Achalasia and its subtypes: a Moroccan cohort in Ibn Sina Hospital, Rabat
Yasmine Essadni, Ilham Serraj, Mouna Salihoun, Mohammed Acharki, Nawal Kabbaj
Corresponding author: Essadni Yasmine, Ibn Sina Hospital, Mohamed V University, Rabat, Morocco 
Received: 27 Dec 2023 - Accepted: 05 Mar 2024 - Published: 25 Mar 2024
Domain: Gastroenterology
Keywords: Achalasia, dysphagia, high-resolution esophageal manometry
©Yasmine Essadni et al. PAMJ Clinical Medicine (ISSN: 2707-2797). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Yasmine Essadni et al. Achalasia and its subtypes: a Moroccan cohort in Ibn Sina Hospital, Rabat. PAMJ Clinical Medicine. 2024;14:32. [doi: 10.11604/pamj-cm.2024.14.32.42519]
Available online at: https://www.clinical-medicine.panafrican-med-journal.com//content/article/14/32/full
Achalasia and its subtypes: a Moroccan cohort in Ibn Sina Hospital, Rabat
![]() Yasmine Essadni1,&, Ilham Serraj1, Mouna Salihoun1, Mohammed Acharki1, Nawal Kabbaj1
Yasmine Essadni1,&, Ilham Serraj1, Mouna Salihoun1, Mohammed Acharki1, Nawal Kabbaj1
&Corresponding author
Introduction: achalasia is an esophageal motility disorder, characterized by irregular peristalsis and inadequate relaxation of the lower esophageal sphincter, typically manifests with dysphagia as its primary symptom. The advent of high-resolution manometry (HRM) has transformed our comprehension of achalasia. It has delineated three distinct subtypes based on variations in pressurization and contractions, contributing significantly to the understanding of this condition. This study aimed to describe and compare clinically and manometrically the patients suffering from the different subtypes of achalasia.
Methods: it is a retrospective single-center study including all patients with achalasia diagnosed by high-resolution manometry (HRM) between April 2018 and January 2023. The diagnosis was retained based on the latest Chicago 3.0 classification.
Results: out of 103 patients, 25.2% (n=26) had type I achalasia, 66.9% (n=69) type II, and 7.8% (n=8) type III. Patients with type I and II achalasia were younger than patients with type III achalasia (mean age 43.2 years vs. 55.6 years, P=0.0053). A female predominance was found in type I achalasia and a male predominance in type III. The most frequent symptoms were: dysphagia (found in all our patients). At HRM, all our patients had a pathological IRP with a mean of 26.95 mmHg for the 3 types of achalasia. Resting IBS pressures were higher in patients with type III achalasia compared to types I and II (35.28 mmHg vs 32.7 mmHg and 31.04 mmHg, P=0.40).
Conclusion: achalasia is one of the most studied esophageal motility disorders. Tools such as HRM have permitted us not only to identify achalasia early but also to define different subtypes, which can have therapeutic implications.
Achalasia represents one of the primary and most prevalent motor disorders affecting the esophagus. It manifests as an esophageal condition marked by incomplete relaxation of the lower esophageal sphincter (LES) during swallowing, coupled with the absence of peristaltic contractions in the esophageal body [1]. Consequently, the passage of food into the stomach becomes hindered, leading to common symptoms such as dysphagia and regurgitation. Achalasia exhibits an estimated incidence ranging from 0.7 to 2.3 new cases per 100,000 individuals annually, with no discernible variations based on geography, race, or gender, though it appears to be more prevalent in older demographics. Despite its low incidence, the prevalence of achalasia is believed to be substantially higher, estimated to be approximately 10 times greater than its incidence, with approximately 10-23 individuals per 100,000 population affected by the disease [2,3].
Achalasia is characterized by the consistent destruction of myenteric ganglion cells in the LES region, yet the exact cause of this phenomenon remains largely elusive. Advancements in both the diagnosis and management of achalasia have been made over the past decade. The introduction of high-resolution manometry (HRM) has facilitated the development of new parameters for characterizing esophageal motility, including the integrated relaxation pressure of the LES, the distal contractile integral, and the distal latency. These parameters are integrated into the Chicago classification, which identifies three manometric subtypes of achalasia with significant prognostic and therapeutic implications. Our study aims to comprehensively describe and compare patients afflicted with different subtypes of achalasia, both clinically and manometrically.
