Barriers and facilitators of research in Cameroon (Part I) - an e-survey of physicians
Ulrick Sidney Kanmounye, Joel Noutakdie Tochie, Mazou Temgoua, Aimé Noula Mbonda, Francky Teddy Endomba, Jan René Nkeck, Cynthia Wafo, Ferdinand Ndom Ntock, Desmond Tanko Jumbam
Corresponding author: Ulrick Sidney Kanmounye, Global Neurosurgery Initiative, Program in Global Surgery and Social Change, Harvard Medical School, Boston, MA, USA 
Received: 27 Jun 2020 - Accepted: 24 Jul 2020 - Published: 08 Oct 2020
Domain: Health Research
Keywords: Barriers, Cameroon, facilitators, physician, research
©Ulrick Sidney Kanmounye et al. PAMJ Clinical Medicine (ISSN: 2707-2797). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Ulrick Sidney Kanmounye et al. Barriers and facilitators of research in Cameroon (Part I) - an e-survey of physicians. PAMJ Clinical Medicine. 2020;4:58. [doi: 10.11604/pamj-cm.2020.4.58.24608]
Available online at: https://www.clinical-medicine.panafrican-med-journal.com//content/article/4/58/full
Barriers and facilitators of research in Cameroon (Part I) - an e-survey of physicians
Ulrick Sidney Kanmounye1,2,3,&, Joel Noutakdie Tochie4,5,, Mazou Temgoua6,7, Aimé Noula Mbonda8,9,, Francky Teddy Endomba10,11, Jan René Nkeck5, 6,7, Cynthia Wafo4, Ferdinand Ndom Ntock12, Desmond Tanko Jumbam13
&Corresponding author
Introduction: high-quality health research is needed in Africa to find innovative solutions for health care challenges on the continent. However, research output remains low, and obstacles to research poorly understood. This study aimed to determine the facilitators and barriers to health research among Cameroonian physicians.
Methods: an e-survey was conducted among a convenience sample of Cameroonian physicians between May 23, 2020, to June 07, 2020. The Likert scale responses were coded and used to calculate a Preference Score (PS). The median and total PS were used to categorize and rank the barriers and facilitators. The Mann-Whitney U and Kruskal-Wallis H tests were used with a threshold of significance of 0.05. Also, the Bonferroni test was used to correct the P-value (0.025).
Results: two hundred and ninety five physicians aged 29.2 ± 3.5 years responded to the survey. Most participants were male (56.3%), French speakers (75.9%), and general practitioners (56.6%). Respondents published 2.4 articles (95% CI: 1.5-3.2), and significant barriers to research included the lack of a research team (Kruskal-Wallis H=6.29, P=0.012) and difficulties to get an ethical clearance (Kruskal-Wallis H=5.57, P=0.018). Grant availability was an important determinant of research involvement (Kruskal-Wallis H=3.90, P=0.048).
Conclusion: high-quality and context-appropriate research can help tackle the high burden of disease in sub-Saharan Africa. To increase research output among Cameroonian physicians, strategies should minimize the barriers and maximize the facilitators identified in this study.
While much progress has been made since most African countries gained their independence in the sixties, they continue to consistently rank lowest among the highest burden of infectious, non-communicable, and injury-related diseases [1-3]. Cumulatively, average life expectancy at birth remains the lowest in the world, while infant mortality rates, maternal mortality rates, and under-five mortality rates, though decreasing slowly, remain high [4]. Despite this global disproportion in disease burden, which necessitates significant research to identify context-specific innovations and solutions, health research capacity in many African countries remains significantly low and underfunded [5]. Health research activity in African countries is relatively low when compared to high-income countries due to several challenges that can be broadly grouped into infrastructural, institutional, financial, and educational challenges [5]. African researchers often face several infrastructural challenges such as limited laboratory space, lack of equipment, and necessary supplies needed to conduct research [5,6]. Institutional barriers, such as the lack of clearly defined career pathways for trained research scientists or students interested in research careers, have also been noted [5,7]. Furthermore, in many African countries, there are educational barriers that prevent proper training of health research, including inadequate curricula for students and continued education for professionals [5]. Furthermore, limited funding is a major barrier to health research on the continent. Currently, collectively African countries only spend about 0.5% of their Gross Domestic Products (GDP) on research and development, significantly lower than the 2.2% global average [8,9]. Investments in health research by national governments in most African countries has been severely restricted. Few African countries have been able to deliver on their 2006 African Union commitment to raise their national expenditure on research and development to at least 1% of their national GDPs [10].
