Urodynamic profile of pelvic prolapse before surgical treatment
Tarik Mhanna, Amine El Houmaidi, Mohammed Aynaou, Mohammed Irzi, Ali Barki
Corresponding author: Tarik Mhanna, Department of Urology, Mohammed VI University Medical Center, Mohammed The First University Oujda, Oujda, Morocco 
Received: 11 Dec 2019 - Accepted: 11 Feb 2020 - Published: 20 Apr 2020
Domain: Urology
Keywords: Prolapse, urinary trouble, urodynamics
©Tarik Mhanna et al. PAMJ Clinical Medicine (ISSN: 2707-2797). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Tarik Mhanna et al. Urodynamic profile of pelvic prolapse before surgical treatment. PAMJ Clinical Medicine. 2020;2:151. [doi: 10.11604/pamj-cm.2020.2.151.21274]
Available online at: https://www.clinical-medicine.panafrican-med-journal.com//content/article/2/151/full
Urodynamic profile of pelvic prolapse before surgical treatment
Tarik Mhanna1,&, Amine El Houmaidi1, Mohammed Aynaou1, Mohammed Irzi1, Ali Barki1
1Department of Urology, Mohammed Vi University Medical Center, Mohammed The First University Oujda, Oujda, Morocco
&Corresponding author
Tarik Mhanna, Department of Urology, Mohammed VI University Medical Center, Mohammed The First University Oujda, Oujda, Morocco
This is a descriptive prospective study spread over 2 years, involving 30 patients with symptomatic urogenital prolapse, collected at the urodynamic consultation in the urology department at the CHU Mohammed VI in Oujda. The average age is 57 years, the majority of patients had several risk factors for pelvic floor disorders, all patients had a urinary complaint associated with urge prolapse (66.7%), urinary Incotinence iue (63.3%), mixed urinary incontinence (40%), dysuria (40%), and pollakiuria (70%). Twenty six percent point seven had cystocele stage II and 73.3% had cystocele stage III, 26.7% had a prolapse of more than one floor according to the classification of Baden and Walker. Their mean body mass index (BMI) was 27.5 kg/m2. For the urodynamic assessment (BUD): at the flowmeters: dysuria was found in 11 patients (36.7%), with a significant post-voiding residue in 5 patients (16.7%), the normal flow was found in 63.3% of cases. At cystomanometry: bladder hypersensitivity was found in 8 patients (26.7%), reduced bladder capacity in 4 patients (13.3%) and detrusor overactivity in 9 patients (30%). Profilometry had demonstrated sphincter insufficiency in 17 patients (56.7%), whereas it was normal in 13 patients (43.3%). Urodynamic explorations are part of the diagnostic and prognostic elements in the evaluation of bladder and sphincter disorders associated with urogenital prolapse. They make it possible to objectify the impact of prolapse on the bladder sphincter equilibrium.
Genital prolapse is defined by visceral expulsion from the abdominal-pelvic enclosure (through the vulvar opening) [1]. The cause of genitourinary prolapse is multifactorial: pregnancy, childbirth, genetic factors, abdominal hyper pressure, history of pelvic surgery. On average, 18 out of 10,000 women have genitourinary prolapse [2]. This condition is not always symptomatic, most often, the discomfort is represented by the sensation of a pelvic gravity or intravaginal or externalized ball, urinary disorders are often associated with dysuria type or urinary incontinence [3]. The urodynamic assessment is indicated for patients with prolapse of stage two or more and candidates for surgery to detect clinical or unmasked clinical urinary incontinence by treatment of prolapse [4]. Through our work, we have tried to explore the urodynamic profile of urinary disorders associated with urogenital prolapse and the interest of urodynamic explorations in subsequent management.
This is a descriptive prospective mono-centric study of a series of cases presented to the urology department at Oujda Mohammed VI Hospital, over two years conducted between May 2017 and August 2019, including 30 patients presenting urogenital prolapse with bladder sphincter disorders that are candidates for surgical treatment. Exclusion criteria: operated urogenital prolapse and prolapse without urinary disorders. The study of our patients was based, on the one hand, on a precise clinical examination before performing the Urodynamic testing. A detailed interview preceded the clinical examination in search of functional signs related to pelvic statics precisely age, parity, the course of delivery and chronic constipation. Prolapse was classified according to the classification of Baden and Walker. We looked for urinary incontinence in a standing position and gynaecological position on a full urinary bladder, cough and Ulmsten manoeuvre. A muscle testing of levers anus was practised. All the patients had a bacteriological examination of the sterile urine, an essential condition before the urodynamic testing. The Urodynamic testing was performed in a half-sitting position over three times: flowmeter on a properly filled bladder with post-void residual measurement; a cystomanometry using a bladder catheter, the probe used is Charrière 9, flexible and dual current with a flow rate of 20 ml/min of physiological saline; a profilometry: made with a semi-full bladder and with reduction of prolapse, allowing the measurement of maximum urethral closure pressure.
