Management of infectious complications of a neglected craniocerebral wound in rural areas: about a case
Haboubacar Chaibou Sode, Assoumane Ibrahim, Hamissou Nouri, Brice Sawa, Hamidou Yaya, Moussa Younoussa, Sanoussi Samuila
Corresponding author: Haboubacar Chaibou Sode, Neurosurgery Department, Niamey National Hospital, Republic of Niger, Niamey, Niger 
Received: 25 Mar 2020 - Accepted: 18 May 2020 - Published: 23 Jun 2020
Domain: Neurosurgery
Keywords: Traumatic brain injury, complications, infection, surgery
©Haboubacar Chaibou Sode et al. PAMJ Clinical Medicine (ISSN: 2707-2797). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Haboubacar Chaibou Sode et al. Management of infectious complications of a neglected craniocerebral wound in rural areas: about a case. PAMJ Clinical Medicine. 2020;3:67. [doi: 10.11604/pamj-cm.2020.3.67.22494]
Available online at: https://www.clinical-medicine.panafrican-med-journal.com//content/article/3/67/full
Case report 
Management of infectious complications of a neglected craniocerebral wound in rural areas: about a case
Management of infectious complications of a neglected craniocerebral wound in rural areas: about a case
Haboubacar Chaibou Sode1,2,&, Assoumane Ibrahim3, Hamissou Nouri4, Brice Sawa1, Hamidou Yaya2, Moussa Younoussa2, Sanoussi Samuila1,5
&Corresponding author
Infection remains a major risk of the opened traumatic brain injury due to cutaneous losses, osteitis, meningitis or collected cranio-encephalic suppurations that might occur in the evolution. We report the case of a 3 years old patient, admitted in our unit during September 2017 for an opened head trauma with initial loss of consciousness following motorbike-pedestrian traffic accident. The admission period was ten days. The diagnosis of an infected neglected opened trauma brain injury was made, and he benefited from medical and surgical treatment but the follow up was complicated by infection at various stages with several medico-surgical care. The evolution is finally favorable after 98 days in hospital. This observation portrays the difficulties of management of crânio-encephalic wounds in rural areas; the delay in consultation exposes to complications that are difficult to manage.
The opened traumatic brain injury brings the external environment in communication with the osteomeningeal envelopes and sometimes with the brain itself. Although hemorrhage is a real immediate threat in such lesion, infection remains a major risk as it is responsible of cutaneous losses, osteitis, meningitis or collected cranioencephalic suppurations. This is mainly linked to the delay in treatment [1]. We report the case of a patient, admitted to the regional hospital of Tahoua in September 2017 for opened trauma of the skull with an admission period of ten (10) days which is late; he presented several complications despite antibiotic therapy and repetitive surgical procedures.
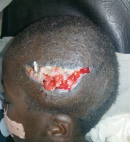
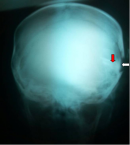
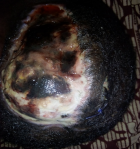
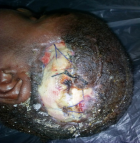
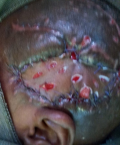
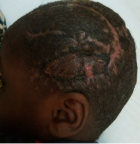
This is a 3-year-old patient victim of an opened head trauma with initial loss of consciousness following a motorbike pedestrian traffic accident in his village. He was conducted to the closest Integrated Health Centre where he received local care (wound dressing) and antibiotics during three days. A week later, he was referred to Tahoua RH surgery department for better management. On admission the clinical examination noticed a conscious, febrile child with a temperature oscillating between 38.5°C to 39°C, a broca´s aphasia and right hemiplegia. There was a large decaying wound with cerebral matter, cerebrospinal fluid leak and bone chips located at the left temporo-parieto-occipital region (Figure 1). The AP view of skull X-ray showed a bone discontinuity and a left temporal transfixing fragment (Figure 2). As of its admission we instituted a medical treatment made of a bi antibiotic therapy based on a 3rd generation cephalosporin associated with metronidazole, the serum and the tetanus vaccine. The child was operated upon urgently. In the theater, under general anesthesia we proceeded to the trimming of the wound whose enlargement allowed us to discover the multi fragmentary fronto-temporal fracture with a piece of transfixing bone. We proceeded to the extraction of the bony scales, which allowed us to discover a large wound of the dura mater of approximately 5 cm with irregular edges requiring a plasty with galea taken far from the wound. There was also a loss of skin substance but the detachment allowed us to suture without tension after handing over the bony scales. We did a superficial and deep sample for bacteriological examination but that was not conclusive. The patient benefited a 250 ml of whole blood iso group iso rhesus. A few days later, we noticed loose stitches with a parietal suppuration and cerebrospinal fluid (CSF) leakage (Figure 3). We had carried out local care accompanied with bi antibiotic therapy according to the previous protocol for ten days. Because of CSF leakage through the wound, we had taken the patient back to the theater, where under general anesthesia we had trimmed the wound. We had found a channel through which CSF was leaking. We had closed the hole using galea followed by a skin closure by a few stitches. The aftermath was further complicated by loose stitches, skin necrosis and osteitis without CSF leakage (Figure 4). We admitted him in the theater to proceed with the removal of the necrotic skin and the infected bone fragment, the brain not being exposed, we had continued the local care until the budding of the wound. The patient was taken back to the theater for skin closure by a total skin graft taken at the suprapubic level (Figure 5 and Figure 6). The physiotherapy was concomitant during all this care which lasted ninety eight days. The evolution at 03 months was marked by a considerable improvement in his clinical state (hemiplegia and aphasia) and a bone cement plasty is planned later.