In addition, the private sector, mainly pharmaceutical companies, have been reticent to invest in many low-income countries due to seemingly limited prospects for profits even if innovations and treatments are found [11]. All these barriers have led to a significant shortage of health researchers in sub-Saharan Africa. The WHO estimates that there are only 21 health researchers per million inhabitants in Africa compared to about 225 health researchers per million inhabitants in Europe [12]. Local research is particularly necessary for adapting evidence-based practices and interventions to the local contexts. Recent studies suggest that the most unsuccessful public health and clinical initiatives that have been ventured in Africa were not sufficiently or adequately adapted to the local context and hence not adopted and sustained by the local community [13,14]. For this reason, more recent emphasis has been placed on evidence-based practices and interventions being informed by locally-sourced and rigorous scientific evidence through the use of such methods as implementation science [15]. To resolve these challenges, African countries through regional institutions like the Africa Center for Disease Control, have set research agendas and are increasing support for local researchers [16,17]. The rationale being that context-specific findings from studies led and conducted by researchers in Africa are more likely to resolve Africa-specific issues than the studies led solely by non-African institutions and researchers. This can only be possible with more high-quality research. Although over the last two decades, there has been an increase in scholarly output by African researchers, this research output still lags significantly behind their colleagues from other regions [18]. The realities and challenges highlighted above have been anecdotally referenced by health researchers in Cameroon. However, primary research studies assessing the barriers and challenges faced by health researchers in Cameroon have been scant. Such studies would be necessary to advocate for increasing the quality and output of research in Cameroon. To this end, the primary objective of this study was to identify facilitators and barriers to engaging in health research among physicians in Cameroon. Findings from this study are aimed at informing interventions and policies to improve health research quality and quantity in Cameroon.
Study population: the study was specifically designed to assess barriers and facilitators to health research among physicians working in Cameroon. Cameroon is a sub-Saharan African country located in West-Central Africa, with a population of about 25 billion people and a GDP per capita of US$1,533 [19]. It is classified as a lower-middle-income country by the World Bank. The average life expectancy at birth is 65.2 years and 61.0 years for females and males, respectively, while the top causes of death and disability remain HIV/AIDS, malaria, and neonatal disorders [20], although non-communicable diseases and injuries are on the rise. According to the latest estimates, Cameroon has a physician density of 0.09 physicians per 1,000 people [21] and an estimated health researcher density of 3.9 per 1 million people [12,22].
Data collection tool: a seven-section questionnaire e-survey was designed by the first author on Google Forms (Google, USA) and validated by others (JNT, MT, AM, JRN, and FTE). The survey items were informed by focus group discussions with Cameroonian physicians and themes extracted from peer-reviewed literature [6,7]. After the design, the e-survey was piloted among 20 Cameroonian medical practitioners in Cameroon. The results of the pilot were then used to improve the e-survey. The final e-survey contained 33 multiple-choice, checkbox, Likert scale, and open-ended questions (Appendix). The e-survey was translated into French by the first author.
Data collection: the e-survey was distributed daily via WhatsApp (WhatsApp, USA) and Facebook (Facebook, USA) to a convenience sample of physicians practicing in Cameroon from May 23, 2020, to June 07, 2020. To increase the response rate, the authors sent the survey link both in the Cameroonian physician WhatsApp groups and privately to potential respondents. The sampling was non-randomized and consecutive, and the survey was collected anonymously. The survey was conducted in French and English. Only the questions about the participants' eligibility were marked mandatory, so the respondents could choose not to answer any of the other questions. The survey data was stored on Google Drive (Google, USA) in a password-protected account, and access to the data was limited to the investigators. The anonymized data is available on Open Science Framework [18].
