Successful endovascular limb salvage revascularization in a patient with chronic total occlusion of the superficial femoral artery in Nigeria: a case report
Olurotimi Badero, Bamikole Osibowale, Adebola Oluwabusayo Adetiloye
Corresponding author: Olurotimi Badero, Department of Interventional Cardiology, Iwosan Lagoon Hospitals, Victoria Island, Lagos, Nigeria 
Received: 17 Apr 2024 - Accepted: 27 May 2024 - Published: 31 May 2024
Domain: Cardiology
Keywords: Endovascular procedure, arterial occlusive disease, limb salvage, femoral arteries, case report
©Olurotimi Badero et al. PAMJ Clinical Medicine (ISSN: 2707-2797). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Olurotimi Badero et al. Successful endovascular limb salvage revascularization in a patient with chronic total occlusion of the superficial femoral artery in Nigeria: a case report. PAMJ Clinical Medicine. 2024;15:12. [doi: 10.11604/pamj-cm.2024.15.12.43675]
Available online at: https://www.clinical-medicine.panafrican-med-journal.com//content/article/15/12/full
Case report 
Successful endovascular limb salvage revascularization in a patient with chronic total occlusion of the superficial femoral artery in Nigeria: a case report
Successful endovascular limb salvage revascularization in a patient with chronic total occlusion of the superficial femoral artery in Nigeria: case report
![]() Olurotimi Badero1,&, Bamikole Osibowale1,
Olurotimi Badero1,&, Bamikole Osibowale1, ![]() Adebola Oluwabusayo Adetiloye2
Adebola Oluwabusayo Adetiloye2
&Corresponding author
The burden of peripheral arterial disease (PAD) is huge and carries a risk of limb amputation if not well managed. Endovascular revascularization technique has become a treatment option; however, its accessibility is currently hindered by a range of multi-dimensional challenges. We report here a case of a middle-aged man with type 2 diabetes mellitus (DM) who presented with critical limb ischemia, found to have chronic total occlusion (CTO) of the superficial femoral artery and had endovascular revascularization with balloon angioplasty and stenting for limb salvage with no residual stenosis. This is the first reported case of critical limb ischemia of the lower extremity with chronic total occlusion treated successfully with endovascular technique in Nigeria. PAD with critically limb ischemia can be effectively managed in Nigeria using endovascular non-surgical techniques with reduction in limb amputation rates.
Endovascular revascularization technique is a minimally invasive treatment option for peripheral arterial disease, but it is not readily available in most cardiovascular centers in Nigeria due to cost, lack of expertise and facilities for such procedures [1]. Peripheral arterial disease (PAD) constitutes a significant cardiovascular morbidity globally and it has emerged as a major cause of lower extremity amputation in Nigeria [1-3]. There are studies that suggest the burden of PAD in sub-Saharan Africa may be as high as that of developed countries but rather underdiagnosed and undertreated [1,2]. Furthermore, a number of these cases end up with avoidable limb amputations [4]. Treating chronic total occlusion (CTO) in peripheral arterial disease (PAD) with endovascular interventions can be challenging unless advanced technological devices are utilized to navigate lengthy occlusions. The complexity and failure to cross the occlusion may necessitate consideration for surgical intervention [5]. With the advent of advanced peripheral vascular imaging techniques in Nigeria with endovascular intervention, it is hoped that the amputation rate will decrease with improved morbidity and mortality of PAD patients. Here we report a case of symptomatic superficial femoral artery (SFA) CTO with critical limb ischemia treated with balloon angioplasty and stenting with no residual stenosis in a Nigerian Male.
Patient information: a 62-year-old man with multiple comorbidities including long-standing type 2 diabetes mellitus (DM), hypertension, dyslipidemia, coronary artery disease, and chronic kidney disease (stage 3a) presented to the cardiology clinic with critical limb ischemia of the left lower extremity with worsening ischemic rest pain for over six months. Symptoms initially began with lifestyle limiting of less than a block, with gradual worsening to ischemic rest pain of the left lower limb at rest in the preceding six months. No leg ulcer was reported. He gave a history of recurrent leg swelling but had no dyspnea, orthopnea, or paroxysmal nocturnal dyspnea. The patient had failed a structured exercise program with worsening symptoms despite optimal medical therapy, and was subsequently referred for further evaluation. Outpatient medications include amlodipine/valsartan 10/160 mg daily, subcutaneous insulin 14 I.U. a.m. and 8 I.U. p.m., atorvastatin 20 mg, clopidogrel 75 mg daily and cilostazol 100 mg twice daily.
