Bullous disease in infant: think of cutaneous mastocytosis
Kaoutar Achehboune, Khadija Elboukhari, Hanane Baybay, Sara Elloudi, Fatima Zahra Mernissi
Corresponding author: Kaoutar Achehboune, Department of Dermatology, Venereology, Hospital University, Hassan II, Fez, Morocco 
Received: 10 Dec 2019 - Accepted: 11 Feb 2020 - Published: 13 Feb 2020
Domain: Dermatology,Pediatrics (general)
Keywords: Mastocytosis, bullous, infant, Darier sign
©Kaoutar Achehboune et al. PAMJ Clinical Medicine (ISSN: 2707-2797). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Kaoutar Achehboune et al. Bullous disease in infant: think of cutaneous mastocytosis. PAMJ Clinical Medicine. 2020;2:49. [doi: 10.11604/pamj-cm.2020.2.49.21265]
Available online at: https://www.clinical-medicine.panafrican-med-journal.com//content/article/2/49/full
Bullous disease in infant: think of cutaneous mastocytosis
Kaoutar Achehboune1,&, Khadija Elboukhari1, Hanane Baybay1, Sara Elloudi1, Fatima Zahra Mernissi1
1Department of Dermatology, Venereology, Hospital University, Hassan II, Fez, Morocco
&Corresponding author
Kaoutar Achehboune, Department of Dermatology, Venereology, Hospital University, Hassan II, Fez, Morocco
Mastocytosis is a rare disease. The cutaneous form is the most frequent. There are several clinical forms of cutaneous mastocytosis including the bullous form which is rare. We report a case of a 16-month-old girl, presenting pruriginous lesions, evolving since the age of 10 months, treated as bullous impetigo 2 times without improvement. The examination clinic had found post-bullous erosions, resting on healthy skin on the trunk; with hypo-pigmented cicatricial macules, Darier's sign and dermographism were positive. There were no other extra-cutaneous signs. Histology favored cutaneous mastocytosis in its bullous form.
Mastocytosis is a rare disease. There are dermatological and systemic forms. The cutaneous form is the most frequent. We report a case of cutaneous mastocytosis of the infant in its bullous form which is very rare.
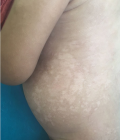
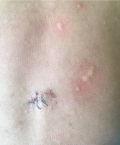
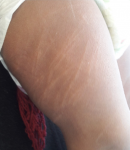
It was a 16-month-old girl born at term by caesarean section of non-consanguineous parents. She had pruritic fluid lesions, evolving since the age of 10 months, treated as bullous impetigo 2 times without improvement. The clinical examination had found post-bullous erosions (Figure 1), well limited, 1cm largest surmounted by hemorrhagic crusts in places, resting on healthy skin, sitting at the trunk, with hypopigmented macular scars (Figure 2). There was no appearance of bullous impetigo or mucosal involvement, Darier sign (Figure 3) and the dermographism (Figure 4) were positive. Moreover, there were no other extra-cutaneous signs. The histology was in favor of cutaneous mastocytosis in its bullous form. Since there was no sign of systemic damage, no further examination was performed. We treated the infant with an oral antihistamine and topical corticosteroids and emollient cream and we explained to the mother hygiene measures to follow: avoid friction by wearing large cotton clothes. We issued a list of drugs and foods to avoid that induce a degranulation masctocyte. At a month's check, no bubbles or erosion were present, with a persistent sign of Darier. Surveillance was scheduled.
Cutaneous mastocytosis is the most common form of mastocytosis [1]. They are characterized by proliferation and abnormal accumulation of mast cells in different tissues. They are thought to be associated with an activator-acquired point mutation of the tyrosine kinase receptor c-KIT, which is also the receptor for the main normal mast cell growth factor, the stem cell growth factor [2]. Several clinical presentations of cutaneous mastocytosis have been described. The bullous form is very rare. Bullous cutaneous mastocytosis can spread on all the integuments. The bubbles are tense, fragile and sometimes hemorrhagic; who healed without scar, intense pruritus and dermographism may be present. The Darier sign is pathognomonic of cutaneous mastocytosis [3]. Systemic damage is possible even though it is rare. It manifests by headache, dyspnea, gastrointestinal bleeding, flushes and sometimes hemodynamic instability or anaphylactic shock or sudden death. The serum tryptase assay can be performed but the predictive value of systemic involvement is difficult to assess in children. The benignity of the disease in the vast majority of cases makes the complementary examinations non-systematic [4]. The diagnosis can be confirmed by histology. The differential diagnoses are first bullous impetigo, staphylococcal epidermolysis, neonatal herpes simplex virus infection, hereditary epidermolysis bullosa, syphilis and bullous pemphigoid [5].
