Zirconia cantilever bridge and computer-aided design/manufacturing technology: a case report
Hariri Ismail, El Yamani Amal
Corresponding author: Hariri Ismail, Department of Fixed Prosthodontics, Mohammed V University of Rabat, Faculty of Dentistry, Rabat, Morocco 
Received: 30 Mar 2024 - Accepted: 02 May 2024 - Published: 07 May 2024
Domain: Prosthodontics
Keywords: Cantilever bridge, zirconia, digital technology, aesthetic, case report
©Hariri Ismail et al. PAMJ Clinical Medicine (ISSN: 2707-2797). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Hariri Ismail et al. Zirconia cantilever bridge and computer-aided design/manufacturing technology: a case report. PAMJ Clinical Medicine. 2024;15:3. [doi: 10.11604/pamj-cm.2024.15.3.43461]
Available online at: https://www.clinical-medicine.panafrican-med-journal.com//content/article/15/3/full
Case report 
Zirconia cantilever bridge and computer-aided design/manufacturing technology: a case report
Zirconia cantilever bridge and computer-aided design/manufacturing technology: a case report
&Corresponding author
The replacement of an extracted tooth within the aesthetic zone is significantly enhanced by the introduction of a novel dental restoration technique developed by Professor Mathias Kern, which utilizes a one-retainer bonded bridge (Cantilever bridge) made of zirconia. This method, leveraging the precision of computer-aided design/ manufacturing technology, offers a superior solution in terms of aesthetics, functionality, and tissue preservation compared to traditional bridges. Focusing on a case involving a 58-year-old patient with good overall health, this approach demonstrates the importance of meticulous clinical analysis, the expertise of the dental technician, and strict adherence to preparation standards. The zirconia cantilever bonded bridge, supported by computer-aided design/manufacturing (CAD-CAM) technology, not only promises long-term durability but also optimizes the restoration's aesthetic and functional outcomes, making it a noteworthy advancement in the field of dental prosthetics.
Restoring aesthetics in dentistry remains an enduring challenge, necessitating a delicate balance between visual appeal and functional effectiveness. Solutions span from removable prostheses to implant-supported rehabilitation, including conventional bridges. La Rochette introduced a method in 1972 [1], showing tissue preservation potential, but faced detachment issues, yielding a 28% 7.5-year survival rate [2]. However, the paradigm shift brought by digital dentistry and the progressive evolution of adhesive techniques and ceramic material properties has engendered a significant transformation in the landscape of cantilever bridges. A significant leap is the cantilever-bonded zirconia bridge by Prof. Mathias Kern [3]. This prosthetic innovation involves the incorporation of a fin, which effectively engages with a supporting abutment tooth, an intermediary element that adeptly serves as a surrogate for the missing tooth, and a connecting mechanism that seamlessly integrates these constituents. Notably, Computer-Aided Design and Computer-Aided Manufacturing (CAD/CAM) techniques are instrumental in achieving the precise construction of these bridges. We report a case of replacing an upper lateral incisor using a cantilever zirconia bridge fabricated by computer-aided design/manufacturing technology in a 58-year-old patient with good overall health to showcase this novel technique.
Patient information: a 58-year-old patient presented to the fixed prosthodontics department of Rabat, Morocco in January 2022 to have an upper lateral incisor restored. The patient expressed embarrassment about the missing tooth and desired a solution that was both aesthetic and functional, the patient was in good overall health with no medications mentioned. No parafunctional habits were detected, and the incisor had to be extracted due to dental caries. The patient underwent scaling and dental extraction treatment.
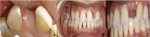
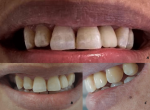
Clinical findings: upon extra-oral examination, facial proportions were found to be harmonious, and the vertical dimension of occlusion was correct (VDO). Concerning the intra-oral examination, the patient maintained satisfactory oral hygiene. As for occlusal examination, a stable occlusion throughout the dental arch was observed. Evaluation of the abutment tooth (left maxillary central incisor) revealed the absence of dental caries or infectious pathology. Periodontal health was deemed satisfactory, with moderate bone resorption. The edentulous ridge revealed a gap aligning with the intended position of the lateral incisor. The oral mucosa in this region appeared healthy, and the degree of bone resorption was not significantly advanced. The tooth displayed neither tipping nor rotation and was appropriately positioned within the dental arch (Figure 1 (A, B, C)).
