Anomalous pulmonary venus return: a report of a case diagnosed by ct pulmonary angiogram
Amal Moukhliss, Soukaina Safir, Rihab Machtache, Hatim Zahidi, Abdennaser Drighil, Rachida Habbal, Kawtar Charef, Fadwa Kossale, Saloua Lazaar, Saloua Elmanjra, Fatiha Essodeigui
Corresponding author: Amal Moukhliss, Cardiology Department, IBN ROCHD University Hospital Center, Casablanca, Morocco 
Received: 12 Dec 2019 - Accepted: 11 Feb 2020 - Published: 24 Feb 2020
Domain: Cardiology
Keywords: Anomalous pulmonary venous return, pulmonary vein, CT Angiogram
©Amal Moukhliss et al. PAMJ Clinical Medicine (ISSN: 2707-2797). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Amal Moukhliss et al. Anomalous pulmonary venus return: a report of a case diagnosed by ct pulmonary angiogram. PAMJ Clinical Medicine. 2020;2:66. [doi: 10.11604/pamj-cm.2020.2.66.21288]
Available online at: https://www.clinical-medicine.panafrican-med-journal.com//content/article/2/66/full
Case report 
Anomalous pulmonary venus return: a report of a case diagnosed by ct pulmonary angiogram
Anomalous pulmonary venus return: a report of a case diagnosed by ct pulmonary angiogram
Amal Moukhliss1,&, Soukaina Safir1, Rihab Machtache1, Hatim Zahidi1, Abdennaser Drighil1, Rachida Habbal1, Kawtar Charef2, Fadwa Kossale2, Saloua Lazaar2, Saloua Elmanjra2, Fatiha Essodeigui2
1Cardiology Department, IBN ROCHD University Hospital Center, Casablanca, Morocco, 2Radiology Department, IBN ROCHD University Hospital Center, Casablanca, Morocco
&Corresponding author
Amal Moukhliss, Cardiology Department, IBN ROCHD University Hospital Center, Casablanca, Morocco
Partial anomalous pulmonary venous return is a rare congenital cardiopathy that can progress to right heart failure in the absence of treatment. It can be associated with an intra-auricular communication. The APVR remains often asymptomatic and its discovery is in the majority of cases fortuitous. The thoracic CT Angiogram is the examination of choice to make the diagnosis by showing the localization, the number and the path APVR drainage. We report the case of a 26-year-old female patient with congenital heart disease type an atrial septal defect; who was diagnosed with a partial bilateral APVR associated with PAH signs. We describe the history of the patient whose symptomatology was nonspecific and in whom the imaging examinations, in particular the CT angiogram, made it possible to reach the diagnosis.
