Evolution of hospitalized neurological disorders in Western Madagascar
Rahamefy Odilon Randrianasolo, Imelda Rosy, Raphael Fidelis Randrianarivo, Julien Razafimahefa, Alain Djacoba Tehindrazanarivelo
Corresponding author: Rahamefy Odilon Randrianasolo, University of Mahajanga, Faculty of Medicine, Neurological Department, Hospital CHU PZAGA, Mahajanga, Madagascar 
Received: 28 Mar 2024 - Accepted: 21 Apr 2024 - Published: 03 May 2024
Domain: Neurology (general)
Keywords: Profile, Madagascar, neurological disorders, stroke
©Rahamefy Odilon Randrianasolo et al. PAMJ Clinical Medicine (ISSN: 2707-2797). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Rahamefy Odilon Randrianasolo et al. Evolution of hospitalized neurological disorders in Western Madagascar. PAMJ Clinical Medicine. 2024;15:2. [doi: 10.11604/pamj-cm.2024.15.2.43437]
Available online at: https://www.clinical-medicine.panafrican-med-journal.com//content/article/15/2/full
Evolution of hospitalized neurological disorders in Western Madagascar
![]() Rahamefy Odilon Randrianasolo1,&, Imelda Rosy2, Raphael Fidelis Randrianarivo3,
Rahamefy Odilon Randrianasolo1,&, Imelda Rosy2, Raphael Fidelis Randrianarivo3, ![]() Julien Razafimahefa4, Alain Djacoba Tehindrazanarivelo4
Julien Razafimahefa4, Alain Djacoba Tehindrazanarivelo4
&Corresponding author
Introduction: morbidity and mortality from neurological disorders are increasing, especially in low-income countries like Madagascar. Our objective was to describe the neurological diseases seen in the neurological department and to determine the evolution compared to previous data.
Methods: a descriptive, retrospective study was carried out in the neurological department of a public hospital in Mahajanga in the west of Madagascar in 2020 and 2021. All hospitalized subjects whose discharge diagnosis was a neurological disease were included.
Results: three hundred thirty-four subjects were included. Strokes represented 46.11% of neurological disease in hospitalization, epileptic disease 21, 26%, headaches 9.58%, neuro-infectious disease 7.49%, alcohol withdrawal 5.39%, neuromuscular disease 4.19%, tumor pathologies 3.59% and others neurological diseases 2, 40%. No variation in the disease was seen during the study periods (p=0.26). 83.12% of subjects with stroke were hypertensive and 94.53% were untreated or irregularly treated. Fifty-two percent (n=13) of infectious pathologies were neurological complications of tuberculosis, 2 of which were with co-infection with HIV. A change in the profile of neurological pathologies was noted compared to the data carried out in the same department in the 90s with an increase in strokes, neurological complications of tuberculosis, and HIV, and a decrease in neuropathy.
Conclusion: an adaptation of preventive measures is necessary given this change in the neurological disease profile in our country.
Deaths and disabilities related to neurological disease increased in the past decade [1]. In Africa, this increase in morbidity and mortality is associated with changing disease patterns, such as increased strokes and HIV-related complications [1-4]. In Madagascar, an increase in stroke mortality was reported and became the first cause of death reported in our population [5]. In western Madagascar in the neurological department, the main causes of neurological disease in order of frequency were epilepsy, stroke, central nervous system infections, and neuropathies in the 1990s [6]. The most recent study on neurological pathologies in the locality was carried out in a primary health center that did not allow the comparison and evaluation of the evolution of neurological disease [7]. Our aim in this research was to characterize the neurological conditions that are observed in the neurological department and to ascertain how these have evolved in comparison to earlier data.
Study design and setting: this is a retrospective descriptive study, carried out in the neurology department of Professor Zafisaona Gabriel (PZAGA) University Hospital in Mahajanga in Madagascar for two years from January 1, 2020, to December 31, 2021. This study was carried out in the city of Mahajanga. It is a city located 560km northwest of the capital. It is an urban, coastal district with about 274 720 inhabitants in 2020. It has an area of about 57 km2. One neurology department exists in Mahajanga. It is an adult general neurology department. The department's hiring is represented by the subjects living in the city of Mahajanga and the region of Boeny. A descriptive, retrospective study of patients hospitalized in the neurology department of the PZAGA Mahajanga University Hospital in 2020 and 2021 was carried out. Patients with COVID-19, including those with neurological symptoms, were admitted to a different hospital during the study period.
