Adenoid cystic carcinoma of head and neck
Fatma Dhouib, Wicem Siala, Semia Ben Hassine, Nejla Fourati, Wafa Mnejja, Bouthaina Hammami, Jamel Daoud
Corresponding author: Fatma Dhouib, Department of Oncology Radiotherapy, Habib Bourguiba University Hospital, Al Firdaws Street, Sfax 3029, Tunisia 
Received: 28 Jun 2020 - Accepted: 03 Jul 2020 - Published: 22 Jul 2020
Domain: Oncology
Keywords: Adenoid cystic carcinoma, head and neck, surgery, adjuvant radiotherapy
©Fatma Dhouib et al. PAMJ Clinical Medicine (ISSN: 2707-2797). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Fatma Dhouib et al. Adenoid cystic carcinoma of head and neck. PAMJ Clinical Medicine. 2020;3:132. [doi: 10.11604/pamj-cm.2020.3.132.24624]
Available online at: https://www.clinical-medicine.panafrican-med-journal.com//content/article/3/132/full
Adenoid cystic carcinoma of head and neck
Fatma Dhouib1,2,&, Wicem Siala1,2, Semia Ben Hassine1,2, Nejla Fourati1,2, Wafa Mnejja1,2, Bouthaina Hammami2,3, Jamel Daoud1,2
&Corresponding author
Adenoid cystic carcinoma is a relatively rare tumor of head and neck. Due to lack of high-quality evidence, optimal treatment still controversial and continues to evolve over time. We conducted a retrospective review of 26 patients with adenoid cystic carcinoma of head and neck treated between 1993 and 2015 in the radiation Oncology Center of Habib Bourguiba Hospital, Sfax, Tunisia. Demographic, clinical, treatment, and survival details of the patients were collected and analyzed. Disease-free survival (DFS) and overall survival (OS) were estimated by Kaplan-Meier method. The mean age of patients in the study was 51 years (range:16-73 years), with a male preponderance (54% vs. 46%). The most commonly primary disease sites were the parotid glands (34.6%), the oral cavity (19.66%) and the submandibular glands (11.5%). More than half the patients presented with earlier-stage disease (T1/2:73%); most had a negative nodal status (92.3%). Twenty-four patients (92.4%) received surgery with adjuvant RT; one (3.8%) RT only and another (3.8%) surgery only. Fourteen (53.8%) patients had positive margins and no additional patients had close margins. Perineural invasion (PNI) was documented in 8 (32%) patients. The median time to any recurrence was 21 months (range:3-204 months). Five-year overall survival and disease-free survival rates were 62% and 53%. Solid histological subtype, positive surgical margins, PNI and advanced stages were predictors of poor outcome in adenoid cystic carcinoma of head and neck. Surgery followed by adjuvant radiotherapy remains the treatment of choice that may provide local control and prolong patient survival.
Adenoid cystic carcinoma (ACC) accounts for 1% of all head and neck (HN) cancers and about 10-22% of all malignant tumors of the salivary glands [1]. Adenoid cystic carcinoma occurs primarily in the salivary glands, but can also be found at other sites [2]. Minor salivary glands (65%) are more frequently involved than major salivary glands (submandibular: 19%, parotid: 16%) [1]. The disease usually presents in a localized manner, but is known for its propensity for late metastasis (up to 15 years after initial diagnosis) [3]. Although ACC can be found at any age, it typically presents in the 5th decade (median age: 57.4 years), and it has a slight female preponderance (up to 60%) [2]. Although these tumors are usually low-grade malignancies as per histologic differentiation, management of these tumors is a distinct therapeutic challenge because of the propensity for local invasion, perineural involvement, distant metastasis and ability to recur over a prolonged period. Surgery is the cornerstone of management of ACC. Studies have demonstrated the utility of adjuvant radiation in terms of superiority of the disease control over either modality alone [4]. However, the improvement in loco-regional control with combined modality treatment did not translate into a significant improvement in overall survival rate [4]. The role of chemotherapy in ACC is not yet optimally defined and is still considered investigational [5]. Most studies concur that overall survival rate for ACC is favorable, with 5-year survival ranging between 64% and 89% and 10-year survival between 37% and 77% [6]. The aim of the present study was to evaluate patient and disease characteristics and treatment modalities in ACC, and to identify prognostic factors.