Study design and setting: the present study consisted of a retrospective cohort study. It was carried out at the EFD-HGE Unit in Ibn Sina Hospital in Rabat, Morocco.
Study population: our research included patients with achalasia diagnosed by high-resolution manometry (HRM) between April 2018 and January 2023. 103 patients were included. Patients with other esophageal motor disorders and those previously treated for achalasia were excluded.
Data collection and definition: data were collected from the medical records of patients with a complete protocol of HRM including socio-demographic characteristics and clinical profiles of the patients. The parameters studied in HRM were: integrated relaxation pressure (IRP), resting pressure, and proportion of swallows with panesophageal pressurization. Note that an IRP greater than 21 mmHg was considered pathological. Patients already treated for achalasia were excluded from this study. We used a HRM unisensor catheter and the MMS 9.5 software for interpretation.
Statistical analysis: data were analyzed using Excel 2021 and then transported to JAMOVI for analysis. Demographic characteristics of the study subjects were analyzed descriptively. Categorical data was analyzed using frequencies (n) and percentages (%). Continuous data were analyzed using mean (SD) for normally distributed data or median (IQR) for skewed data. A two-sided P value of <0.05 was considered statistically significant.
Ethical considerations: approval was obtained from the Ethics Committee on Biomedical Research in Morocco. Observations remained anonymous and no patient information was disclosed to maintain privacy.
Socio-demographic characteristics: out of 316 HRM, 103 patients (32.6%) were included, of whom 60 (58.2%) were women. The mean age was 43.9 years (extremes 16 to 84 years) (Table 1).
Clinical characteristics: 25.2% (n=26) had type I achalasia, 66.9% (n=69) type II, and 7.8% (n=8) type III. Patients with type I and II achalasia were younger than patients with type III achalasia (mean age 43.2 years vs. 55.6 years, P=.0053). A female predominance was found in type I achalasia and a male predominance in type III (sex ratio M/F: 0.24 and 3.5 respectively). The most frequent symptoms were (without difference according to the 3 types): dysphagia (found in all our patients) in 100% of the cases, chest pain in 26.2% (n= 27) of cases, and regurgitation in 23.3% (n= 24) of cases. The average duration of symptoms was 13 months (range 1 to 32 months) (Table 2).
Endoscopic results: all patients had a fibroscopy before manometry showing: a sign of regurgitation in 34.9% (n=36) of cases, lower esophageal stricture in 14.6% (n=15), and normal endoscopy in 50.5% (n=52) of cases.
High-resolution manometry results: at HRM, all our patients had a pathological IRP with a mean of 26.95 mmHg for the 3 types of achalasia. Resting IBS pressures were higher in patients with type III achalasia compared to types I and II (35.28 mmHg vs 32.7 mmHg and 31.04 mmHg, P=40) (Table 3).
Our research revealed that Type II achalasia exhibited the highest prevalence among the studied cases. The average age at diagnosis was 43 years, with type I and II achalasia appearing to affect younger patients compared to type III achalasia. Type I achalasia displayed a female predominance. Interestingly, symptoms did not serve as reliable indicators to differentiate between the three types of achalasia, as our study found no discernible differences in symptoms among them. Furthermore, the comparison of pressure values in high-resolution manometry (HRM) revealed no significant distinctions among the three types of achalasia. In the literature, Achalasia´s occurrence is relatively rare, estimated at approximately 1.6 cases per 100,000 individuals [1], equally distributed between men and women, with no racial predilection, increasing with age, with a peak incidence between 30 and 60 years [1,2]. In most studies on achalasia, the mean age at diagnosis was around 50 years, similar to the present study [3]. The mean age of achalasia did not vary among achalasia [4].
Our study showed that patients with type III Achalasia seemed to be older at diagnosis. The pathophysiology of achalasia is only partially described. Achalasia is associated with dysfunction or degeneration of ganglion cells in the myenteric (Auerbach's) plexuses of the distal esophagus and LES [1,5]. The pathogenic mechanisms have a variable expression. They lead to a heterogeneous clinical expression, with a common point: absence of relaxation of the LES and absence of peristaltic esophageal contraction during swallowing [1,5]. Diagnosis of achalasia is relatively straightforward with a well-documented history, upper endoscopy, and esophageal motility test. The clinical manifestations of achalasia are numerous but non-specific. The classic revelatory sign of achalasia is dysphagia, which is present in about 95% of patients [6]. It is usually progressive, low, involving solids and liquids, intermittent and capricious. In our study, all the patients had dysphagia with these same characteristics. The second symptom in terms of frequency is represented by regurgitations (42% to 91%) secondary to esophageal stasis [7]. Heartburn, reported by 40-50% of patients, is an uncomfortable burning sensation behind the breastbone. Interestingly, in achalasia, this symptom doesn't arise from abnormal gastroesophageal reflux but rather from the stasis and food fermentation in the esophagus. This can lead to irritation and discomfort similar to heartburn.