Data analysis: the Likert scale responses were illustrated as stacked bar charts, and the barriers and facilitators to health research were measured then ranked using a Preference Score (PS).
Preference Score (PS) = ((-2 x number of Strongly disagree responses) + (-1 x number of Disagree disagrees) + (0 x number of Neutral responses) + (1 x number of Agree responses) + (2 x number of Strongly agree responses)). We used the median Preference Scores (PS) for each item to categorize the barriers and facilitators into three categories: weak (median PS<0), moderate (median PS=0), and strong (median PS>0). We then ordered them based on their total PS. Data analyses were done using SPSS v26 (IBM, USA). Continuous variables were expressed as measures of central tendency, and Q-Q tests were performed to determine the distribution of the data. The distribution of the data then informed the choice of bivariate tests. Qualitative variables were expressed as frequencies and percentages. Bivariate analyses (Wilcoxon Rank-Sum test, Fisher's exact test, and Spearman's correlation) were used, with a threshold of statistical significance set at 0.05 to measure the association between variables. Then the Kruskal-Wallis H test was used to evaluate the relationship between the barriers and facilitators of research (Likert scale responses) and the number of publications (divided into three categories: no publications and ≥1 publication). Next, Mann-Whitney U tests were used to identify the significant differences between the publication categories. The Bonferonni test was used to correct for the inflation in the alpha value, and the threshold of significance was set at 0.025. Ethics approval was sought and waived by the institutional review board of the Higher Institute of Health Sciences, Cameroon.
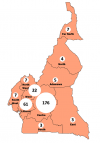
Demographics characteristics: we recorded 295 responses during the study period. Respondents had a mean age of 29.2 ± 3.5 years and had graduated from medical school 3.9 ± 3.0 years ago. More than half (176, 59.7%) of physicians lived in the Centre Region of Cameroon (Figure 1). Most of respondents were male (166, 56.3%), Francophone (224, 75.9%), and general practitioners (167, 56.6%). The majority had taken biostatistics (286, 96.9%) and research methodology (247, 83.7%) courses in medical school, and 93 (31.5%) had complementary research training online. Less than half of the respondents (144, 48.8%) had a research mentor, 137 (46.4%) had attended a conference, 46 (15.6%) had presented an abstract at a conference, and 52 (17.6%) had a graduate degree in addition to their medical degree (Table 1).
Experiences and resources: respondents who had a graduate degree in addition to their medical degree were more likely to follow research courses online (OR=3.5, 95% CI: 1.9-6.5, P<0.01), have a research mentor (OR=3.5, 95% CI: 1.8-6.8, P<0.01), present abstracts (OR=2.4, 95% CI: 1.2-5.0, P=0.01), and attend scientific conferences (OR=5.0, 95% CI: 2.5-10.0, P<0.01). Furthermore, respondents who had been to a conference were more likely to have a mentor (OR=11.6, 95% CI: 4.4-30.4, P<0.01) and to have presented an abstract (OR=0.4, 95% CI: 0.3-0.4, P<0.01).
Academic output: about half (149, 50.5%) of the respondents had published at least one article, and only 58 (19.7%) were the first authors. Respondents who had taken at least one research methodology course in medical school, on average, published 1.6 articles more than those who had not taken this course (P=0.02). Similarly, respondents who had taken supplementary research online lessons on average published 1.8 articles more than those who had not (P=0.01). Moreover, respondents with a mentor (P<0.01), who had attended a conference (P<0.01), and those who had presented an abstract (P<0.01) published more articles than their counterparts. Also, respondents who had a degree in addition to their medical degree published twice as many articles as those who did not have another degree (P=0.03) (Table 2). On average, the period between the publication of the respondents' first articles and the time when this study was conducted was 2.6 (95% CI: 2.2-3.0) years. The number of published articles was correlated with the period between the publication of the respondents' first articles and the survey (R=0.40, P<0.01), respondent's age (R=0.26, P<0.01), time since graduation from medical school (R=0.34, P<0.01), and the number of first-author publications (R=0.57, P<0.01).