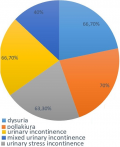
Thirty patients were included in our study, their ages ranged from 40 to 75 years, with an average of 57 years. The average parity was 3.43. Low lane was the mode of delivery in 93% of cases. Their BMIs ranged from 21 to 33 with an average of 27.57 kg/m2. The urinary disorders are represented by dysuria, urinary stress incontinence, urinary incontinence, mixed urinary incontinence and pollakiuria leakage reported by our patients (Figure 1). The classification of prolapse was based on that of Baden and Walker. Of these, 26.7% had a stage II, 73.3% had a cystocele stage III, 26.7% had a prolapse of more than one stage. The average muscle testing of the levers of the anus was 2.20.
Urodynamic results: eleven patients (36.7) had dysuria, of which five (16.7%) had a significant post-voiding residue. Also, 63.3% of the patients had a normal flow rate. However, the bladder capacity was decreased in 4 patients (13.3%) and normal for the rest of the patients. The detrusor hyperreactivity was objectified in 9 patients (30%), with hypo-compliance in 6 cases (20%). Bladder hypersensitivity was noted in 8 patients (26.7%). Besides, profilometry, we objectified sphincter insufficiency in 17 patients (56.7%) and a normal profilometry in the rest of the patients (Table 1). All our patients were programmed for prolapse treatment with or without a urethral surgery according to the results of the urodynamic testing.
Definition: prolapse refers to a falling, slipping or downward displacement of a part or organ. Pelvic organ refers most commonly to the uterus and/or the different vaginal compartments and their neighboring organs such as bladder, rectum or bowel. Pelvic organ prolapse (POP) is thus, primarily, a definition of anatomical change. Some such changes may well be considered within the range of normality for certain women. A diagnosis of POP ideally demands clear clinical evidence, starting with a woman having symptoms related to the “downward displacement” of a pelvic organ [5].
Clinical examination and urinary symptoms: the interrogation: he goes back on the medical history and the patient's surgical risk of prolapse, it makes it possible to evaluate the impact of prolapse on daily life and tolerance by the patient, these elements have a significant impact on the decision therapeutic. The sensation of pelvic heaviness is frequent, walking, there may be ulcerations, haemorrhages or leucorrhea 'Es. Prolapse is responsible for urinary symptoms (urinary incontinence of obvious effort, urgency, urination, terminal drops, pollakiuria) which are not correlated with the prolapse stage. This is concordant with several observational works [6], urge maybe associated with urinary incontinence, it is due to the hernia phenomenon, an observational study prospective including 158 women with prolapse from stages 2 to 4 according to the POP-Q classification, found decreased urgency and leaks 1 year after treatment prolapse in 75% of cases [7]. The clinical examination is done in a gynaecological position, bladder correctly filled, in order to detect incontinence the effort, or stress urinary incontinence masked by the prolapse, it defines a clinical urinary leak that occurs after the repression of prolapse in a patient who does not complains of no incontinence in his daily life. Masked urinary stress incontinence is a diagnosis that is done by clinical examination, its estimated impact in the between 36 and 80% [8], some authors suggest that take into account urodynamic parameters such as urethral closing pressure [9], which explains the discrepancy published results.
The clinical examination is done with a speculum or valve vaginal; it is possible to stagger the prolapse according to two classifications that are the most used [3]: The classification of Baden and Walker: stage 1: intravaginal; stage 2: flush with the vulva; stage 3: exceeding the vulva; stage 4: excreted; the classification of POP-Q: points-based intravaginal at the anterior, mean, and post-prolapse, prolapse is also classed as classification of Baden and Walker. The clinical examination must also evaluate the muscle testing of relievers of the anus and abdominals. Complementary investigations [3]: they have no place in case of genitourinary prolapse asymptomatic; in case of urgency, pollakiuria or incontinence urine, a bacteriological examination of urines looking for an infection or cystoscopy at the search for an associated bladder pathology can be request; pelvic ultrasound can provide information on the state of the uterus and ovaries and assist in the choice of the approach; ultrasound and renal assessment may be requested in the event ofstage IV prolapse, to evaluate the impact on the upper urinary tract; pelvic MRI allows visualization of all organs prolapsed; anorectal manometry in case of evacuation disorder rectal (faecal incontinence, anorectal dyschezia).
