Implementing the elderly-friendly hospital initiative in the intensive care unit with a review of policy and practice
Osayomwanbo Osaheni, Obehi Aituaje Akoria, Darlington Ewaen Obaseki
Corresponding author: Osayomwanbo Osaheni, Anesthesiology Department, Intensive Care Team Lead, University of Benin Teaching Hospital Benin City, Edo State, Nigeria 
Received: 25 Jul 2021 - Accepted: 02 Sep 2023 - Published: 22 Jan 2024
Domain: Intensive care medicine
Keywords: Elderly, friendly, initiative, aging, intensive care unit
©Osayomwanbo Osaheni et al. PAMJ Clinical Medicine (ISSN: 2707-2797). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Osayomwanbo Osaheni et al. Implementing the elderly-friendly hospital initiative in the intensive care unit with a review of policy and practice. PAMJ Clinical Medicine. 2024;14:8. [doi: 10.11604/pamj-cm.2024.14.8.30921]
Available online at: https://www.clinical-medicine.panafrican-med-journal.com//content/article/14/8/full
Essay 
Implementing the elderly-friendly hospital initiative in the intensive care unit with a review of policy and practice
Implementing the elderly-friendly hospital initiative in the intensive care unit with a review of policy and practice
![]() Osayomwanbo Osaheni1,&, Obehi Aituaje Akoria2, Darlington Ewaen Obaseki3
Osayomwanbo Osaheni1,&, Obehi Aituaje Akoria2, Darlington Ewaen Obaseki3
&Corresponding author
Aging is an unavoidable part of life. Every human must go through the aging process. A decline in organ function is a part of the aging process that leads to various health-related challenges. These healthcare challenges may require critical care. The uniqueness of the aged population needs to be considered to provide adequate and satisfactory care befitting this subset of clients seeking critical care. Using the elder-friendly approach, improved care tailored to meet the demands of increased organ support can be achieved in the intensive care unit.
The specific onset of aging is uncertain and this has made the definite cut-off for the elderly difficult. It is generally agreed that the elderly consist of humans above 60 years of age [1]. This is the retirement age for civil servants in Nigeria. Although this definition is not synonymous with the point at which there is a marked decline in physiological function, it provides a global definition of the elderly for better communication. Associated with aging is a reduction in physiological functions. This could impact negatively the state of physical, mental, and emotional wellbeing even in the absence of ill health [2]. Conversely, illness can overstretch the health status of the elderly patient. If elderly patients´ physiological needs are not taken into consideration during their care, there could be far-reaching adverse financial implications, and individual and family stress. The older person´s self-esteem, self-determination, and independence could also be seriously affected.
Elderly patients are more likely to need in-hospital and intensive care unit care than others. About 12.6% of the patients admitted into the intensive care unit of the University of Benin Teaching Hospital, Nigeria are elderly [3]. One-third of the frail elderly patients admitted into hospital lose their ability to perform activities of daily living [4,5]. The implication for policymaking is to proactively develop elder-friendly intensive care units that will cater to the elderly population [6]. Intensive care is an expensive project. Ideally, if the resources are available, there should be a geriatric-specific intensive care unit that is fully oriented toward caring for elderly patients. Nevertheless, the orientation of health workers within any Intensive Care Unit (ICU) towards the provision of an elder-friendly environment will no doubt improve the chances of wholesome recovery [6].
Policy targets for elder-friendly intensive care units: for appropriate policy implementation, the framework, guidelines, and challenges that could mitigate the implementation of policies, especially in low-resource settings need to be reviewed.
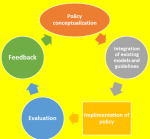
Framework review: setting up a successful elder-friendly initiative for ICUs requires a holistic approach. Although there is no specific framework or guideline for implementing elder-friendly initiatives in the intensive care unit some recommendations exist that could be adapted to suit the care for the critically ill elders [7]. For example, the Hospital Elder Life Program (HELP) focuses on the prevention of delirium, functional decline in hospitalized older adults, early mobilization, and cognitive function. The Nurses Improving Care for Health-system Elders (NICHE) program framework concentrates on improving communication, and staff education. The comprehensive design model described by the Acute Care for Elders (ACE) model also exists. Person-centered care focuses on the patients and their individualized needs. Weaving these frameworks of care closely within existing guidelines is essential in implementing senior intensive care units in low-income settings [8-13] (Figure 1).