However, this distinction is crucial because achalasia-related symptoms are often misdiagnosed as gastroesophageal reflux disease, leading patients to be treated with proton pump inhibitors (PPIs), which might not address the underlying issue, delaying the diagnosis [6,8]. Chest pain is another common symptom experienced by 19 to 79% of achalasia patients. This pain can vary in intensity and may be described differently among individuals. Its prevalence underscores the need for a thorough evaluation to differentiate achalasia from other conditions presenting with similar symptoms [9,10]. Achalasia can also lead to varying degrees of weight loss or nutritional deficiencies [11,12]. The study's groups, similar to Alvand's results, did not significantly differ when speaking of reported symptoms [4]. Whereas in Patel's study, chest pain was more prevalent in type III and weight loss in type I [13]. In our study, the average time to detection was 13 months, while Alvand's study's average time was 2 years, which is only half as long as Hassanzadeh's (4.9 years) [14]. The education of clinicians, the early referral of patients with dysphagia to gastroenterologists, and the improvement of HRM's accessibility can be the main reasons for this decrease.
In addition to careful questioning, diagnostic modalities include upper endoscopy, oeso-gastro-duodenal transit, and high-resolution manometry. Endoscopy with esophageal biopsies is used to rule out neoplastic or benign esophageal strictures. A suggestive aspect of achalasia-associated dilatation of the esophageal lumen, salivary or alimentary stasis, and a puckered gastroesophageal junction may be described but is absent in 40% of achalasia patients [1]. All of our patients had an upper endoscopy, and it was normal for half of them. Barium transit esophageal transit may reveal a classic megaesophagus appearance with a tapering oesogastric junction. The gold standard for confirming the diagnosis of achalasia is esophageal manometry. The introduction of the Chicago Classification (CC) v3.0 helped categorize esophageal motor disorders using high-resolution manometry. Additionally, it presents a standardized method for interpretation [5]. Achalasia is diagnosed if the residual pressure of the lower esophageal sphincter is greater than 15 mmHg, and if 100% of esophageal contractions are pathological [15]. Achalasia presents in three subtypes: Type I is diagnosed by an elevated median IRP and complete absence of contractility (100% failed peristalsis) (Figure 1). Type II shows abnormal median IRP, absent contractility (100% failed peristalsis), and panesophageal pressurization in at least 20% of swallows (Figure 2). Type III displays abnormal IRP, evidence of spasm (at least 20% swallows with premature contraction), and lacks evidence of peristalsis (Figure 3) [16].
Presently, the Chicago Classification version 4.0 is in use, establishing stricter criteria using specific protocols involving supine and upright positions alongside provocative maneuvers. Moreover, for inconclusive diagnoses on HRM, CC v4.0 strongly recommends supportive tests like timed barium esophagography (TBE) or endoluminal functional lumen imaging probe (FLIP) to help clinical decisions [11,17]. According to the Chicago classification, type II was shown to be the most prevalent type in the study conducted by Alvand (50%), followed by types I and III (37% and 12.9%, respectively) [4]. This was consistent with the American College of Gastroenterology report from 2020, which found that type II was the most prevalent form and made up between 50 to 70 percent of all achalasia patients [18]. This was also true in our study. Surdea-Blaga et al. study showed that the resting LES pressure (64.7±22.6 mmHg vs. 54.3±21.6 mmHg, p=0.019) and 4s-IRP (45.3±17.6 mmHg vs. 38.4±15.5 mmHg, p=0.036) were higher in type II compared to type I achalasia. In our study, type III seemed to have higher pressures, but the differences were insignificant [19]. The Chicago Classification impacts the choice of the initial approach for treating achalasia. Treatment options for achalasia encompass pharmaceutical, endoscopic, and surgical interventions. Typically, for types I and II, less invasive treatments like pneumatic dilatation prove effective, while type III often benefits more from oral endoscopic myotomy [20-22].