Diagnostic assessment: a panoramic radiography showed a moderate resorption of the ridge along with a healthy periodontium around the abutment (left central maxillary incisor) with no osteolytic lesions. For better precision, a wax-up in a plaster model for the maxillary arch visualized the future prosthetic reconstruction in all the space planes and showed that the dimension of the edentulous ridge matches the physiological dimensions of the maxillary lateral incisor.
Diagnosis: the collection of all the information through the physical and radiographic examinations revealed a Class III MOD 2 (modification 2) of Kennedy-Appelgate classification on the maxillary arch and a Class III MOD 1 (modification 1) on the mandibular arch along with the absence of any periodontal disease and a stable maximal intercuspation occlusion (OIM).
Therapeutic interventions: the chosen therapeutic approach involved utilizing a one-retained zirconia bonded bridge (cantilever bridge) created through the computer-aided design and computer-aided manufacturing (CAD/CAM) technique. The treatment procedure begins with the tooth preparation of the upper central incisor. This involved creating a rounded shoulder as a finish line with a 0.5mm depth using a cylinder rounded shoulder diamond bur, the shoulder extended from the embrasure to the opposite distal surface to ensure more than 180-degree encircling of the tooth for optimized stabilization. An upper limit was established 2mm away from the free edge to maintain the translucent appearance. On the distal face, a 6mm2 box (3mm in height and 2mm in width) was created using a rugby ball-shaped diamond bur (1.2mm). A macro retention was established at the center of the palatal surface to counteract dislodging force and achieved with a diamond round bur (1.2mm) inserted halfway into its thickness (Figure 2 (A, B, C)). After validating the preparation, a secondary impression was taken using a double mix technique with polyvinylsiloxane (Figure 2 D). The impression of the antagonist arch was taken using an irreversible hydrocolloid. Both the working and antagonist models were poured, followed by sequential digital scans of the working model (Figure 3 (A, B)), the antagonist model (Figure 3 (C, D)), and models in occlusion, using a dedicated computer-aided design/manufacturing laboratory scanner. The next step involved manually identifying the finishing line of the preparation in the computer-aided design software (CAD) marked by the red line (Figure 3 E). The automatic determination of the margin line (purple line) identified automatically by the computer-aided software was not taken into consideration. The insertion axis of the future prosthetic reconstruction was defined (Figure 3 (F, G)), followed by the step-by-step conception of the prosthesis infrastructure. This process is considered the three-dimensional space. Concerning this step; started by designing the pontic (position, shape, and thickness) to meet aesthetic and functional criteria (Figure 4 (A, B, C, D)).
Regarding the connector, it had to be rigid enough to resist mechanical stress. The red color indicates inadequate surface support for loads and an imminent risk of fracture. Once this color disappears, it signifies sufficient surface support for loads. The connection surface must be a minimum of 9mm2, considering the patient's occlusion. The process ended by designing the retainer, following the previously marked limit (red line) to ensure precise positioning (Figure 4 (E, F, G, H, I, J, K)).The computer-aided design was transferred to the computer-aided manufacturing software, which acted as a link between the computer-aided design and the milling machine. The designed prosthesis was then materialized (Figure 4 L). Once the infrastructure was fabricated, a try-in was performed to ensure marginal adaptation, occlusion, and space for cosmetic ceramic. After confirming the try-in, the ceramic shade was selected. The infrastructure was sent back for the application of cosmetic ceramic (layering) (Figure 5 (A, B, C)). A final try-in after layering was performed to check occlusion and aesthetic harmony (Figure 5 (D, E, F)). After the try-in, the ceramic was glazed and the assembly procedure for the zirconia cantilever bridge was conducted, this procedure starts by sandblasting the prosthetic intrados with 50µm alumina oxide at a pressure of 2 bars and by treating it with silane for 3 minutes (Figure 6 (A, B)). Concerning the tooth treatment, a dental isolation was obtained using a rubber dam. The tooth was etched with 37% orthophosphoric acid, rinsed, and dried (Figure 6 (C, D, E)), following by the application of a primer for 20 seconds (Figure 6 F). Excess primer was removed, and the zirconia cantilever bridge was bonded using adhesive resin cement. Excess cement was removed with a micro brush, and photopolymerization was carried out for 20 seconds per face three times (Figure 6 (G, H)). The rubber dam was removed, and the final result was checked (Figure 7 (A)).