Incorporation of guidelines: other aspects to consider in the implementation of elder-friendly ethos in intensive care units is a review of existing guidelines or recommendations on key care areas like the holistic care of the elderly. Holistic management of elderly syndrome entails regular comprehensive assessment of both the cognitive, psychomotor, and psycho-social functions to identify potential, actual needs or risks; provide emotional support, and encourage participation with environmental consideration. Environmental considerations would include, for example, adequate lighting, noise reduction, and clear signage [14]. Early mobilization is necessary; equally important is the need for the elderly to have adequate sleep. This can be done by deliberating integrating care provided by multiple practitioners in such a way that frequent interruptions are reduced. Guidelines for mobility and rehabilitation will include speech therapy for early functional recovery.
The healthcare worker in the intensive care unit has to be aware of the potential for a fall. Beds used to care for older patients should be low and have bed rails. The floor tiles should be non-slip. Senior care management with emphasis on the “4 Ms”: matters most, mobility, medications, and mentation should be considered and implemented. The use of the ABCDEF critical care bundle would also improve ICU care and outcomes for older persons: assess, prevent, and manage pain; both spontaneous awakening trials and spontaneous breathing trials, choice of analgesia and sedation; assess, prevent, and manage delirium; early mobilization and exercise; family engagement and empowerment. Frailty and agitation sedation scores assessment would also reduce delirium which is a major challenge in hospitalized older persons [8,15-19]. Palliative care principles recommendations should also be integrated to achieve elder-friendly intensive care units, especially for patients who require end-of-life care, being worked up for transfer to palliative care units. Palliative care principles include the provision of pain-free management, communication of care goals, psychosocial support, and symptomatic management of complaints [18,20]. Importantly, periodic evaluation would ensure continuous quality improvement. Regular review of care outcomes, patient and family satisfaction, and peer review of clinical care are also recommended in the guidelines. It is important to note that guidelines should be gleaned, adopted, or adapted in the context of specific institutional or organizational needs and available resources. This is especially pertinent in low-resource settings.
Location of the intensive care: if possible, the intensive care should be located in an area that is easily accessible to the geriatric ward. It could actually be fashioned out of a geriatrics ward [21]. Beautifully designed attractive walls; curtains, window blinds, slip-free floors, and netted windows should be prioritized to achieve a geriatric-friendly intensive care unit. There could be colored shuttle services that convey ill older persons through smooth pavements to the unit from the emergency room or surgical suite.
Admission and nursing care in the ICU: early admission and prompt management of the elderly patient in the intensive care unit could prevent deterioration. Modified early warning scores can be an effective policy tool in triaging elderly patients who need intensive care or for monitoring daily progress in the intensive care unit. Ill senior elders (i.e. elderly patients above the age of 80 years) are a unique category with self-esteem. Some may experience cognitive dysfunction including memory loss, limited self-care, altered sleep patterns, and comorbidities. Specialized nursing care is required. One elder per nurse ratio is the least expected for adequate nursing care. The ill elder should be assisted as much as possible with understanding and patience in the performance of those routine functions that cannot be performed unaided. Any assistance should be provided in such a way as to aid full recovery and return the elder to complete independence or at least to baseline functional status, if possible. Physical care that may be required includes bed baths, oral care, perineum care, pressure area care, provision of range of motion exercises, early mobilization to prevent deep venous thrombosis, care of indwelling catheters, drains care, and judicious recording of intake and output. Such care should be executed in a coordinated manner to allow adequate time for the patient to sleep and rest. The use of nightshade in an open ICU could encourage sleep and should be considered. Engaging the elderly patient in discussion also helps maintain their mental integrity. It is important to always introduce the team member once at the bedside of the elderly patient and the procedure that is to be carried out should be explained in plain terms. The time and the day of the week should be announced every day. These interventions will help in maintaining and improving the cognitive function of elderly patients who may forget the time or day of the week with a continuous stay in intensive care where lights are on both day and night. Medication dosing should be planned with due consideration to alterations in pharmacokinetics and pharmacodynamics. Drug interactions (drug-drug, drug-disease, and drug-food) should also be proactively considered and mitigated. Every effort should be made to reduce unnecessary polypharmacy.
