Survival of asthma patients attended at Chitungwiza Central Hospital in Zimbabwe
Pisirai Ndarukwa, Moses John Chimbari, Elopy Sibanda
Corresponding author: Pisirai Ndarukwa, School of Nursing and Public Health, University of KwaZulu Natal, College of Health Sciences, School of Nursing and Public Health, Durban, South Africa 
Received: 20 Nov 2020 - Accepted: 28 Jun 2021 - Published: 06 Jul 2021
Domain: Respiratory diseases
Keywords: Asthma, hazard ratio, survival, death proportion, Zimbabwe
©Pisirai Ndarukwa et al. PAMJ Clinical Medicine (ISSN: 2707-2797). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Pisirai Ndarukwa et al. Survival of asthma patients attended at Chitungwiza Central Hospital in Zimbabwe. PAMJ Clinical Medicine. 2021;6:19. [doi: 10.11604/pamj-cm.2021.6.19.27063]
Available online at: https://www.clinical-medicine.panafrican-med-journal.com//content/article/6/19/full
Survival of asthma patients attended at Chitungwiza Central Hospital in Zimbabwe
&Corresponding author
Introduction: Asthma is a leading global public health problem. It is estimated that 300 thousand people die annually from asthma worldwide. In Zimbabwe 9/100 000 population died from asthma in 2014, accounting for 1.02% of total deaths. The association between asthma survival and socio-demographic and pathologic factors has not been evaluated in Zimbabwe. The purpose of our study was to determine the survival of patients with asthma at Chitungwiza Central Hospital, Zimbabwe over a period of 20 years (1997 to 2017).
Methods: records for 158 asthma patients were analysed in this retrospective cohort study. The patient records were sampled from the computerised health information department at the hospital. Data were collected using a patient record checklist that was divided into four sections: (i) demographic information, (ii) clinical characteristics of asthma patients, (iii) health service utilization and (iv) asthma self-management. Descriptive data analysis was performed using the Kaplan Meier survival function curves. The Kaplan Meier survival curves were differentiated by the log-rank test, median survival times and mortality rates. Significant hazard ratios were used for multivariate cox regression model and a test on proportional hazards assumption based on Schoenfeld residuals were conducted.
Results: the total follow-up time was 2208 person years. The study showed that 94/153(61.4%) had since died. The median age at death was 25.5 years (IQR; 21-34). Smoking history [p=<0.001], presence of respiratory disease and cardiovascular disease [p=0.002] were significantly associated with a higher proportion of death in the cohort. A multivariate cox proportional hazards analysis after controlling for smoking history and history of rhinitis showed that seeing same doctor for asthma had a HR=0.22(CI 0.07-0.62; p=0.005 and being hospitalised in the past 2 years for asthma had a HR=3.61 (CI 1.42-9.16; p=0.007.
Conclusion: the study concluded that having a history of smoking and presence of comorbidities such as respiratory and cardiovascular diseases could increase risk of death among the patients.
Asthma is a global public health problem [1]. This heterogeneous disease is characterised by chronic inflammation of the small airway and reversible bronchoconstriction. The symptoms of asthma include chest tightness, wheezing, shortness of breath and cough which vary over time and in intensity with variable expiratory airflow limitation [2]. Globally 334 million people suffer from asthma and approximately 300 thousand patients die annually [3]. Twenty-two million disability-adjusted life years (DALYs) are lost annually. Asthma leads to reduced educational opportunities for children and increased time off from work for parents resulting in the negative impacts on the economy through loss of productivity [3]. Asthma accounts for an estimated 0.89% of deaths in Zimbabwe compared to 0.27% in the United Kingdom [4,5]. The all age group adjusted death rate was 16.81 per 100,000 of population for asthma in Zimbabwe and the country was ranked number 15 in the world [6,7]. Asthma has been associated with increased hospital admission over the past 25 years in South Africa with reports of 25-200 times increase of admission [8]. Most asthma deaths occur among senior citizens, although comparisons of mortality rates tend to focus on children and young adults. In Zimbabwe, the asthma mortality rate among those aged >80 years is high, 253.5 deaths per 100 000 men and 185.8 deaths per 100 000 women [7]. Deaths from asthma although infrequent, are of serious concern because they are often preventable [9]. Over the past 50 years, death rates among the young age groups in many high-income countries have been decreasing. The gainswere attributed to modifications in the managementof asthma, and the availability and use of the novel asthma medications. In contrast, in Zimbabweanecdotal evidence revealed that deaths among asthma patients was high at Chitungwiza Central Hospital. This motivated the conduct of aretrospective clinical cohort study to determine the survival of adult patients with asthma during the 20-year periodspanning 1997 to 2017.
