Are ommaya shunt infection rates low in craniopharyngioma patients?
Luxwell Jokonya, Aaron Musara, Tariro Mduluza-Jokonya, Ignatius Esene
Corresponding author: Luxwell Jokonya, Department of Surgery, College of health Science, University of Zimbabwe, Harare, Zimbabwe 
Received: 16 Jun 2020 - Accepted: 11 Oct 2020 - Published: 12 Oct 2020
Domain: Neuro-oncology,Neurosurgery
Keywords: Craniopharyngioma, ommaya infection, shunt infection
©Luxwell Jokonya et al. PAMJ Clinical Medicine (ISSN: 2707-2797). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Luxwell Jokonya et al. Are ommaya shunt infection rates low in craniopharyngioma patients?. PAMJ Clinical Medicine. 2020;4:61. [doi: 10.11604/pamj-cm.2020.4.61.22497]
Available online at: https://www.clinical-medicine.panafrican-med-journal.com//content/article/4/61/full
Are ommaya shunt infection rates low in craniopharyngioma patients?
Luxwell Jokonya1,2,&, Aaron Musara1, Tariro Mduluza-Jokonya2, Ignatius Esene3
&Corresponding author
Tumours are generally associated with a high rate of infections. More so for craniopharyngiomas which may have cranial hardware which increases the infection risk. We have however observed that in reality, cystic fluid shunts in craniopharyngioma patients have an unusually low infection rate, sometimes despite significant risk factors. We present 2 cases of children with histologically confirmed adamantinomatous type craniopharyngioma. Both had ommaya shunts inserted for cystic fluid aspiration as part of treatment. They then presented with exposed shunts but no signs of infection, despite significant risk factors for infection. Studies need to be carried out to determine the factors involved in this seeming ommaya shunt infection resistance to these group of patients.
Craniopharyngioma (Cp) is a very rare tumour with annual incidence of 1.3 per million people. As a result very few studies have been done on them [1]. Tumours in general, are known to increase the host infection rate [2]. This is mainly by host immunosuppression due to tumour effects such as physical obstruction by tumour in the different body systems, destruction of normal skin and mucosal barriers, surgical diagnostic and therapeutic procedures, radiotherapy and also by the administration of chemotherapy that is immunosuppressive [2]. For tumours like Cp, the use of surgical implants in their management would theoretically increase this risk considering that ventriculoperitoneal shunt infection rate is up to 12.9% [3,4]. In a Cp patient with shunt hardware that has been exposed it would seem most likely that their risk of infection would be very high. We have however noted a number of Cp patients with ommaya shunts implanted into tumour cyst who seemed to have some level of resistance to infection despite the risk factors. Here we report only two of such cases.
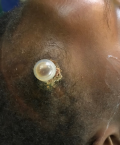
Case1: a 9-year-old girl presented 6 months after biopsy and ommaya reservoir insertion for an unresectable cystic adamantinomatous craniopharyngioma. She presented with a 3-week history of an exposed ommaya shunt reservoir due to skin erosion. The mother had kept the exposed part covered with a dry bandage while waiting to go to the hospital. No urgency was made to access medical care because according to the mother the child was “okay” apart from the exposed shunt. On presentation, their only complaint was the exposed ommaya reservoir dome. On examination the child was playful and apyrexic. The skin surrounding the exposed shunt was not erythematous nor were there any signs of infection (Figure 1). The rest of the examination findings were normal. Full blood count done was normal. Staphylococcus aureus was isolated from the exposed part of the shunt, suggesting contamination of exposed hardware which did not translate to infection. No organisms were found on the intracystic component as well as the tumour cystic fluid and blood culture. The child underwent uneventful replacement with a new Ommaya shunt. On 6 weeks follow-up there were no signs of infection and the child was doing well.
Case 2: an 11-year-old male patient presented with a one-week history of exposed ommaya reservoir (Figure 2). The child had been diagnosed of adamantinomatous craniopharyngioma eight months prior to presentation after a biopsy and insertion of an ommaya reservoir into the large cystic component had been done. He had been doing relatively well until a week prior to presentation that he started having erosion of the skin overlying the shunt dome. The erosion progressed until the reservoir together with the whole intracystic component eventually just fell off whilst the child was bathing in their rural home. It fell onto a dirty makeshift bathroom floor. When the mother discovered this a couple of minutes later, in her ignorance she wiped it with a piece of cloth and reinserted it intracranially (supposedly into the cyst). Due to the brain pulsations the shunt kept being pushed out so she used an unsterile cloth to tie it around the head to keep it secure. They presented a week later because of financial constraints and long distance to the nearest health facility. On examination the child was fully awake with normal body temperature. A dirty cloth was wrapped around the head securing the shunt from falling off (Figure 2). There was seepage of machinery oil fluid from the tumour cyst. There was no erythema, pus or any signs of infection around the shunt entry point. There were no other signs or symptoms of infection. The rest of the examination was unremarkable. Full blood count, C reactive protein done was normal. Contrasted Computer tomography did not show any signs of infection. The child had subsequent replacement of the reservoir uneventfully and recovered well. Three months down the line there was no infection noted or any other complications.
