A rare case of cobb syndrome in a black person managed conservatively
Luxwell Jokonya
Corresponding author: Luxwell Jokonya, Department of Surgery, Division of Neurosurgery, University of Zimbabwe, College of Health Sciences, Harare, Zimbabwe 
Received: 01 May 2020 - Accepted: 21 May 2020 - Published: 11 Jun 2020
Domain: Neurology (general),Neurosurgery
Keywords: Cobb syndrome, vascular skin lesion, paraplegia
©Luxwell Jokonya et al. PAMJ Clinical Medicine (ISSN: 2707-2797). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Luxwell Jokonya et al. A rare case of cobb syndrome in a black person managed conservatively. PAMJ Clinical Medicine. 2020;3:50. [doi: 10.11604/pamj-cm.2020.3.50.23247]
Available online at: https://www.clinical-medicine.panafrican-med-journal.com//content/article/3/50/full
A rare case of cobb syndrome in a black person managed conservatively
Luxwell Jokonya1,&
1Department of Surgery, Division of Neurosurgery, University of Zimbabwe, College of Health Sciences, Harare, Zimbabwe
&Corresponding author
Luxwell Jokonya, Department of Surgery, Division of Neurosurgery, University of Zimbabwe, College of Health Sciences, Harare, Zimbabwe
Cobb syndrome is a rare metameric disorder, characterized by either an angioma or an arteriovenous malformation of the spinal cord, with an associated vascular skin lesion of the same metamere. They are less than 50 cases reported to date. Most of the cases were in whites. We report a case of an 18-year-old black man who presented with sudden severe backache with rapidly progressing paraplegia and bowel and bladder symptoms. Magnetic resonance imaging showed an arteriovenous malformation from forth to the twelfth thoracic vertebrae (T4-T12). He had a congenital cutaneous vascular back lesion covering the same dermatomes. This is diagnostic of Cobb´s syndrome.
Cobb syndrome is an exceedingly rare non inherited condition characterised by vascular cutaneous lesions in the same metamere with a spinal arteriovenous malformation (SAVM) or a spinal angioma [1-3]. It was first described in 1890 by Berenbruch [4], and further described by Cobb in 1915 [5]. There are less than 50 documented cases of Cobb´s syndrome to date [3,5]. The actual incidence may be much higher since only symptomatic patients were documented. Post mortem studies suggest a possibly higher incidence of this syndrome [1]. It may be possible therefore that most of these subtle skin lesions are missed and hence a diagnosis of Cobb syndrome is not often made. No racial predilection has been noted but most case reports had been white patients. There is a slight male preponderance. Presentation is usually in childhood and adolescence [6]. Cobb syndrome is suspected when you get spinal neurological deficits in a patient with a congenital cutaneous vascular lesion [4]. Most cases however are asymptomatic. The cutaneous manifestations typically are present as port-wine stains or angiomas. However, reports exist of angiokeratomas, angiolipomas, and lymphangioma circumscriptum [1,7]. The cutaneous lesion can be very faint and may be more pronounced when the patient performs a valsalva manoeuvre. The increased abdominal pressure causes preferential filling of the cutaneous angioma. Unilateral cutaneous lesion may tell the side of the feeding artery in the spinal arteriovenous malformation. The level of cutaneous lesion does not necessarily correspond to the level of the arteriovenous malformation [7].
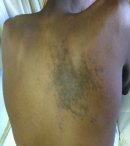
An 18-year-old previously well black man, presented with a 2-day history of severe backache and paraplegia. He was awoken one morning by a sharp, sudden and severe lower back ache. At that time, he felt numbness in his right lower limb and on trying to mobilise discovered that it was now weak. The weakness in his right leg gradually worsened as the day progressed. By the following morning he could not move both lower limbs and had bilateral numbness up to the waist. He then developed acute urinary retention and also lost bowel continence. The previous year he had an almost similar event of back ache associated with paraesthesia of the right lower limb. This however spontaneously resolved completely in a few days. On examination he was fully conscious and apyrexial. He had normal power and sensation in the upper limbs. He had a distinct sensory level at L1, with flaccid paralysis of all muscle groups of the lower limbs. All reflexes below T4 were absent, with loss of anal tone. There was a large vascular lesion covering from T4 up to T7 dermatomes on the back (Figure 1). The lesion was enhanced by performing valsalva manoeuvres. Full blood count, urea and electrolytes done were normal. Lumber puncture was essentially normal except for a slightly increased cerebral spinal fluid protein of 0.48 grams per litre. See Figure 2 for Magnetic resonance imaging (MRI). An angiogram was not available. The patient received high dose steroids and showed gradual recovery of function until he returned to premorbid state.