Open traumatic brain injury are relatively less frequent compared to the numerous consequences of head trauma. They represent 11.11% in the general population [2] and 13% in children. There is a predominance of men and an average age of patients in the literature of around five years [3] close to that of our patient. The patient we present is admitted to our unit with a delay of 10 days which is too long, this can be explained by the poor health coverage in the country. E C Rasolonjatovo [4] has also reported in a 39 patients series a long delay which explained occur of infection. This long delay is alleged in the literature as source of infectious complications or even sepsis [5,6]. The diagnosis of a opened traumatic brain injury was obvious due to the presence of cerebral parenchyma, of bone fragments in an oozing wound. On admission the patient was conscious Glasgow 15/15, this is explained in the literature by the fact that in trauma brain injury, the traumatic energy is largely absorbed at the point of impact by the scalp and the skull causing fractures and limits the diffusion of this energy in the cerebral parenchyma; this would alleviate the intensity of disturbances of consciousness [3,4]. There is also a repercussion with a focal sign of hemiplegia and aphasia which are observed in case of left temporo-parietal location of the wound. On the work up level we contented ourselves with the simple radiography of the skull which is the only examination we had. This examination nevertheless made it possible to reveal a transfixing fragment whose removal could be hemorrhagic in damaging a cortical vessel. This examination is no more used in the current practice of the management of this pathology because it provides limited information on the lesion assessment as pointed out by several authors. [3,7]. The patient is admitted to the department with an infectious syndrome made of intermittent fever which fluctuates between 38.5°C and 39°C, hyperleukocytosis 18,600, a CRP greater than 6 mg with anemia at 9 g/dl.
We quickly instituted bi antibiotic therapy based on the combination of a 3rd generation cephalosporin and imidazole. E C Rasolonjatovo [4] also uses the same protocol and A. B. Thiam used 3rd generation cephalosporin alone in first line in Dakar [8]. If the need for antibiotic prophylaxis is trivial, the choice of the molecule and the duration of treatment are subject to debate. Currently, in French armies, antibiotic prophylaxis of opened traumatic brain injury is based on the use of amoxicillin-clavulanic acid for a period of at least 48 hours. This period can be extended to 5 days or more if persistence of liquorrhea [9]. DIOP also uses the amoxicillin - clavulanic acid combination [10]. The intraoperative sampling of superficial and deep pus did not allow us to identify a germ despite the obvious infection. This can be explained by the limited technical platform of the laboratory which is that of a poorly equipped regional hospital. According to the literature, the main germs incriminated are, in order of frequency, Staphylococcus aureus, various Streptococcus, gram negative bacilli and anaerobes (Clostridium). [11]. We continued this antibiotic therapy for two weeks, clinical improvement was noted the day after the intervention, and the control biology gives white blood cells at 7,900 elements, hemoglobin at 10.6 g/dl and CRP positive Infection is the major complication of open trauma; often pneumococcal meningitis; brain abscess; wall infection, risk factor of osteitis are frequently cited in the literature. [3,12]. The second intervention was indicated because of the CSF leak. This secondary complication is the subject of a wait-and-see attitude for some authors for 24 to 48 hours, but in the absence of spontaneous drying up they recommend surgery because of increased risk post traumatic meningitis [3]. Jonathan [13] considers that the persistence of the CSF leak beyond 24 hours after a head trauma can be the cause of meningitis, sometimes recurrent, and in most cases requires surgery. Moreover, opened trauma brain injuries are associated with a high risk of early (10%) or delayed (40%) secondary epilepsy [14]. Cobodon [15] specifies that in cranio-cerebral wounds, the frequency can reach 50% in the case of infected cranio-cerebral wounds. Our patient throughout his stay did not have such a crisis. We nevertheless systematically administered sodium valproate at a dose of 30 mg per kg for one month.
