Iatrogenic ureterocutaneous fistula and incisional hernia following laparotomy - case report
Nasir Oyelowo, Abdullahi Sudi, Aliyu Ibrahim, Mubarak Zubair Abdullahi, Ahmad Tijani Lawal
Corresponding author: Nasir Oyelowo, Department of Surgery Ahmadu Bello University Zaria, Kaduna Nigeria 
Received: 13 Jul 2020 - Accepted: 24 Jul 2020 - Published: 13 Aug 2020
Domain: Gynecology,Urology
Keywords: Ureterocutaneous fistula, ureteric injury, incisional hernia
©Nasir Oyelowo et al. PAMJ Clinical Medicine (ISSN: 2707-2797). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Nasir Oyelowo et al. Iatrogenic ureterocutaneous fistula and incisional hernia following laparotomy - case report. PAMJ Clinical Medicine. 2020;3:170. [doi: 10.11604/pamj-cm.2020.3.170.24985]
Available online at: https://www.clinical-medicine.panafrican-med-journal.com//content/article/3/170/full
Case report 
Iatrogenic ureterocutaneous fistula and incisional hernia following laparotomy - case report
Iatrogenic ureterocutaneous fistula and incisional hernia following laparotomy - case report
Nasir Oyelowo1,&, Abdullahi Sudi1, Aliyu Ibrahim2, Mubarak Zubair Abdullahi2, Ahmad Tijani Lawal1
&Corresponding author
Ureteric injuries are known and preventable complications that may follow pelvic surgeries. These injuries are commonly ligation of the distal ureters and are frequently missed intraoperatively. Symptoms typically comprise of post-operative flank pain, fever, and flank swelling from urinary tract obstruction or urinoma. We hereby present a rare case of iatrogenic ureteric injury, ureterocutaneous fistula, and an associated incisional hernia in a middle-aged woman who had ovarian cyst excision.
Ureteric injuries are an uncommon complication that may follow open and laparoscopic procedures in the pelvis such as gynecological, colorectal, or vascular surgeries [1]. Gynecological surgeries account for 50-70% of these injuries [2]. The distal ureter may by inadvertently ligated or transected during the control of vascular pedicles in the pelvis especially as it lies beneath the infundibulopelvic ligament during gynecological procedures such as abdominal hysterectomy [3]. Most of these injuries are not recognized intraoperatively in 70% of cases, hence the diagnosis is made following evaluation for postoperative fever, flank pain, flank mass, or anuria from bilateral urinary tract obstruction [4]. Rarely a fistula may occur. We present a case of iatrogenic ureteric injury with subsequent complications from the ureteric injury.
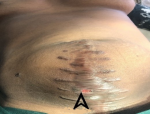
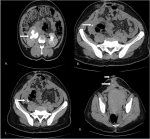
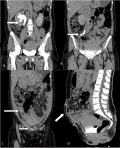
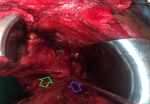
A 38-year-old woman was referred with complaints of an 8-weeks history of discharge of urine from a site on the anterior abdominal wall following abdominal surgery as well as a painless anterior abdominal wall swelling which was exaggerated on exertion. She had earlier presented to the referring hospital with 6 months history of recurrent pelvic pain. She was evaluated and a diagnosis of a right ovarian cyst was made for which she was counseled and had laparotomy and excision of the cyst. She, however, had dull right flank pain and fever in the first-week post-surgery and by the second week, the leakage of urine and abdominal swelling were noticed. She had no comorbidities. We found a middle-aged woman who was afebrile, well-nourished, and body mass index of 23.9kg/m2. She had a wide poorly healed midline abdominal scar extending from the pubic symphysis to the umbilicus with an underlying incisional hernia; facial defect of 12cm. In the middle of the scar lies hyperemic 0.5cm fistula with continuous egress of urine. Figure 1 shows the clinical image at presentation with the fistula. The abdomen was non-tender, with no palpable mass. Other systemic examinations were normal. An assessment of iatrogenic ureterocutaneous fistula with an incisional hernia was made. Abdominopelvic ultrasound finding was that of a right hydroureteronephrosis and normal left kidney and bladder while computerized tomography (CT) Urography scan with intravenous contrast showed a dilated right renal pelvis and proximal ureter with spillage of contrast in the region of the right middle ureter. The contrast was also noted in the peritoneal cavity and the anterior abdominal wall. In addition, defect in layers of the lower anterior abdominal wall was also noted. Figure 2 and Figure 3 depicts the CT- Urography images of the patient. She was counseled and prepared for exploration and reconstruction of the urinary tract and anterior abdominal wall. Intraoperative findings were abdominal scar, widely separated recti and facial defect of 15cm, multiple fibrous adhesions between small bowel loops and the anterior abdominal wall, an 8cm epithelialized fibrous tract between the anterior abdominal wall and the right ureter at the level of the distal right sacroiliac joint surrounded by fibrous adhesions with dilation of the ureter proximal to the point of adhesions. Figure 4shows the intraoperative findings The renal function was normal. She had excision of the fistulous tract, right ureteroneocystostomy with a Boari Flap and psoas hitch as well as a double J stenting of the right ureter. Also, the anterior abdominal defect was repaired using tension-free tissue repair. She had an uneventful and satisfactory postoperative recovery. The clinical image at the second week after reconstruction is shown in Figure 5.
