Accidental poisoning of hydrocarbon in a child complicated lung abscess : a case report
Dondo Mara, Francois Kouda, Anas Mimi Lahlou, Meriem Haloua, Badr Alami, Youssef Alaoui Lamrani, Mustapha Maaroufi, Meryem Boubbou
Corresponding author: Dondo Mara, Department of Radiology, Mother and Child Hassan II University Hospital, Fes, Morocco 
Received: 21 Mar 2020 - Accepted: 08 Apr 2020 - Published: 15 Apr 2020
Domain: Radiology,Pulmonology,Pediatrics (general)
Keywords: Hydrocarbon, lung, abscess
©Dondo Mara et al. PAMJ Clinical Medicine (ISSN: 2707-2797). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Dondo Mara et al. Accidental poisoning of hydrocarbon in a child complicated lung abscess : a case report. PAMJ Clinical Medicine. 2020;2:146. [doi: 10.11604/pamj-cm.2020.2.146.22432]
Available online at: https://www.clinical-medicine.panafrican-med-journal.com//content/article/2/146/full
Accidental poisoning of hydrocarbon in a child complicated lung abscess : a case report
Dondo Mara1,&, Francois Kouda1, Anas Mimi Lahlou1, Meriem Haloua1, Badr Alami1, Youssef Alaoui Lamrani1, Mustapha Maaroufi1, Meryem Boubbou1
1Department of Radiology, Mother and Child Hassan II University Hospital, Fes, Morocco
&Corresponding author
Dondo Mara, Department of Radiology, Mother and Child Hassan II University Hospital,
Fes, Morocco
Accidental hydrocarbon poisoning encountered in children is often a cause of pneumonia without complications or sequelae. We report a new case of pneumonitis hydrocarbons complicated parenchymatous lung abscess in a child of 3 years following accidental ingestion. The particularity of this clinical case is the scarcity of previous study.
Hydrocarbons exposure occurs by inhalation, ingestion with or without aspiration, or simply skin exposure [1]. According to the characteristics of the substance or its significant systemic absorption, many systems in the body can be affected by these same routes of exposure. The pulmonary system is most often affected by inhalation or aspiration [2]. The prevalence of severe pneumonitis after aspiration of hydrocarbon is less than 2% [3]. They are more frequently found in children during accidental ingestion [4]. However the acute intoxication to hydrocarbons often found in chemical pneumonia cases rarely develops the pneumatocele, lung abscess, pleural effusion or distress syndrome acute respiratory (ARDS) [5]. Thus, we report a case of pneumonia with hydrocarbons, complicated by pulmonary parenchymal microabscess.
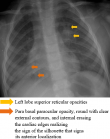
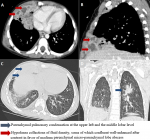
This was a 3-year-old boy admitted after 2 hours of accidental ingestion of gasoline. The mother would have tried to treat her child traditionally giving him milk, olive oil and honey. When he was admitted to our department, he had food vomiting without any respiratory signs or hyperthermia. Subsequently a biological assessment and a chest x-ray were carried out, but without anomaly. An antibiotic prophylaxis based on amoxicillin-clavulanic acid has been introduced. The patient was put under observation for 24h and released with appointment in a week. At three days post-ingestion of gasoline the child was readmitted for respiratory discomfort, irritative cough and appearance of hyperthermia at 39.3°C. On physical examination he was conscious, with a respiratory rate at 32 cycles/min, a heart rate at 120b/min, with pulmonary auscultation which revealed crackling rails at the right basal level. The biological assessment indicated a correct kidney function, a hemoglobin at 11.5 g/dl, leukocytes to 16910/mm3, and the C-reactive protein to 210 mg/l. Radiologically, the frontal chest x-ray had noted the appearance of left superior lobar reticular opacities, and parabasal paraocular opacity, round with clear external contours, and internal erasing the cardiac edges realizing the sign of the silhouette that signs its anterior localization (Figure 1). The chest computerized tomography (CT) scan had individualized lung parenchymatous condensation, in the upper left lobe, middle lobar, and right lower lobar, traversed by an aerial broncho gram, of which the middle lobar was dotted with hypodense collections of fluid density, some of which confluent with contrast-enhanced walls in favor of pulmonary parenchymal micro abscesses (Figure 2). The boy was hospitalized for 10 days under 3rd generation cephalosporin antibiotic treatment. The evolution was marked by a good clinical and biological improvement with drop of leukocytes from 16910 to 9000/mm3, C-reactive protein from 210 to 14 mg/l and total disappearance of the clinical symptomatology.
Chemical pneumonitis is the most common complication of oil poisoning [6]. It occurs most often in children, by accidental ingestion and is a common reason for admission to emergencies in a tropical environment [7, 8]. Hydrocarbons being very volatile, very few are absorbed through the skin : absorption is primarily through respiratory and digestive [9]. Low viscosity and high volatility hydrocarbons such as gasoline, kerosene, stain removers and minerals are easily aspirated [1]. In domestic accidents, boys are the most affected, with a sex ratio (M/F) of 1.5 [9]. Our patient was male and had accidentally drank gasoline in a bottle thinking it was water. Intoxication is tracheal way, causing injury edema, either by duodenal absorption and passage in the alveoli. A secondary inhalation vomiting may worsen the clinical picture [9]. Lung complications which include development of a pneumothorax, a pneumatocele, an abscess, ARDS or broncho-pleural fistula are rare [10]. The beginning of intoxication is often brutal, and the table is dominated by a dry, quintessential cough. Then, during the next few hours, dyspnea of variable intensity, chest pain and sometimes severe fever appear. Polynucleosis is almost constant and the rate of sedimentation is usually high [9]. The clinical symptoms of our patient began three days after ingestion of gasoline marked by respiratory discomfort, irritative cough and 39.3�C hyperthermia associated with elevated leukocytosis and C-reactive protein.