Urodynamic testing [10]: there are no technical recommendations today precise details on the practical details of the balance sheet urodynamics in case of genital prolapse. The ideal is to perform reduced prolapse and prolapse examination externalized to evaluate the detrusor-sphincteric balance in both situations and predict the operation detrusor-sphincteric postoperative. two fills with cystomanometry, the one prolapse externalized the other reduces, but most laboratories get content with a reduced prolapse examination. Prolapse can be reduced with a pessary or vaginal compresses. This reduction can be laborious or impossible fully externalized stage 4 prolapse. Urination phase is performed, especially in a sitting position, it is not uncommon for prolapse to become externalized again. During profilometry, care must be taken that compresses vaginal reducing prolapse does not compress the urethra, artificially increasing urethral pressures. It is probably preferable when profilometry of withdraw and perform the prolapsed measurements exteriorized then reduced by the fingers of the operator. The following sequence can be proposed: the flow rate in a sitting position, externalized prolapse; measurement of the residual after urination by survey; reduction of prolapse by compresses or pessary; cystomanometry filling prolapse reduced with voiding phase if possible; prolapse profilometry externalized then reduced by operator's fingers; full bladder cough test (if no micturition phase), externalized prolapse then reduced, without retaining the manoeuvre of the urethra; flow rate (if no voiding phase) in position sitting prolapse reduced. Regarding the interpretation of the examination, it is traditional to discuss the bad specificity, sensitivity and reproducibility sheet with many possible artefacts.
Urodynamic abnormalities found in case of prolapse urogenital
At the flowmetry: this is the first time of urodynamic testing, it is of great interest in the diagnosis of dysuria, women with prolapse have less normal flow rate, more dysuria, post-void residue , indicating the obstructive effect of prolapse [11]. Normally, the flowmeter curve is monophasic and harmonious. In a study involving 348 patients, Costantini et al. consider that a max flow rate of less than 15 mL/s, whether or not associated with an RPM greater than 50 mL for a urine volume greater than or equal to 150 mL, would be in favour of dysuria [12].
At the cystomanometry: the interpretation of the cystomanometry curve makes it possible to detect the presence or absence of detrusor hyper activities, the amplitude and bladder volume of occurrence of these detrusor contractions. The diagnostic value of cystomanometry for the diagnosis of detrusor hyperactivity remains limited. For Rosenzweig et al. [13], 41% of patients with prolapse have clinical signs of overactive bladder (urgency, urinary leakage) of which only 56% have detrusor overactivity. Surgical treatment with cystocele greater than or equal to two improves urgency in 70% of patients, urgency leakage for 82% and pollakiuria in 60% of patients, and eliminates overactive bladder for one out of two patients [14]. It, therefore, seems obvious that prolapse surgery improves the bladder irritative signs without the urodynamic assessment bringing additional prognostic information and besides it will be the objective of our next article comparing the results of the urodynamic testing in post-operative with the initial results.
At the profilometry: it allows to measure the maximum urethral closing pressure. According to the authors, some formulas give its normal value as a function of age (92 - age) [15]. In practice, it is considered that a value of less than 30 cm H2O indicates a sphincter deficiency. Rosenzweig et al. [16] compared flow, cystometry and profilometry in three groups of patients with different stages of cystocele found no differences in the onset and cystometry, the only significant difference is the maximum urethral closure pressure.
Interest of the urodynamic testing before surgical treatment of prolapse genitourinary: the main risk to avoid is to persist or appear stress urinary incontinence following treatment of genital prolapse. Several situations are to consider. The risk of reintervention in women with neither clinical urinary incontinence nor masked incontinence is low in the order of 8.3%. The absence masked urinary incontinence during the urodynamic testing is also a factor of good prognosis of continence postoperative. Conversely, if a stress urinary incontinence is found, the risk reoperation for postoperative urinary leakage passes at 30% [17].
The urodynamic testing remains an important element in the management of patients with urinary disorders associated with urogenital prolapse, allowing assessment of bladder-sphincteric function and guide the indication to associate or not a urinary gesture with the surgery of the prolapse. Also, it represents a reference document in case of failure of the intervention.
What is known about this topic
- Urodynamic assessment is recommended before the price in prolapse surgery;
- The most common urodynamic disorders in front of prolapse: dysuria, urinary stress incontinence, urinary incontinence, mixed urinary incontinence and pollakiuria leakage;
- The treatment depends essentially on the results of the functional gene thus the results of the urodynamic assessment.