Anomalous pulmonary venous return is an abnormality of connection of the pulmonary veins to the left atrium. It consists in the drainage of one or more pulmonary veins other than in the left atrium. Numerous anatomical variants are encountered, ranging from the partial APVR of incidental discovery to the totally blocked APVR (due to an infradiaphragmatic obstacle) which is considered a neonatal emergency [1].
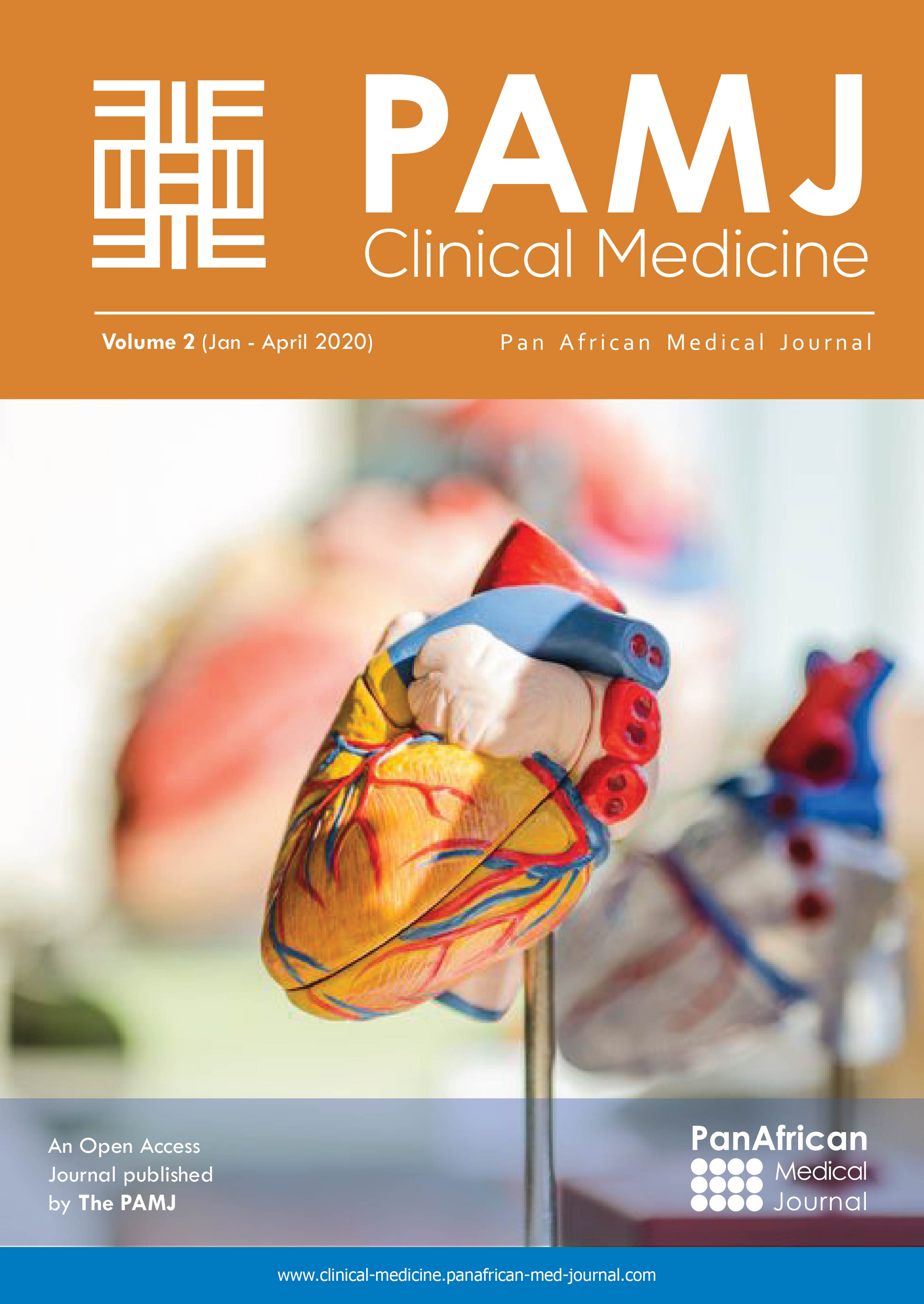
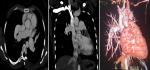
A 26-year-old lady, followed for an atrial septal defect at the cardiothoracic surgery department of Ibn Rochd University Hospital of Casablanca, consults for dyspnea and chest pain progressing rapidly without fever. On clinical examination, signs of right heart failure were found; SpO2 was 95%, her blood pressure was at 120/80mmHg, her pulse at 80 beats/min. On auscultation, a pulmonary outflow murmur was detected with some wheezing sounds. Blood tests (blood count, CRP, Troponin and D-Dimers) revealed no abnormalities. The patient underwent an arterial blood gas test. The arterial blood pH was at 7.47, partial pressure of oxygen was at 60mmHg, partial pressure of carbon dioxide was at 37mmHg and oxygen saturation at 95%. The ECG showed a regular sinus rhythm with an incomplete right bundle branch block, without conduction or repolarization disorder or signs of right ventricular hypertrophy. The chest X-ray displayed a cardiomegaly with a cardio-thoracic index equal to 0.6 and a dilatation of the pulmonary trunk without pulmonary opacities or pleural effusion. A CT pulmonary angiogram was then performed, showing abnormal drainage of the left superior pulmonary vein into the innominate vein and right SPV into the superior vena cava. It also reported significant dilatation of the pulmonary trunk, the right and left pulmonary arteries without intraluminal material. The diagnosis was that of partial left and right bilateral APVR with CT signs of pulmonary arterial hypertension, without signs of pulmonary embolism (Figure 1,Figure 2).