Follow-up and outcomes: a follow-up examination after 6 months revealed that the patient had not experienced any discomfort. The aesthetic and functional integration of the prosthetic reconstruction was achieved due to the adherence and cooperation of the patient to the treatment plan (Figure 7 (B, C)).
Patient perspective: with the integration of the aesthetic and the function of the prosthetic reconstruction, the patient regained a confident harmonious smile.
Informed consent: informed written consent was obtained from the patient to publish this work.
The evolution of bonded bridges has been characterized by progressive refinement, facilitated by the introduction of the cantilever bonded bridge design. Notably, this novel configuration demonstrates a pronounced capacity for prolonged survival compared to its conventional two-retained bonded counterpart. As elucidated by Mine A et al. in 2020, the cantilever bonded bridge yields impressive 10-year survival rates of 89.4% and 100%, whereas the conventional two-retainer bonded bridge exhibits comparatively lower rates of 58%, 70.6%, and 71% [4]. This notable disparity can be attributed to the inherent capability of the cantilever design to alleviate stress resulting from variations in abutment mobility. In contrast to the traditional bonded bridge, where divergent abutment mobility can result in adverse outcomes, such as detachment of the retainer from the less robust abutment, the cantilever bonded bridge proficiently confronts and mitigates this issue, as elucidated in our clinical case [5]. It offers benefits such as optimal tissue preservation, therapy reversibility, dental biomimicry, and favorable aesthetic outcomes [5]. However, there are certain disadvantages associated with this bridge design, one of which is the possibility of the ceramic material becoming detached or fractured. Consequently, a comprehensive evaluation of the clinical case is imperative. This assessment primarily hinges on the patient's occlusion, which should exhibit stability and harmony with a consistent maximum intercuspation occlusion (OIM).
Additionally, the periodontal health of the entire oral cavity, particularly that of the abutment tooth, plays a pivotal role in the determination. When selecting the central incisor or canine abutment tooth, several critical factors warrant consideration [6]. Notably, the bonding surface area of the central incisor surpasses that of the canine. Moreover, a preference exists for an abutment tooth devoid of any prior restorations. The concept of passive eruption further comes into play; it is generally observed that the central incisor attains complete passive eruption in adolescents, while the same cannot be said for the canine, however, a recently published study in 2023 [7], conducted through the finite element method, yielded intriguing findings regarding the clinical performance of these abutment options in cantilever bonded bridge therapy. The study demonstrates that the canine exhibits superior clinical performance compared to the central incisor. During maximum intercuspation, the bonded bridge exhibits significantly lower maximum stress (47.5 MPa) when the extension is mesial (canine abutment), as opposed to when the extension is distal (central incisor abutment), where the maximum stress reaches around 93.6 MPa. Turning to the principles of preparations, their parameters are influenced by the prosthetic reconstruction material, whether zirconia or lithium disilicate. For zirconia, a preparation with a 0.5mm internal rounded shoulder is advised at the cervical level of the palatal face. In the case of lithium disilicate, a thickness ranging from 0.8 to 1mm is recommended. It is imperative that the occlusal limit avoids highly translucent areas to preserve the material's translucency along the free edge. Additionally, supragingival preparation is advocated to fulfill bonding requirements. On the proximal aspect, a proximal box should be created, providing a connection surface. If opting for lithium disilicate, the surface area must be 12mm2; for zirconia, 6mm2 is sufficient. To enhance stabilization and retention, an enamel macro-retention is incorporated into the preparation [8].
Bonding procedures are material dependent. For lithium disilicates, after alcohol disinfection, hydrofluoric acid (4-9%) etching is performed for 20 seconds, followed by a 3-minute silane application and the use of a dual composite adhesive. In contrast, for zirconia, alumina oxide 50µm sandblasting is followed by primer application, using an adhesive containing the monomer 10-MDP (Methacryloyloxydecyl dihydrogen phosphate) the preferred choice for zirconia bonding [9]. Tooth treatment involves a 30-second etch with orthophosphoric acid on enamel and 15 seconds on dentin, succeeded by adhesive/primer application and air-assisted spreading.