Study design and setting: we conducted a retrospective cohort study to determine the survival of adult patients with asthma from 1997 to 2017. This study was conducted at Chitungwiza Central Hospital in Zimbabwe.The hospital has a bed capacity of 500 beds including general, specialised, maternity and emergency care beds. Patients with acute asthma attend the casualty department from where they may be admitted to medical or paediatric wards as indicated. More complex cases of asthma such as status asthmaticus are managed in the high dependence unit.
Data collection: records of patients with a diagnosis of asthma were identified using the computer-based application systems used in the hospital. These included the Systems Application Product (SAP) for admitting and discharging patients and the District Health Information System (DHIS). Data were then extracted manually from the patient files using a standard patient record checklist. All available asthma patients records from 1997 to 2017 were captured from the health information and records department at the hospital. Additionally, we extracted data on asthma deaths from the death certificates, and when available post-mortem results which were in the patients´ files. We collected data on patients smoking history. The smoking history looked at only two variables as was recorded in patients´ records, which were either smoker or non-smoker. In this study, smoker was defined as any person who has admitted to inhalation of the smoke of burning tobacco that is used mostly in three forms: cigarettes, pipes, and cigars [10]. A non-smoker is therefore the opposite of a smoker. Data from the checklist was then entered into a KoBO Collect platform that also acted as a double entry. The patient information collected was divided into four sections: (i) demographic information, (ii) clinical characteristics of asthma patients, (iii) health service utilization and (iv) asthma self-management. Patient data with all the above-mentioned sections were included in the study. Data collectors were trained on how to use the KoBo Collect Toolbox before actual data collection commenced on 29th of November 2018 ending on 16th of December 2018.
Sample size determination and sampling techniques: we calculated a minimum sample size of 157. Sample calculations were based on the following; an unknown proportion of asthma death in the setting leading to the use of a hazard ratio (HR) of 50% to calculate the sample size. This was based on the following formula H0: S1(t)=S2(t), alpha =0.0500 (two sided), s1=0.4000 s2=0.6325, hratio=0.5000, power=0.8000, p1=0.333 and withdrawal =10.00%.
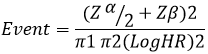
Data analysis: the data were transferred to an Excel 2013 spreadsheet for cleaning and coding and analysed using the Stata Version 13 package. Descriptive statistics were performed on the demographic characteristics which included gender, employment status and smoking history, reporting sex differences (proportion: student t-test; p-value <0.05). Clinical characteristics, health services utilization and asthma self-management were also descriptively analysed making comparisons between alive and dead participants (proportion: student t-test; p-value <0.05). Comparisons of survival times for the asthmatic patients by these different characteristics were performed using the Kaplan Meier survival function curves. Further analysis of the cohort was done using bivariate Cox regression models. Significant hazard ratios were then used for multivariate Cox regression model. Finally a test on proportional hazards based on Schoenfeld residuals was done to check if the model was consistent to Cox regression assumptions [11].
Ethical considerations: permission to conduct the study was given by the Biomedical Research Ethics Committee of the University of KwaZulu-Natal (BE613/18) and the Medical Research Council of Zimbabwe (A/2352). Gatekeepers´ permission was granted by Zimbabwe Ministry of Health and Child Care and Chitungwiza Central Hospital. The community advisory board for Chitungwiza allowed the study to be conducted. Data captured through mobile electronic devices did not capture personal identifying information for the patient records and only computer generated codes were used for each participant record. We did not seek permission from individual patients since we were using patient files kept by the hospital´s records and information department.
