Abernethy syndrome a rare cause of dyspnea a case report
Camelia Neftah, El Bakkari Asaad, Nazik Allali, Chat Latifa
Corresponding author: El Bakkari Asaad, Radiology Department of the Children Hospital of Rabat, Rabat, Morocco 
Received: 06 May 2020 - Accepted: 18 May 2020 - Published: 11 Jun 2020
Domain: Radiology,Pediatric cardiology,Pediatric gastroenterology
Keywords: Dyspnea, abernethy malformation, porto systemic shunt
©Camelia Neftah et al. PAMJ Clinical Medicine (ISSN: 2707-2797). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Camelia Neftah et al. Abernethy syndrome a rare cause of dyspnea a case report. PAMJ Clinical Medicine. 2020;3:51. [doi: 10.11604/pamj-cm.2020.3.51.23333]
Available online at: https://www.clinical-medicine.panafrican-med-journal.com//content/article/3/51/full
Abernethy syndrome a rare cause of dyspnea a case report
Camelia Neftah1, El Bakkari Asaad1,&, Nazik Allali1, Chat Latifa1
1Radiology Department of the Children Hospital of Rabat, Rabat, Morocco
&Corresponding author
El Bakkari Asaad, Radiology Department of the Children Hospital of Rabat, Rabat, Morocco
Abernethy malformations are rare vascular abnormalities of the splanchnic venous system. It´s about a congenital portosystemic shunts which result from the persistence of embryonic vessels. We report a case of type II Abernethy malformation which associates a hyperplasic intrahepatic portal vein, a deviation of blood to the inferior vena cava with side-by-side extrahepatic communication, in addition we noted an abnormal return of the pulmonary veins, and ectopic drainage of the superior vena cava into the right atrium. With uncommon dyspnea, congenital extrahepatic shunts are more and more diagnosed due to improved imaging techniques, but most are discovered by chance.
Abernethy malformations are rare vascular anomalies of the splanchnic venous system. They consist of congenital portosystemic shunts and result from persistence of the embryonic vessels. We report a case of Abernethy malformation type II who associate a hyperplasic intra hepatic portal vein, a blood diversion to the inferior veina cava with a side to side extra hepatic communication, in addition we noted an abnormality of pulmonary veins return, and an ectopic draining of the superior veina cava in the right atrium.In front of an uncommon dyspnea congenital extrahepatic shunts are being diagnosed with increased frequency as imaging techniques become more and more refined but most of them are incidentally discovered.
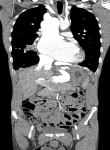
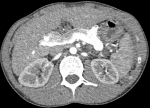
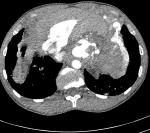
A 24-year-old male was admitted to our hospital with dyspnea stage III of the New York heart association (NYHA). Patient´s medical history talked about a cerebral abscess at 7 year old. The physical examination revealed a chest distention with mitral insufficiency sound at the cardiac auscultation. No fever, oedema of arms or legs, jaundice, skin rash was noted. The abdomen was soft with no organomegaly or clinical ascites. Electrocardiogram (ECG) showed a complete arrhythmia by atrial fibrillation ACFA with heart rate of 110 per minute. Blood tests revealed no abnormalities. A transthoracic chest ultrasound showed a left atrial enlargement (LAE) with abnormal venous return. A thoraco-abdominal enhanced CT was advised, revealed portosystemic shunts (PSS) between portal vein (PV), spleno-mesaraic trunk (SMT) and superior vena cava (SVC) which are all delated, with three big veins connecting the portal system with the superior vena cava. All of these veins flow into a common collector (24mm) behind the left atrium which goes to the right of the spine to flow into the superior vena cava (Figure 1). It showed an important enlargement of inferior vena cava, superior mesenteric vein and upper hepatic veins. Also, a partial abnormal pulmonary venous return with superior pulmonary veins flowing into the superior vena cava (Figure 2). Varicose collaterals are also described connecting the vena cava and upper hepatic veins with the right and left diaphragmatic areas (Figure 3).