The chest x-ray immediately shows reticular or reticulonodular opacities, as well as condensations with fuzzy contours, sometimes confluent, more or less well systematized. Liquid effusions may be associated. Bilateral attacks are not uncommon. In a study of pneumonia with hydrocarbons : a case reppot, Benjelloun et al., found that CT showed homogenous pulmonary condensation of the right base associated with an air bronchogram and pleural effusion [9]. In our case, the x-ray had noted upper left lobar reticular opacities parabasal paraocular opacity, round with clear external contours, and internal erasing the cardiac edges realizing the sign of the silhouette that signs its anterior localization. The CT scan also revealed pulmonary parenchymal condensations associated with pulmonary parenchymal micro abscesses that are rarely found in the literature. Indeed, in the literature, the factors favoring the appearance of pulmonary abscess in the wake of hydrocarbon pneumonia are still unclear. Our case had developed pulmonary micro-abscesses after repeated vomiting following a traditional treatment provided by the mother. This may be responsible for inhaling the ingested food products and therefore considered as a likely factor promoting the development of lung abscesses. In the literature, antibiotics are used in almost all cases, while steroids are used only in some cases. However, it is difficult to determine whether the changes that occur in the first period of these cases are due to infection or not. Thus, a risk-benefit analysis suggests that antibiotics should generally be given as early treatment [11]. Borer and Koelz reported that treatment is vital and that in complicated cases, the use of antibiotics is beneficial [12]. Thus an antibiotic prophylaxis based on amoxicillin-clavulanic acid was instituted in our patient but given the appearance of signs of superinfection and complications, the antibiotic was changed by a third generation cephalosporin followed by a good clinical evolution and biological.
In sum, pulmonary abscess after ingestion of hydrocarbons remains a rare entity in the pediatric population. However, patients admitted to a chart of hydrocarbon poisoning must be fully assessed and given at least 48 hours of compliance, even if they do not suffer from breathing problems because it is important to keep in mind pulmonary complications that may occur. Last but not least, the best way to avoid pneumonia and their complication would be primary prevention and it would be advisable to put these substances out of the reach of children, by keeping them in their original packaging under cover of safety but also to make parents aware of the use of dietary substances or emetics as a means of detoxification, which is a source of complication.
The authors declare no competing interests.
All authors contributed to this work and read and approved the final manuscript.
Figure 1 : front chest
x-ray
Figure 2 : computerized
tomography image at the thoracic stage in the mediastinal window in axial (A),
sagittal
(B) and pulmonary parenchymal window in axial section (C), coronal (D) with Phosphatidyl
choline (PDC)
injection at the portal phase
- Tormoehlen LM, Tekulve KJ, Nañagas KA. Hydrocarbon toxicity : a review. Clin Toxicol (Phila). 2014 Jun; 52(5):479-89. PubMed | Google Scholar
- Kristin Brown W, Tyler Armstrong J. Hydrocarbon inhalation Treasure Island (FL): StatPearlsPublishing. Jan 2018. Consult� le 20/11/2018
- Colombo JL. Aspiration syndromes. In : Behrman RE, Kliegman RM, Jenson HB (eds). Nelson textbook of pediatrics (17th edition) Philadelphia : WB Saunders Co. 2004. p 1427-1428.
- Lamour C, Bouchaud C, Doré P, D'Arlhac M , Bodin J. Pneumopathies par inhalation d´hydrocarbures volatiles. Revue des Maladies Respiratoires. 2003 Dec;20(6 Pt 1):959-64. PubMed | Google Scholar
- Semiha Bahceci Erdem, Hikmet Nacaroglu T, Rana Isgüder, Canan Unsal Karkiner S, Hüdaver Alper, Demet Can. Pulmonary complications of chemical pneumonia ; a case report. Arch Argent Pediatr. 2016;114(4):245-248. PubMed | Google Scholar
- Argo A, Bongiorno D, Bonifacio A, Pernice V, Liotta R, Indelicato S et al. A fatal case of a paint thinner ingestion: comparison between toxicological and histological findings. Am J Forensic Med Pathol. 2010;31(2):186-91. PubMed | Google Scholar
- Agbessi V. Problèmes posés par l´intoxication au pétrole chez l´enfant. Bull Soc Med Afr Noire Lgue Fr. 1971;16:105-13.
- Huber C, Huber-Braun MC, Desrentes M, Lautier F. Les intoxications aiguës par le pétrole chez l´enfant du Gabon. Bull Soc Pathol Exot. 1987;80:682.
- Benjelloun A, Ait Benasser MA, Driouche A. Pneumopathie aux hydrocarbures : à propos d´un cas. Rev Pneumol Clin. 2006 Jun;62(3):191-4. PubMed | Google Scholar
- Chaudhary SC, Sawlani KK, Yathish BE, Singh A, Kumar S, Parihar A et al. Pyopneumothorax following kerosene poisoning. Toxicol Int. 2014;21(1):112-4. PubMed | Google Scholar
- Bartlett JG. Aspiration disease and anaerobic infection. In : Fishman AP et al. Fishman's pulmonary diseases and disorders (3rd edition) Vol 2. New York : The Mc Graw-Hill Co; 1998, pp. 2011-2019.
- Borer H, Koelz AM. Fire-eater´s lung (hydrocarbon pneumonitis). Schweiz Med Wochenschr. 1994 Mar 5;124(9):362-7. PubMed | Google Scholar