Embryonal rhabdomyosarcoma of the infratemporal fossa: a case report
Mariam Ameziane Hassani, Masfioui Oumaima, Zineb Belmajdoub, Abdellatif Oudidi, Mohamed Noureddine El Alami El Amine
Corresponding author: Mariam Ameziane Hassani, Department of Otolaryngology and Head and Neck Surgery, Hassan II University Hospital Center, Fes, Morocco 
Received: 10 Apr 2024 - Accepted: 21 Apr 2024 - Published: 20 May 2024
Domain: Otolaryngology (ENT)
Keywords: Aggressive tumor, multimodal treatment, case report
©Mariam Ameziane Hassani et al. PAMJ Clinical Medicine (ISSN: 2707-2797). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Mariam Ameziane Hassani et al. Embryonal rhabdomyosarcoma of the infratemporal fossa: a case report. PAMJ Clinical Medicine. 2024;15:6. [doi: 10.11604/pamj-cm.2024.15.6.43587]
Available online at: https://www.clinical-medicine.panafrican-med-journal.com//content/article/15/6/full
Embryonal rhabdomyosarcoma of the infratemporal fossa: a case report
![]() Mariam Ameziane Hassani1,&,
Mariam Ameziane Hassani1,&, ![]() Masfioui Oumaima1, Zineb Belmajdoub1, Abdellatif Oudidi1, Mohamed Noureddine El Alami El Amine1
Masfioui Oumaima1, Zineb Belmajdoub1, Abdellatif Oudidi1, Mohamed Noureddine El Alami El Amine1
&Corresponding author
Rhabdomyosarcoma (RMS) is a rare primary mesenchymal malignant tumor in adults, an aggressive tumor often diagnosed at an advanced stage. Treatment is multimodal, and based on surgery with radio-chemotherapy. We report the case of a 21-year-old patient admitted for the management of a maxillary mass that had been evolving for 7 months. Imaging revealed a locally advanced tumor of the infratemporal fossa. Biopsy showed inflammatory remodeling. The patient underwent hemimaxillectomy, with an anatomopathological study revealing a rhabdomyosarcoma. The patient underwent chemoradiotherapy and died within 8 months of the start of treatment. Rhabdomyosarcoma is a rare tumor in adults. The clinical picture is non-specific, and the diagnosis of certainty is based on anatomopathological examination with immunohistochemical study. Treatment is multimodal, and based on surgery with radiochemotherapy. The prognosis remains poor.
Rhabdomyosarcoma (RMS) is a primary malignant mesenchymal tumor and belongs to soft tissue sarcomas with striated muscular differentiation. It is observed mainly in children and adolescents. It is rarely diagnosed in adults. These tumors have very rapid spontaneous growth and the diagnosis is often made at an advanced stage. The treatment is multimodal and based on surgery with radio-chemotherapy.
Patient information: this study involved a 21-year-old patient, with no previous history, admitted for treatment of right maxillary swelling with associated dental pain evolving over 7 months.
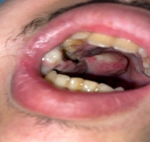
Clinical findings: the clinical examination found a conscious patient, hemodynamically stable, and afebrile. Examination of the face revealed a mass next to the maxillary sinus that was hard, fixed and painful. Anterior rhinoscopy did not find any visible suspicious lesion (Figure 1). Examination of the oral cavity revealed a budding mass on the inner side of the cheek with absence of lymphadenopathy on cervical examination (Figure 2).
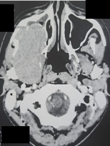
Diagnostic and assessment: the patient underwent a facial and cervico-thoraco-abdominal CT scan which showed a mass centered on the right infratemporal fossa measuring 7cm, locally advanced, without signs of lymph node or distant metastases (Figure 3).
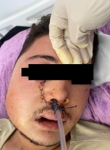
Therapeutic interventions: a biopsy was performed, and the anatomopathological examination with immunohistochemical study came in favor of inflammatory changes. The patient underwent a hemimaxillectomy via the para-lateronasal route (Figure 4).
Follow-up and outcome of interventions: the postoperative course was uneventful with good healing of the surgical incision. The anatomopathological examination confirmed a diagnosis of rhabdomyosarcoma. The case was discussed in a multidisciplinary consultation meeting and the patient was referred for induction chemotherapy followed by radiotherapy if progress was good. The patient was put on chemotherapy based on ifosfamide, vincristine, and actinomycin with palliative radiotherapy. Death occurred 8 months after the start of treatment (Figure 5).