Clinical findings: physical examination revealed a well-nourished male in no painful or respiratory distress. His vitals were all within normal limits. Lower extremity examination was remarkable for absent dorsalis pedis and posterior tibial pulses bilaterally.
Diagnostic and assessment: computerized tomography angiography (CTA) obtained at the referring center showed left superficial femoral artery (SFA) chronic total occlusion (CTO) reconstituting at the popliteal region via collaterals from the deep femoral artery (DFA) with single vessel run-off via posterior tibial (PT) artery which was diffusely diseased. Anterior tibial and peroneal arteries were occluded bilaterally. Laboratory results revealed; prothrombin time of 12.8s (normal range: 10-14s), international normalized ratio was 1.0 (normal range: 0.7-1.2), electrolytes, urea and creatinine showed sodium of 140 mmol/L (normal range: 135-145 mmol/L), potassium of 4.9 mmol/L (normal range: 3.5-5.0 mmol/L), chloride of 106 mmol/L (normal range: 98-105 mmol/L), bicarbonate of 27 mmol/L (normal range: 20-30 mmol/L), urea of 69 mmol (normal range: 10-5 5 mmol/L), creatinine 1.8 mg/dl (normal range: 0.6-1.1 mg/L), haemoglobin:12.6 g/dl (normal range: 12.0-16.0), hematocrit of 41.5% (normal range: 36-46%), WBC: 6,260/mm3 (normal range: 4,000-11,000/mm3), platelet count 308,000/mm3 (normal range: 150,00-400,000/mm3).
Diagnosis: a diagnosis of Rutherford stage 4 ischemic rest pain with abnormal CTA was made, and the patient was planned for abdominal aortogram, bilateral femoral run-off with possible endovascular revascularization.
Therapeutic interventions: in the cardiac catheterization lab, the patient was pre-treated with normal saline to prevent contrast media-induced nephropathy, prepped, and draped in the usual sterile fashion. After administration of conscious sedation with 1% lidocaine local anesthesia, arterial access was obtained, and a 5-Fr sheath was placed in the right common femoral artery. A 4-Fr modified hook catheter was advanced over a 0.035 advantage wire and placed in the abdominal aorta and an abdominal aortogram was performed revealing: patent normal renal arteries and abdominal aorta. The common, internal, and external iliac arteries were moderately calcified without significant stenoses. A right lower extremity angiogram was performed via the sheath. A left lower extremity angiogram was performed via selective contralateral catheter placement in the SFA. Lower extremity angiogram revealed patent bilateral common and deep femoral arteries, with occluded proximal left superficial femoral artery reconstituting in the P2 segment of the popliteal artery via collaterals from the left profunda femoris artery. There was a flow-limiting dissection of the left popliteal artery, with occluded left anterior tibial and peroneal arteries. There was a single vessel run-off to the left foot via the left posterior tibial artery, which had significant diffuse disease. On the right, there was mild right superficial femoral artery stenosis, and patent right popliteal and tibia-peroneal trunk arteries. The right anterior tibial and peroneal arteries were occluded. Run-off to the right leg was via the right posterior tibial artery which was occluded proximally reconstituting via collaterals from the right tibial peroneal trunk.
The decision was made to revascularize the left SFA CTO, popliteal, and posterior tibial arteries. Following standard anticoagulation, the 5-Fr sheath was exchanged for a 65 cm 7-Fr destination sheath placed in the left superficial femoral artery. The left superficial femoral artery CTO was crossed successfully with a 4-French angled navicross catheter and the 0.035 advantage wire. A quick angiogram via the navicross catheter confirmed intraluminal position. The navicross catheter was then exchanged for a 0.014 quick cross-support catheter and the left posterior tibial artery stenosis was crossed with a 0.014 PT choice wire and the quick cross-support catheter. The wire was placed in the distal left posterior tibial artery. Balloon angioplasty of the left superficial femoral artery was performed with a 6.0 x 100 mm balloon inflated to nominal pressure for 3 minutes. The superficial femoral artery was then stented with 6.0 x 100 mm self-expanding stents. The stents were post-dilated with the 6.0 x 100 mm balloon inflated to nominal pressures for 30 seconds. Repeat angiogram demonstrated good angiographic results with 0% residual stenosis and brisk flow in the vessel. The flow-limiting dissection of the left popliteal artery was stented with a 6.0 x 80 mm self-expanding stent. The stent was post-dilated with the 6.0 x 80 balloon. Repeat angiogram demonstrated good angiographic results with 0 percent residual stenosis and brisk flow in the vessel. The distal left popliteal artery stenosis was treated with balloon angioplasty using a 4.0 x 60 mm balloon inflated to 12 atmospheres (ATM) for 3 minutes. The left peroneal, anterior, and posterior tibial arteries were also revascularized with balloon angioplasty. Repeat angiogram demonstrated good angiographic results with 0 percent residual stenosis and brisk flow in the vessel. The arteriotomy site was sealed with a closure device. His left dorsalis pedis pulse was now palpable. He was discharged home the next day on Xarelto 2.5 mg twice daily, aspirin 81mg daily, and atorvastatin 40 mg daily in addition to his previous home medications.