John Abernethy was the first to give account of an absent portal vein with accompanying congenital mesenterico-caval shunt in 1793 [1-3]. There are two main types of Abernethy malformations that have been described initially divided by G Morgan and R Superina in type I: end-to-end shunts and type II: side-to-side shunts [2]. In type I shunts (end-to-end), there is a congenital absence of the portal vein with a complete diversion of portal blood into systemic veins (inferior vena cava, renal veins, or iliac veins). These are further subdivided into: type Ia: separate drainage of the superior mesenteric vein and splenic vein into systemic veins type Ib: superior mesenteric vein and splenic vein join to form a short extra-hepatic portal vein which drains into a systemic vein (inferior vena cava, right atrium or iliac veins) In type II shunts (side-to-side), there is a hypoplasic portal vein with portal blood diversion into the inferior vena cava through a side-to-side, extrahepatic communication. The portal vein is normally formed between weeks 5 and 10 of embryogenesis by selective involution of the peri-intestinal vitelline venous loop. On the other hand, the IVC, is developed as an amalgamation of several embryologic venous channels with the common hepatic vein, which gives rise to the hepatic segment of the IVC. Excessive involution between fetal weeks 4 and 10 can result in complete absence of the portal vein, and this leads to CEPS with abnormal mesenteric-caval connection. Incomplete involution produces duplication of the portal vein [4].
Early diagnosis and treatment are important to prevent complications. Imaging plays an important part in diagnosing these congenital extrahepatic portosystemic shunts. Computed tomography with dynamic contrast-enhanced angiography is the main exam to get the diagnosis, classify the pathology and search of the associated malformation. CTA with arterial and venous phase isolation allows mapping of the course of the shunt and accurate classification, It demonstrates the congenital extra hepatic portosystemic shunts. The presence or absence of intrahepatic portal vein branches forms the basis of this classification [5]. In Type I CEPS malformations, an end-to-side extrahepatic portosystemic shunt exists, with total diversion of portal mesenteric blood into the IVC, renal or iliac vein, and complete absence of intrahepatic portal vein branches. Type II CEPS malformations constitute incomplete bypass of the liver, and a side-to-side extrahepatic shunt exists between the splanchnic and systemic circulation, with the portal vein being hypoplastic and thin intrahepatic portal vein radicals present in hepatic parenchyma. In general, the treatment of congenital malformations of the portal system depends on the type of shunt, the presenting symptoms, coexisting congenital anomalies, hepatic insult, complications and comorbidity. The most important determinant appears to be the type of the lesion [1]. However, no surgical strategy has been described for adult patients with a type II shunt. When these patients have serious symptoms, such as hepatic encephalopathy or collateral bleeding, the shunt should be closed soon, which may help avoid the development of mesenteric venous congestion. Reported treatments of Abernethy malformations include operations, such as closure of shunt, liver nodule resection, liver transplantation, and interventional treatment, such as percutaneous balloon-occluded obliteration, percutaneous trans-catheter embolization with metallic coils or plug, stent placement, and stent-graft placement [6, 7].
Abernethy malformation is a congenital extra hepatic portosystemic shunt that is developed between the porto-mesenteric vasculature and the systemic veins. There are two main types of Abernethy malformations. The clinic may be variable and related to the associated anomalies.
The authors declare no competing interests.
All the authors have read and agreed to the final manuscript.
Figure 1: coronal-angio CT section shows an important enlargement of the upper hepatic veins and the superior mesenteric veins
Figure 2: axial angio-CT section shows an important dilatation of the extra hepatic portal trunc, an absence of intra hepatic veins and a peri splenic collateral vein
Figure 3: axial angio-CT section shows a multiples collateral veins connecting veina cava and upper hepatic veins with right and left peri diaphragmatic areas
- Howard E, Davenport M. Congenital extrahepatic portocaval shunts-The Abernethy Malformation. J of Pediatr Surg. 1997;32(3):494-497. PubMed | Google Scholar
- Morgan G, Superina R. Congenital absence of the portal vein: two cases and a proposed classification system for portasystemic vascular anomalies. J Pediatr Surg. 1994;29(9):1239-41. PubMed | Google Scholar
- Abernethy J. Account of Two Instances of Uncommon Formation in the Viscera of the Human Body: From the Philosophical Transactions of the Royal Society of London. 1797;7:100-108. PubMed | Google Scholar
- Marks C. Developmental basis of the portal venous system. Am J Surg. 1969;117(5):671-681. PubMed | Google Scholar
- Niwa T, Aida N, Tachibana K, Shinkai M, Ohhama Y, Fujita K et al. Congenital absence of the portal vein: Clinical and radiologic findings. J Comp Assist Tomogr. 2002;26(5):681-686. PubMed | Google Scholar
- Sanada Y, Urahashi T, Ihara Y, Wakiya T, Okada N, Yamada et al. The role of operative intervention in management of congenital extrahepatic portosystemic shunt.Surgery. 2012;151(3): 404-11. Google Scholar
- Franchi-Abella S, Branchereau S, Lambert V, Fabre M, Steimberg C, Losay J et al. Complications of congenital portosystemic shunts in children: therapeutic options and outcomes. J Pediatr Gastroenterol Nutr. 2010 Sep;51(3):322-30. PubMed | Google Scholar