Medical records were reviewed and data collected on all HN ACC over a 22-year period (1993-2015) from the radiation oncology center of Habib Bourguiba Hospital Fax. A total of 27 patients of HNACC cases were identified. One case with missing data was excluded from analysis. The study included all patients who, in the medical record, the result of histological analysis was adenoid cystic carcinoma. Were excluded the cylindromas not dependent on HN, patients with a date diagnosis beyond December 2015 and those for which the medical record was unusable. Collected data were analyzed for a demographic profile, clinical presentation, disease site, stage, treatment modalities, and survival outcome. Patients were retrospectively staged as per American Joint Committee on Cancer (2010) TNM classification. Data were analyzed using the IBM Statistical Package for Social Sciences (SPSS) statistics base (version 20.0). Categorical variables are expressed as frequencies and percentages; patient age is expressed as mean and standard deviation. Overall survival (OS) was defined as the period from date of diagnosis to date of death or last follow-up visit, with patients censored at their last follow-up visit. Disease free survival (DFS) was defined as the period from date of diagnosis to date of relapse, progression, death, or last follow-up visit, and was similarly censored at the last follow-up visit. The Kaplan-Meier method was used to estimate both 5-and 10-year OS and DFS. For each estimate, 95% confidence intervals are also reported. A P-value less than 0.05 was considered statistically significant.
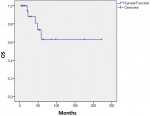
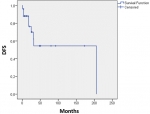
Mean age of patients was 51 years (range: 16-73 years), with a male preponderance (54% vs. 46%). The sites most commonly involved were the parotid glands (34.6%), the oral cavity (19.66%), the submandibular glands (11.5%), and the nasal cavity or nasopharynx (2%). More than half the patients presented with earlier-stage disease (T1/2: 73%); most had a negative nodal status (92.3%). Twenty-five patients underwent surgery of whom only one patient (4%) was treated with surgery alone and 24 (96%) received adjuvant radiotherapy following surgical resection. The type of surgical procedure was governed by the primary site, extent of disease, cosmetic considerations, and discretion of the operating surgeon. In general, an attempt was made to maximize local control with preservation of cosmetic and functional outcome. Modified neck dissection was performed in 15 (57.7%) patients three of whom (20%) underwent bilateral neck dissection. Only 2 (13.3%) of these 15 patients had positive lymph nodes on histopathology. The cut margin status was recorded as negative, close (<5 mm) or positive. Fourteen (53.8%) patients had positive margins and no additional patients had close margins. PNI was defined as positive when tumor cells were identified in the perineural space or epineurium. Tumors that were only adjacent to nerves without entering in the perineural space were not considered to have PNI. PNI was documented in 8 (32%) patients. One (3.8%) patient, with a tongue primary was poor surgical candidate, and was treated with radical external beam radiotherapy (EBRT). Twenty-four (92.4%) patients we retreated with postoperative adjuvant EBRT with conventional once-daily fractionation. The indications for adjuvant radiotherapy were the presence of PNI, close or positive margins, T4 stage, and nodal positivity. The radiation technique was dictated by the primary site, presence of PNI, stage, and nodal involvement. The treatment volume was designed to cover the tumor bed with a 2 cm margin. For patients with PNI the field was extended till the skull base for occult disease. The median total dose of radiation (including patients with radical radiotherapy) was 64 Gy (range, 50-75 Gy). None of the patients received concurrent or adjuvant systemic chemotherapy. Table 1 summarizes patients and disease characteristics. A total of 4 patients (15.4%) recurred at the primary site, 2 being isolated local failures. Two (7.7%) patients had a regional recurrence. Twelve (46.2%) patients were detected to have distant metastases, four (33.3%) of which were associated with some loco-regional failure. The median time to any recurrence was 21 months (range: 3 - 204 months).There was no significant difference between time to local or regional failure (median 21 months; range: 3 - 204 months) vs. time to distant metastases (median 24.5 months; range: 1-204 months). Seven of the twelve (58.3%) patients with distant metastases had lung as the first site of distant failure. The OS and DFS rates for patients with ACC of head and neck were 87% at 3 years, 62% at 5 years and 70% at 3 years, 53% at 5 years, respectively (Figure 1, Figure 2)
