Ileosigmoid knot during pregnancy: unusual cause of intestinal obstruction
Mohamed Anajjar, Yasser El Brahmi ,Faisal El Mouhafid, Aziz Fadili, Mohammed Elfahssi , Mbarek Yakka, Abderrahman Elhjouji, Abdelkader Ihirchiou, Aziz Zentar, Abdelmounaim Ait Ali
Corresponding author: Mohamed Anajjar, Department of Visceral Surgery II, Mohammed V Military Teaching Hospital, Ryad, Rabat, Morocco 
Received: 27 Apr 2020 - Accepted: 18 May 2020 - Published: 15 Jun 2020
Domain: Emergency medicine,Gastroenterology,General surgery
Keywords: Sigmoid, volvulus, ileosigmoid knot, pregnant, bowel, obstruction
©Mohamed Anajjar et al. PAMJ Clinical Medicine (ISSN: 2707-2797). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Mohamed Anajjar et al. Ileosigmoid knot during pregnancy: unusual cause of intestinal obstruction. PAMJ Clinical Medicine. 2020;3:54. [doi: 10.11604/pamj-cm.2020.3.54.23130]
Available online at: https://www.clinical-medicine.panafrican-med-journal.com//content/article/3/54/full
Ileosigmoid knot during pregnancy: unusual cause of intestinal obstruction
Mohamed Anajjar 1,&, Yasser El Brahmi1, Faisal El Mouhafid1, Aziz fadili1, Mohammed Elfahssi1, Mbarek Yakka1, Abderrahman Elhjouji1, Abdelkader Ihirchiou1, Aziz Zentar1, Abdelmounaim Ait Ali1
&Corresponding author
Ileosigmoid knotting also known as compound volvulus or double volvulus, is a rare cause of intestinal obstruction. In this condition the ileum wraps around the base of the sigmoid colon and forms a knot, the condition is serious, generally progressing rapidly to gangrene. The occurrence during pregnancy is very rare and the diagnosis is difficult because of its infrequency and atypical radiographic findings. This report describes a case in a 23-year-old female and through a literature review describes the management of this rare condition.. .because better understanding of the problem, increases probabilities of preoperative diagnosis and improves the prognosis.
Ileosigmoid knot (ISK) is a rare surgical condition where patients present with acute intestinal obstruction. This condition is also known as compound volvulus because small bowel loops wrap around the base of the sigmoid colon, obstructing it, the occurrence during pregnancy is very rare and the diagnosis is difficult because of its infrequency and atypical radiographic findings. We present a case of pregnant women with ileosigmoid knot unfortunately diagnosed late, which caused the loss of the fetus outline our management, and discuss the surgical options available.
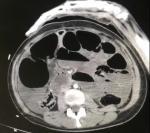
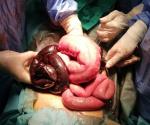
A 23-year-old woman at 12 weeks of pregnancy presented to our clinic in shock with history of abdomen pain and non-passage of flatus or stools for 2 days. She had neither a medical or surgical history and had thus far experienced a normal pregnancy. Her vitals were blood pressure 80/40 mmHg, pulse rate 127/min regular, respiratory rate of 29 bpm and a temperature of 37.7oC. Her abdomen was distended with marked generalized tenderness, guarding, rebound tenderness and absent bowel sounds. Vaginal and digital rectal examinations were unremarkable. The patient was resuscitated with IV fluids and vasopressin. Laboratory investigations showed a white blood cell count of 22,000/mm3, hemoglobin level of 8.9 g/dl. Transvaginal ultrasonography revealed a dilated bowel with ascitic fluid and no sign of cardiac fetal activity A diagnosis of an acute bowel obstruction complicated of fetal death was made. Enhanced abdominal computed tomography (CT) was performed to reach an accurate diagnosis and revealed a dilated loop of the sigmoid colon in the right lower abdomen, suggestive of a sigmoid volvulus. There is also a radial distribution of several dilated, fluid-filled bowel loops (Figure 1). Urgent exploratory laparotomy was done, the peritoneal cavity contained about a litre of foul-smelling dark fluid. A 360o sigmoid volvulus was encountered (Figure 2), with several loops of necrotic small bowel wrapped around a viable mega-dolichosigmoid colon next to a gravid uterus. The volvulus was detorsed, the necrotic bowel was resected, obliged by the hemodynamic instability no anastomosis was permitted, sigmoid resection was deferred and a ileostomy was done the patient expulse the fetus , made an uneventful recovery and was discharged after 7 days ,she had prophylactic sigmoidectomy to prevent next volvulus and the closure of ileostomy after 12 weeks from the day of discharge.
