Pure plantar isolated navicular bone dislocation: an exceptional case
Mohammed Hajjioui, Najia Hajjioui, Mohamed Ouahidi, Toufik Cherrad, Hassan Zejjari
Corresponding author: Mohammed Hajjioui, Orthopedic Surgery and Traumatology, Military Hospital Moulay Ismail BP 50000 Meknes, Morocco 
Received: 07 Mar 2020 - Accepted: 30 May 2020 - Published: 16 Jun 2020
Domain: Orthopedic surgery
Keywords: Plantar dislocation, navicular bone, surgery
©Mohammed Hajjioui et al. PAMJ Clinical Medicine (ISSN: 2707-2797). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Mohammed Hajjioui et al. Pure plantar isolated navicular bone dislocation: an exceptional case. PAMJ Clinical Medicine. 2020;3:57. [doi: 10.11604/pamj-cm.2020.3.57.22209]
Available online at: https://www.clinical-medicine.panafrican-med-journal.com//content/article/3/57/full
Pure plantar isolated navicular bone dislocation: an exceptional case
Mohammed Hajjioui1,&, Najia Hajjioui2, Mohamed Ouahidi3, Toufik Cherrad3, Hassan Zejjari3
&Corresponding author
Pure dislocation of the tarsal navicular bone is an exceptional and serious injury. It´s a trauma emergency. Few cases have been reported in the literature. The mechanism and the treatment of these lesions present particularities. We report the case of a young patient who presented with pure dislocation without a fractured navicular bone following a sports accident. The surgical treatment allowed a good functional result.
Pure plantar isolated navicular dislocation is an exceptional and serious lesion, most often occurring during a violent trauma to the foot. It´s a trauma emergency. Few cases have been reported in the literature. The objective of our work is to discuss in the light of the literature and through a case of an isolated plantar dislocation of the navicular, the mechanism of this infrequent entity, its therapeutic modalities and its evolutionary profile
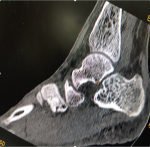
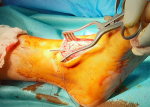
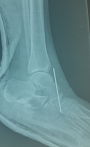
A young 23-year-old patient presented to the emergency department with pain in his left foot following a mechanical fall. The patient fell after loss of control, the left forefoot stuck in a ladder, which caused a dorsal hyperflexion probably combined with an external rotation mechanism. On examination, there was a marked deformation with edema and pain in the middle of the foot. The skin, vascular and nervous examination of the foot was without abnormality. The patient´s radiograph showed a dislocation of the navicular and was supplemented by a CT scan which had objectified a pure plantar navicular dislocation without fracture (Figure 1). The reduction was open to the eye before the reduction by external maneuver failed. The approach to the lesion was dorsomedial (Figure 2). Surgical exploration revealed dislocation of the navicular bone without fracture, with a cartilaginous coating on the joint surfaces intact. The reduction in dislocation was maintained by a talo-naviculo-cuneiform Kirschner wire (Figure 3). ). An additional immobilization by plastered splint was put in place for six weeks. The pins are removed at the end under local anesthesia. The functional rehabilitation of the foot lasted five weeks. At one year of follow-up, the functional result was good with a stable and painless movable foot.
Pure navicular dislocation is very rare because of its geometry and the security with which the tarsal navicular is maintained by ligaments, bones, tendons and neighboring muscles [1]. Severe violent force is necessary to cause this lesion and is the result of a force transmitted along the metatarsal rays while the ankle is in the equine [2]. In our case, the mechanism seems to be a dorsal hyperflexion wound on the talus foot, causing a capsiligament rupture with plantar dislocation without associated fracture. Isolated dislocation of the tarsal navicular without navicular fracture seems impossible. The stability of the navicular bone is ensured by a very solid dorsal and plantar ligament system, which makes it more vulnerable to fracture than dislocation [3]. This dislocation can be done either superolateral or infero-lateral, depending on whether the direction of the trauma is dorsal or plantar [4]. The spontaneous reduction in dislocation pushes the navicular bone at the talo-navicular joint which will dislocate in various medial positions depending on the movement of the forefoot and the residual insertion of the soft parts [1]; this is similar to the mechanism of perilunar luxation of the carpus. The most reported mechanism is plantar compression [4,5] in which the position of the foot and the direction of the trauma will determine the direction of dislocation.