The presentation of our case was similar to that of some documented in literature. Having had a cutaneous lesion for as long as he can remember, our patient developed a sudden onset of back ache associated with paraparesis and sensory disturbances. The sudden onset of the pain is highly suggestive of a bleed in the spinal arteriovenous malformation. This can be further supported by the isolated elevated protein count. The area of increased signal in the non-enhanced T1 image could also add to confirm a bleed. The fact that the patient had a similar episode several years back could also suggest that this was not the first bleed. Even though an angiogram could not be done, the presence of a cutaneous vascular lesion in addition to a magnetic resonance image with vascular flow voids in itself can be diagnostic of Cobb syndrome [2,5]. However this does not remove the need for an angiogram as this is important in identifying the malformation and can also provide an opportunity for embolization either as a sole treatment modality or in combination with surgery. Treatment modalities range from mere observation, use of steroids, surgery and more recently embolization [2,3,6]. At the time of initial examination our patient was in spinal shock as evidenced by complete absence or reflexes including bulbocavernosus reflex. Since this was at least the second time the arteriovenous malformation had bled, he had more chances of disease progression with a real risk of ending up completely paraplegic [4]. Hence an angiogram and possible embolization was indicated. An angioma was unlikely based on the magnetic resonance image, which showed typical flow voids that one would see in an arteriovenous malformation.
Cobb syndrome is a rare metameric disorder. It can also be found in the black population, where the cutaneous vascular lesions may not be so obvious. If actively searched out for this condition may not be as rare as currently thought. Its management remains a challenge particularly in low resource countries.
The author declare no competing interests.
LJ conceived the idea and wrote up the manuscript. The author have read and approved the final version.
Many thanks to the Parirenyatwa Hospital Neurosurgery team involved in the management of the case and also to the patient for allowing us to publish his case.
Figure 1: vascular skin lesion
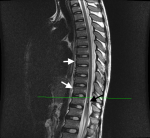
Figure 2: MRI scan showing multiple flow voids in and around the spinal cord, (white arrows. A focal hyperintense area (black arrow) T9/T10 Junction (line)
- Tubridy Clark M, Brooks EL, Chong W, Pappas C, Fahey M. Cobb Syndrome: a case report and systematic review of the literature. Pediatr Neurol. 2008;39(6):423-5. PubMed | Google Scholar
- Akio Soeda, Nobuyuki Sakai, Koji Iihara, Izumi Nagata. Cobb syndrome in an infant: Treatment with endovascular embolization and corticosteroid therapy: Case report. Neurosurgery. 2003;52(3):711-5. PubMed | Google Scholar
- Pal P, Ray S, Chakraborty S, Dey S, Talukdar A. Cobb syndrome: a rare cause of paraplegia. Ann Neurosci. 2015;22(3):191-3. PubMed | Google Scholar
- Miyatake S, Kikuchi H, Koide T, Yamagata S, Nagata I, Minami S et al. Cobb´s syndrome and its treatment with embolization. Case report. J Neurosurg. 1990;72(3):497-9. PubMed | Google Scholar
- Doppman JL, Wirth F, Giovanni C, Ommaya A. Value of cutaneous angiomas in the arteriographic localization of spinal cord artreriovenous malformations. N Engl J Med. 1969 Dec 25;281(26):1440-4. PubMed | Google Scholar
- Johnson WD, Petrie MM. Variety of spinal vascular pathology seen in adult Cobb syndrome: Report of 2 cases. J Neurosurg Spine. 2009;10(5):430-5. PubMed | Google Scholar
- Bhatt A, Kalina P. Cobb Syndrome: a case report with review of clinical and Imaging findings. Open J Clin Diagnostics. 2014;04(04):237-42. Google Scholar