Parker has been credited for describing the first patient of ileosigmoid knot in 1845. It is common in Africa, Asia, Middle East and South Africa. It is more common in males (80.2%) than females and presents at a mean age of 40 years (range 4-90 years). ISK in pregnancy is rare. There are only 9 reported cases of ISK in pregnancy in literature between 1967 and 2009; in literature the reported incidence of ISK in pregnancy ranges from 3.2% to 5.9%of all ISK cases and 12.5% to 36.4% of ISK cases in female patients [1]. Alver [2] classified the ileosigmoid knot into 3 types, based on mechanism of formation of knot. In Type I (commonest), ileum is the active component, wrapping itself around the sigmoid colon (passive component) to form the knot in clockwise or anti-clockwise direction. In Type II, the sigmoid colon (active component) wraps itself around a loop of ileum (passive component) in clockwise and anticlockwise direction. In Type III, ileocaecal segment (active component) wraps itself around the sigmoid colon (passive component). Types I and II have been classified into A and B, depending on whether knot was clockwise or anticlockwise.
The etiology of intestinal knotting, including ileo-ileal knotting, is unknown. The condition is most common in areas where small intestinal and sigmoid volvulus is common. This may be related to the diet in the area that is bulky and high in fiber [3]. It may also be associated with a long mesentery of small bowel, freely mobile small bowel and a long sigmoid colon on a narrow pedicle are believed to predispose to the condition. Late pregnancy trans mesenteric herniation, ileocolic intussusception and a floating caecum are possible predisposing factors [4]. The predominant symptoms and signs of presentation include abdominal pain and tenderness, abdominal distension, nausea and vomiting, rebound tenderness and shock, [5]. Despite the critical condition, preoperative diagnosis is not easy. The diagnostic difficulty is partly caused by the unfamiliarity of this rare entity and the confusing and self-contradictory features of the disease. While clinical features such as vomiting suggest small bowel obstruction, the radiographic findings are that of colonic distension, which is uncommon in small bowel obstruction. Radiographically, ISK is often mistaken for simple sigmoid volvulus. However, unlike sigmoid volvulus, attempts to deflate the distended colon using a sigmoidoscope or a flatus tube, often fails in ISK. This is because the ileum tightly envelops the base of sigmoid colon, defying any such attempt. These three features of the clinical picture of small bowel obstruction, radiographic evidence of predominately large bowel obstruction, and inability to insert a sigmoidoscope could possibly form a useful diagnostic triad.
The radiographic findings of the ileosigmoid knot are sporadically described [6], and include a dilated loop of the pelvic colon, the evidence of a small intestinal obstruction, and the retention of feces in an undistended proximal colon. Computerized tomography(CT): can reveal the findings of a sigmoid volvulus including the characteristic whirl sign created by the twisted intestine and mesocolon [6]. CT can also reveal signs of bowel ischemia caused by strangulation such as pneumatosis. However, the findings of an ileosigmoid knot are not easily detected because the ileal twist is higher in the abdomen than the location of a sigmoid volvulus. The whirl is visible on more contiguous slices than that of the sigmoid volvulus. which it is often confused with. It is important to differentiate between the two because ISK is a surgical emergency in which endoscopic reduction is contraindicated [7]. Treatment: management should begin at presentation with aggressive fluid resuscitation and correction of electrolyte and acid-base imbalances where present. Empiric antibiotic therapy should commenced early due to the high incidence of bowel gangrene and associated bacterial translocation, and continued after the operation especially in gangrenous bowel [8]. The operative procedure undertaken should be based on the degree of physiological disturbance, operative risk assessment and intraoperative findings Patients who are unstable should have damage control laparotomy as the default procedure. This involves enblock resection of the volvularized segment with care not to spill bowel contents, closure of the bowel, peritoneal lavage and temporary abdominal closure [8].