Importantly, the advent of CAD/CAM technology has revolutionized prosthetic precision. A study in 2014 highlighted that CAD/CAM-produced prostheses exhibited superior marginal precision (48 ± 25 µm2) compared to artisanal counterparts (74 ± 47 µm2) [10]. This technology facilitates comprehensive case visualization across three-dimensional space, streamlining prosthetic design in terms of thickness, surface, shape, and more. However, a learning curve is necessary to harness the full potential of this technology and ensure seamless integration into clinical practice.
Bonded cantilever zirconia bridge therapy offers a compelling blend of aesthetics, functionality, and tissue preservation. However, the key to its success lies in a thorough pre-prosthetic analysis, ensuring enduring outcomes. The use of computer-aided design/manufacturing technology can be useful to visualize and control the conception of the zirconia cantilever bridge in all the space planes.
The authors declare no competing interests.
Patient management: Hariri Ismail. Manuscript drafting and revision: Hariri Ismail, and El Yamani Amal. Both authors have contributed to the production of this article. They also declare reading and approving the final version of this manuscript
Figure 1: initial situation of the clinical case: (A) palatal view shows the gap between the central incisor and the canine; (B) frontal view reveals alignment and space from the missing tooth; (C) the lateral view details the bite and space relations
Figure 2: final form of the abutment´s tooth preparation and the final impression technique: (A) shows the final preparation on the natural teeth; (B) presents the preparation replicated on a plaster model for accuracy testing; (C) visualizes the preparation in a virtual environment via computer-aided design (CAD) software; (D) captures the final impression using polyvinylsiloxane with the one-step double mixing technique
Figure 3: model scanning and determining preparation parameters for cantilever zirconia bridge: (A, B) detail the scanning of the maxillary arch; (C, D) focus on scanning the mandibular arch; (E) illustrates the manual determination of the preparation limits by the green line; (F, G) highlights the process of determining the axis of preparation
Figure 4: design and fabrication of pontic, connection, and fin for the cantilever bridge: (A, B, C, D) depict the pontic design phase in all the space plans, focusing on aesthetic and functional considerations; (E, F, G, H, I, J, K) illustrate the intricate design of the fin and connection components; (L) presents the prosthetic infrastructure immediately post-milling
Figure 5: try-in of the zirconia infrastructure and the final restoration after ceramic layering: the zirconia infrastructure is tested intraorally (A, B, C) to assess fit, comfort, and any necessary adjustments; following this, a final try-in before bonding (D, E, F) is conducted to ensure precise fit, aesthetic harmony, and patient satisfaction before the bonding process photopolymerization
Figure 6: sequential bonding procedure for zirconia cantilever bridge: (A, B) silane application (C) rubber dum isolation; (D) applying phosphoric acid 37%; (E) rinsing and drying; (F) primer application; (G) applying adhesive resin; (H) photopolymerization
Figure 7: immediate outcome and six-month follow-up post bonding: (A) the immediate aesthetic and functional integration of the prosthesis post-bonding; (B, C) provide evidence of the prosthesis's durability and stability, along with the maintenance of aesthetic appeal over time
- Rochette AL. Attachment of a splint to enamel of lower anterior teeth. J Prosthet Dent. 1973 Oct;30(4 Pt 1):418-23. PubMed | Google Scholar
- Creugers NH, Käyser AF, Van´t Hof MA. A seven-and-a-half-year survival study of resin-bonded bridges. J Dent Res. 1992 Nov;71(11):1822-5. PubMed | Google Scholar
- Kern M, Gläser R. Cantilevered all-ceramic, resin-bonded fixed partial dentures: a new treatment modality. J Esthet Dent. 1997;9(5):255-64. PubMed | Google Scholar
- Mine A, Fujisawa M, Miura S, Yumitate M, Ban S, Yamanaka A et al. Critical review about two myths in fixed dental prostheses: Full-Coverage vs. Resin-Bonded, non-Cantilever vs. Cantilever. Jpn Dent Sci Rev. 2021 Nov;57:33-38. PubMed | Google Scholar