Barriers: all the barriers were strong determinants of scholarly output except for the lack of financial incentives (moderate), lack of statisticians (moderate), difficulties getting authorizations to collect data (moderate), and English (weak). The top three barriers to health research identified by respondents were difficulties getting authorization to collect data, lack of financial incentives, and lack of grants (Figure 2). Lack of a supportive research team (Kruskal-Wallis H=6.29, P=0.012) and difficulties of getting an ethical clearance (Kruskal-Wallis H=5.57, P=0.018) were significant barriers to publication among respondents (Table 3). After adjustment, the difference observed between physicians without publications and those with ≥1 peer-reviewed article remained statistically significant for the lack of a research team (P<0.01) and difficulty getting an ethical clearance (P<0.01) (Table 4).
Facilitators: the top three facilitators were scientific recognition, interest in the research topic, and previous research experience (Figure 3). The determinants of scholarly output with the highest Preference Score (PS) were interested in the research subject (total PS=386) and the potential to improve practice (total PS=375) (Figure 4). Physicians without peer-reviewed articles felt grant availability was as an essential research facilitator (P<0.01) (Table 4).
The study sought to identify barriers and facilitators to health researchers among physicians in Cameroon. Health research that is driven by African researchers is vital for setting research agendas that aim to solve context-specific health problems and identifying and adapting solutions to address these problems in the African context. Health research capacity in many African countries remains low, and there has been little research conducted to identify barriers and facilitators to health research for African researchers. Such research is needed to develop strategies for increasing research capacity in African countries like Cameroon. To the best of our knowledge, this is the first study evaluating barriers and facilitators to health research among Cameroonian physicians. The majority of respondents in this study were early career researchers, and the most crucial barrier to research was getting authorization to collect data. This barrier may be the result of slow and outdated organizational structures within local research institutions. Organizational barriers such as delays in getting approval for data collection are especially accentuated in research that involves patients and is more common in countries with lower physician densities and limited clinical research experience [7]. This is the case in Cameroon, Ethiopia, and Iran, where organizational barriers such as lack of incentives and weak administrative systems represent the most significant barrier to clinical trial research [23,24]. This suggests that research institutions in Cameroon and other African countries have an essential role to play in increasing research capacity by ensuring that they set up effective organizational processes that will expedite research productivity for physicians.
Ethical clearance: the obtention of ethical clearance was a significant barrier to research involvement identified in our study. This finding is a cause of concern because medical research is governed by ethical principles [25-27], and application for ethical clearance before conducting any human or animal research is mandatory [28]. Unfortunately, African ethics committees inadvertently constitute a barrier to research because they face difficulties that slow down the process of obtaining ethical clearances [29]. Ethics committees lack the resources to meet the current need for ethical approvals in time [30]. There have been efforts to bolster the research ethics capacity in Africa to meet local needs, but ethics committees still struggle to meet local demands [29,31]. These factors might explain why obtaining ethical approval was a significant barrier to research in Cameroon. Regional collaborations such as the Pan-African Bioethics Initiative, the African Center for Disease Control, and World Health Organization Africa Region could be explored to identify and consolidate efforts to strengthen ethical processes in Cameroon and Africa [32,33].
Mentorship: we found that mentorship was associated with higher numbers of research publications among Cameroonian physicians. This is unsurprising because lack or inadequate mentorship are considerable barriers to research in Africa [5,6]. We note. However, that only half of Cameroonian physicians had research mentors. This is alarming because the majority of researchers were novices. Unguided novices will find academic medicine to be complicated and might feel discouraged from pursuing a career in research [34]. Not only can mentorship increase academic productivity, but it can also facilitate the development of skills among early-career researchers [35]. It is possible that the limited mentorship opportunities for novel researchers could be due to the limited number of experienced researchers to act as mentors. Cameroon only has a health researcher density of 3.9 per 1 million people [12,36], researchers who are often also involved in clinical work. Health researchers in Cameroon with the capacity to mentor young health researchers should be encouraged to do so, along with support from their institutions. Equitable partnerships could also be explored between Cameroonian and experienced researchers in African countries with higher research capacity and Western and Eastern countries to provide mentorship and skills transfer to young researchers.