Salivary gland neoplasms are uncommon head and neck tumors with widely varied histologic subtypes, diverse clinical behavior, and vastly different prognosis [7]. Adenoid cystic carcinoma is a rare salivary gland tumour that accounts for 1 percent of all head and neck malignancies. It affects people in all decades of life and has no known risk factors. In the literature we found a female predominance and a median age of 59 years with a peak incidence between 50 and 60 years [8]. Mean age in our study was 51 years (range: 16-73 years), with a discrete male preponderance (54% vs. 46%). Tumours are classified into solid, cribriform and tubular histotypes: the solid type is considered a high-grade lesion with more aggressive biological behaviour and is associated with a poorer short-term survival rate [9]. Head and neck adenoid cystic carcinoma is a locally aggressive tumour with a tendency for nerve involvement. Various clinicopathological factors are associated with a poor prognosis, including advanced age, site, nodal metastases, close or positive margins, tumour site, advanced pathological tumour and node stage, histological grade, extracapsular spread, bone invasion, muscle invasion, and distant metastases [10]. Surgical resection is the mainstay of treatment for adenoid cystic carcinoma. The respectability depends on the tumour size, location and extent, as well as the presence of co-morbidities. The optimal non-surgical management is undefined. However, in unresectable disease, radical radiotherapy with palliative intent can result in excellent disease control. Therefore, patients with unresectable adenoid cystic carcinoma with or without distant metastasis should be considered for definitive radiotherapy on an individual basis at the discretion of the local multidisciplinary team [10]. The efficacy of radiotherapy alone as a primary treatment modality for adenoid cystic carcinoma in the head and neck has been debated. When used as a primary modality alone it does not confer a good overall survival rate [11]. Postoperative adjuvant radiation therapy is recommended by literatures because of the high rates of recurrence of ACC [2]. However, the role of postoperative radiation therapy is still controversial, and indications for its use currently differ both within and between institutions. Although some people advocate radiation therapy for essentially all patients with adenoid cystic carcinoma of the head and neck, others reserve radiation therapy for only those with unfavorable features such as PNI or positive surgical margins [4,12].
Shezhi He et al. showed that surgery with postoperative radiation provided a better OS and DFS (89%, 70.4%) compared with surgery alone (82.2%, 63.3%), but there was no significant difference (P>0.05) [13]. Most studies report that treatment of adenoid cystic carcinoma at multiple sites with surgery and adjuvant radiotherapy enhances local control [14,15]. Garden et al. analyzed 198 cases of ACC of the head and neck at MD Anderson Cancer Center [15], 42% of all patients had microscopic positive margins and 28% had close (< or = 5 mm) or uncertain margins. After a treatment of surgery and postoperative radiotherapy, only 18% of patients with positive margin developed local recurrences, compared to 9% with close or uncertain margins, and 8% with negative margins. They recommend a dose of 60 Gy to the tumor bed for most ACC patients, supplemented to 66 Gy for patients with positive margins. Shezhi He et al. revealed that surgical margin status was independent predictor of outcome [13]. Positive surgical margins were found in 42.3% of the patients, 72.7% of whom had local recurrences compared with 16% of patients with negative margins had local recurrences. Other authors reported the presence of surgical positive margins as a significant parameter for survival and tumor control [6]. Advanced stage had a negative impact on OS and DFS; this suggests that these tumors are larger, more aggressive, and it may be more difficult to achieve adequate resection margins in this group [13]. In order to evaluate the importance of PNI, Garden et al. found in their series that was a negative survival predictor because of a higher incidence of distant metastasis [15]. Recently, Ju et al. analyzed the importance of clinical evidence of PNI on patients with ACC and found it was an independent factor for poor prognosis [16]. In our study, the overall survival and disease-specific survival rates for patients with ACC of head and neck were 87% at 3 years, 62% at 5 years and 70% at 3 years, 53% at 5 years, respectively. As our series was small (n = 26), limited conclusions can be drawn from the univariate analysis. A role for chemotherapy in adenoid cystic carcinoma treatment is still developing. Trials have shown that current chemotherapy regimens may improve the quality of life but not the overall survival rate for patients with distant metastases from adenoid cystic carcinoma of the head and neck [17]. Metastases usually occur in the lungs and bone: outcomes are worse for patients with bone involvement with or without lung metastases than for those with isolated pulmonary metastasis [18]. In Van Weert S et al. study, 52% of patients developed metastases within the first five years post-treatment [19]. In our series, 58.3% of patients with distant metastases had lung as the first site of distant failure with a median time to distant events of 24.5 months.