Demographic characteristics of the asthma cohort: 1997-2017: a total of 158 records were collected for an asthma cohort which was analysed for a 20 years follow up period. Table 1 shows characteristics of the cohort focusing on smoking history, cause of death and place of death. The analysis included 153 asthma patients while the other 5 patients with asthma were lost to follow-up. The median age of cohort between sexes (male 18.5 (IQR 11-23): female 19 (IQR13-25); p=0.330). The total follow up period was 2208 person years (males (891 person years): females (1317 person years)). All-cause mortality was 94/153(61.4%) among the participants in the cohort.There were more males 37/60(61.7%) than females 57/93(61.3%) who died during the follow-up period due to asthma. There was no significant difference in the median age at death by sex. The overall age was 25.5 [21-34] years, (p=0.340) and 25 [19-32] years for males and 26[21-37] years for females. The levels of education of the cohort participants did not differ by gender [p=0.474] or marital status [p=0.121]. The study showed 73/158(46.2%) of participants reported an income between US$201 and US$500, there was no significant difference in the level of income between males and females [p=0.232]. More males (53.2%) were current or former cigarette smokers, while only 24% of the women had ever smoked cigarettes. [p=<0.001]. The prevalence of a history of cigarette smoking differed amongst patients using the different inhaled glycocorticosteroid formulations. The percentage of smokers amongst patients treated with beclamethasone and salmeterol fluticasone propionate was 20.3%, with 13.9% and 6.3% on beclamethasone and the combination of salmeterol and fluticasone propionate respectively. The majority 85/94(90.4%) of asthma patients died in health facilities, the remainder died at home. There was no gender bias between males or females dying at health facilities [p=0.677] (Table 1).
Clinical characteristics of the asthma patients: the clinical characteristics of the asthma patients are shown in Table 2. The extent of asthma control was evaluatedfrom patient notes, which included the Asthma Control Test (ACT). Patients with an ACT score below 19 were considered uncontrolled while those with a score above >19 were considered well controlled. The proportion of patients who died with asthma during the period of interest was significantly higher in those with uncontrolled asthma [p=0.040]. Participants in the cohort did not show any significant difference in the regularityof use of maintenance medications [p=0.421] nor adherence to asthma medications [p=0.476]. Adherence, to asthma medication was extracted from patient notes, which showed whether the patient was adherent or not as recorded by the consulting doctor. In our study, we defined asthma exacerbation as use of systemic corticosteroids or an increase from a stable maintenance dose, for at least 3 days and associated with either hospitalisation or visit to emergency department for asthma management. A history of asthma exacerbation significantly correlated with case the fatality rate [p=<0.001]. Patients inhaling prescribed beclomethasone were less likely to have controlled asthma when compared to those on the salmeterol/fluticasone propionate combination. The respective proportions of patients with controlled asthma were beclomethasone(11.4%) and in those using salmeterol/fluticasone propionate (22.7%).When compared to use of the beclomethasone inhaler, participants who had used salmeterol/fluticasone propionate were significantly less likely to have died during the follow up period [p=0.026]. The majority 54/94(57.5%) of those who died with asthma had a co-existing history of rhinitis. Majority (63.9%) reported not having a history of emphysema/chronic bronchitis (Table 2).
Death amongst patients with asthma: age and causes: the median age of the patients at the time of their demise was 25.5 [21-34] years. This was similar in males 25[19-32] as in females 26[21-37] years. The main 44/94(46.8%) cause of death in the cohort of asthma patients was a respiratory condition, including pneumonia, COPD and bronchitis. The second commonest category included patients with HIV, diabetes or kidney diseases 22/94(23.4%). The proportion of patients with gastro-oesophageal reflux disease (GERD) was 20.2%. Cardiovascular diseases accounted for less than 10% mortality. More males (62%) than females (37%) died from respiratory conditions (p=0.002). Death from cardiovascular diseases was only registered in the death certificates of female patients (p=0.001). Mortality due to GERD, and HIV, diabetes or kidney diseases were comparable in both sex (Table 1).
