A 14-year-old female with multi-organ failure and cutaneous manifestations of COVID-19: a case report from Mthatha, South Africa
Asanda Ndudane, Lindubuhle Beba, Khaled Elmezughi, Chukwuma Ekpebegh, Thozama Dubula
Corresponding author: Khaled Elmezughi, Department of Internal Medicine, Walter Sisulu University, Mthatha, South Africa 
Received: 24 Aug 2020 - Accepted: 16 Sep 2020 - Published: 23 Sep 2020
Domain: Infectious disease,Internal medicine
Keywords: COVID-19, SARS-CoV-2, cutaneous manifestations, skin rash, exanthem Mthatha, South Africa
©Asanda Ndudane et al. PAMJ Clinical Medicine (ISSN: 2707-2797). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Asanda Ndudane et al. A 14-year-old female with multi-organ failure and cutaneous manifestations of COVID-19: a case report from Mthatha, South Africa. PAMJ Clinical Medicine. 2020;4:37. [doi: 10.11604/pamj-cm.2020.4.37.25729]
Available online at: https://www.clinical-medicine.panafrican-med-journal.com//content/article/4/37/full
Case report 
A 14-year-old female with multi-organ failure and cutaneous manifestations of COVID-19: a case report from Mthatha, South Africa
A 14-year-old female with multi-organ failure and cutaneous manifestations of COVID-19: a case report from Mthatha, South Africa
Asanda Ndudane1, Lindubuhle Beba1, Khaled Elmezughi1,&, Chukwuma Ekpebegh1, Thozama Dubula1
&Corresponding author
We report on a 14-year-old black South African female with severe COVID-19 disease who presented with cutaneous manifestations. She developed multiorgan failure and succumbed to the disease.
The Corona virus disease (COVID-19) is defined as an illness caused by a novel coronavirus now called severe acute respiratory syndrome virus 2 (SARS-COV 2)) which was first identified amid an outbreak of respiratory illness cases in Wuhan City, Hubei Province, China [1]. The SARS-CoV-2, virus pathophysiology is not completely known, but is thought that it infects human cells by attaching to angiotensin converting enzyme 2 (ACE2) receptors, which suggest that it may have a similar pathogenesis to previous SARS [2,3]. The organs considered more vulnerable to SARS-CoV-2 infection include the lungs, heart, esophagus, kidneys, bladder, and ileum [4]. The clinical presentation of COVID-19 could range from mild respiratory infection to a severe pneumonia leading to acute respiratory distress syndrome which is potentially fatal. The most reported manifestations include fever, fatigue, dry cough, anorexia, myalgias, dypsnoea, sore throat, rhinorrhea, loss of smell, loss of taste, nausea, and diarrhea [5-7]. There are increasing reports of various cutaneous manifestations in patients with COVID-19, but they remain sparse, non-specific, and devoid of any prognostic significance [8,9]. A case study of cutaneous manifestations of COVID-19 from Lombardy in Italy found most cutaneous presentations to be erythematous skin rash (77.8%) with few cases of urticarial (16.7%) and vesicle formation (5.6%) [8]. Currently the most common cutaneous manifestations of COVID-19 are maculopapular and papulovesicular rashes while the less commonly reported skin lesions include livedo reticularis and petechiae [10]. We herein, report on a young female with severe COVID-19 disease and skin rashes at presentation who died shortly after presentation and before skin biopsy could be done for a histological diagnosis of the skin lesions.
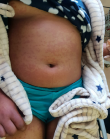
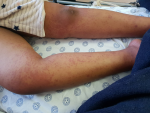
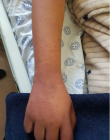
A 14-year-old black South African female presented to the Emergency Unit of Nelson Mandela Academic Hospital (NMAH) in the Eastern Cape Province of South Africa with five days history of sore throat and frontal headaches, low grade fever. She had initially consulted a general practitioner (GP) and was prescribed medications that she received for four days on outpatient basis. She had then developed a generalized erythematous urticarial rash with accompanying shortness of breath. Examination revealed low grade fever of 38°C, tachypnea with respiratory rate of 28 breaths per minute and oxygen saturation of 84% while breathing room air. She was tachycardic with pulse rate of 125 beats per minute. Blood pressure was elevated at 141/121 mmHg. Generalized erythematous rash involving the face, trunk, back and all the limbs was observed as shown on Figure 1, Figure 2 and Figure 3. The palms and soles were spared. There was no conjunctival hyperemia or oral mucosal ulcerations. Grade III tonsillitis was observed as well. Her chest examination revealed crepitations in both middle and lower lung zones. All other systems were unremarkable.
Laboratory results at presentation confirmed COVID-19 by RT-PCR (reverse transcriptase polymerase chain reaction from a nasopharyngeal swab). she had markedly elevated inflammatory markers and acute phase reactants: WBC of 41.2 x 109/L (3.90-12.60), CRP of 502 mg/L (<10), ESR of 56mm/hr (0-10), Serum ferritin of 1285 ug/L (13-68), Haemoglobin of 12g/dl (12-15) and platelet count of 197 x 109 /L (186-454). There was elevated urea and creatinine of 19.4 mmol/L (1.4-5.4) and 254 umol/L (40-72) respectively. Blood glucose was normal. She was HIV negative. Chest radiograph revealed bilateral infiltrates consistent with bronchopneumonia. The assessment was that of severe COVID-19 disease with multiorgan involvement: bronchopneumonia, renal failure, and skin rash. She was reviewed by a dermatologist who described it as a widespread maculopapular erythematous skin rash with no mucosal involvement. She was admitted into the intensive care unit and started on supplemental oxygen, intravenous fluids, broad spectrum antibiotics, anticoagulation, antihistamine, parenteral and topical steroids. She demised soon after admission.