Follow-up and outcome of interventions: patient´s symptoms improved significantly with increased walking distance and performance on outpatient follow-up. He continued with his structured outpatient exercise program and medications.
Patient perspective: this case exemplifies the importance of early recognition of an urgent, threatening medical condition with prompt referral which led to a favorable outcome. The patient sent a follow-up e-mail stating that he continues to remain pain-free. He reports being able to walk long distances now with no limitation and no pain. He is very happy with his results. “I was having pain in my legs for some time and after some years my legs feel heavy. I was put on many drugs with no improvement. I was told I would need my legs cut off eventually. I heard of a doctor coming from the US to help people with my condition without surgery. I was referred to the hospital and my leg was worked on, and blood started flowing again. I can now feel my legs and walk around normally. I consider myself lucky to not have my leg cut off”.
Informed consent: an informed consent was obtained from the patient.
Peripheral arterial disease (PAD) is a disease condition characterized by the narrowing of branches of the aorta excluding cerebral and coronary arteries. It is regarded as the third most common cause of cardiovascular morbidity globally [6]. The burden in both developed and developing countries is similar, though underdiagnosed and undertreated in Nigeria [6,7]. Multiple risk factors, such as cigarette smoking, diabetes mellitus, previous coronary artery disease, and a sedentary lifestyle, have been linked to peripheral arterial disease. Peripheral arterial disease is chiefly influenced by advancing atherosclerotic disease, leading to diminished blood flow to major organs and resultant end-organ ischemia. The progression of atherosclerosis is highly intricate, encompassing a multifaceted interplay among different cells, proteins, and pathways within the vascular system. This intricate biological process involves a series of dynamic events that contribute to the development and progression of atherosclerotic plaques. Cells such as endothelial cells, smooth muscle cells, and immune cells play crucial roles, interacting with various proteins and signaling pathways. Endovascular peripheral percutaneous intervention is a minimally invasive treatment option for advanced symptomatic PAD with good outcomes, but it is non-existent in many parts of the country for many reasons. Firstly, there are few interventional cardiology experts in West Africa, including Nigeria, and not all are trained in peripheral interventions. Secondly, the needed equipment and devices are not readily accessible. In addition, cost implications are huge, hence, many patients with significant PAD end up with avoidable limb amputations.
Chronic total occlusion is defined as complete occlusion of a vessel with the absence of antegrade flow through the lesion with a presumed or documented at least 3 months. It is a common finding in over 40% of PAD patients [8]. It is also a complex disease with variable morphological characteristics and treatment is quite challenging, therefore, care must be individualized. Chronic total occlusions of the SFA are common among patients with chronic PAD often presenting with intermittent claudication that eventually progresses to ischaemic rest pain as seen in our case [9]. Traditionally, CTOs were either managed medically or surgically due to difficulty with recanalization. Current guideline recommends that symptomatic patients with isolated CTO of the SFA Rutherford classes 1, 2, and 3 claudication should be managed conservatively using risk factor modification, structured exercise program, and medications. However, Rutherford class 4 ischemic rest pain as seen in our case should have endovascular revascularization if the CTO has favorable characteristics, including a short length of less than 10 cm. The past three decades have witnessed significant advancements in the treatment of complex PAD with the development of lesion-crossing devices and techniques.
Arterial access is typically achieved through contralateral arterial access of the common femoral artery as done in our case, however, factors such as abdominal aortic aneurysm repair, iliac artery tortuosity, severe aorto-iliac femoral occlusive disease, obesity, trauma, scarring, and hematoma may preclude its use necessitating other viable alternatives such as radial, brachial, popliteal, and pedal access. In our case, the contralateral arterial access strategy was utilized with no difficulty. Two main strategies are usually employed in the endovascular treatment of peripheral CTOs: a primary wire approach or the use of a CTO recanalization device [10]. The primary wire approach is particularly challenging and has an attendant risk of dissection and embolization. Saminathan et al. reported no difference in acute procedural success between the two treatment strategies [10] In our case, a primary wire approach was used with good outcomes. An important limitation of endovascular revascularization is failure to cross the true lumen. This may be due to difficulty with keeping the wire in the lumen, heavy calcifications, and the presence of collaterals at the occlusion site.