Funding: in our study, easy access to funding was found to be an essential facilitator to research among Cameroonian physicians. Access to funding is a known determinant of research involvement and productivity in most low- and middle-income countries, especially in Africa [31]. African health research is underfunded primarily because the health systems have competing budget priorities, and research without immediate returns are not seen as worthwhile investments [11,33]. Private companies have traditionally been reticent to invest in health research in Africa as well [6,7,9]. Consequently, the financial voids left by local health systems are often filled by foreign non-governmental organizations and academic institutions with access to global health funds [15,34]. Foreign academic institutions often drive the local research agenda and carry out research on local data sometimes without much investments in elevating the capacity of their local counterparts [34]. In Cameroon, 48.2% of studies are sponsored by foreign organizations, and their funds are earmarked for specific diseases [37]. Local researchers should seek grants from international funding agencies and should explore funding from the local private sector.
Research training: the majority of Cameroonian physicians in this study had trained in biostatistics and research methodology in medical school. Research training in medical school has been shown to increase postgraduate scholarly output and is correlated with more exceptional career achievements [9,24]. Unfortunately, few medical schools in low-resource settings offer comprehensive research training [25], and as a result, their graduates tend to have limited research experience and output [10,31]. This was confirmed by the fact that Cameroonian physicians who had received research training published more articles than those who had not received training. In light of these findings, Cameroonian medical schools should revisit and revise their research curriculums to ensure that their graduates received adequate and comprehensive research training.
Despite the training, the research output of Cameroonian physicians was low in comparison with their colleagues from South America, Europe, or North America [38-40]. All Cameroonian medical students are required to defend a thesis during their last year of medical school. During this period, medical students familiarize themselves with clinical research and realize the importance of technical skills in carrying out sound research. Most Cameroonian medical schools offer the biostatistics and research methodology courses during the first couple of years of medical school, leaving a 5-6 year gap between the didactic and practical aspects of research. The gap between the theoretical and practical aspects of research might explain the low proportion of physicians who understood the courses and the low scholarly output. Exposure to the practical aspects of the research should not be limited to the thesis. Medical students should be involved early on in the practical aspect of research because early exposure correlates with a better understanding of concepts and higher research output [26,41,42].
Teamwork: Cameroonian physicians in this study reported that a lack of research teams was a significant deterrent to research involvement. Middle Eastern studies have reported similar findings [24]. It is challenging to carry out research today as a solo researcher, especially as a novice. Research collaborations foster mentorship relations and facilitate the transfer of capacities and reduce individual workload, so most researchers are part of teams [27,28]. One reason for the lack of research teams identified in our study could be limited information on the work of experienced research team leaders. Researchers should consider identifying local researchers on ResearchGate, joining established teams, recruiting competent researchers to their teams, or building capacity among available researchers [29]. Once the teams are established, researchers should harness the best out of their colleagues and out of themselves by creating a supportive environment [33]. A supportive environment can favor creativity and productivity, especially among early-career researchers [29,30].
Limitations: we recognize some limitations of our study. First, the respondents were unintentionally younger than anticipated, and they had less research experience. The young age of the respondents may be explained by our dissemination strategy (social media and mostly through acquaintances). Early-career researchers might not face the same barriers or have the same facilitators as researchers with more experience. Hence our findings may not be generalizable to older researchers with more experience. Also, practitioners without access to broadband will have been excluded from our study. This subgroup is likely to have limited financial resources or to work in resource-limited settings. This subgroup is likely to face different obstacles and facilitators to health researchers. Our sampling was non-randomized, so the effect of confounders could not be eliminated from our analysis. Nevertheless, we maximized the response rate by disseminating the survey regularly through multiple media. We equally minimized bias by anonymizing the survey. While in this study, we discuss a lot of the implications of the study to the broader African continent, we recognize that barriers and facilitators to health research likely vary from country to country. Therefore, we encourage similar research like this one to be conducted in other African countries to identify specific contextual factors and develop local solutions to address local health research gaps.