Adenoid cystic carcinoma is a relatively rare tumor of head and neck. Due to lack of high-quality evidence, optimal treatment continues to evolve over time. Surgical resection with clear margins is currently considered as the standard of care for the vast majority of patients with adenoid cystic carcinoma of head and neck. The use of adjuvant radiotherapy though somewhat controversial is increasing over time. Surgery combined with postoperative radiation provides the best overall survival in patients with ACC of the minor salivary glands. Radiotherapy or chemotherapy only still cannot cure this disease. Solid histological subtype, PNI, positive surgical margins and advanced stages are poor prognostic factors that significantly affect local control and survival. Further larger prospective studies are warranted to better characterize the disease and to define optimal therapeutic modalities that would maximize outcomes and minimize treatment-related morbidity.
What is known about this topic
- Adenoid cystic carcinoma is a relatively rare tumor of head and neck;
- Surgical resection with clear margins is the cornerstone of management of adenoid cystic carcinoma.
What this study adds
- Solid histological subtype, positive surgical margins, PNI and advanced stages were predictors of poor outcome in adenoid cystic carcinoma of head and neck;
- Surgery followed by adjuvant radiotherapy may provide better disease local control and prolong patient survival.
The authors declare no competing interests.
All the authors contributed to the conduct of this work. All authors also state that they have read and approved the final version of the manuscript.
Table 1: patient and disease characteristics
Figure 1: overall survival for all patients with adenoid cystic carcinoma of head and neck
Figure 2: disease free survival for all patients with adenoid cystic carcinoma of head and neck
- Spiro RH, Huvos AG, Strong EW. Adenoid cystic carcinoma of salivary origin: a clinicopathologic study of 242 cases. Am J Surg. 1974 Oct;128(4):512-20. PubMed | Google Scholar
- Ellington CL, Goodman M, Kono SA, Grist W, Wadsworth T, Chen AY, Owonikoko T, Ramalingam S, Shin DM, Khuri FR, Beitler JJ, Saba NF. Adenoid cystic carcinoma of the head and neck: incidence and survival trends based on 1973-2007 Surveillance, epidemiology, and end results data. Cancer. 2012 Sep 15;118(18):4444-51. PubMed | Google Scholar
- Matsuba HM, Simpson JR, Mauney M, Thawley SE. Adenoid cystic salivary gland carcinoma: a clinicopathologic correlation. Head Neck Surg. 1986;8(3):200-4. PubMed | Google Scholar
- Miglianico L, Eschwege F, Marandas P, Wibault P. Cervico-facial adenoid cystic carcinoma: study of 102 cases. Influence of radiation therapy. Int J Radiat Oncol Biol Phys. 1987 May;13(5):673-8. PubMed | Google Scholar
- Papaspyrou G, Hoch S, Rinaldo A, Rodrigo JP, Takes RP, Van Herpen C et al. Chemotherapy and targeted therapy in adenoid cystic carcinoma of the head and neck: a review. Head Neck. 2011 Jun;33(6):905-11. PubMed | Google Scholar
- Chen AM, Bucci MK, Weinberg V, Garcia J, Quivey JM, Schechter NR et al. Adenoid cystic carcinoma of the head and neck treated by surgery with or without postoperative radiation therapy: prognostic features of recurrence. Int J Radiat Oncol Biol Phys. 2006;66(1):152-9. PubMed | Google Scholar