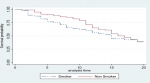
Health service utilisation by asthma patients: health service utilisation was defined in this study as the quantification or depiction of the use of services by asthma patients for the purpose of preventing and curing health problems, promoting maintenance of health and well-being, or obtaining information about one's health status and prognosis. The factors associated with all-cause mortality were not seeing the same doctor or specialist doctor over the two years preceding death. Also, a history of having visited a doctor to get asthma treatment or a hospital admission after a severe asthma attack over the past two years was associated with all-cause mortality [p=<0.001] (Table 3). The Kaplan Meier survival curves (Figure 1) showed significant differences between smokers and non smokers during the first 10 years follow up period (p=0.004). However, there was no significant difference for the last 10 years follow up period. Smokers had a median survival of 15 person years compared to 16 person years for the non smokers.
Kaplan Meier survival curves for clinical characteristics of asthma
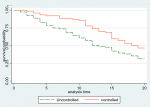
Asthma control status: the Kaplan Meier survival curves (Figure 2) below showed significant differences (p=0.009) in survival during a follow up period of 20 years. Patients who had controlled asthma had a median survival time of 19 person years while those with uncontrolled asthma had a median survival time of 13 person years. The mortality rate amongst those with controlled asthma was 4/100 compared to 6/100 over the 20-year follow up period for those with uncontrolled asthma. Poor asthma control significantly contributed to death, with the hazard ratio of 1.68(p=0.01). Thus, a patient with uncontrolled asthma was 68% more likely to die compared to those who had controlled asthma.
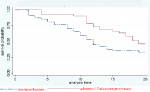
Use and types of inhaled glucocorticosteroids: the log-rank test for equality of survival times between patients with asthma who were prescribed beclomethasone inhaler or salmeterol/fluticasone propionate showed that users of salmeterol/fluticasone propionate had significantly higher survival (p=0.04). The use of salmeterol/fluticasone propionate resulted in a significantly lower mortality rate (4/100) compared to users of the beclomethasone inhaler whose mortality rate was 6/100 over the 20 year follow up period (p=0.04) (Figure 3). Patients who used beclamethasone inhaler were 1.75 times more likely to die over the follow-up period compared to those using salmeterol/fluticasone propionate. The use of ipratropium was a borderline significant hazard ratio with an estimate of 1.98(p=0.07).
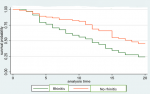
Respiratory co-morbidities: patients with a history of rhinitis had a lower median survival time 12 persons years than those without the history of rhinitis whose median survival time of 17 persons years over the follow up period of 20 years. There were significant differences between asthma patients who indicated history of allergic rhinitisor lack thereof (p=0.03) (Figure 4). Patients with asthma and a history of rhinitis were 1.93 times more likely to die compared with to those without a history of rhinitis. Death rates amongst patients with other co-morbid respiratory conditions, (pneumonia, COPD and bronchitis) were 6/100 patients over the 20-year follow-up period.
Non-respiratory co-morbid conditions: the participants´ survival time also differed by diagnosed conditions. Gastroesophageal reflux diseases had an incidence death rate of 5/100 patients, whilst this figure was 3/100 patientsin patients with cardiovascular diseases. HIV, diabetes and kidney diseases contributed to a combined incidence death rate of 4/100 patients of the follow-up period (Figure 5).
Survival times for asthma patients according to health services utilization: health access options available to the patients were: (a) none, (b) local, nurse run health centre, (c) local public hospital, (d) private general practitioner, (e) specialist physician and/or local private hospital. The specialists were neither allergists nor pulmonologists. The log-rank test showed a lack of significance between the survival of participants who consulted the same or different general practitioners over the 20 year follow-up period. Patients who consultedthe same doctor had a lower mortality rate (5/100) compared to those who consulted multiple doctors, whose mortality rate was 8/100 over a 20-year follow-up period. Seeing a specialist doctor in the first 10 years was associated with better survival contrasted to consulting the specialists during the last 10 years. However, there were no significant differencesin all-cause mortality associated with consultinga specialist doctor for asthma management. (p=0.647). The log-rank test for identifying differences in Kaplan Meier Curves on asthma patients according to doctor visited in the past 2 years did not show significant differences. However, the follow-up period of 5 and 15 years depicted some significant differencesbetween those who visited a doctor in the preceding two years and those who did not visit a doctor in that period. In bivariate analysis, seeing same doctors and a specialist doctor were not a risk factor as compared to seeing different doctors (Table 4).