What this study adds
- Prove the value of the urodynamic assessment before urogenital prolapse;
- Describe the urodynamic profile of the patients studied;
- A literature review on this subject.
The authors declare no competing interest.
Tarik Mhanna, Amine El houmaidi ,Mohammed Aynaou, and Mohammed Irzi contributed to the design and implementation of the research and to the writing of the manuscript. Ali Barki supervised the manuscript. All the authors have read and agreed to the final manuscript.
Table 1: urodynamic results found in our patients
Figure 1: urinary problems reported by our patients
- Deval B, Parratte B. Prolapsus génitaux : analyse anatomoclinique et place de l´utérus dans la statique pelvipérinéale de le femme. EMC Elsevier Masson, Gynécologie. 2009;320-A-10.
- Lousquy R, Costa P, Delmas V, Haab F. Etat des lieux de l´épidémiologie des prolapsus génitaux. Prog Urol. 2009;19: 907-15. Google Scholar
- Le Normand L. Management of Genito-Urinary Prolapse. Prog Urol. 2014;24(14):925-8. PubMed | Google Scholar
- Bump RC, Mattiasson A, Bø K, Brubaker LP, DeLancey JO, Klarskov P et al. The standardization of terminology of female pelvic organ prolapse and pelvic floor dysfunction. Am J Obstet Gynecol.1996;175(1):10-7. PubMed | Google Scholar
- Haylen BT, Maher CF, Barber MD, Camargo SFM, Dandolu V, Digesu A et al. International Urogynecological Association (IUGA)/International Continence Society (ICS) Joint Report on the Terminology for pelvic organ prolapse (POP). Int Urogynecol J. 2016;27(2):165-194. PubMed | Google Scholar
- Bradley CS, Nygaard IE. Vaginal wall descensus and pelvic floor symptoms in older women. Obstet Gynecol. 2005;106(4):759-66. PubMed | Google Scholar
- Miedel A, Tegerstedt G, Maehle-Schmidt M, Nyren O, Hammarstrom M. Symptoms and pelvic support defects in specific compartments. Obstet Gynecol. 2008;112(4):851-8. PubMed | Google Scholar
- Chaikin DC, Groutz A, Blaivas JG. Predicting the need for antiincontinence surgery in continent women undergoing repair of severe urogenital prolapse. J Urol. 2000;163(2):531-4. PubMed | Google Scholar
- Colombo M, Maggioni A, Scalambrino S, Vitobello D, Milani R. Surgery for genitourinary prolapse and stress incontinence: a randomized trial of posterior pubourethral ligament placation and Pereyra suspension. Am J Obstet Gynecol. 1997;176(2):337-43. PubMed | Google Scholar
- Donona L, Warembourgb S, Laprayc JF, Cortessed A, Hermieue JF, Fattonb B et al. Le Normandi: Bilan avant le traitement chirurgical d´un prolapsus génital : Recommandations pour la pratique clinique. Progrès en urologie. 2016;26:S8-S26. Google Scholar
- Coates KW, Harris RL, Cundiff GW, Bump RC. Uroflowmetry in women with urinary incontinence and pelvic organ prolapse. Br J Urol. 1997;80(2):217-21. PubMed | Google Scholar
- Costantini E, Mearini E, Pajoncini C, Biscotto S, Bini V, Porena M. Uroflowmetry in female voiding disturbances. Neurourol Urodyn. 2003;22(6):569-73. PubMed | Google Scholar
- Rosenzweig BA, Pushkin S, Blumenfeld D, Bhatia NN. Prevalence of abnormal urodynamic test results in continent women with severe genitourinary prolapse. Obstet Gynecol. 1992;79(4): 539-42. PubMed | Google Scholar
- Digesu GA, Salvatore S, Chaliha C, Athanasiou S, Milani R, Khullar V. Do overactive bladder symptoms improve after repair of anterior vaginal wall prolapse. Int Urogynecol J Pelvic Floor Dysfunct. 2007;18(12):1439-43. PubMed | Google Scholar
- Constantinou CE. Urethrometry: considerations of static, dynamic, and stability characteristics of the female urethra. Neurourol Urodyn. 1988;7(6):521-39. Google Scholar
- Rosenzweig BA, Soffici AR, Thomas S, Bhatia NN. Urodynamic evaluation of voiding in women with cystocele. J Reprod Med 1992;37(2):162-6. Google Scholar
- Ballert KN, Biggs GY, Isenalumhe A, Jr., Rosenblum N, Nitti VW. Managing the urethra at transvaginal pelvic organ prolapse repair: a urodynamic approach. J Urol. 2009;181(2):679-84. PubMed | Google Scholar