Bilateral cataract in a teenage girl with type 1 diabetes (T1D): case report
Djibril Boiro, Lamine Thiam, Idrissa Basse, Mar Ndiaye, Aliou Abdoulaye Ndongo, Ndiogou Seck, Amadou Sow, Babacar Niang, Demba Diedhiou, Modou Gueye, Ousmane Ndiaye
Corresponding author: Djibril Boiro, Abass Ndao Hospital, Cheikh Anta Diop University Dakar, Dakar, Senegal 
Received: 22 Jun 2021 - Accepted: 25 Jul 2021 - Published: 29 Jul 2021
Domain: Pediatric endocrinology
Keywords: Cataract, type 1 diabetes, adolescent, case report
©Djibril Boiro et al. PAMJ Clinical Medicine (ISSN: 2707-2797). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Djibril Boiro et al. Bilateral cataract in a teenage girl with type 1 diabetes (T1D): case report. PAMJ Clinical Medicine. 2021;6:35. [doi: 10.11604/pamj-cm.2021.6.35.30477]
Available online at: https://www.clinical-medicine.panafrican-med-journal.com//content/article/6/35/full
Bilateral cataract in a teenage girl with type 1 diabetes (T1D): case report
![]() Djibril Boiro1,&, Lamine Thiam2, Idrissa Basse3, Mar Ndiaye4, Aliou Abdoulaye Ndongo1, Ndiogou Seck5,
Djibril Boiro1,&, Lamine Thiam2, Idrissa Basse3, Mar Ndiaye4, Aliou Abdoulaye Ndongo1, Ndiogou Seck5, ![]() Amadou Sow1, Babacar Niang1, Demba Diedhiou1, Modou Gueye1,
Amadou Sow1, Babacar Niang1, Demba Diedhiou1, Modou Gueye1, ![]() Ousmane Ndiaye1
Ousmane Ndiaye1
&Corresponding author
Cataract is a rare complication in young type 1 diabetics. We describe the case of an 18-year-old adolescent girl with diabetes since the age of 12 following diabetic ketoacidosis. She was on regular insulin with a premix and a rapid. She had poorly balanced diabetes with an annual HbA1c averaging 10.6%. During diagnosis, she complained of ocular pain and a reduced visual acuity confirmed at 1/10. Clouding of the lens was identified and she received surgical intervention. The postoperative course was good with a visual acuity recovery of 8/10 and a normal ocular fundus. Cataracts should be screened for in young diabetics as well as other complications related to type 1 diabetes (T1D).
A cataract is a rare ocular complication of T1D among pediatric patients with an estimated prevalence of 0.7% to 3.4% [1]. It can go up to 16% in Haitian or African patients [2]. The pathophysiological mechanisms of cataract formation at the onset of T1D have not been fully elucidated. The most widely accepted theory is the activation of the polyol pathway, osmotic damage, and oxidative stress due to hyperglycemia leading to clouding of the lens in diabetic patients [3]. Surgical treatment remains the gold standard [4]. We describe the case of a teenage girl who suddenly presented a severe decline of the visual acuity.
Patient and observation: it was an 18-year-old teenage girl with type 1 diabetes discovered during ketoacidosis in 2014 and followed in our department since 2018. Her mother has type 2 diabetes, there is no parental consanguinity and no history of familial cataract. She had menstruated at the age of 13 and is currently in high school. She was on insulin with three injections per day with a premixed (Rapid-NPH) 30/70 in the morning and evening as well as a rapid at noon, for a total 0.7IU/kg day. She ate three meals and snacks often in between meals. Blood sugar control is rare. She practices physical activity (gymnastics) for 5 hours per week. She had several hospitalizations for ketoacidosis. Her average glycated hemoglobin over the past year was at 10.6%. She complained of bilateral eye pain with reduced visual acuity for several months.
Clinical findings: on examination: weight: 55kg, height: 177cm, BMI: 17.57kg/m2, PA100/70mmHg. The general condition was maintained, and the rest of physical examination was within normal limits. The search for microalbuminuria was negative; an ophthalmic consultation with fundus examination was requested.
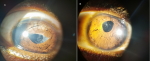
Diagnosis:at diagnosis, the ophthalmologic examination (Table 1) found a visual acuity of 1/10 on the right and just a light perception on the left. Examination of the lens of both eyes revealed cataracts (Figure 1) and an inaccessible fundus. The diagnosis of secondary bilateral cataract to poorly balanced diabetes was made.
Therapeutic interventions: two cataract surgeries 15 days apart were performed after strict glycemic control and ocular echobiometry. We performed an extra capsular extraction (Figure 2) with the placement of a posterior chamber implant under sub-tenonian anesthesia.
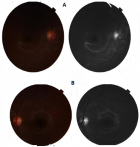
Follow-up and outcome of interventions: the postoperative course was normal for both eyes. The stitches were removed 60 days after surgery for each eye. We noted secondary capsulosis in the right eye which prompted a needle capsulotomy under local anesthesia. At the control examination (Table 2), visual acuity was normalized to 8/10 for both eyes. Bilateral pseudophakia was noted (Figure 3) and the retinograph (Figure 4) was normal on both sides.