Participant: included in the study were all hospitalized subjects whose discharge diagnosis was a neurological disease. Incomplete records that did not allow the patient's diagnosis to be determined were excluded.
Variables: the diagnosis of neurological disorders of the patients was evaluated and was classified according to the main cause retained at the discharge in stroke, epileptic disorders, headache, neuroinfectious disease, neuromuscular disease, alcohol withdrawal, tumor disease, dementia, and other neurological diseases.
Data source: we collected retrospective data from the patient's medical record.
Bias: this study's etiological analysis and neurological disorder diagnosis were limited since not all patients had access to neuroimaging and neurophysiological testing such as brain CT scans and electromyography. A neurologist examined every medical file to confirm the accurate diagnosis.
Study size: an exhaustive selection was carried out of all patients hospitalized for neurological disorders in the neurology department during the years 2020 and 2021.
Quantitative variable: demographic data was analyzed for each patient: age, gender, occupation, and city of origin. Diagnosis of neurological disorders upon discharge from hospitalization was analyzed.
Statistical methods: the mean and frequency for each variable were calculated. A comparison of the difference in frequency of neurological disorders seen between 2020 and 2021 was carried out using a Chi-square test. Data recording and analysis were done using Microsoft Excel and EPI info software.
Socio-demographic characteristics of participants: three hundred and thirty four (334) subjects were included as hospitalized for neurological disease. Seven subjects were excluded due to the lack of information. Males represented 52.69% and females 47.31% of all cases. The average age of the subjects was 51.04 years with an extreme of 15 to 94 years. The subjects lived in the city of Mahajanga in 74.85% of cases (Table 1).
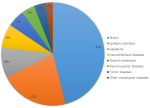
Outcome data: stroke represented 46.11% of all cases, epileptic disease 21.26%, headaches 9.58%, neuro-infectious disease 7.49%, alcohol withdrawal 5.39%, neuromuscular disease 4.19%, tumor disease 3.59% and other neurological diseases 2.40% (Figure 1). The mean age of the stroke patients was 59.64 years. The sex ratio was 0.79 men to one woman. 69.48% were undocumented strokes, 17.53% were hemorrhagic strokes, 11.04% were ischemic strokes, and 1.95% were cerebral venous thrombosis. Minor stroke was found in 25.32%, moderate in 47.40%, and severe in 27.27% according to the NIHS score. 83.12% of the subjects with stroke were hypertensive and 94.53% were untreated or irregularly treated. Neuroinfectious diseases were represented by 13 (52%) cases of neurological complications of tuberculosis, 2 of which were associated with co-infection with HIV, 4 cases of cerebral abscesses, 4 cases of bacterial meningitis, 1 case of viral encephalitis, 1 case of neurocysticercosis, 1 case of leprous neuropathy, 1 case of infectious myelitis. No case of neuro malaria was found in the neurological department. For neuromuscular disease, 8 (57.14%) cases of polyneuropathy, 3 cases of myopathy, 2 cases of Guillan barré syndrome, and 1 case of amyotrophic lateral sclerosis were found.
Other analysis: there was no significant difference between the neurological disorders seen in 2020 and 2021 (p=0.26).
Ethical approval: prior authorization from Hospital staff and the head of the department was requested beforehand.
In Mahajanga, stroke was the most frequent neurological pathology in hospitalization in a neurology department, followed by epilepsy, headaches, and infectious pathologies. Compared to the study which was carried out in the same department in 1995 [6], the most change was the increase in cases of hospitalization for stroke, which represented 21.80% of the causes of hospitalization in 1995 to 46.11% in 2020 and 2021. The number of stroke cases was multiplied by 3 over the 2 years of our study, compared to the number of cases seen over 3 years from 1993 to 1995. Cases of epilepsy did not change and represented 22.22% in 1995 and 21.26% in 2021. A decrease in cases of neurological infectious disease and neuropathies was noted. The clinical and epidemiological context limits the comparison between these two studies. In the previous studies, it was noted the unavailability of certain means of exploration such as computed tomography (CT) scans, magnetic resonance imaging (MRI), and electroencephalogram (EEG) which were available now in our country even if all the patients did not have access to these explorations. This strong increase in stroke cases in Madagascar has been reported by studies of causes of death in our population, where stroke was the 4th cause reported in 1990 and became the leading cause in 2016 [5]. This increase follows the trend in Africa where morbidity and mortality from stroke are increasing [3,4,8].