The high burden of disease and lack of resources in sub-Saharan Africa explains the need for local and context-tailored research studies. As identified in this study, strategies to address the low health research capacity should aim to increase research funding opportunities for African researchers, provide mentorship opportunities for novice researchers, improve institutional research approval processes, and augmentation of research curriculums in universities and medical schools. Further research works in other African countries are needed to confirm our findings and to assess the impact of the establishment of research teams in scientific production in our context.
What is known about this topic
- There is an epidemiological growth of diseases (especially non-communicable conditions) in sub-Saharan Africa, and thereby in Cameroon;
- There is a lack of scientific works in parallel to this epidemiologic evolution.
What this study adds
- This study provides quantitative and qualitative data on the research experiences of early-career Cameroonian physicians;
- This study is the first to highlight barriers and facilitators of medical and health research in Cameroon.
The authors declares no competing interests.
USK: conceptualization, data curation, formal analysis, investigation, methodology, project administration, visualization, writing original draft, writing review, and editing. JNT, MT, AM, FTE, and JRN: investigation, methodology, project administration, writing original draft, writing review and editing. CW and FNT: investigation, writing original draft, writing review, and editing. DJ: conceptualization, investigation, project administration, validation, investigation, writing original draft, writing review, and editing. All the authors read and approved the final version of the manuscript.
We thank Berjo Takoutsing, Yvan Zolo, and Ornella Pokam Feunou for their material assistance.
Table 1: sociodemographic characteristics and research experience of Cameroonian physician respondents
Table 2: subgroup comparison of the research output of Cameroonian physicians
Table 3: perceived barriers to research according to Cameroonian physicians
Table 4: factors that influence the decision of Cameroonian physicians to conduct research
Figure 1: geographic distribution of Cameroonian physicians who responded to the online survey. The figures within the circles are the number of respondents per region
Figure 2: stacked bar chart of the perceived barriers to research according to early-career Cameroonian physicians. The red circles represent the average response
Figure 3: stacked bar chart of the perceived facilitators of research according to early-career Cameroonian physicians. The red circles represent the average response
Figure 4: butterfly chart of the barriers and facilitators of health research in Cameroon. Barriers are indicated by the letter B while facilitators are indicated by the letter F. Strong determinants (median PS>0) are green, moderate determinants (median PS=0) are orange, and weak determinants (median PS<0) are red
- Michaud CM. Global burden of infectious diseases. Encycl Microbiol. 2009;444-454. PubMed
- Bigna JJ, Noubiap JJ. The rising burden of non-communicable diseases in sub-Saharan Africa. Lancet Glob Health. 2019;7(10):e1295-e1296. PubMed | Google Scholar
- Haagsma JA, Graetz N, Bolliger I, Naghavi M, Higashi H, Mullany EC et al. The global burden of injury: incidence, mortality, disability-adjusted life years and time trends from the Global Burden of Disease study 2013. Inj Prev. 2016;22(1):3-18. PubMed | Google Scholar
- World Bank Group. Open Data. The World Bank - Data. 2020. Accessed April 06 2020.
- Kokwaro G, Kariuki S. Medical research in Africa: problems and some solutions. Malawi Med J J Med Assoc Malawi. 2001;13(3):40. PubMed | Google Scholar
- Dhalla KA, Guirguis M. Barriers and incentives for conducting research amongst the ophthalmologists in Sub-Sahara Africa. PLOS ONE. 2018;13(10):e0197945. PubMed | Google Scholar
- Conradie A, Duys R, Forget P, Biccard BM. Barriers to clinical research in Africa: a quantitative and qualitative survey of clinical researchers in 27 African countries. Br J Anaesth. 2018;121(4):813-821. PubMed | Google Scholar
- OECD. Gross domestic spending on R&D. the OECD. 2020. Accessed June 20 2020.
