Multiple Intestinal cystic schwannoma mimicking an ovarian tumor with carcinomatosis: case report
Khalil Maamar, Rachid Jabi, Mohammed Boudou, Tijani El Harroudi, Mohammed Bouziane
Corresponding author: Khalil Maamar, University Mohammed VI, General Surgery, Oujda, Morocco 
Received: 18 Dec 2020 - Accepted: 18 Jan 2021 - Published: 20 Jan 2021
Domain: General surgery
Keywords: Schwannoma, ovarian tumor, gastroIntestinal tract
©Khalil Maamar et al. PAMJ Clinical Medicine (ISSN: 2707-2797). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Khalil Maamar et al. Multiple Intestinal cystic schwannoma mimicking an ovarian tumor with carcinomatosis: case report. PAMJ Clinical Medicine. 2021;5:23. [doi: 10.11604/pamj-cm.2021.5.23.27474]
Available online at: https://www.clinical-medicine.panafrican-med-journal.com//content/article/5/23/full
Case report 
Multiple Intestinal cystic schwannoma mimicking an ovarian tumor with carcinomatosis: case report
Multiple Intestinal cystic schwannoma mimicking an ovarian tumor with carcinomatosis: case report
![]() Khalil Maamar1,&, Rachid Jabi1, Mohammed Boudou1, Tijani El Harroudi, Mohammed Bouziane1
Khalil Maamar1,&, Rachid Jabi1, Mohammed Boudou1, Tijani El Harroudi, Mohammed Bouziane1
&Corresponding author
Schwannomas are benign tumors composed of schwann cells, these tumors theoretically can present anywhere in the body where nerves reside rarely on gastroIntestinal tract. The definitive diagnosis of this rare form is made on complete excision of the mass but it can be identified through the combination of imaging and biopsy. We report a case of an intestinal cystic schwannoma simulating an ovarian tumor.
Schwannoma is a benign tumor of ectodermal origin developed from the nerve sheath that envelops the axons. The incidence of gastrointestinal schwannoma is extremely low, and it mainly occurs in the stomach but rarely in the intestines. Intestinal schwannoma lacks specific clinical manifestations, and its symptoms mainly depend on the size and location of the tumor. We report a case of an intestinal cystic schwannoma simulating an ovarian tumor.
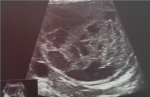
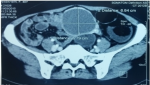
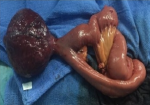
We present a case of a-41 year old woman, mother of 4 living children, with no notable pathological history who has had pelvic pain for 4 months with signs of urinary compression. The clinical examination is without particularity. The tumor markers: CA125, ACE, CA 15-9 were negative, the objective pelvic ultrasound in the left lateral uterine, a rounded image of 79/69 mm net contours with double fluid and tissue components (Figure 1). The abdominal and pelvic CT was favorable of a mass probably of ovarian origin associated with multiple intraperitoneal cystic nodules (Figure 2). Laparoscopic exploration revealed a huge vascularized tumor (Figure 3) at the expense of the prolapsed intestine in the pouch of Douglas. Conversion to mini para-umbilical laparotomy allowed resection of the hail carrying the tumor with anastomosis. The postoperative follow-up was simple and the result of the anatomopathology was in favor of a multiple intestinal cystic schwannoma.
Gastrointestinal schwannomas are rare mesenchymal tumors, and account for approximately 5% of all mesenchymal tumors [1,2]. Schwannomas can be solitary or multiple, the most common site (60-70% of all GI cases) is the stomach, followed by the colon and rectum (3%) {1] , Small-intestinal and esophageal schwannomas have been very rarely reported [3]. Most GI schwannomas are incidental findings during screening colonoscopy or imaging [2] the size of the tumor does not condition the prognosis. In a systematic literature review of schwannomas of the colon and rectum published by Bohlok et al. a large portion of patients were asymptomatic on diagnosis (36%), but others presented with rectorrhagia, abdominal pain, or constipation [4]. Other studies noted that GI schwannomas can manifest as colonic obstructions or as intussusceptions [5,6]. Advances in imaging, however, have made it possible to diagnose these tumors earlier, at the first manifestations or sometimes accidentally before their appearance or they can simulate an ovarian tumor as is the case in our observation. The abdominal CT scan is a test of choice to highlight and specify the extent of the tumor before an excisional procedure. With CT imaging, it appears as an exophytic mass with homogenous enhancement. Cystic changes, necrosis, or calcifications within tumors are not commonly found [7]. The complete surgical resection seems to be the treatment of choice because of the preoperative diagnostic uncertainty and the excellent long-term outcome, as these tumors are uniformly benign [8,9] .
Neurogenic tumors of the small intestine are extremely rare. Although schwannoma is often clinically indolent for many years, complications such as gut compression or bleeding might occur. In these cases, surgical management is required.
The authors declare no competing interests.
All the authors have read and agreed to the final manuscript.
Figure 1: pelvic ultrasound: Image of 79/69 mm net contours with double fluid and tissue components
Figure 2: abdominal and pelvic CT scan: a rounded image of 684/679 mm probably of ovarian origin
Figure 3: tumor depending of large bowel
- Oh SJ, Suh BJ, Park JK. Gastric schwannoma mimicking malignant gastrointestinal stromal tumor exhibiting increased fluorodeoxyglucose uptake. Case Rep Oncol. 2016 Apr 21;9(1):228-34. PubMed | Google Scholar
- Pansari M, Lodin D, Gupta AK, Genuit T, Moseson J. Rare case of a transverse colon schwannoma. Cureus. 2020 Apr 9;12(4):e7604. PubMed | Google Scholar
- Levy AD, Quiles AM, Miettinen M, Sobin LH. Gastrointestinal schwannomas: CT features with clinicopathologic correlation. AJR Am J Roentgenol. 2005 Mar;184(3):797-802. PubMed | Google Scholar
- Bohlok A, El Khoury M, Bormans A, Galdon MG, Vouche M, El Nakadi I et al. Schwannoma of the colon and rectum: a systematic literature review. World J Surg Oncol. 2018 Jul 3;16(1):125. PubMed | Google Scholar
- González Ruiz Y, Reyes Delgado A, Guiterrez Alonso C, Franco Rubio JI, González Herrero M. Sigmoid intussusception as a clinical presentation of colonic schwannoma: pediatric case (Article in Spanish). Arch Argent Pediatr. 2019 Feb 1;117(1):e68-e71. PubMed | Google Scholar
- Wang WB, Chen WB, Lin JJ, Xu JH, Wang JH, Sheng QS. Schwannoma of the colon: a case report and review of the literature. Oncol Lett. 2016 Apr;11(4):2580-2582. PubMed | Google Scholar
- Mekras A, Krenn V, Perrakis A, Croner RS, Kalles V, Atamer C et al. Gastrointestinal schwannomas: a rare but important differential diagnosis of mesenchymal tumors of gastrointestinal tract. BMC Surg. 2018 Jul 25;18(1):47. PubMed | Google Scholar
- Goh BK, Chow PK, Kesavan S, Yap WM, Ong HS, Song IC et al. Intraabdominal schwannomas: a single institution experience. J Gastrointest Surg. 2008 Apr;12(4):756-60. PubMed | Google Scholar
- Hu J, Liu X, Ge N, Wang S, Guo J, Wang G et al. Role of endoscopic ultrasound and endoscopic resection for the treatment of gastric schwannoma. Medicine. 2017 Jun;96(25):e7175. PubMed | Google Scholar