This strong increase can be linked to several factors, including the urbanization of lifestyle, the high prevalence of arterial hypertension, and the increase in smoking [3]. In our study, 83.12% of subjects with stroke were hypertensive and 94.53% were untreated or irregularly treated, excluding this being the most frequently encountered risk factor for stroke [9,10]. For epilepsy, the hospital prevalence has not changed in 25 years with a high prevalence of more than 20% compared to studies in other African countries which could range from 3 to 10% of the causes of hospitalization in neurology [11-14]. Indeed, Madagascar is a country with a high prevalence of epilepsy [15] and this finding contrasts with estimates where the prevalence and mortality of epilepsy have decreased in recent decades [16]. One of the major changes in the profile of the diseases seen in neurology in our practice was the reduction and change in the neurological infectious pathologies encountered. In the study carried out in 1995, the infectious pathologies of the central nervous system (CNS) represented 19.24% of hospitalizations and were only 7.49% in our study.
The pathologies found were neurocysticercosis first, followed by meningitis and encephalitis, by neuro malaria, then leprosy and neurosyphilis. In our study, the infections found were dominated by complications of tuberculosis with two co-infections with HIV, followed by meningitis, abscesses, and encephalitis, a case of neurocysticercosis and leprosy. The difference between these results can be explained by the diagnosis of neurocysticercosis which was evoked by the clinic and the biological explorations in the 1995 study and by the scanner in our study [6]. The fact that not all of our patients could benefit from a brain CT scan could reduce the cases of neurocysticercosis in our results. These results with an increase in tuberculosis could be explained by the fact that in Madagascar, tuberculosis is constantly increasing, which is associated with the increase in HIV infection [17,18]. It was also observed the absence of cases of neuro malaria and these can be linked to our recruitment, but also a decrease in cases of malaria in the city of Mahajanga. In our hospital, malaria cases could be hospitalized in the emergency room or the infectious disease department. The cause of the decrease in cases of neuropathy is difficult to identify because the cause of these pathologies was not determined, but was later reported to be a high prevalence of mononeuropathy [6]. It was also to observe the persistence of cases of leprosy, which remains frequent, especially in rural areas in the region [6,7].
Limitations: access to paraclinical analyses could limit etiological research for neurological disorders in our context.
This study allows us to see the evolution of neurological disorders seen in a neurology department in Mahajanga over 3 decades and forecasts the evolution of neurological pathologies in developing countries. The epidemic context of 2020 and 2021 with COVID-19 could modify our recruitment, even if no significant variation of neurological disease encountered was noted during 2020 and 2021. A similar situation could be observed in other regions of Madagascar, but over studies would be necessary. Improved preventive measures and care, in particular for stroke, epilepsy, tuberculosis, and HIV, should be improved given the evolution of these pathologies.
What is known about this topic
- Madagascar is a country with a high prevalence of epilepsy and stroke;
- Poor blood pressure control is observed in Madagascar.
What this study adds
- It also shows a strong increase in strokes, which urgently requires improvement in prevention and care in our country;
- This study shows a change in the profile of neurological diseases seen in hospitalization in the neurology department compared to the 1990s in western Madagascar.
The authors declare no competing interests.
All the individuals listed as co-authors in this manuscript have participated in the research work and manuscript write-up.
We thank the staff of the CHU PZAGA Mahajanga Hospital.
