Cryptorchid testicular torsion: a case report
Ossama Jalal, Imad Ziouziou
Corresponding author: Ossama Jalal, Faculté de Médecine et de Pharmacie d´Agadir, Urology Departement, CHU Agadir, Morocco 
Received: 11 Jun 2021 - Accepted: 02 Aug 2021 - Published: 20 Aug 2021
Domain: Urology
Keywords: Cryptorchid, torsion, undescended testis, inguinal pain, case report
©Ossama Jalal et al. PAMJ Clinical Medicine (ISSN: 2707-2797). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Ossama Jalal et al. Cryptorchid testicular torsion: a case report. PAMJ Clinical Medicine. 2021;6:41. [doi: 10.11604/pamj-cm.2021.6.41.30302]
Available online at: https://www.clinical-medicine.panafrican-med-journal.com//content/article/6/41/full
Cryptorchid testicular torsion: a case report
&Corresponding author
Torsion of undescended testis is an uncommon surgical emergency rarely documented. We report a case of a 17 years old patient with an acute inguinal pain with an empty hemiscrotum related to torsion of an inguinal undescended testis. We discuss the clinical presentation, paraclinical investigation, and the outcome after surgery. Our objective is to highlight the importance of a meticulous clinical examination in front of inguinal pain.
The spermatic cord torsion is a well-recognized urological emergency [1]. However the torsion of a cryptorchid testicle is described in the urology literature; but not as well known by the clinician, which could be confused with many common inguinal pain. In this article we present a case of a 17-year-old male patient with a torsion of an undescended testicul. And discuss diagnostic and therapeutic of this rare emergency.
Patient information: a 17-year-old male patient was admitted in the emergency department for an acute left inguinal pain installed suddenly for 30 hours. No recent volume increase of both testicle was noticed. There was no history of urinary symptoms, neither scrotal pain neither of trauma, except an undescended left testicle diagnosed at the age of 3 years.
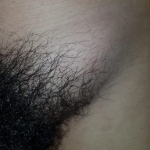
Clinical findings: the physical examination revealed a maximum of pain in the left inguinal area related to a 3.5 x 2 cm mass (Figure 1). The mass was fix with no induration, with discreet local erythema. The left hemiscrotum was empty, and the right testicle was normal, with no fever.
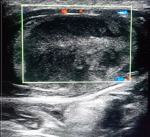
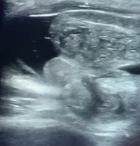
Diagnostic assessment: a scrotal Doppler-ultrasound was performed immediately that revealed a heterogeneous echotexture of an inguinal testicle, with no doppler flow associated to a small reactional hydrocele (Figure 2), and individualization of many spins of the left spermatic cord (positive whirlpool sign) [2] (Figure 3).
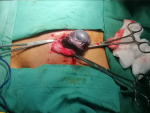
Therapeutic intervention: the patient underwent a surgical exploration of the left inguinal pouch. An intravaginal torted cryptorchid left testicle was identified (Figure 4) with a necrotic blue color. There was no recoloration after the surgical detorsion, and an orchidectomy was performed.
Follow-up and outcomes: the patient had a simple enventful postoperative course, and discharged home in the third day. Pathological examination revealed a necrotic testicle.
Patient perspective: the patient and his parent were informed of about the all procedure, complications and outcome, and they were satisfied about it.
Informed consent: a written informed consent to permit publish of the patient case was signed by the father.
The cryptorchidism or undescended testis is a rare congenital malformation, that could be responsible of many serious sequelae such subfertility, testicular malignancy, testicular torsion. It may be accompanied by inguinal hernia. Ivy HY Chan et al. estimated its incidence at 22.8 per 10000 live births or 8% of mal births in other studies [3,4]. In fact, the rate of cryptorchidism is estimated at 1.0 to 4.6% at birth in term and/or birth weight >2.5 kg; at the age of 3 months from 0.9 to 1.6% and at 1 year from 1.0 to 1.5%. At 6 years of age, Cryptorchidism rate is under 2.6%, and under 6.6% at the age of 11 years; and at 15 years in 1.6-2.2% of the boys. At an older age, the Cryptorchidism becomes rare [5]. The testicular descent start at the eighth month of fetal life. It transits from its first abdominal localization into the scrotum through the inguinal canal [6]. Many entities of undescended testis were described: abdominal, inguinal, and subinguinal. It´s called cryptorchidism when the migration of the testis is interrupted in the usual path of descent which is the inguinal canal (70%). When the testis is found out of this path it´s called ectopic testis (30%), and could be localized into Scarpa´s triangle, the base of penis, oblique muscle, ischial spine or into the contralateral inguinal canal [7,8]. Early surgical cure of cryptorchidism is recommended in order to enhance preserving of germinal cells, and also to reduce the rate of infertility [9].