Informed consent: the patient gave his approval for the publication.
Patient perspective: he was grateful for the surgical treatment, which enabled him to have a diagnosis and additional treatment with radiotherapy and painkillers.
Rhabdomyosarcoma (RMS) is a primary malignant tumor, observed mainly in children, and less common in adults. The World Health Organization distinguishes three histological subtypes: embryonal, alveolar, and pleomorphic [1,2]. The worst prognoses are attributed to the alveolar and pleomorphic subtype which is most often found in adults [1-4]. Head and neck RMS can be classified based on location into orbital RMS (25% of cases), parameningeal RMS occurring in the middle ear, nasal cavity, sinus cavities, nasopharynx, and infratemporal fossa, (50% of cases) and non-para meningeal RMS with involvement of the scalp, parotid, oral cavity, pharynx, thyroid, and parathyroid glands (25% of cases) [5].
Adult rhabdomyosarcoma exhibits distinct characteristics when compared to pediatric rhabdomyosarcoma, differing in incidence, location, and prognosis. Incidence of rhabdomyosarcoma in adults is exceedingly low, accounting for only 3% of all malignant tumors in adults. Conversely, in children under 15 years old, rhabdomyosarcoma stands as the most prevalent mesenchymal tumor. Adult RMS tends to occur more frequently in the extremities, whereas pediatric RMS predominantly affects the head and neck region. Ultimately, overall survival rates are poorer for adults than for children with this condition [6].
Clinically, ear, nose, and throat (ENT) rhabdomyosarcoma may manifest with early-onset epistaxis accompanied by exophthalmos and ophthalmoplegia, or present with nonspecific symptoms such as a fixed painful mass, nasal obstruction, rhinorrhea, or otitis. In some cases, particularly the embryonic subtype, it may resemble a gelatinous nasal polyp. Imaging assessments are not diagnostic but aid in determining the tumor's origin, size, and locoregional extension. Computed tomography (CT) scans delineate the tumor's margins and its relationships with adjacent vital and bony structures. Magnetic resonance imaging (MRI) is highly recommended for para-sinus, pterygopalatine fossa, and infra-temporal fossa locations to assess tumor extension. The tumor typically exhibits a heterogeneous signal on MRI, often intensifying or mirroring the muscular signal.
Extension assessments should include a myelogram, brain, and sinus MRI, cervical-thoracic-abdominal CT scan with injection, and 18 FDG PET. The prognosis is grim, especially in cases where lymph node, pulmonary, or bone metastases are present [1,3,7]. Only histological examination with immunohistochemical analysis allows the specific diagnosis, by showing diffuse marking with desmin and myogenin [1,3,8].
The differential diagnosis of head and neck rhabdomyosarcomas in adults includes a wide range of malignant tumors that can affect the head and neck, due to their similar radiological imaging findings. Squamous cell carcinomas are more common in the elderly than rhabdomyosarcomas [5]. In the case of multifocal lesions, lymphoma should be considered rather than rhabdomyosarcoma. Faced with a fatty component, a liposarcoma must be considered and the presence of calcifications points towards a chordoma, a chondrosarcoma, or an osteosarcoma [5]. The embryonic RMS diagnosis can also be confused with a microbial infection or an abscess, but the absence of significant contrast and the rapid increase in the size of the mass point towards a neoplastic pathology [3,6].
There is no consensus on the optimal therapeutic strategy. However, multimodal treatment including surgery combined with chemoradiotherapy is commonly used [1-3,7]. For an operable tumor, surgery is the first-line treatment; additional adjuvant radiotherapy (66-70 Gy) may be offered to maximize tumor control. Inoperable forms benefit from neo-adjuvant chemotherapy (classically combining vincristine and dactinomycin-cyclophospham) then, depending on tumor regression and the patient's general condition, surgery followed by chemo-radiotherapy or radio-chemotherapy [1,3,7,8]. Wagemans et al [2] reported a series of seven cases of embryonal rhabdomyosarcoma of the head and neck of adults. The tumor was resectable in only one patient and was treated postoperatively with radiotherapy alone with good progress and absence of recurrence over 7 years of follow-up. The other six patients started a chemotherapy protocol, and two patients with good responses benefited from surgery with radiotherapy the evolution witnessed the vanishing of the illness. For the remaining patients, the tumor proved inoperable, leading to radiotherapy. Despite treatment, the disease persisted, resulting in death within 26 months of diagnosis.