- Atabong AB. Africa's medical scientists are struggling to get funding to back their research. Quartz Africa. Accessed June 20 2020.
- United Nations Economic Commission for Africa. Towards Achieving the African Union's recommendation of expenditure of 1% of GDP on Research and Development. Accessed 20 June 2020.
- World Health Organization. Research and Development to Meet Health Needs in Developing Countries: Strengthening Global Financing and Coordination. Geneva, Switzerland, World Health Organisation. 2012. Google Scholar
- World Health Organization. Health researchers (in full-time equivalent) per million inhabitants, by WHO Region. WHO. 2018. Accessed 20 June 2020.
- Madhukar P. Archives of Failures in Global Health. Nature Research Microbiology Community. 2019. Accessed 17 June 2020.
- Kouyaté B, Sie A, Yé M, De Allegri M, Müller O. The Great Failure of Malaria Control in Africa: A District Perspective from Burkina Faso. PLoS Med. 2007 Jun;4(6):e127. PubMed | Google Scholar
- Boum II Y, Burns BF, Siedner M, Mburu Y, Bukusi E, Haberer JE. Advancing equitable global health research partnerships in Africa. BMJ Glob Health. 2018 Aug 23;3(4):e000868. PubMed | Google Scholar
- Our Work. Africa CDC. Accessed 12 June 2020.
- Rayne S, Burger S, Straten SV, Biccard B, Phaahla MJ, Smith M. Setting the research and implementation agenda for equitable access to surgical care in South Africa. BMJ Glob Health. 2017;2(2):e000170.. PubMed | Google Scholar
- Kanmounye US. Barriers and Facilitators of Medical Research in Cameroon. Open Sci Framew. 2020;1(1). Google Scholar
- Omolase CO, Egberongbe A, Komolafe O, Olasinde A, Omolase B, Adeosun O. Practice of bio-medical research amongst doctors in Owo. South Afr Fam Pract. 2015;57(2):112-115. PubMed | Google Scholar
- World Bank Group. Cameroon | Data. World Bank Country Data. Accessed 28 November 2019.
- Institute for Health Metrics and Evaluation. Cameroon. Institute for Health Metrics and Evaluation. 2015. Accessed 27 March 2020.
- Central Intelligence Agency. Physicians density. 2017. Accessed 23 June 2020.
- Safdari R, Ehtesham H, Robiaty M, Ziaee N. Barriers to participation in medical research from the perspective of researchers. J Educ Health Promot. 2018 Feb 9;7:22. PubMed | Google Scholar
- Franzen SRP, Chandler C, Atashili J, Angus B, Lang T. Barriers and enablers of locally led clinical trials in Ethiopia and Cameroon: a prospective, qualitative study. The Lancet. 2013;382:14. Google Scholar
- Hren D, Lukic IK, Marusic A, Vodopivec I, Vujaklija A, Hrabak M et al. Teaching research methodology in medical schools: students´ attitudes towards and knowledge about science. Med Educ. 2004;38(1):81-86. PubMed | Google Scholar
- White AM, Lu N, Cerulli C, Tu X. Examining Benefits of Academic-Community Research Team Training: Rochester´s Suicide Prevention Training Institutes. Prog Community Health Partnersh Res Educ Action. 2014;8(1):125-137. PubMed | Google Scholar
- Nelson LE, Morrison-Beedy D. Research team training: moving beyond job descriptions. Appl Nurs Res ANR. 2008;21(3):159-164. PubMed | Google Scholar
- Sharma M, Razzaque B. Research capacity strengthening in South Asia: based on the experience of South Asian Hub for Advocacy, Research and Education on Mental Health (SHARE). Glob Ment Health. 2017 May 16;4:e9. PubMed | Google Scholar
- Straus SE, Johnson MO, Marquez C, Feldman MD. Characteristics of Successful and Failed Mentoring Relationships: A Qualitative Study Across Two Academic Health Centers. Acad Med J Assoc Am Med Coll. 2013;88(1):82-89. PubMed | Google Scholar