The incidence of APVR is estimated to be 0.4 to 0.7 in the autopsy series [2]. There is a difference between total abnormal pulmonary venous return TAPVR, which represents 2% of all congenital heart defects, and 30% of pulmonary venous return abnormalities. These are severe malformations in which all pulmonary veins drain into the right atrium or its afferent vessels. This abnormality is responsible for heart failure and cyanosis in the first days after birth. An interatrial communication is obligatorily associated and partial venous return (RVPAP). It accounts for 70% of cases, often discovered by chance. The anomaly concerns either a pulmonary vein or both ipsilateral pulmonary veins [3]. PAPVR is mainly found in adults in a fortuitous way [4,5]; occurring either alone or most often in association with congenital heart disease (interatrial or interventricular septal defects). It is an abnormal connection of the pulmonary vascular plexuses and the primary pulmonary vein [6]. The symptomatology, related to the importance of the left-right shunt (increased by interatrial communication), reflects the elevation of pulmonary arterial pressures.
The PAPVR is most often asymptomatic, as in our observation and fortuitously discovered in adulthood during a CT scan, which represents the best diagnostic tool [7]. Clinical signs are mostly absent but asthenia, exercise dyspnea, revealing dry cough, palpitations and chest pain are reported [4]. Heart failure is also possible. The embryonic development of these malformations is still poorly understood. APVRs are 10 times more frequent on the right than on the left [8]. In our case we noted right and left PAPVR. APVRs are twice as frequent on the right and are located on the upper lobes. They drain into the superior subazygotic vena cava, into the large azygos vein or directly into the right atrium [5]. Left APVRs are more rarely observed and was analyzed in a recent retrospective series of 29 adult patients [4]. They drain to the left in the left brachiocephalic venous trunk, in the superior vena cava, in the coronary sinus or in the azygous system [4,5]. Chest CT scan with iodinated contrast injection (CT pulmonary angiogram) or injected thoracic MRI (MR angiography), transesophageal echocardiography and cardiac catheterization are, ranked from the least to the most invasive imaging, currently the key diagnostic tests [9]. In asymptomatic patients, therapeutic abstinence is the rule. In case of a significant shunt, the surgical treatment consists of directing the venous return to the left atrium, with a Dacron tube if necessary and to close the possible interatrial communication [6].
Abnormal pulmonary venous return (APVR) is a rare condition. The diagnosis in adulthood is often difficult. CT pulmonary angiogram simplifies its diagnosis.
The authors declare no competing interests.
All the authors have read and agreed to the final manuscript.
Figure 1: axial CT angiography with coronal reconstruction and VR showing the entry of the right upper pulmonary vein draining into the SVC
Figure 2: axial CT angiography with coronal reconstruction and VR showing the opening of the left superior pulmonary vein which drains towards the innominate venous trunk
- Francart C. Retours veineux pulmonaires anormaux. Encycl Méd Chir Cardiologie. 2003;11.
- Snellen HA, Van Ingen HC, Hoefsmit EC. Patterns of anomalous pulmonary venous drainage. Circulation. 1968;38(1):45-63. PubMed | Google Scholar
- Haloua Meriem. Interet de l´angioscanner dans la prise en charge des malformations congenitales des gros vaisseaux du mediastin: experience du service de radiologie, chu hassan II de fes. mai 2017.
- Haramati LB, Moche IL, Rivera VT, Patel PV, Heyneman L, McAdams HP et al. Computed tomography of partial anomalous pulmonary venous connection in adults. Comput Assist Tomogr. 2003;27(5):743-9. PubMed | Google Scholar
- Greene R, Miller SW. Cross-sectional imaging of silent pulmonary venous anomalies. Radiology. 1986;159(1):279-81. PubMed | Google Scholar
- Kastler B. Retours veineux systémiques et pulmonaires anormaux: aspect IRM et classification. EMC-consulte. 2002.
- Ho ML, Bhalla S, Bierhals A, Gutierrez F. MDCT of partial ano-malous pulmonary venous return (PAPVR) in adults. J Thorac Imaging. 2009;24(2):89-95. PubMed | Google Scholar
- Javangula K, Cole J, Cross M, Kay PH. An unusual manifestation of left partial anomalous pulmonary venous connection. Interactive Cardiovascular and Thoracic Surgery. 2010;11(6):846-8. PubMed | Google Scholar
- Dujon C, Azarian R, Mignon F, Petitpretz P. Retour veineux pulmonaire anormal révélé par un œdème pulmonaire localisé. Rev Mal Respir. 2006;23(1 Pt 1):89-91. PubMed | Google Scholar