Radiological aspect of hydranencephaly: a case report
Soukaina Wakrim
Corresponding author: Soukaina Wakrim, Radiology Department, Faculty of Medicine and Pharmacy, Ibn Zohr University, Agadir, Morocco 
Received: 01 Apr 2020 - Accepted: 18 May 2020 - Published: 19 Jun 2020
Domain: Pediatrics (general)
Keywords: Hydranencephaly, imagery, diagnosis
©Soukaina Wakrim et al. PAMJ Clinical Medicine (ISSN: 2707-2797). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Soukaina Wakrim et al. Radiological aspect of hydranencephaly: a case report. PAMJ Clinical Medicine. 2020;3:62. [doi: 10.11604/pamj-cm.2020.3.62.22604]
Available online at: https://www.clinical-medicine.panafrican-med-journal.com//content/article/3/62/full
Radiological aspect of hydranencephaly: a case report
Soukaina Wakrim1,&
&Corresponding author
Hydranencephaly is a severe destructive cerebral lesion with absence of the cerebral hemispheres. It can be the consequence of a vascular accident, infection, maternal exposure to toxins, or death of a co-twin in a monochorionic pregnancy. The typical US appearance is a large cystic structure replacing the fetal brain, but the brainstem and the thalami are preserved. It is usually identified at midgestation, but it also can occur later in pregnancy. The prognosis is very poor.
Hydranencephaly is characterized by the absence of the cerebral hemispheres, with incomplete or absent cerebral falx. The fluid-filled sac that replaces the brain is formed by the leptomeninges and the cerebrospinal fluid [1]. The prognosis is universally poor, and death usually occurs within the first year of life. Termination of pregnancy should be advised if possible. Hydranencephaly is considered to be sporadic, with a recurrence in cases of infectious disorders [2].
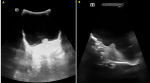
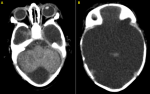
We present the case of newborn admitted at J7 of life, male, from a followed pregnancy estimated at 40 SA, no notion of consanguinity, delivery by caesarean section of a 35 year old mother; first gestures first parities. The infectious history was positive. Apgar at birth is 10/10. Since birth, the newborn presented with major macrocrania, early vomiting, and a refusal to suckle in a context of apyrexia. Clinical examination finds a subicteric neonate hypotone with a sunset look. Transfontanelle Ultrasonography was objectived an extreme hydrocephalus and cerebellum preserved (Figure 1). Cranial Computed Tomography without intravenous injection identified the hydranencephaly which demonstrates the fluid-filled sac almost completely replacing the cerebral hemispheres. The cerebellum was preserved (Figure 2).
Hydranencephaly is defined as the absence of the cerebral hemispheres; the hemispheres are replaced by a fluid-filled sac [3]. It is rare. The exact cause of hydranencephaly is not clear. However, it has been proposed infarction (Occlusion of the internal carotid arteries or of the middle cerebral arteries), diffuse hypoxic-ischemic brain necrosis and Infection [4, 5]. All imaging modalities, including US, computed tomography, and magnetic resonance, can be used to identify the features of hydranencephaly. In all cases, the imaging findings are the same. The cerebral tissue is absent. The thalami, brain stem, and cerebellum are preserved. In many cases, islands of residual tissue are seen at the occipital poles and orbitofrontal regions. The falx is usually present, and the cranial cavity is filled with fluid [6-8]. Hydranencephaly is associated with a poor prognosis, and most of the affected infants do not survive beyond the first year of life [9]. Hydranencephaly must be distinguished from extreme hydrocephalus, porencephaly, and alobar holoprosencephaly. The presence of even minimal frontal cerebral cortex is indicative of hydrocephalus. Color Doppler may be useful for differential diagnosis because anterior and middle cerebral arteries are not visualized in hydranencephaly [10, 11].
Understanding the typical imaging manifestations of hydranencephaly, in the antenatal period, permits a more specific and accurate diagnosis. Wherever, it allows for discussion of medical termination of the pregnancy if possible.
The author declares no competing interests.
The author read and agreed on the final manuscript.
Figure 1: transfontanelle ultrasonography: coronal and axial section showing the fluid-filled sac almost completely replacing the cerebral hemispheres
Figure 2: cranial computed tomography without intravenous injection (axial section): the fluid-filled sac almost completely replacing the cerebral hemispheres and the cerebellum was preserved
- Myers RE. Brain pathology following fetal vascular occlusion: an experimental study. Invest Ophthalmol. 1969 Feb;8(1):41-50. PubMed | Google Scholar
- Fernàndez F, Pèrez-Higueras A, Hernàndez R, Verdu A, Sánchez C, González A et al. Hydranencephaly after maternal butane-gas intoxication during pregnancy. Dev Med Child Neurol. 1986 Jun;28(3):361-3. PubMed | Google Scholar
- Larroche JC, Droulle P, Delezoide AL, Narcy F, Nessmann C. Brain damage in monozygous twins. Biol Neonate. 1990;57(5):261-78. PubMed | Google Scholar
- Christie JD, Rakusan TA, Martinez MA, Lucia HL, Rajaraman S, Edwards SB et al. Hydranencephaly caused by congenital infection with herpes simplex virus. Pediatr Infect Dis. 1986;5(4):473-8. PubMed | Google Scholar
- Sarno M, Sacramento GA, Khouri R, do Rosário MS, Costa F, Archanjo G et al. Zika virus infection and stillbirths: a case of hydrops fetalis, hydranencephaly and fetal demise. PLoS Neglected Tropical Diseases. 2016;10(2):e0004517. PubMed | Google Scholar
- Barkovich AJ. Pediatric Neuroimaging. 4th ed Philadelphia, PA: Lippincott Williams and Wilkins. 2005;191Y192. Google Scholar
- Dublin AB, French BN. Diagnostic image evaluation of hydranencephaly and pictorially similar entities, with emphasis on computed tomography. Radiology. 1980 Oct;137(1 Pt 1):81-91. PubMed | Google Scholar
- Greene MF, Benacerraf B, Crawford JM. Hydranencephaly: US appearance during in utero evolution. Radiology. 1985 Sep;156(3):779-80. PubMed | Google Scholar
- Wheeler TC. Hydranencephaly. Accessed October 5, 2012.
- Kurtz AB, Johnson PT. Case 7: Hydranencephaly. Radiology. 1999 Feb;210(2):419-22. PubMed | Google Scholar
- Poe LB, Coleman LL, Mahmud F. Congenital central nervous system anomalies. Radiographics. 1989 Sep;9(5):801-26. PubMed | Google Scholar