- Mokgatla B, IJsselmuiden C, Wassenaar D, Kasule M. Mapping research ethics committees in Africa: Evidence of the growth of ethics review of health research in Africa. Dev World Bioeth. 2018;18(4):341-348. PubMed | Google Scholar
- Brem H, Amundson E. Preparing Hopkins medical students for a career in academic neurosurgery. Surgery. 2003;134(3):414-415. PubMed | Google Scholar
- Rusakaniko S, Makanga M, Ota MO, Bockarie M, Banda G, Okeibunor J et al. Strengthening national health research systems in the WHO African Region - progress towards universal health coverage. Glob Health. 2019;15(1):50. PubMed | Google Scholar
- Petros B. Ethical review of health-related biotechnology research in Africa: a role for the Pan African Bioethics Initiative (PABIN). Afr J Med Med Sci. 2007;36 Suppl:43-47. PubMed | Google Scholar
- Sánchez JP (ed). Succeeding in Academic Medicine: a Roadmap for Diverse Medical Students and Residents. Springer International Publishing. 2020. Google Scholar
- Straus SE, Straus C, Tzanetos K, International Campaign to Revitalise Academic Medicine. Career choice in academic medicine: systematic review. J Gen Intern Med. 2006;21(12):1222-1229. PubMed | Google Scholar
- ChartsBin. Number of Researchers per million inhabitants by Country. ChartsBin. Accessed 24 June 2020.
- Walter EA, Jerome A, Marceline DN, Yakum MN, Pierre W. Map of biomedical research in Cameroon; a documentary review of approved protocols from 1997 to 2012. Glob Health. 2017;13(1):85. PubMed | Google Scholar
- Cunha A, dos Santos B, Dias ÁM, Carmagnani AM, Lafer B, Busatto GF. Success in publication by graduate students in psychiatry in Brazil: an empirical evaluation of the relative influence of English proficiency and advisor expertise. BMC Med Educ. 2014;14:238. PubMed | Google Scholar
- Gorraiz J, Reimann R, Gumpenberger C. Key factors and considerations in the assessment of international collaboration: a case study for Austria and six countries. Scientometrics. 2012;91(2):417-433. Google Scholar
- Keck A-S, Sloane S, Liechty JM, Fiese BH, Donovan SM. Productivity, impact, and collaboration differences between transdisciplinary and traditionally trained doctoral students: A comparison of publication patterns. PLoS ONE. 2017 Dec 15;12(12):e0189391. PubMed | Google Scholar
- Reinders JJ, Kropmans TJB, Cohen-Schotanus J. Extracurricular research experience of medical students and their scientific output after graduation. Med Educ. 2005;39(2):237. PubMed | Google Scholar
- Amgad M, Man Kin Tsui M, Liptrott SJ, Shash E. Medical Student Research: An Integrated Mixed-Methods Systematic Review and Meta-Analysis. PloS One. 2015;10(6):e0127470. PubMed | Google Scholar
Search
This article authors
On Pubmed
On Google Scholar
Citation [Download]
Navigate this article
Similar articles in
Key words
Tables and figures
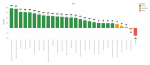 Figure 4: butterfly chart of the barriers and facilitators of health research in Cameroon. Barriers are indicated by the letter B while facilitators are indicated by the letter F. Strong determinants (median PS>0) are green, moderate determinants (median PS=0) are orange, and weak determinants (median PS<0) are red
Figure 4: butterfly chart of the barriers and facilitators of health research in Cameroon. Barriers are indicated by the letter B while facilitators are indicated by the letter F. Strong determinants (median PS>0) are green, moderate determinants (median PS=0) are orange, and weak determinants (median PS<0) are red