Main and Jowett [2] predicted that the longitudinal compression forces transmitted by the metatarsals will drive out the navicular bone, the dorsal ligaments of which are ruptured by the plantar flexion of the foot. The radiological and especially CT scan examines the extent of the bone lesions. A three-dimensional reconstruction provides a relief representation of the bone parts and allows us to see the type of dislocation and to understand the lesion mechanism. Magnetic resonance imaging (MRI) is useful for the diagnosis of ligament lesions and to assess the vascular risk of the bone by declaring the residual insertion of the soft tissue [6]. Closed hearth reduction is doomed to failure, several authors report open hearth reduction with internal fixation using Kirschner wire and that there is no justification for arthrodesis [1]. Main and Jowett report that many patients behave well even with joint damage. Some offer orthopedic treatment with a plantar orthosis and an adjusted sole to relieve symptoms at the start of the loading phase once the plaster is removed. This could reduce the need for possible arthrodesis. Kirschner's wires should be removed after at least eight weeks to avoid the complication of resubluxation. The arthrodesis must be reserved for cases of serious lesions such as major cartilage lesions in particular in the elderly and avascular necrosis associated with dislocation of the navicular tarsus judged to be 25% [4,7] and it is favored by the reduction of reduction and complete disinsertion of the soft parts, in particular of the posterior tibial tendon, the residual insertion of the latter being able to be the only source brought vascular to the bone. Adequate reduction can improve prognosis, but the outcome also depends on damage to cartilage and adjacent structures caused by trauma
Pure isolated dislocation of the navicular bone is an exceptional and serious lesion. It is an emergency occurring during a high energy foot trauma. The positive diagnosis is essentially based on the radiological assessment. Early surgical management with an anatomical reduction often allows a good functional result to be obtained.
The authors declare no competing interests.
All the authors have read and agreed to the final manuscript.
Figure 1: CT scan of the ankle and foot in sagittal view showing a plantar dislocation of the navicular bone
Figure 2: intraoperative image showing the medial dorso approach
Figure 3: postoperative control profile radiology of the surgical procedure
- Vaishya R, Patrick JH. Isolated dorsal fracture dislocation of tarsal navicular injury. J Bone Joint Surg Br. 1991;22(1): 47-48. Google Scholar
- Main BJ, Jowett RL. Injuries of the mid tarsal joint. Bone Joint Surg. 1975;57(1):78-89. Google Scholar
- Freund KG. Isolated dislocation of the tarsal navicular. 1989 Mar;20(2):117-8. PubMed | Google Scholar
- Dhillon MS, Nagi ON. Total dislocation of the navicular: are they ever isolated injuries. J Bone Joint Surg Br.1999 Sep;81(5):881-5. PubMed | Google Scholar
- Kennedy JG, Maher MM, Stephens MM. Fracture dislocation of the tarsal navicular bone: A case report and proposed mechanism of injury. Foot Ankle Surg.1999;5(3):167-70. Google Scholar
- Preidler KW, Peicha G, Laitai G, Seibert FJ, Fock C, Szolar DM et al. Conventional radiography, CT, and MR imaging in patients with hyperflexion injuries of the foot: diagnostic accuracy in the detection of bony and ligamentous changes. AJR Am J Roentgenol. 1999 Dec;173(6):1673-7. PubMed | Google Scholar
- Berman S. Complete dislocation of tarsal scaphoid. JAMA. 1924;83(3):181-183. Google Scholar