Communication: effective communication among team members, with the elder and family is essential. When relating with the elder the team should ensure that there is no hearing impairment. Every effort should be made to ensure that the elder understands the discussions. Adequate vision and hearing aids should be provided as required. Adequate time should be allowed for the senior to think things through before making informed decisions on any treatment plan. The patient and Family-Centered Care approach is integral to the holistic care of the elderly in the intensive care unit.
Family involvement: the patient and family should be involved in care, decision-making processes, care planning, and setting of treatment goals. Their preferences and values should be incorporated into all care processes. Care protocols, visit hours, personal protective wear, need for infection prevention, and cost of ICU admission should be explained during the review for admission of the elderly into the intensive care unit. Regular family conferences and updates on the progress of patients should be ensured. The family should know about long-term specialized care if necessary, and should be incorporated into how it can be provided and sustained. Arrangements to provide end-of-life support for the terminally ill elder should be made during such family briefings [22].
Multidisciplinary care, physiotherapy, health education: a multidisciplinary team made of health care professionals including the intensivist, geriatrician, physiotherapist, internist, and nurses is needed in caring for elders. One nurse to a ventilated patient is required [23,24]. The elderly usually have diverse systemic manifestations of aging that require collaboration of team members in care provision. For example, the elderly patient may have comorbidities that require the coordinated input of various medical specialists. The physiotherapist should be involved early in patient care. Enteral feeding is a preferred option for feeding whenever possible. However, the unconscious elderly patient may require nasogastric feeding. The nutritionist and dentist should be involved in feeding and oral care. The elderly patient could be on multiple therapies. Education about the use of mobile applications and mobile sensors that can monitor physical exercise, sense and report health indices like blood pressure, and pulse rate, and provide reminders on drug adherence should be provided while in the unit and before transfer out of the unit [9].
Training of staff: regular training of health workers is necessary to provide desired orientation and quality care. Training can be in the form of updates, seminars, clinical meetings, ward reviews, and peer reviews of performance.
Challenges: implementing elder-friendly initiatives in critical care units in low-resource countries could be challenging. Accessing health care could be daunting because of transportation costs, long distances to health care facilities, absence of motorable roads, out-of-pocket payments for health services, etc. This is amidst negative stereotypes of cultural perceptions and social norms about the sick elderly. The elderly patient is often undervalued in some communities. Cultural and communication gaps also create delays in older persons accessing prompt care. For example, their ill health may be attributed to evil forces or spiritual misdemeanors, possession by evil spirits that require exorcism and prayer rather than critical care. Most elders no longer work. They usually cannot provide resources for their own regular care, not to talk about intensive unit care, which could be a huge bundle of healthcare costs for seniors. Some elders may not be able to access their meager retirement funds, which often lag behind inflation. Thus, many are absolutely at the mercy of their children, if they have any, family members or other Good Samaritans, who themselves have other pressing life challenges. Furthermore, navigating the healthcare system requires multiple processes that are tiring and strenuous for the elderly patient. Points of payment, laboratory investigations, consultation rooms, and pharmacies are wide apart and energy-sapping to transverse [25-27].
Underfunding because of limited or poorly allocated resources leads to inadequate infrastructure, staffing, and medical equipment. Specialized beds, assistive devices, monitoring, and other equipment required for the care of older persons are largely lacking. Training of healthcare personnel on care for the elderly is usually not considered a priority. Health facilities may lack comprehensive care, protocols, and guidelines for the elderly in the critical care unit. Data on geriatric care outcomes, guidelines, and protocol implementations are not available. Nevertheless, the potential solutions may lie in public-private partnerships, collaboration with international donors and funding agencies, prioritizing the training of healthcare and allied personnel in elder care, and consciously investing in improving infrastructure with the goal of deliberate inclusion of the elderly in healthcare improvement efforts [12,18,20,27-30]. These challenges are summarized in Table 1 below.