It's important to acknowledge several limitations inherent in this study that may impact its interpretation and applicability to broader contexts. Firstly, the study is based on data from a single center and primarily focuses on outpatient cases, potentially limiting the representation of diverse patient populations. Consequently, the findings may not fully encompass the range of cases seen in different healthcare settings. Furthermore, due to data availability constraints and the retrospective nature of the study, certain important clinical indicators such as quality of life assessments, evolution, and specific treatments chosen could not be included in the analysis. The absence of these variables may have resulted in the exclusion of potential confounding factors from the final statistical model. However, efforts were made to ensure the completeness of the model specification, thus providing reliable and valid estimates of association measure parameters. Additionally, the consistency of these results was cross-verified against findings from other studies to enhance their credibility.
Achalasia, among the extensively studied esophageal motility disorders, is defined by compromised LES relaxation and a lack of esophageal peristalsis. The subgrouping of achalasia types directly correlates with treatment outcomes, predicting positive responses to treatment. Our study, showed, that Type II achalasia was the most prevalent. The mean age of discovery was 43 years, and type I and II achalasia seemed to touch younger patients than type III achalasia. A female predominance was observed in type I achalasia. Symptoms couldn´t be used to distinguish the 3 types of achalasia as our study showed no differences in symptoms between the 3 types. The comparison of pressure values in HRM showed no significant difference between the 3 types of achalasia. Only demographic data can point to one type of this motility disorder. Thus, despite advancements in diagnostic techniques and treatment modalities, there is still much to uncover about the underlying mechanisms for this pathology and this comes with a better understanding of each type of Achalasia. Greater awareness among healthcare providers and the public is essential to facilitate early diagnosis and prompt intervention, ultimately enhancing the prognosis and well-being of individuals living with achalasia.
What is known about this topic
- Achalasia is one of the main and most frequent motor disorders of the esophagus;
- The diagnosis is made by high-resolution manometry that helped identify 3 subtypes of achalasia distinct by pressurization and contraction variations;
- Achalasia is equally distributed between men and women, with no racial predilection, increasing with age, and the mean age of achalasia was not various among achalasia types.
What this study adds
- This manuscript discusses the similarities and differences between the different types of achalasia to help understand this pathology and its subtleties better for the finest medical care;
- Patients with type I and II achalasia were younger than patients with type III achalasia. A female predominance was found in type I achalasia and a male predominance in type III. No differences on the clinical side between the different types of achalasia;
- It is the first work that studied Achalasia and compared its subtypes with HRM in North Africa.
The authors declare no competing interests.
Conception and study design: Yasmine Essadni, Ilham Serraj, Mohamed Acharki, Nawal Kabbaj. Data collection: Yasmine Essadni, Ilham Serraj. Data analysis and interpretation: Yasmine Essadni and Ilham Serraj. Manuscript drafting: Yasmine Essadni Manuscript revision: Yasmine Essadni, Ilham Serraj, Mouna Salihoun, Nawal Kabbaj. All authors approved the final version of the manuscript.
Table 1: demographic results according to the different types of achalasia
Table 2: clinical symptoms experienced by the patients in our study
Table 3: manometric results according to the different types of achalasia
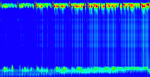
Figure 1: high-resolution manometry (HRM) image of type I achalasia: absence of contraction and pressurization
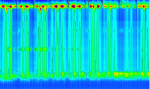