This case is a perfect illustration of the morbidities of this pathology, the infection lies in for medium and long term consequences. This is the case of our patient who had several infectious complications which earned him several surgeries as such lengthening his stay in hospital with social and economic consequences for the parents and the community. This case illustrates the management difficulties of an opened traumatic brain injury encountered in rural areas, the delay in consultation exposing to complications that are difficult to manage.
The authors declare no competing interests.
All the authors have read and agreed to the final manuscript.
Figure 1: decaying wound containing pus, brain matter, bone scraps
Figure 2: A-P view of the skull X-ray showing the fracture (white arrow) and the transfixing fragment (red arrow) on the left side
Figure 3: novel suppuration; loose threads, CSF leakage
Figure 4: cutaneous necrosis and osteitis without CSF leakage
Figure 5: full skin graft
Figure 6: good skin graft taking
- Quenuma JKM, Quenumab B, Fanouab L, Akadiriab R, Gnangnonab A. Management of cranio-cerebral wounds in Cotonou. (Republic of Benin). 2013;59(6):251.
- Kanikomo D, Sogoba Y, Dama M, Coulibaly O, Diarra MS, Thiam AB et al. Epidemiological, clinical and therapeutical study of depressed skull fractures in the neurosurgical department of the Gabriel Toure Hospital: about 72 cases. Mali Med. 2015;30(3):7-12. PubMed | Google Scholar
- Salaou O, Naja A, Aboudou Y, Ibahiouin K, Elkamar A, El Az-hari A. Management of cranio-cerebral wounds in children in 60 cases. AJNS. 2006;255(1):1-9.
- Rasolonjatovo EC, Tsiaremby MG, Rakotondraibe WF. Management of craniocerebral wounds at CHU Joseph Ravoahangy Andrianavalona, Antananarivo-Madagascar. Rev anesth-Réanim Med Urg Toxicol. 2016;8(2):4-7.
- Cushing H. Notes on penetrating wounds of the brain. Br Med J.1918 Feb 23;1(2982):221-6. PubMed | Google Scholar
- Jefferson G. The physiological pathology of gunshot wounds of the head. Br Med J Surg. 1919;7(26):262-89. Google Scholar
- Aenderl I, Gashaw T, Siebeck M, Mutschler W. Head injury--a neglected public health problem: a four-month prospective study at Jimma University Specialized Hospital, Ethiopia. Ethiop J Health Sci. 2014;24(1). PubMed | Google Scholar
- Thiam AB, Mudekereza PS, Ndoye N. Cranio-cerebral wounds anatomo-clinical aspects about 39 cases. Journal of Neurosurgery October. 2013;80:246-50.
- Management of cerebrospinal fluid leaks. J Trauma. 2001 Aug;51(2 Suppl):S29-33. PubMed
- Diop A, Tine I, Hope L. Cranioencephalic wounds: epidemioclinical and therapeutic aspects in Dakar (Senegal). AJNS. 2011;30(1):1-10.
- Antibiotic prophylaxis for penetrating brain injury. J Trauma. 2001;51:S34-40. PubMed
- Houdart R. Craniocerebral wounds. Pathologie Chirurgicale Masson, 3rd edition, Paris. 1978:294-297.
- Friedman JA, Ebersold MJ, Quast LM. Post traumatic cerebrospinal fluid leakage. World J Surg. 2001 Aug;25(8):1062-6. PubMed | Google Scholar
- Daban JL, Delmas JM, Dulou R, Debien B. Craniocerebral wounds: from hospital in Afghanistan to care in France. Emergency. 2012.
- Cobodon F, Richer E. Late complications and sequelae of head trauma. Rev prat. 1985;35(37):2287-2292. PubMed