Up to a quarter of the patients requiring intensive unit care in hospitals are elderly patients with unique physiological and healthcare needs. In order to meet these needs, a policy-guided orientation of ICU care is needed. These policies should integrate the physiological needs of the patient with their daily care in an elder-friendly service delivery approach that makes the intensive unit care a pleasant and safe environment for the elderly ill patient.
The authors declare no competing interests.
Osayomwanbo Osaheni: conceptualized, did a literature search, and drafted the manuscript. Obehi Aituaje Akoria was involved in the conceptualization, and review of the draft manuscript while Darlington Ewaen Obaseki was involved in the conceptualization, revision, and final approval of the manuscript for publication. All the authors have read and agreed to the final manuscript.
We are grateful to the management of the University of Benin Teaching Hospital for the continuous motivation of staff towards the provision of quality care.
Table 1: challenges of implementing elder-friendly intensive care unit in low resource setting and suggested solutions
Figure 1: elderly friendly implementation framework
- Orimo H, Ito H, Suzuki T, Araki A, Hosoi T, Sawabe M. Reviewing the definition of “elderly”. Geriatr Gerontol Int. 2006;6(3):149-158. Google Scholar
- Sartorius N. The Meanings of Health and its Promotion. Croat Med J. 2006;47(4):662. PubMed | Google Scholar
- Tobi KU, Ndokwu EO, Edomwonyi NP. Characteristics of Critically Ill Elderly Patients Admitted to a Tertiary Intensive Care Unit in Nigeria and Outcome of Management. Glob Anesth Perioper Med. 2017;2(5):223-225. PubMed | Google Scholar
- Lankoandé M, Bonkoungou P, Simporé A, Somda G, Kabore RAF. Inhospital outcome of elderly patients in an intensive care unit in a Sub-Saharan hospital. BMC Anesthesiol. 2018;18(1):1-6. PubMed | Google Scholar
- Huang AR, Larente N, Morais JA. Moving Towards the Age-friendly Hospital: A Paradigm Shift for the Hospital-based Care of the Elderly. Can Geriatr J CGJ. 2011;14(4):100-103. PubMed | Google Scholar
- Kim YS, Han SH, Hwang JH, Park JM, Lee J, Choi J et al. Development of the Korean framework for senior-friendly hospitals: a Delphi study. BMC Health Serv Res. 2017 Aug 4;17(1):528. PubMed | Google Scholar
- Harnett PJ, Kennelly S, Williams P. A 10 step framework to implement integrated care for older persons. Ageing International. 2020 Sep;45(3):288-304. Google Scholar
- Cleveland J. Acute Care for Elders units: a model from the past or for the future. J Am Geriatr Soc. 2022;70(10):2758-2760. PubMed | Google Scholar
- Malone ML, Capezuti EA, Palmer RM, editors. Acute care for elders: a model for interdisciplinary care. Springer; 2014 Jul 21. Google Scholar
- Hshieh TT, Yang T, Gartaganis SL, Yue J, Inouye SK. Hospital Elder Life Program: Systematic Review and Meta-analysis of Effectiveness. Am J Geriatr Psychiatry. 2018;26(10):1015-1033. PubMed | Google Scholar
- Capezuti E, Brush BL. Implementing Geriatric Care Models: What Are We Waiting For. Geriatr Nur (Lond). 2009;30(3):204-206. PubMed | Google Scholar
- Hendrix CC, Matters L, West Y, Stewart B, McConnell ES. The Duke-NICHE Program: An academic-practice collaboration to enhance geriatric nursing care. Nurs Outlook. 2011;59(3):149-157. PubMed | Google Scholar
- Allen J, Close J. The NICHE Geriatric Resource Nurse Model: Improving the Care of Older Adults with Alzheimer´s Disease and Other Dementias. Geriatr Nur (Lond). 2010;31(2):128-132. PubMed | Google Scholar