Multiple cox proportional hazards analysis: a multivariate cox proportional hazard analysis showed that after controlling for smoking, history of rhinitis, the above factors were significant to explain the survival of asthma patients. The model showed that the most significant risk factor for mortality was seeing different doctors (p=0.005). However, those recent exacerbations necessitating hospital admission in the past 2 years were 3.6 times more likely to die due to uncontrolled asthma after adjusting for other factors (smoking, history of rhinitis) (Table 5).
The aim of this study was to determine the survival of asthma patients at a Zimbabwean Central Hospital over a period of 20 years. To the authors´ knowledge, this is the first research to analyse survival of asthma patients attended to at any public hospital in Zimbabwe. This retrospective clinical cohort study revealed that the all-cause mortality rate amongst patients with asthma who were followed up for 20 years was high. The average at death was 25 years. Higher all-cause mortality rates were observed among males compared to females. These findings are comparable to those reported in Brazil [12] and Australia [13]. The reasons why males had a higher risk of death were unclear but could be related to non-adherence to medication and poor health-seeking behaviour. Another plausible explanation for higher male mortality in our setting could be due to gendered differences around smoking behaviour in Zimbabwe with more males being smokers than their female counterparts. Results from this study showed that a history of smoking was a risk factor for death among asthma patients. Previous research has demonstrated that lifetime tobacco consumption increases the risk of death from asthma [14].
The findings from our study showed that poor asthma control was associated with poor outcomes. This was comparable to those reported by Zahrani et al. [15]. Our results that showed most asthma patients had poor asthma control point to the need to use the ACT that can assist in detecting level of asthma control, which can assist in early interventions to achieve better control. The use of either beclomethasone or salmetrol/fluticasone propionate was influenced by access to health care service providers and prescribing practices. Beclomethasone, which was part of the national formulary in the relevant period,was predominantly prescribed at public health facilities, while salmeterol/fluticasone propionate tended to be prescribed by private practitioners and specialist physicians. Access to private or public healthcare services is commonly associated with socioeconomic status (income) and access to health care, which is an indicator for asthma mortality. Therefore, we recommended that services should be determined not by the financial means of the patient, but by their medical needs. Further, there should be uniformity of care for poor and rich. Our study revealed a high prevalence of uncontrolled asthma among those using beclamethasone compared to salmeterol/fluticasone propionate. This maybe becauseuse of ICS/LABA has improved clinical asthma outcomes and reduces the number of exacerbations [16,17], and it does not increase the risk of asthma-related hospitalizations [18], and achieves clinical control of asthma in more patients more rapidly and at a lower dose of ICS than with ICS given alone [19]. This may explain why there was a higher prevalence rate of all-cause mortality among those using beclamethasone compared to salmeterol/ fluticasone propionate. Death in healthcare facilities is an opportunity for medical certification of causes of death and sometimes post mortem evidence of the cause of death. This was the case with our results that revealed more patients were dying at health care facilities and therefore had a medically certified cause of death and in some cases post-mortem examinations. The finding from our study concurred with what was observed in Brazil [12]. Such findings are unsurprising since patients with severe symptoms of asthma require hospitalization.
Concurrent affliction by two or more conditions has more outcomes that are adverse in asthma. This was shown in our study where the co-occurrence of respiratory diseases and cardiovascular disease was significantly related to mortality, a phenomenon that has also been reported in other settings where respiratory disorders were shown to exacerbate death among asthma patients [13, 14]. Our study also showed a high proportion death occurred among asthma patients with GERD. GERD has been shown to be a major contributor of uncontrolled asthma [20]. A major finding was that uncontrolled asthma was related to all-cause mortality. This mandates the implementation of interventions targeting the control of asthma severity within the community and healthcare institutions [21]. This study suggests that clinical characteristics of asthma patients including lack of asthma control, history of atopy and using ICS/LABA offered a survival benefit compared to ICS alone. These clinical characteristics of asthma patients might be related to severity of the condition. In addition, our findings also suggest that patients who consulted a specialist doctor and who visited an emergency department because of asthma in the past 2 years had significantly higher proportion of death. This suggests a link between uncontrolled asthma and mortality. These results echo those reported in Australia and New Zealand [22]. According to Fernandes et al. [12] and Omachi et al. [23], a lack of asthma control is a risk factor for mortality among individuals with severe asthma.