Figure 2: high-resolution manometry (HRM) image of type II achalasia: pan-oesophageal pressurization
Figure 3: high-resolution manometry (HRM) image of type III achalasia: more than 20% premature contractions
- Guillaumot MA, Barret M, Leblanc S, Leconte M, Dousset B, Oudjit A et al. Focus on Achalasia. Presse Med. 2018 Jan;47(1):11-18. PubMed | Google Scholar
- Sonnenberg A. Hospitalization for achalasia in the United States 1997-2006. Dig Dis Sci. 2009 Aug;54(8):1680-5. PubMed | Google Scholar
- Tanaka S, Abe H, Sato H, Shiwaku H, Minami H, Sato C et al. Frequency and clinical characteristics of special types of achalasia in Japan: A large-scale, multicenter database study. Journal of Gastroenterology and Hepatology. 2021;36(10):2828-2833. PubMed | Google Scholar
- Alvand S, Aghaee B, Momayez Sanat Z. Characteristics of Achalasia Subtypes: Result of a Study in a Tertiary Hospital. Caspian J Intern Med. 2022 Winter;13(1):100-106. PubMed | Google Scholar
- Sodikoff JB, Lo AA, Shetuni BB, Kahrilas PJ, Yang GY, Pandolfino JE. Histopathologic patterns among achalasia subtypes. Neurogastroenterol Motil. 2016 Jan;28(1):139-45. PubMed | Google Scholar
- Schlottmann F, Patti MG. Esophageal achalasia: current diagnosis and treatment. Expert Review of Gastroenterology & Hepatology. 2018;12(7):711-721. PubMed | Google Scholar
- Metman EH, Debbabi S, Negreanu L. Troubles moteurs de l´esophage, Encyclopédie medico-chirurgicale. Elsevier Ed. 2006;4:1-19. Google Scholar
- Jung DH, Park H. Is gastroesophageal reflux disease and achalasia\coincident or not. J Neurogastroenterol Motil. 2017;23(1):5-8. PubMed | Google Scholar
- Dunaway PM, Wong RKH. Achalasia. Curr Treat Options Gastroenterol. 2001;4(1):89-100. PubMed | Google Scholar
- Eckardt VF, Aignherr C, Bernhard G. Predictors of outcome in patients with achalasia treated by pneumatic dilation. Gastroenterology. 1992;103(6):1732-1738. PubMed | Google Scholar
- Vaezi MF, Pandolfino JE, Yadlapati RH, Greer KB, Kavitt RT. ACG Clinical Guidelines: Diagnosis and Management of Achalasia. American Journal of Gastroenterology. 2020;115(9):1393-1411. PubMed | Google Scholar
- Francis DL, Katzka DA. Achalasia: Update on the disease and its treatment. Gastroenterology. 2010;139(2):369-74. PubMed | Google Scholar
- Patel DA, Lappas BM, Vaezi MF. An overview of achalasia and its subtypes. Gastroenterol Hepatol (NY). 2017 Jul;13(7):411-421. PubMed | Google Scholar
- Hasanzadeh A, Mikaeli J, Elahi E. Demographic, clinical features and treatment outcomes in 700 achalasia patients in iran. Middle East J Dig Dis. 2010 Sep;2(2):91-6. PubMed | Google Scholar
- Eckardt VF. Clinical presentations and complications of achalasia. Gastrointest. Endosc Clin N Am. 2001 Apr;11(2):281-92, vi. PubMed | Google Scholar
- Kahrilas PJ, Bredenoord AJ, Fox M, Gyawali CP, Roman S, Smout AJ et al. The Chicago Classification of esophageal motility disorders, v3.0. Neurogastroenterol Motil. 2015 Feb;27(2):160-74. PubMed | Google Scholar
- Noh JH, Jung KW, Yoon IJ, Na HK, Ahn JY, Lee JH et al. Comparison of Diagnosis of Esophageal Motility Disorders by Chicago Classification Versions 3.0 and 4.0. J Neurogastroenterol Motil. 2023 Jul 30;29(3):326-334. PubMed | Google Scholar
- Yadlapati R, Kahrilas PJ, Fox MR, Bredenoord AJ, Prakash Gyawali C, Roman S et al. Esophageal motility disorders on highresolution manometry: Chicago classification version 4.0�. Neurogastroenterology and Motility. 2021;33(1):e14058. PubMed | Google Scholar
- Surdea-Blaga T, David L, Pop A, Tantau M, Dumitrascu DL. Clinical and Manometric Characteristics of Patients with Achalasia: One Disease with Three Presentations or Three Diseases with One Presentation. J Gastrointestin Liver Dis. 2020 Oct 27;29(4):501-508. PubMed | Google Scholar
- Laurino-Neto RM, Herbella F, Schlottmann F, Patti M. Evaluation of esophageal achalasia: from symptoms to the chicago classification. Arq Bras Cir Dig. 2018;31(2):e1376. PubMed | Google Scholar
- Herbella FA, Moura EG, Patti MG. Achalasia 2016: Treatment Alternatives. J Laparoendosc Adv Surg Tech A. 2017 Jan;27(1):6-11. PubMed | Google Scholar
- Pesce M, Pagliaro M, Sarnelli G, Sweis R. Modern Achalasia: Diagnosis, Classification, and Treatment. J Neurogastroenterol Motil. 2023 Oct 30;29(4):419-427. PubMed | Google Scholar