These cases demonstrate an unusual resistance to shunt related infection in Cp patients whose shunt is inserted into cystic fluid. This raises speculation as to what qualities this fluid may possess that confers this resistance. In literature very little is known about this machinery oil fluid, and there have been speculations about its possible toxicity effects [5]. The antibacterial effects of this fluid if any, seems to be of localised effect. Direct inoculation into the tumour cyst by implanting a potentially infected, obviously unsterile ommaya shunt that had fallen off is a cocktail for disaster and ordinarily would result in an infection. But the child surprisingly did not seem affected by it in any way. Treatment of cystic Cp by insertion of ommaya shunts is not only well recognised but is very effective too [6]. Ommaya reservoir infections have been documented in literature [7]. Large studies of patients with ommaya shunts showed an infection rate of 5.5-8%. However, all these shunts were intrathecal and non in Cp patients [8]. In our English literature search we did not find any reports on intracystic ommaya shunts to treat Cp being infected. While this may be because the tumour is rare and not all of the Cp patients are treated this way, it may also be because Cp patients have some inherent resistance to intracystic ommaya shunts infection. This report is not to dispute that the systemic infection rates in Cp patients is more than in the general population [9]. It is merely pointing out that Ommaya reservoirs inserted into Cp tumour cyst may have reduced chances of getting infected. More studies however, would need to be done on the composition and properties of this fluid.
There is very little if any documentation of infection of an ommaya shunt inserted into a craniopharyngioma cyst. These patients we report, showed no infection despite increased risk. Factors involved in this apparent reduced ommaya shunt infection with craniopharyngioma fluid need to be further elucidated.
The authors declare no competing interests.
All the authors have read and agreed to the final manuscript.
Figure 1: exposed ommaya reservoir shunt of first case
Figure 2: exposed ommaya reservoir shunt of second patient
- Bunin GR, Surawicz TS, Witman PA, Preston-Martin S, Davis F, Bruner JM. The descriptive epidemiology of craniopharyngioma. J Neurosurg. 1998;89(4):547-551. PubMed | Google Scholar
- Rolston KVI. Infections in cancer patients with solid tumors: a review. Infect Dis Ther. 2017;6(1):69-83. PubMed | Google Scholar
- Lee RP, Venable GT, Vaughn BN, Lillard JC, Oravec CS, Klimo P. The impact of a pediatric shunt surgery checklist on infection rate at a single institution. Clin Neurosurg. 2018;83(3):508-520. PubMed | Google Scholar
- Pelegrín I, Lora-Tamayo J, Gómez-Junyent J, Sabó N, García-Somoza D, Gabarrós A et al. Management of ventriculoperitoneal shunt infections in adults: analysis of risk factors associated with treatment failure. Clin Infect Dis. 2017;64(8):989-997. PubMed | Google Scholar
- Andrea Yosajany MLTS. Craniopharyngioma and oil machinery fluid: review. J Clin Exp Pathol. 2015;05(02). Google Scholar
- Moussa AH, Kerasha AA, Mahmoud ME. Surprising outcome of ommaya reservoir in treating cystic craniopharyngioma: a retrospective study. Br J Neurosurg. 2013;27(3):370-373. PubMed | Google Scholar
- Park DM, DeAngelis LM. Delayed infection of the ommaya reservoir. Neurology. 2002;59(6):956-957. PubMed | Google Scholar
- Szvalb AD, Raad II, Weinberg JS, Suki D, Mayer R, Viola GM. Ommaya reservoir-related infections: clinical manifestations and treatment outcomes. J Infect. 2014;68(3):216-224. PubMed | Google Scholar
- Olsson DS, Andersson E, Bryngelsson IL, Nilsson AG, Johannsson G. Excess mortality and morbidity in patients with craniopharyngioma, especially in patients with childhood onset: a population-based study in Sweden. J Clin Endocrinol Metab. 2015;100(2):467-474. PubMed | Google Scholar