The peculiarity of our case is that the patient has been treated as impetigo several times which is a true differential diagnosis but the presence of a very important pruritus associated with a dermographism very pronounced on the clinical level, which prompted us to achieve Darier's sign was positive and pathognomonic for cutaneous mastocytosis. This has been confirmed by histology. The treatment is mainly based on the elimination of the factors favoring degranulation of the mast cells and which aggravate the symptoms [6] several food and drugs are incriminated. The codeine and morphine are among the best known and are to contraindicate, the pain itself can be a factor triggering [7] in anesthesia, the curares of the family of benzylisoquinolines, except cis-atracurium, are to be avoided since they are highly histamine liberators. At a lesser degree, nefopam and gelatine-based solutes are to avoid in case of mastocytosis [7]. The antihistamines anti-H1 and anti-H2 are used in first line of treatment and topical corticosteroid are also effective [8]. In severe forms, it is possible to use systemic corticosteroids even treatment with alpha interferon or with therapies cytoreductive [9]. In some cases, the interest of imatinib methylate has been shown [1] Children must be equipped with an injectable adrenaline pen for use in case of hypotension deep or choc [10].
Bullous mastocytosis is an exceptional form of cutaneous mastocytosis. Its evolution is generally benign. The first cause of infantile bubbles is impetigo, but it is necessary to know how to evoke a bullous mastocytosis during the association of the bubbles with the dermographism and the sign of Darier to avoid the complications.
The authors declare no competing interest.
All the authors have read and agreed to the final manuscript.
Figure 1: hypopigmented macular scars
Figure 2: positive Darier
sign
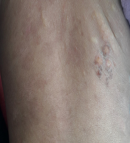
Figure 3: positive dermographism
Figure 4: post-bullous erosions on the back
- Deverrière G, Carré D, Nae I, Cailliez D, Boulloche J. Mastocytose bulleuse diffuse du nourrisson: une forme clinique rare. Archives de Pédiatrie. 2012;19(7):722-725. PubMed | Google Scholar
- Bodemer C, Hermine O, Palmérini F, Yang Y, Grandpeix-Guyodo C, Leventhal PS et al. Pediatric mastocytosis is a clonal disease associated with D816V and other activating c-KIT mutations. J Invest Dermatol. 2010;130(3):804-15. PubMed | Google Scholar
- Akin C, Valent P. Diagnostic criteria and classification of mastocytosis in 2014. Immunol Allergy Clin North Am. 2014;34(2):207-18. PubMed | Google Scholar
- Zaouri H, Amarouch H, Elmakrini N, Tazi N, Ismaili N, Benzekri L et al. Mastocytose cutanée diffuse du nourrisson: à propos d´un cas. Arch Pediatr. 2016 Nov;23(11):1150-1152. PubMed | Google Scholar
- Koga H, Kokubo T, Akaishi M, Iida K, Korematsu S. Neonatal onse diffuse cutaneous mastocytosis: a case Report and review of the literature. Pediatr Dermatol. 2011;28(5):542-6. PubMed | Google Scholar
- AAbid A, Malone MA, Curci K. Mastocytosis. Prim Care. 2016;43(3):505-518. PubMed | Google Scholar
- Dewachter P, Mouton-Faivre C, Cazalaà JB, Carli P, Lortholary O, Hermine O. Mastocytoses et anesthésie. Annales Francaises d´Anesthe'sie et de Re'animation. 2009;28(1):61-73. PubMed | Google Scholar
- Heide R, Tank B, Oranje AP. Mastocytosis in Childhood. Pediatric Dermatology. 2002;19(5):375-381. PubMed | Google Scholar
- Silva I, Carvalho S, Pinto PL, Machado S, Rosado Pinto J. Mastocytosis: a rare case of anaphylaxis in paediatric age and literature review. Allergol Immunopathol (Madr). 2008 May-Jun;36(3):154-63. PubMed | Google Scholar
- Murphy M, Walsh D, Drumm B, Watson R. Bullous mastocytosis: a fatal outcome. Pediatr Dermatol. 1999;16(6):452-5. PubMed | Google Scholar