- Agarwal JP, Jain S, Gupta T, Tiwari M, Laskar SG, Dinshaw KA et al. Intraoral adenoid cystic carcinoma: prognostic factors and outcome. Oral Oncology. 2008 Oct;44(10):986-93. PubMed | Google Scholar
- Kokemueller H, Eckardt A, Brachvogel P, Hausamen JE. Adenoid cystic carcinoma of the head and neck: a 20 years experience. Int J Oral Maxillofac Surg. 2004 Jan;33(1):25-31. PubMed | Google Scholar
- Bhayani MK, Yener M, El-Naggar A, Garden A, Hanna EY, Weber RS et al. Prognosis and risk factors for early-stage adenoid cystic carcinoma of the major salivary glands. Cancer. 2012 Jun 1;118(11):2872-8. PubMed | Google Scholar
- Ali S, Yeo J C-L, Magos T, Dickson M, Junor E. Clinical outcomes of adenoid cystic carcinoma of the head and neck: a single institution 20-year experience. The Journal of Laryngology & Otology. 2016 Jul;130(7):680-5. PubMed | Google Scholar
- Iseli TA, Karnell LH, Graham SM, Funk GF, Buatti JM, Gupta AK et al. Role of radiotherapy in adenoid cystic carcinoma of the head and neck. J Laryngol Otol. 2009 Oct;123(10):1137-44. PubMed | Google Scholar
- Dubal PM, Unsal AA, Chung SY, Patel AV, Chan Woo Park R, Baredes S et al. Population-based trends in outcomes in adenoid cystic carcinoma of the oral cavity. American journal of otolaryngology. 2016;37(5):398-406. PubMed | Google Scholar
- Shizhi H, Pingdong L, Qi Z, Lizhen H, Zhenkun Y, Zhigang H et al. Clinicopathologic and prognostic factors in adenoid cystic carcinoma of head and neck minor salivary glands: a clinical analysis of 130 cases. American Journal of Otolaryngology-Head and Neck Medicine and Surgery. 2017;38(2):157-62. PubMed | Google Scholar
- Terhaard CH, Lubsen H, Van der Tweel I, Hilgers FJ, Eijkenboom WM, Marres HA et al. Salivary gland carcinoma: independent prognostic factors for locoregional control, distant metastases, and overall survival: results of the Dutch head and neck oncology cooperative group. Head Neck. 2004 Aug;26(8):681-92. PubMed | Google Scholar
- Garden AS, Weber RS, Morrison WH, Ang KK, Peters LJ. The influence of positive margins and nerve invasion in adenoid cystic carcinoma of the head and neck treated with surgery and radiation. Int J Radiat Oncol Biol Phys. 1995 Jun 15;32(3):619-26. PubMed | Google Scholar
- Ju J, Li Y, Chai J, Ma C, Ni Q, Shen Z et al. The role of perineural invasion on head and neck adenoid cystic carcinoma prognosis: a systematic review and meta-analysis. Oral surgery, oral medicine, oral pathology and oral radiology. 2016;122(6):691-701. PubMed | Google Scholar
- Spiro RH. Distant metastasis in adenoid cystic carcinoma of salivary origin. Am J Surg. 1997 Nov;174(5):495-8. PubMed | Google Scholar
- Sung MW, Kim KH, Kim JW, Min YG, Seong WJ, Roh JL et al. Clinicopathologic predictors and impact of distant metastasis from adenoid cystic carcinoma of the head and neck. Arch Otolaryngol Head Neck Surg. 2003 Nov;129(11):1193-7. PubMed | Google Scholar
- Van Weert S, Bloemena E, Van der Waal I, De Bree R, Rietveld DH, Kuik JD et al. Adenoid cystic carcinoma of the head and neck: a single-center analysis of 105 consecutive cases over a30-year period. Oral Oncol. 2013 Aug;49(8):824-9. PubMed | Google Scholar