A planned second look laparotomy should be performed 24 - 48 hours later based on the patient´s response to resuscitation. Patients who are stable intra-operatively, may have a definitive procedure done at the initial laparotomy. If both loops are viable, the knot may be undone by sigmoid enterotomy and traction of the sigmoid loop may be performed. This procedure may also be selected when the sigmoid colon alone is viable. When the ileum and the sigmoid colon are gangrenous, it can be difficult to untie the knot, and rupture of the gangrenous loop could lead to spillage of toxic bowel contents. Therefore, intestinal clamps should be applied before dissection or resection of the knot followed by resection of both the loops. Primary anastomosis of the small bowel is preferable, but if the terminal ileum is gangrenous and within 10 cm of the ileocecal valve, an end-to-end anastomosis should be avoided because of the risk of leak [5]. The distal stump can be closed and end-to-side ileocecostomy can be performed as safer option Resection of the sigmoid colon is often advised in all instances even when it is viable [5]. Recurrent volvulus or repeat knotting due to redundancy of the loop may cause gangrene after surgery. In the past, a Hartmann operation or a covering colostomy was advocated to avoid the risk of fecal leak from colonic anastomosis. However, recent data suggest that primary colonic anastomosis may be under taken safely when the history is short and the remaining bowel is clean, well vascularized, and undistended. The reported mortality from ISK varies from 0% to 48% (mean, 35.5%) The mortality figures are generally related to the duration of symptoms, the presence or absence of gangrene and the general status of the patient, including the presence of septicemic shock [5].
Unfamiliarity with the disease and atypical radiographic findings make preoperative diagnosis rare. However, it should be always considered in the differential diagnosis of patients with signs and symptoms of small bowel obstruction. Because the condition is associated with high rate of morbidity and mortality, a high index of suspicion remains the most useful tool. A prompt diagnosis and early surgical intervention significantly improve outcomes.
The authors declare no competing interests.
All authors have contributed to the writing of this manuscript. All the authors have read and approved the final version of this manuscript.
Figure 1: axial CT image showing dilated loop of the sigmoid colon, suggestive of a sigmoid volvulus, there is also a radial distribution of several dilated, fluid-filled bowel loops
Figure 2: intraoperative image several loops of necrotic small bowel wrapped around a viable mega-dolichosigmoid colon
- Maunganidze AJV, Mungazi SG, Siamuchembu M, Mlotshwa M. Ileosigmoid knotting in early pregnancy: A case report. International journal of surgery case reports. 2016;23:20-22. PubMed | Google Scholar
- Chakma SM, Singh RL, Parmekar MV, Singh GH, Rudrappa S. Ileosigmoid knot-A Surgeon´s Nightmare. Journal of clinical and diagnostic research: JCDR. 2013;7(12):2986. PubMed
- Abebe E, Asmare B, Addise A. Ileo-ileal knotting as an uncommon cause of acute intestinal obstruction. Journal of surgical case reports. 2015 Aug 6;2015(8):rjv102. PubMed | Google Scholar
- Mungazi SG, Mutseyekwa B, Sachikonye M. A rare occurrence of viability of both small and large bowel in ileosigmoid knotting: A case report. International journal of surgery case reports. 2018;49:1-3. PubMed | Google Scholar
- Mandal A, Chandel V, Baig S. Ileosigmoid knot. Indian Journal of Surgery. 2012;74(2):136-142. PubMed | Google Scholar
- Lee SH, Park YH, Won YS. The ileosigmoid knot: CT findings. American Journal of Roentgenology. 2000;174(3):685-687. PubMed | Google Scholar
- Bain K, Lelchuk A, Nicoara M, Meytes V. A unique surgical emergency: ileosigmoid knotting. AME case reports. 2018 Jun 8;2:29. PubMed | Google Scholar
- Ooko PB, Saruni S, Oloo M, Topazian HM, White R. Ileo-sigmoid knotting: a review of 61 cases in Kenya. Pan African Medical Journal. 2016 Apr 15;23:198. PubMed | Google Scholar