Table 1: demographic characteristics of the study population
Figure 1: distribution of neurological disorders in the Mahajanga Neurology Department
- Feigin VL, Nichols E, Alam T, Bannick MS, Beghi E, Blake N et al. Global, regional, and national burden of neurological disorders, 1990-2016: a systematic analysis for the Global Burden of Disease Study 2016. Lancet Neurol. 2019;18(5):459-80. PubMed | Google Scholar
- Vos T, Lim SS, Abbafati C, Abbas KM, Abbasi M, Abbasifard M et al. Global burden of 369 diseases and injuries in 204 countries and territories, 1990-2019: a systematic analysis for the Global Burden of Disease Study 2019. The Lancet. 2020;396(10258):1204-22. PubMed | Google Scholar
- Akinyemi RO, Ovbiagele B, Adeniji OA, Sarfo FS, Abd-Allah F, Adoukonou T et al. Stroke in Africa: the profile, progress, prospects, and priorities. Nat Rev Neurol. 2021;17(10):634-56. PubMed | Google Scholar
- Feigin VL, Vos T, Nichols E, Owolabi MO, Carroll WM, Dichgans M et al. The global burden of neurological disorders: translating evidence into policy. Lancet Neurol. 2020;19(3):255 65. PubMed | Google Scholar
- Masquelier B, Pison G, Rakotonirina J, Rasoanomenjanahary A. Estimating cause-specific mortality in Madagascar: an evaluation of death notification data from the capital city. Popul Health Metr. 2019 Jul 29;17(1):8. PubMed | Google Scholar
- Andriantseheno LM, Andrianasy TF. Hospital-based study on neurological disorders in Madagascar. Data from the northwestern part of the island. Afri J Neuro Sci. July 1997:16(2). Google Scholar
- Gaud S, Sauvée M, Debouverie M. Pathologies neurologiques en milieu tropical et rural?: expérience malgache d´un centre de santé primaire de la région de Boeny. Médecine Santé Trop. 2014;24(3):312-6. Google Scholar
- Adeloye D. An Estimate of the Incidence and Prevalence of Stroke in Africa: A Systematic Review and Meta-Analysis. PLOS ONE. 2014;9(6):e100724. PubMed | Google Scholar
- Wajngarten M, Silva GS. Hypertension and Stroke: Update on Treatment. Eur Cardiol Rev. 2019;14(2):111-5. PubMed | Google Scholar
- Lemogoum D, Degaute JP, Bovet P. Stroke Prevention, Treatment, and Rehabilitation in Sub-Saharan Africa. Am J Prev Med. 2005;29(5, Supplement 1):95-101. PubMed | Google Scholar
- Siddiqi OK, Atadzhanov M, Birbeck GL, Koralnik IJ. The spectrum of neurological disorders in a Zambian tertiary care hospital. J Neurol Sci. 2010;290(1):15. PubMed | Google Scholar
- Chapp-Jumbo EN. Neurologic admissions in the niger delta area of Nigeria - a ten-year review. Afr J Neurol Sci. 15 Oct 2004;23(1). Google Scholar
- Hassane DS, TCF N, AbelChristian TA, Youssouf SO, Zoumana TR, Salimata DI et al. Epidemiological, clinical, diagnostic, and therapeutic profile of hospitalized patients in the neurology department of CHU Gabriel Touré in 2016. Rev int sc méd Abj -RISM-2019;21:124-129. Google Scholar
- Mapoure NY, Doumbe JI, Massi DG, Nynyikua NT, Kuate TC, Luma NH. Epidémiologie clinique des affections neurologiques dans la ville de Douala. Rev Médecine Pharm. 2018;8(1):738-50. Google Scholar
- Andriantseheno LM, Ralaizandriny D. Prévalence communautaire de l´épilepsie chez les Malgaches. Epilepsies. 2004;16(2):83 6. Google Scholar
- Beghi E, Giussani G, Nichols E, Abd-Allah F, Abdela J, Abdelalim A et al. Global, regional, and national burden of epilepsy, 1990-2016: a systematic analysis for the Global Burden of Disease Study 20 Lancet Neurol. 2019;18(4):357-75. PubMed | Google Scholar
- Rakotonirina EJ, Mahadimby JYN, Ravaoarisoa L, Rakotomanga JDM, Macq J. Results of tuberculosis control programs in Madagascar from 1996 to 2004. Med Trop Rev Corps Sante Colon. 2009;69(5):493-5. PubMed | Google Scholar
- Dwyer-Lindgren L, Cork MA, Sligar A, Steuben KM, Wilson KF, Provost NR et al. Mapping HIV prevalence in sub-Saharan Africa between 2000 and 2017. Nature. 2019;570(7760):189-93. PubMed | Google Scholar