A cataract may be the first sign of T1D or it occurs within 6 months of a diagnosis of T1D in most pediatric patients [5]. For our patient, the diagnosis was made 6 years after the diagnosis of diabetes. It appears to be a late onset or delayed diagnosis in the absence of an ophthalmologic consultation. Authors have diagnosed cases of cataracts one month before the diagnosis of diabetes. Some cases was diagnosed one month before the diagnosis of diabetes [5]. The diagnosis age varies. Wilson et al. reported the average age of diagnosis at 11.7 years. The youngest patients described in the literature with early diabetic cataracts were 5 years old, but many patients were adolescents as in our case [6,7]. Most authors have reported that cataracts were significantly associated with female patients [8,9]. However, lafusco et al. reported an equal gender distribution in the pediatric population with T1D [7]. Our patient had several hospitalizations for ketoacidosis. Her average glycated hemoglobin over the past year was 10.6%. High blood sugar and hemoglobin A1c levels at the time of diagnosis are associated with an increased risk of developing cataracts [7,10]. Lafisco et al. showed in their study that for each percentage point of 12.8 to 14.1% of the level of HbA1c, the appearance of early diabetic cataract increased by 3.6 times [7]. Currently, there are many experimental therapies for the treatment of diabetic cataracts, but cataract surgery remains the gold standard in the treatment of diabetic cataracts [11]. The postoperative course is generally favorable with good recovery of the visual acuity. According to Wilson et al. nineteen out of twenty-three operated eyes had better postoperative visual acuity corrected at 20/40 or better [5].
Although rare, cataracts in young diabetics must be screened as well as other complications of type 1 diabetes. Surgery is essential but is not without risk, hence the importance of emphasizing prevention by improving the patients' glycemic control.
The authors declare no competing interests.
Djibril Boiro; final draft. Lamine Thiam; bibliographic search. Idrissa Basse; formatting first draft. Mar Ndiaye; drafting of the ophthalmology section. Aliou A. Ndongo, Ndiogou Seck, Amadou Sow, Babacar Niang, Demba Diedhiou, Modou Gueye, Ousmane Ndiaye; corrections and contributions. All the authors have read and agreed to the final manuscript.
Table 1: results of the ophthalmological examination
Table 2: results of the ophthalmologic examination after surgery
Figure 1: examination of the lens of both eyes revealed cataracts and an inaccessible fundus (A: right eye, B: left eye)
Figure 2: lens after extra capsular extraction
Figure 3: eyes after cataract extraction (A: right eye, B: left eye)
Figure 4: normal retinography on both sides (A:right eye, B: left eye)
- Šimunović M, Paradžik M, Škrabić R, Unić I, Bućan K, Škrabić V. Cataract as early ocular complication in children and adolescents with type 1 diabetes mellitus. Int J Endocrinol. 2018 Mar 20;2018:6763586. PubMed | Google Scholar
- Robinson ME, Altenor K, Carpenter C, Ric B, Jean-Baptiste E, Von Oettingen J. High rates of ocular complications in a cohort of Haitian children and adolescents with diabetes. Pediatr Diabetes. 2018 Apr 26. PubMed | Google Scholar
- Quintos JB, Torga AP, Simon MA. Diabetes cataract in a 10-year-old girl with new-onset type 1 diabetes mellitus. BMJ Case Rep. 2019 Jan 29;12(1):e227437. PubMed | Google Scholar
- Pollreisz A, Schmidt-Erfurth U. Diabetic cataract-pathogenesis, epidemiology and treatment. J Ophthalmol. 2010;2010:608751. PubMed | Google Scholar
- Wilson E, Levin AV, Trivedi RH, Stacey JK, Laurie AE, John RA et al. Cataract associated with type-1 diabetes mellitus in the pediatric population. J AAPOS. 2007 Apr;11(2):162-5. PubMed | Google Scholar
- Ciro C, Roberto D, Francesco P, Dario I, Francesca L, Francesco P. Bilateral isolated acute cataracts in three newly diagnosed insulin dependent diabetes mellitus young patients. Diabetes Res Clin Pract. 2007 May;76(2):313-5. PubMed | Google Scholar
- Lafusco F. Prisco M, Romano R, Dell'Omo R, Libondi T, Costagliola C. Acute juvenile cataract in newly diag-nosed type 1 diabetic patients: a description of six cases. Pediatr Diabetes. 2011 Nov;12(7):642-8. PubMed | Google Scholar
- Montgomery L, Batch JA. Cataracts in insulin- dependent diabetes mellitus: sixteen years´ experience in children and adolescents. J Paediatr Child Health. 1998 Apr;34(2):179-82. PubMed | Google Scholar
- Wen-Li L, Po-Chih S, Chen-Hao L, Yu-Tsun S, Li-Min C. High risk of arly cataracts in young type 1 diabetes group: a nationwide cohort study. International Journal of Endocrinology. 2020;8160256. Google Scholar
- Datta V, Swift PG, Woodruff GH, Harris RF. Metabolic cataracts in newly diagnosed diabetes. Arch Dis Child. 1997 Feb;76(2):118-20. PubMed | Google Scholar
- Marko Šimunović, Martina Paradžik, Roko Škrabić, Ivana Unić, Kajo Bućan, Veselin Škrabić. Cataract as early ocular complication in children and adolescents with type 1 diabetes mellitus. Int J Endocrinol. 2018 Mar 20;2018:6763586. PubMed | Google Scholar