There are reports of different types of skin rashes in COVID-19 patients, including petechial and purpuric changes, transient livedo reticularis, and acro-ischemic lesions [8-10]. Whether these manifestations are causally related to COVID-19 remains unclear, since both viral infections and adverse drug reactions are frequent causes of exanthems. This case is significant for two reasons: first, the unusual occurrence of severe and subsequent fatal COVID-19 disease in a teenager with no previously documented co-morbid illness. The second is the cutaneous manifestation which is rarely reported. It is not clear what predisposed our patient to severe COVID-19 disease. There was no documented history of co-morbidities such as diabetes, hypertension, chronic lung disease or immunosuppressive conditions that may have predisposed her to a fatal outcome [11,12]. She however, had elevated blood pressure and it is not certain if it was acute or chronic. Her rash is likely due to COVID-19 as it was present when she presented to the GP. She received injections of tramadol, metronidazole, metoclopramide and Depo-medrol at the GP. It is likely that Depo-medrol which is a glucocorticoid was administered for the rash. At present, there are limited data regarding cutaneous manifestations of SARS-CoV-2 infection. Given the importance of prompt COVID-19 diagnosis during a global pandemic, it is necessary to highlight the possible dermatologic manifestations and to characterize their morphology. Our case report contributes to extending the reports of cutaneous manifestations of COVID-19 and severe disease in the young people and COVID-19 should be considered in the initial differential.
We have reported on a young female with severe COVID-19 disease and cutaneous manifestation who succumbed to her illness. Rash may rarely be a presenting symptom of COVID-19 and should always be kept in mind.
The authors declare no competing interests.
The authors have contributed to the conception, drafting, and revising of this manuscript. They have all read and approved the final manuscript.
The authors are grateful to the staff of Nelson Mandela Academic Hospital (NMAH) for their assistance as well as the patient´s family for kindly collaborating and agreeing to the formation of this article for academic enrichment against the COVID-19 pandemic.
Figure 1: COVID-19 skin rash; maculopapular erythematous skin rash on the abdomen and part of chest
Figure 2: cutaneous manifestations of COVID-19 in the legs
Figure 3: cutaneous manifestation of COVID-19 in the right hand and arm
- CDC. 2019 Novel Coronavirus, Wuhan, China. CDC. Accessed on August 18, 2020.
- Lu R, Zhao X, Li J, Niu P, Yang B, Wu H et al. Genomic characterization and epidemiology of 2019 novel coronavirus: implications for virus origins and receptor binding. Lancet. 2020: 395(1022);565-574. PubMed | Google Scholar
- Yan R, Zhang Y, Li Y, Xia L, Guo Y, Zhou Q. Structural basis for the recognition of the SARS-CoV-2 by full length human ACE2. Science. 2020;367(6485):1444-1448. PubMed | Google Scholar
- Zou X, Chen K, Zou J, Han P, Hao J, Han Z. Single-cell RNA-seq data analysis on the receptor ACE2 expression reveals the potential risk of different human organs vulnerable to 2019-nCoV infection. Front Med. 2020;14(2):185-192. PubMed | Google Scholar
- Marco Cascella, Michael Rajnik, Arturo Cuomo, Scott C Dulebohn, Raffaela Di Napoli. Features, evaluation and treatment coronavirus(COVID-19). In: Stat Pearls Treasure Island (FL): StatPearls Publishing. 2020. PubMed
- Huang C, Wang Y, Li X, Ren L, Zhao J, Hu Y et al. Clinical features of patients infected with 2019 novel coronavirus in Wuhan, China. Lancet. 2020; 395(10223):497-506. PubMed | Google Scholar
- Wang D, Hu B, Hu C, Zhu F, Liu X, Zhang J et al. Clinical characteristics of 138 hospitalized patients with 2019 novel coronavirus-infected pneumonia in Wuhan, China. JAMA. 2020;323(11):1061-1069. PubMed | Google Scholar
- Recalcati S. Cutaneous manifestations in COVID-19: a first perspective. Eur Acad Dermatol Venereol. 2020;34(5):e212-213. PubMed | Google Scholar
- Zheng Y, Lai W. Dermatology staff participate in fight against Covid-19 in China. J Eur Acad Dermatol Venereol. 2020;34(5):e210-211. PubMed | Google Scholar
- Sachdeva M, Gianotti R, Shah M, Bradanini L, Tosi D, Veraldi S et al. Cutaneous manifestations of Covid-19: report of three cases and a review of literature. J Dermatol Sci. 2020;98(2):75-81. PubMed | Google Scholar
- Zhou F, Yu T, Du R, Fan G, Liu Y, Liu Z et al. Clinical course and risk factors for mortality of adult inpatients with COVID-19 in Wuhan, China: a retrospective cohort study. Lancet. 2020;395(10229):1054-1062. PubMed | Google Scholar
- CDC COVID-19 Response Team. Preliminary estimates of the prevalence of selected underlying health conditions among patients with coronavirus disease 2019-United States, 12-march 2020. Morbidity and Mortality Weekly Report.. Accessed on August 18, 2020.