no history of recent hospitalization or surgical intervention. This suggests the hypothesis of self-infestation with bacteremia originating from an endogenous reservoir such as the gastrointestinal tract, urinary, and respiratory pathways. This dissemination could have extended to the meninges, thereby leading to the development of meningitis.
Regarding the treatment, third-generation cephalosporins are generally preferred for the treatment of gram-negative bacillus meningitis due to their broad spectrum of activity and effective penetration through the blood-brain barrier [3].
However, it is now being reported by numerous researchers that certain strains of gram-negative bacilli, notably Enterobacter cloacae, can develop resistance to third-generation cephalosporins as well as glycopeptides during the treatment. They may overexpress AmpC beta-lactamases through the derepression of a chromosomal gene or acquire a transferable ampC gene on plasmids, thereby conferring antibiotic resistance [4].
Several studies have demonstrated the effectiveness of antibiotic therapy using cefepime and carbapenems against enterobacteriaceae. Huang et al. [5], in a limited series of 10 patients, reported successful treatment of enterobacter meningitis with carbapenems. Other studies have also documented successful treatment of enterobacter meningitis cases using cefepime, imipenem in combination with amikacin, TMP-SMX in combination with gentamicin, and ciprofloxacin [6].
The rarity of community-acquired Enterobacter cloacae meningitis cases underscores the significance of carefully searching documented cases in the literature. Following a thorough research of existing reports, we have identified 5 distinct cases that offer interesting perspectives (Table 1).
In the first study conducted by Chang et al. [7], two cases of Enterobacter cloacae meningitis were presented: one in a 33-year-old woman and the other in a 30-year-old man. Although symptoms varied, both patients had fever, while only one of them developed hydrocephalus. It's worth noting that the second case had a history of post-traumatic intracerebral hemorrhage and already had a ventriculoperitoneal shunt in place. However, due to the infection's onset 90 days after initial discharge, it was considered community-acquired. The authors opted for intravenous chloramphenicol at a dosage of 4g per day in the first case, and intravenous ceftazidime at a dosage of 6g per day along with the insertion of a new ventriculoperitoneal shunt in the second case. Both patients responded favorably to treatment.
Maheshwari et al. [8] reported a case of a three-week-old term infant. The infant presented symptoms of lethargy and poor feeding. Initial CT of her brain showed evidence of severe hypoxia and herniation of the frontal lobes through the anterior fontanelle. Care was withdrawn 72 hours after admission, and a postmortem examination confirmed E. cloacae meningo-encephalitis as the cause of her death. Another interesting case of community-acquired E. cloacae meningitis, resulting in the formation of multiple brain abscesses, was documented by Saini et al. [9]. This report concerned a 10-year-old boy with no underlying risk factors, who presented with mild fever, headaches, photophobia, and meningeal signs. Brain magnetic resonance imaging revealed the presence of bilateral and multiple pyogenic abscesses. The patient was successfully treated with intravenous imipenem at a dose of 60 mg/kg/day, in addition to surgical drainage of the abscesses.
Furthermore, Kambourou et al. [10] described the case of a 6-year-old child admitted with seizure episodes, headaches, insomnia, and spontaneous vomiting. These symptoms were accompanied by febrile altered consciousness. Antibiotic therapy in this case consisted of the use of ciprofloxacin. The clinical evolution was favorable, and no sequelae were observed.
These cases reported in the literature, in conjunction with our case, demonstrate the variability of clinical manifestations and treatment responses in community-acquired Enterobacter cloacae meningitis. These cases also underscore the importance of choosing antibiotic options wisely, considering potential resistance and strain susceptibility. As well as rapid and targeted management to improve prognosis and minimize potential sequelae.
Enterobacter cloacae meningitis remains a rare form of community-acquired bacterial meningitis. As is the case with any meningitis etiology, this infection necessitates early and appropriate management to enhance prognosis and minimize the risk of complications and sequelae. The primary challenge lies in antibiotic usage, taking into consideration the potential development of resistance. Close patient monitoring is essential for the effective management of this potentially serious infection.
The authors declare no competing interests.
All the authors read and approved the final version of this manuscript.
Table 1: cases of community-acquired meningitis due to Enterobacter cloacae reported in the literature
Figure 1: (A,B,C) brain CT scan axial and coronal sequence: acute ischemic stroke in the superficial and deep territory of the middle cerebral artery with moderate hydrocephalus
- Sanders WE, Sanders CC. Enterobacter spp.: pathogens poised to flourish at the turn of the century. Clin Microbiol Rev. 1997;10(2):220-41. PubMed | Google Scholar
- Lin PC, Chiu NC, Li WC, Chi H, Hsu CH, Hung HY et al. Characteristics of nosocomial bacterial meningitis in children. J Microbiol Immunol Infect. 2004;37(1):35-8. PubMed | Google Scholar
- Donowitz GR, Mandell GL.. Drug therapy. Beta-lactam antibiotics (2). N Engl J Med. 1988 Feb 25;318(8):490-500. PubMed
- Choi SH, Lee JE, Park SJ, Choi SH, Lee SO, Jeong JY et al. Emergence of antibiotic resistance during therapy for infections caused by Enterobacteriaceae producing AmpC beta-lactamase: implications for antibiotic use. Antimicrob Agents Chemother. 2008;52(3):995-1000. PubMed | Google Scholar
- Huang CR, Lu CH, Chang WN. Adult Enterobacter meningitis: a high incidence of coinfection with other pathogens and frequent association with neurosurgical procedures. Infection. 2001;29(2):75-9. PubMed | Google Scholar
- Foster DR, Rhoney DH. Enterobacter meningitis: organism susceptibilities, antimicrobial therapy and related outcomes. Surg Neurol. 2005;63(6):533-7. PubMed | Google Scholar
- Chang WN, Lu CH, Huang CR, Chuang YC. Mixed infection in adult bacterial meningitis. Infection. 2000 Jan-Feb;28(1):8-12. PubMed | Google Scholar
- Maheshwari N, Shefler A. Enterobacter cloacae: an “ICU bug” causing community acquired necrotizing meningo-encephalitis. Eur J Pediatr. 2009;168(4):503-5. PubMed | Google Scholar
- Saini AG, Rathore V, Ahuja CK, Chhabra R, Vaidya PC, Singhi P. Multiple brain abscesses due to Enterobacter cloacae in an immune-competent child. J Infect Public Health. 2017;10(5):674-7. PubMed | Google Scholar
- Kambourou J, Engoba M, Ocko TLG, Okoko AR, Oko APG, Mamadoud ICN et al. Un cas de méningite communautaire à Enterobacter chez l'enfant au chu de Brazzaville. 2017. Accessed 30th October 2023.