In our scenario, the patient underwent surgical removal of the tumor, followed by chemo-radiotherapy, yet succumbed to the illness within 8 months of initiating treatment. Despite treatment, the prognosis remains very poor in adults [3]. The prognosis depends on age (the prognosis is poorer in adults than in children), the primary site (the parameningeal site is considered a poor prognostic factor) [2], and the size and sub-type of the tumor. Genetic analysis provides additional prognostic information, the t(1;13) (q36;q14) translocation being associated with a worse prognosis than the t(2;13) (q35;q14) translocation in the alveolar forms [3,7]. The prognosis is poor, with the presence of lymph nodes, and pulmonary or bone metastases. The predictive factors for a good prognosis are age less than 20 years, a tumor less than 5cm long axis, the absence of metastases distance, and negative surgical margins [4].
Rhabdomyosarcoma, a rare tumor in adults, seldom occurs in parameningeal locations. Its clinical presentation lacks specificity. Imaging aids in evaluating tumor extent and operability. A definitive diagnosis relies on anatomopathological examination, supplemented by immunohistochemical analysis. Treatment involves a multimodal approach combining surgery with radiochemotherapy. Despite receiving appropriate therapeutic interventions, the prognosis remains unfavorable.
The authors declare no competing interests.
Mariam Ameziane Hassani described the case, did a literature search, and wrote the first draft of the manuscript. Masfioui Oumaima and Zineb Belmajdoub reviewed the manuscript and made a substantial contribution. Abdellatif Oudidi and Mohamed Noureddine El Alami El Amine reviewed the description of the case and did a concurrent literature search. All the authors have read and agreed to the final manuscript.
Figure 1: clinical image showing right maxillary swelling
Figure 2: clinical image showing the intraoral extension
Figure 3: CT image of a locally advanced tumor of the nasal cavity
Figure 4: clinical image showing the immediate postoperative period
Figure 5: clinical image showing progression with adjuvant therapy
- Hamou M, El Amrani Y, Lachkar A, Eabdenbitsen A, Elayoubi F, Ghailan R. Adult embryonal rhabdomyosarcoma of the nose and paranasal sinuses misdiagnosed as an orbital cellulitis: a case report. PAMJ-Clinical Medicine. 2021 Jan 5;5(3). Google Scholar
- Wagemans J, Beuselinck B, Nuyts S, Sciot R, Delaere P, Vander Poorten V et al. A case series of embryonal rhabdomyosarcoma of the head and neck in adults. Acta Clin Belg. 2010 Nov-Dec;65(6):404-10. PubMed | Google Scholar
- El Sanharawi A, Coulibaly B, Bessede JP, Aubry K. Le rhabdomyosarcome sinusien: une tumeur rare de pronostic péjoratif. Annales françaises d'Oto-rhino-laryngologie et de Pathologie Cervico-faciale. 2013 Feb 1;130(1):26-9. Google Scholar
- Sood N, Sehrawat N. Adult onset sinonasal rhabdomyosarcoma - a rare case report with cytohistological features. Malays J Pathol. 2016 Aug;38(2):169-73. PubMed | Google Scholar
- Cadas C. Prise en charge d´un patient atteint de rhabdomyosarcome. Sciences pharmaceutiques. 2017. Google Scholar
- Kang MS, Kim HJ. Embryonic rhabdomyosarcoma of the nose and maxillary sinus Min. J Korean Soc Magn Reson Med. 2009;13(1):97-100. Google Scholar
- El Sanharawi A, Coulibaly B, Bessede JP, Aubry K. Paranasal sinus rhabdomyosarcoma: A rare tumor of poor prognosis. Eur Ann Otorhinolaryngol Head Neck Dis. 2013 Feb;130(1):26-9. PubMed | Google Scholar
- Ahmed AA, Tsokos M. Sinonasal Rhabdomyosarcoma in Children and Young Adults. Int J Surg Pathol. 2007 Apr;15(2):160-5. PubMed | Google Scholar