The study concluded that having a smoking history, respiratory disease, cardiovascular disease and uncontrolled asthmawere risk factors for death among asthma patients. Those patients that presented having a history of rhinitis and who had visited emergency departments as a result of their asthma had high risk of death with asthma compared to those that were alive after the 20 years follow-up period. Although, this study was conducted in only one of Zimbabwe´s five central hospitals, it is the only study that has looked at survival of asthma patients locally. We therefore recommend that future studies be done to explore the situation prevailing in other settings within the country to have a better understanding of the survival of asthma patients. There is also need to institute measures aimed at reducing co-morbidity of asthma and cardiovascular diseases and controlling asthma severity in healthcare institutions if we are to reduce risk of death from asthma.
What is known about this topic
- It has been established that asthma patients have a high mortality rate in the health care settings of the Low-to-middle income countries;
- Prior studies have shown that more asthma patients die from asthma due to poor management.
What this study adds
- This study revealed that presents of comorbidities increases mortality rate among asthma patients;
- Use of inhaled corticosteroids was shown to be associated with good survivorship among asthma patients;
- This study found that uncontrolled asthma was one of the major risk factors for the all-cause mortality among asthmatic patients. There was recommended that achieving good control with the use of inhaled corticosteroids could improve patient survivorship.
The authors declare no competing interests.
PN and MJC conceived the idea. PN with the assistance of MJM designed the protocol and revisions were done by MJC and ENS. PN designed the protocol. PN wrote the first draft of the manuscript and all authors (PN, MJC and ENS) reviewed changes. All authors read and approved the manuscript for submission to the journal. All the authors have read and agreed to the final manuscript.
The authors would like to thank the UKZN and OAK foundation who have supported the PN throughout this study. I would like to acknowledge Dr Chester Kalinda and TafadzwaMadanhire for assisting with designing the sample size and data analysis.
Table 1: characteristics for the asthma patients cohort: 1997-2017
Table 2: clinical characteristics of the asthma patients (cohort) n=153
Table 3: health service utilisation by asthma patients
Table 4: bivariate cox regression hazard analyses for demographic characteristics and clinical characteristics
Table 4 suite: bivariate cox regression hazard analyses for health service utilisation and asthma self-management
Table 5: multiple cox proportional hazards analysis for all-cause mortality of asthma patients
Figure 1: Kaplan Meier survival curves for asthma patients by smoking history
Figure 2: Kaplan Meier survival curves for asthma patients showing control of asthma
Figure 3: Kaplan Meier survival curves for asthma patient by use of corticosteroids inhalers
Figure 4: Kaplan Meier survival curves for asthma patients by history of rhinitis
Figure 5: survival of asthma patients by diagnosed conditions
- Global strategy for asthma management and prevention 2015. Global Initiative for Asthma. 2015;149.
- Khalid Al Efraij, Mark FitzGerald J. Current and emerging treatments for severe asthma. Journal of Thoracic Disease. 2015 Nov;7(11):E522-5. PubMed | Google Scholar
- GBD, Chronic Respiratory Disease Collaborators. Global, regional, and national depths, prevalence, disability-adjusted life years, and years lived with disability for chronic obstructive pulmonary disease and asthma, 1990-2015: a systematic analysis for the Global Burden of Disease Study 2015. Lancet Respiratory Medicine. 2017 Sep;5(9):691-706. PubMed | Google Scholar
- Global Initiative for Asthma (GINA). Global strategy for asthma management and prevention. 2014. Accessed November 20, 2020.
- Zimbabwe National Statistics Agency and ICF International. Zimbabwe Demographic and Health Survey 2015: final report. Rockville, Maryland, USA: Zimbabwe National Statistics Agency (ZIMSTAT) and ICF International. 2016. Google Scholar
- MoHCC (Zimbabwe Ministry of Health and Child Care). The National Health profile 2014 Report. Harare, Government of Zimbabwe. 2014.