- Mourshed B, Samran A, Alfagih A, Samran A, Abdulrab S, Kern M. Anterior Cantilever Resin-Bonded Fixed Dental Prostheses: A Review of the Literature. J Prosthodont. 2018 Mar;27(3):266-275. PubMed | Google Scholar
- Tirlet G, Attal JP. Les bridges collés cantilever en vitrocéramique renforcée au disilicate de lithium raisons du choix et mise en oeuvre clinique, réalités. Cliniques. 2015;26(1):35-46. Google Scholar
- Kihara T, Shigeta Y, Ikawa T, Sasaki K, Shigemoto S, Ogawa T. Designing anterior cantilever resin-bonded fixed dental prostheses based on finite element analysis. J Prosthodont Res. 2023 Jul 31;67(3):418-423. PubMed | Google Scholar
- Chraibi R, Hanine Y, Cherkaoui A, Soualhi H. Ceramic cantilever bridge: A simplified clinical technique. J Dent Spec. 2022 Jul 1;10(2):48-51. Google Scholar
- Soares CJ, Soares PV, Pereira JC, Fonseca RB. Surface treatment protocols in the cementation process of ceramic and laboratory-processed composite restorations: a literature review. J Esthet Restor Dent. 2005;17(4):224-35. PubMed | Google Scholar
- Ng J, Ruse D, Wyatt C. A comparison of the marginal fit of crowns fabricated with digital and conventional methods. J Prosthet Dent. 2014 Sep;112(3):555-60. PubMed | Google Scholar
Search
This article authors
On Pubmed
On Google Scholar
Citation [Download]
Navigate this article
Similar articles in
Key words
Tables and figures
 Figure 2: final form of the abutment�s tooth preparation and the final impression technique: (A) shows the final preparation on the natural teeth; (B) presents the preparation replicated on a plaster model for accuracy testing; (C) visualizes the preparation in a virtual environment via computer-aided design (CAD) software; (D) captures the final impression using polyvinylsiloxane with the one-step double mixing technique
Figure 2: final form of the abutment�s tooth preparation and the final impression technique: (A) shows the final preparation on the natural teeth; (B) presents the preparation replicated on a plaster model for accuracy testing; (C) visualizes the preparation in a virtual environment via computer-aided design (CAD) software; (D) captures the final impression using polyvinylsiloxane with the one-step double mixing technique
 Figure 3: model scanning and determining preparation parameters for cantilever zirconia bridge: (A, B) detail the scanning of the maxillary arch; (C, D) focus on scanning the mandibular arch; (E) illustrates the manual determination of the preparation limits by the green line; (F, G) highlights the process of determining the axis of preparation
Figure 3: model scanning and determining preparation parameters for cantilever zirconia bridge: (A, B) detail the scanning of the maxillary arch; (C, D) focus on scanning the mandibular arch; (E) illustrates the manual determination of the preparation limits by the green line; (F, G) highlights the process of determining the axis of preparation
 Figure 4: design and fabrication of pontic, connection, and fin for the cantilever bridge: (A, B, C, D) depict the pontic design phase in all the space plans, focusing on aesthetic and functional considerations; (E, F, G, H, I, J, K) illustrate the intricate design of the fin and connection components; (L) presents the prosthetic infrastructure immediately post-milling
Figure 4: design and fabrication of pontic, connection, and fin for the cantilever bridge: (A, B, C, D) depict the pontic design phase in all the space plans, focusing on aesthetic and functional considerations; (E, F, G, H, I, J, K) illustrate the intricate design of the fin and connection components; (L) presents the prosthetic infrastructure immediately post-milling
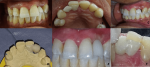 Figure 5: try-in of the zirconia infrastructure and the final restoration after ceramic layering: the zirconia infrastructure is tested intraorally (A, B, C) to assess fit, comfort, and any necessary adjustments; following this, a final try-in before bonding (D, E, F) is conducted to ensure precise fit, aesthetic harmony, and patient satisfaction before the bonding process photopolymerization
Figure 5: try-in of the zirconia infrastructure and the final restoration after ceramic layering: the zirconia infrastructure is tested intraorally (A, B, C) to assess fit, comfort, and any necessary adjustments; following this, a final try-in before bonding (D, E, F) is conducted to ensure precise fit, aesthetic harmony, and patient satisfaction before the bonding process photopolymerization