This presentation has brought to fore the possible preventable complications that may follow a pelvic surgery. Gynecological procedures account for most of the reported ureteric injuries as seen in this case. The unrecognized injury led to the fistula, intrabdominal infection, poor wound healing, and subsequently, an incisional hernia developed. These morbidities warranted reconstruction of the urinary tract, increased cost of healthcare prolonged hospital stay, and increased duration of recuperation and time off work. Besides, the social and psychological burden of the urinary fistula is enormous. Ureteric injuries are relatively rare and a ureterocutaneous fistula following these injuries is even rarer [5]. Most injuries based on the type of injury results in obstruction of the ureter (ligation or ischemia of the ureter) or a flank mass from a urinoma( transection or resection of the ureter). Also, most reported cases of iatrogenic ureterocutaneous fistulae are following procedures in the urinary tract such as partial nephrectomy, renal transplant, or urinary diversion [5,6]. A few reports of ureterocutaneous fistula due to iatrogenic ureteric injury during non-urological procedures such an appendectomy and aortofemoral bypass are in literature [7]. The recommended treatment of this fistula based on its location is a ureteric re-implantation [1]. However, due to the loss of about 8cm of the distal ureter, a Boari flap was raised and a vesico-psoas hitch was done for a tension-free reconstruction. The presence of the urinary fistula and high risk of infection was the basis of the choice of a tension-free repair of the incisional hernia following adequate patient counseling on the risk of recurrence. This is because although mesh repair has a lower risk of recurrence, tissue repair should be considered when the risk of infection or seroma collection is high [8]. Prevention of these ureteric injuries is important. Caution and a low threshold during dissection or ligation of vessels in the region of the course of the ureter may help in observing the principles of primum non nocere. The use of preoperative ureteric catheters or lighted ureteric stents to help in the identification of the ureters as well as iatrogenic ureteric injuries during anticipated complex pelvic procedures have been found to reduce the incidence of these injuries [9]. A high index of suspicion is important to prevent and recognize this injury when it occurs intraoperatively which is the best time for its repair [4].
Iatrogenic ureteric injury and ureterocutaneous fistula may occur following gynecological procedures. Use of good surgical techniques, and in addition, preoperative ureteric stenting, when the risk of inadvertent ureteric injury is high may reduce the incidence of these preventable surgical complications and associated morbidities.
The authors declare no competing interests.
All the authors have read and agreed to the final manuscript.
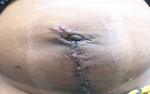
Figure 1: clinical Image at presentation showing the stoma of the fistula
Figure 2: depicts axial CT urography images of the patient. A) right hydronephroses; (B,C) lateral deviation of right distal ureter with intraperitoneal extravasation of contrast; D) extravavsation of contrast through surgical site unto anterior abdominal wall
Figure 3: depicts coronal and sagtital reformatted CT urographic images; A) right hydronephroses; B) lateral deviation of right the middle ureter; C) extravasatiion of contrast intraperitoneally and via surgical site on abdominal wall; D) incisional hernia
Figure 4: intraoperative image with the green arrow depicting the dilated ureters and the blue arrow showing the post-operative adhesions
Figure 5: clinical image at the second post-operative week
- Burks FN, Santucci RA. Management of iatrogenic ureteral injury. Ther Adv Urol. 2014 Jun;6(3):115-24. PubMed | Google Scholar
- Blackwell RH, Kirshenbaum EJ, Shah AS, Kuo PC, Gupta GN, Turk TMT. Complications of Recognized and Unrecognized Iatrogenic Ureteral Injury at Time of Hysterectomy: A Population Based Analysis. J Urol. 2018 Jun;199(6):1540-1545. PubMed | Google Scholar
- Chan JK, Morrow J, Manetta A. Prevention of ureteral injuries in gynecologic surgery. Am J Obs Gynecol. 2003 May;188(5):1273-7. PubMed | Google Scholar
- Abboudi H, Ahmed K, Royle J, Khan MS, Dasgupta P, N'Dow J. Ureteric injury: a challenging condition. Nat Rev Urol. 2013 Feb;10(2):108-15. PubMed | Google Scholar
- Saslawsky M, Niederberger C, Schacht M, Prinz LR. Ureterocutaneous Fistula: a case report of treatment by subtrigonal Injection of polytetrafluoroethylene (Sting Procedure). J Urol. 1989 Nov;142(5):1310-1. PubMed | Google Scholar
- Vázquez Alonso F, Vicente Prados FJ, Pascual Geler M, Funes Padilla C, Cózar Olmo JM, Tallada Buñuel M. Ureterocutaneous fistula after nephrectomy: two cases. Actas Urol Esp. 2008;32:931-933. PubMed
- Huang J, Wadhwa H, Blecha M, Yonover P. Urology Case Reports Case Report of a Ureterocutenous Fistula Post Aortobifemoral Bypass Graft Removal in a Patient With Obstructive UPJ Calculus. Urol Case Reports. 2017;13:53-54. PubMed | Google Scholar
- Sanders DL, Kingsnorth AN. The modern management of incisional hernias. BMJ. 2012; 344. PubMed | Google Scholar
- Jha S, Coomarasamy AA. Ureteric injury in obstetric and gynaecological surgery. Obstet Gynaecol. 2011;6:203-208. Google Scholar