- World life expectancy.com. Zimbabwe: Asthma. Accessed November 20, 2020.
- WHO. Updated guideline: paediatric emergency triage, assessment and treatment. Geneva: World Health Organization; 2016. Google Scholar
- Global Initiative for Asthma. Global strategy for asthma management and prevention. GINA. 2016.
- Ryan H, Trosclair A, Gfroerer J. Adult current smoking: differences in definitions and prevalence estimates-NHIS and NSDUH, 2008. Journal of Environmental and Public Health. 2012;2012:918368. Google Scholar
- Schoenfeld DJB. Partial residuals for the proportional hazards regression model. Biometrika. 1982;69(1):239-41.
- Fernandes AG, Souza-Machado C, Coelho RC, Franco PA, Esquivel RM, Souza-Machado A et al. Risk factors for death in patients with severe asthma. Jornal Brasileiro de Pneumologia. 2014 Aug;40(4):364-72. PubMed | Google Scholar
- Goeman DP, Abramson MJ, McCarthy EA, Zubrinich CM, Douglass JA. Asthma mortality in Australia in the 21st century: a case series analysis. BMJ open. 2013 Jan 1;3(5):e002539. PubMed | Google Scholar
- D´Amato G, Vitale C, Molino A, Stanziola A, Sanduzzi A, Vatrella A et al. Asthma-related deaths. Multidisciplinary Respiratory Medicine. 2016 Dec;11:37. PubMed | Google Scholar
- Al-Zahrani JM, Ahmad A, Abdullah AH, Khan AM, Al-Bader B, Baharoon S et al. Factors associated with poor asthma control in the outpatient clinic setting. Annals of Thoracic Medicine. 2015 Apr;10(2):100. PubMed | Google Scholar
- O'Byrne PM, Barnes PJ, Rodriguez-Roisin R, Runnerstrom E, Sandstrom T, Svensson K et al. Low dose inhaled budesonide and formoterol in mild persistent asthma: the OPTIMA randomized trial. Am J RespirCrit Care Med. 2001;164(8 Pt 1):1392-7. PubMed | Google Scholar
- Ni Chroinin M, Greenstone I, Lasserson TJ, Ducharme FM. Addition of inhaled long-acting beta2-agonists to inhaled steroids as first line therapy for persistent asthma in steroid-naive adults and children. Cochrane Database System Rev. 2009 Oct 7;(4):CD005307. PubMed | Google Scholar
- Jaeschke R, O'Byrne PM, Mejza F, Nair P, Lesniak W, Brozek J et al. The safety of long-acting beta-agonists among patients with asthma using inhaled corticosteroids: systematic review and metaanalysis. Am J RespirCrit Care Med. 2008 Nov 15;178(10):1009-16. PubMed | Google Scholar
- Bateman ED, Boushey HA, Bousquet J, Busse WW, Clark TJ, Pauwels RA et al. Can guideline-defined asthma control be achieved? The Gaining Optimal Asthma ControL study. 2004;170(8):836-44. PubMed | Google Scholar
- Ates F, Vaezi MF. Insight into the relationship between gastroesophageal reflux disease and asthma. Gastroenterology &hepatology. 2014 Nov;10(11):729. PubMed | Google Scholar
- Fassl BA, Nkoy FL, Stone BL, Srivastava R, Simon TD, Uchida DA et al. The Joint Commission Children's Asthma Care quality measures and asthma readmissions. Pediatrics. 2012;130(3):482-91. PubMed | Google Scholar
- Jalaludin BB, Smith MA, Cheyxy T, Orrxy NJ, Smith WT, Leeder SR. Risk factors for asthma deaths: a population-based, case-control study. Australian and New Zealand Journal of Public Health. 1999 Dec;23(6):595-600. PubMed | Google Scholar
- Omachi TA, Iribarren C, Sarkar U, Tolstykh I, Yelin EH, Blanc PD et al. Risk factors for death in adults with severe asthma. Annals of Allergy, Asthma & Immunology. 2008 Aug 1;101(2):130-6. PubMed | Google Scholar