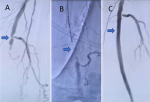
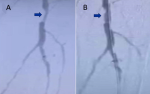
Our case demonstrates an outstanding outcome, with Figure 1 revealing no residual stenosis in the left SFA. The patient also experienced prompt and complete resolution of his symptoms. Figure 2 shows pre- and post-interventional images of the left popliteal artery. The full complement of advanced devices such as rotational devices, high-frequency vibration, blunt microdissection, rotational guidewire, guided approaches using optical coherence tomography or radiofrequency, and facilitated low-profile crossing technology, may not be available in resource-poor settings. Despite this limitation due to the unavailability of adequate resources, revascularization with no residual stenosis is achievable with the requisite skill set, as seen in our case.
Critical limb ischemia is an urgent and potentially devastating condition that left untreated can lead to non-healing ulcers, gangrene, and amputation of the affected limb. The increasing incidence of peripheral arterial disease in Nigeria from the availability of advanced imaging modalities, mandates that the medical community be aware of non-surgical limb salvage treatment options that are locally available to patients. Our patient, with this condition, was able to take advantage of this locally available emerging technology and expertise, preserving his limb and functionality.
The authors declare no competing interests.
Patient management: Olurotimi Badero and Bamikole Osibowale. Data collection: Olurotimi Badero, Bamikole Osibowale. Manuscript drafting: Olurotimi Badero, Bamikole Osibowale, and Adebola Adetiloye. Manuscript revision: Olurotimi Badero, Adebola Adetiloye. All authors approved the final version of the manuscript.
Figure 1: A) angiogram showing chronic total occlusion of the left superficial femoral artery; B) intraluminal crossing of the proximal cap with a 4 french navicross catheter; C) final angiogram with restoration of flow
Figure 2: A) angiogram showing left popliteal artery stenosis: pre-intervention; B) post-intervention
- Edafe E, Dodiyi-Manuel S, Akpa M. Barriers to peripheral artery disease interventions in sub-Saharan Africa- Review article. Clin Pr. 2020;17(1):1436-40. PubMed | Google Scholar
- Johnston LE, Stewart BT, Yangni-Angate H, Veller M, Upchurch GR, Gyedu A et al. Peripheral Arterial Disease in Sub-Saharan Africa: A Review. JAMA Surg. 2016 Jun 1;151(6):564-72. PubMed | Google Scholar
- Okechukwu O, Ikechukwu I, Leonard O, Emmanuel N, Arinze N. Lower limb amputations in Nigeria: An appraisal of the indications and patterns from a premier teaching hospital. Int J Med Health Dev. 2021;26(1):64. Google Scholar
- Anumah FE, Lawal Y, Mshelia-Reng R, Omonua SO, Odumodu K, Shuaibu R et al. Common and contrast determinants of peripheral artery disease and diabetic peripheral neuropathy in North Central Nigeria. Foot Edinb Scotl. 2023 May;55:101987. PubMed | Google Scholar
- Safian RD. CTO of the SFA: what is the best approach? Catheter Cardiovasc Interv. 2013 Sep 1;82(3):493-4 PubMed | Google Scholar
- Lin J, Chen Y, Jiang N, Li Z, Xu S. Burden of Peripheral Artery Disease and Its Attributable Risk Factors in 204 Countries and Territories From 1990 to 2019. Front Cardiovasc Med. 2022 Apr 12;9:868370. PubMed | Google Scholar
- Oyelade BO, OlaOlorun AD, Amole IO, Odeigah LO, Adediran OS. The prevalence of peripheral arterial disease in diabetic subjects in south-west Nigeria. African Journal of Primary Health Care and Family Medicine. 2012 Jan 1;4(1):1-6. Google Scholar
- Hamur H, Onk OA, Vuruskan E, Duman H, Bakirci EM, Kucuksu Z et al. Determinants of Chronic Total Occlusion in Patients With Peripheral Arterial Occlusive Disease. Angiology. 2017 Feb;68(2):151-8. PubMed | Google Scholar
- Shawky K, Marzouk AAE, El-Baz WA, Abd-ElHaseeb AR, Elsayed AMA, Abdelmawla MH. Superficial femoral artery chronic total occlusion crossing strategies. Int J Health Sci. 2022 May 10;2438-53. Google Scholar
- Swaminathan AC, Lokhnygina Y, Kopin D, Miller M, Cox M, Mills J, Crawford L, Patel M, Jones W. Endovascular recanalization of superficial femoral artery chronic total occlusions: a multi-disciplinary, single center experience. Journal of the American College of Cardiology. 2015 Mar 17;65(10S):A2048. Google Scholar