- Valentin A, Ferdinande P, ESICM Working Group on Quality Improvement. Recommendations on basic requirements for intensive care units: structural and organizational aspects. Intensive care medicine. 2011 Oct;37:1575-87. Google Scholar
- Mate K, Fulmer T, Pelton L, Berman A, Bonner A, Huang W et al. Evidence for the 4Ms: Interactions and Outcomes across the Care Continuum. J Aging Health. 2021;33(7-8):469-481. PubMed | Google Scholar
- Geen O, Rochwerg B, Wang XM. Optimizing care for critically ill older adults. CMAJ Can Med Assoc J J Assoc Medicale Can. 2021;193(39):E1525-E1533. PubMed | Google Scholar
- Fulmer T, Reuben DB, Auerbach J, Fick DM, Galambos C, Johnson KS. Actualizing Better Health And Health Care For Older Adults. Health Aff (Millwood). 2021;40(2):219-225. PubMed | Google Scholar
- Ebrahimi Z, Patel H, Wijk H, Ekman I, Olaya-Contreras P. A systematic review on implementation of person-centered care interventions for older people in out-of-hospital settings. Geriatr Nur (Lond). 2021;42(1):213-224. PubMed | Google Scholar
- Tran K, Wright M-D. Senior friendly hospital care: A review of guidelines. Ottawa (ON): Canadian Agency for Drugs and Technologies in Health; 2019 Feb 28. PubMed | Google Scholar
- Heydari A, Sharifi M, Moghaddam AB. Challenges and barriers to providing care to older adult patients in the intensive care unit: a qualitative research. Open Access Macedonian Journal of Medical Sciences. 2019 Nov 11;7(21):3682. Google Scholar
- Osaheni O, Tabowe BT, Tobi KU IH. Intensive care unit set up in low resource countries: an overview of basic essentials. NDJMS. 2019;2(1):15 - 21. Google Scholar
- Boltz M, Capezuti E, Bowar-Ferres S, Norman R, Secic M, Kim H et al. Changes in the Geriatric Care Environment Associated with NICHE (Nurses Improving Care for HealthSystem Elders). Geriatr Nur (Lond). 2008;29(3):176-185. PubMed | Google Scholar
- Jin Z, Jovaisa T, Thomas B, Phull M. Intensive care unit staffing during the periods of fluctuating bed occupancy: An alternative dynamic model. Intensive Crit Care Nurs. 2021;66:103063. PubMed | Google Scholar
- Falk AC. Nurse staffing levels in critical care: The impact of patient characteristics. Nurs Crit Care. 2023;28(2):281-287. PubMed | Google Scholar
- Malelelo-Ndou H, Ramathuba DU, Netshisaulu KG. Challenges experienced by health care professionals working in resource-poor intensive care settings in the Limpopo province of South Africa. Curationis. 2019;42(1):1921. PubMed | Google Scholar
- Atakro CA, Atakro A, Aboagye JS, Blay AA, Addo SB, Agyare DF et al. Older people´s challenges and expectations of healthcare in Ghana: A qualitative study. PloS One. 2021;16(1):e0245451. PubMed | Google Scholar
- Nguyen Y-L, Angus DC, Boumendil A, Guidet B. The challenge of admitting the very elderly to intensive care. Ann Intensive Care. 2011 Aug 1;1(1):29. PubMed | Google Scholar
- Tanyi PL, André P, Mbah P. Care of the elderly in Nigeria: Implications for policy. Cogent Soc Sci. 2018;4(1):1555201. Google Scholar
- Heckman GA. Integrated care for the frail elderly. Healthc Pap. 2011;11(1):62-68; discussion 86-91. PubMed | Google Scholar
- Capezuti E, Boltz M, Cline D, Dickson VV, Rosenberg M, Wagner L et al. Nurses Improving Care for Healthsystem Elders - a model for optimising the geriatric nursing practice environment. J Clin Nurs. 2012;21(21-22):3117-3125. PubMed | Google Scholar