The first torsion of a cryptorchid testis was reported by Delasiauve et al. in 1840, which was taken for a strangled inguinal hernia and was treated by orchidectomy. 15 years later Curling et al. reported the first successful preservation of a torted cryptorchid testicle, that has been untwisted and fixed in the scrotum with a stitch on the dartos [10]. Although many series of cryptorchid testicular torsion cases where reported, the physiopathology remains unexplained. The association with spastic paraplegia was reported by Johnson and Holmes et al. in 1964 and Phillips and Holmes in 1972, meanwhile "scissor leg deformity" (adduction contractures of the hips), abnormal contraction of the cremasteric muscle may be incriminated [7,8]. Nevertheless in our case neither of these anomalies was founded. Moreover, Williamson et al. suggested that the cryptorchidism increased 10 times the risk of torsion. He reported 6.8% of patients with testicular torsion to have an undescended testis [8,11]. The first described torsion of cryptorchid torsion was taken for a strangled inguinal hernia. However, a good clinical examination can be useful and sufficient to diagnose a cryptorchid testicular torsion, when the acute onset inguinal pain and swelling is associated to an empty ipsilateral hemiscrotum [12]. As for the ectopic abdominal testis, the clinical diagnostic may be more challenging, including the non-specific abdominal or inguinal pain, vomiting and restlessness [13], simulating an acute abdomen such incarcerated inguinal hernia, appendicitis and viral gastroenteritis, and ileus [12].
Many studies have reported the use of Doppler ultrasound replacing the historical use of thermographic imaging and scintigraphy. Its importance lies in making decision and eliminating an incarcerated hernia and low abdomen pain etiologies [7,12], especially that it´s available and it´s a non-invasive examination. The existing of a positive whirlpool sign is a valuable diagnostic tool [2]. In fact color doppler ultrasound has 77% of sensitivity and 90% of specificity in testicular torsion diagnostic [12]. It may be normal when the torsion is brief, if not the testis appears inhomogeneous and hypoechoic with decreased or absent Doppler flow [7] enlarged and diffusely edematous [9]. however Slijper et al. has reported two misdiagnosis cases of undescended testicle torsion taken for incarcerated hernia although the Doppler ultrasound has been performed [14], and only the surgical exploration rectified the diagnostic. Being an extreme surgical emergency the use of doppler ultrasound should not be systematic in front of a suspicion of undescended testicular torsion. However the meticulous clinical exams finding a low abdominal pain with absence of an intra-scrotal testicle justify a surgical exploration. The use of CT described by Jiun-Hung Geng et al. finding a isodense or heterodense inguinal mass with hemorrhage and infraction, as well he used Technetium Tc-99m scrotal scintigraphy showing a "Cold spot" related to a avascular testis [15]. The interest of this investigation in the context of emergency remains unclear and not recommended. In our case we could perform the Doppler ultrasound while preparing the surgery room, without delay of the intervention.
Reviewing literature data, the rate of solvation for torsed normally descended testis is proximately 56% - 70% - 92%, this rate is lower for undescended testis which is about 10% [9,12]. All depending on the delay of intervention. Spermatic and sartoli cells necrosis begins in 4 hours after the torsion [7]. Testicular damage begins after as little as 4 hours. A 360 degrees rotation and 24 hours torsion seems to be associated to gangrene of testis [16]. Immediate surgical exploration is the treatment of choice for acute testicular torsion, regardless of its position. The detorsion is performed, and the viability is evaluated [1]. No proved viability predictive parameters are described. Although Cimado et al. predicts that in front of symptoms unset longer than 10 hours, no flow on Doppler ultrasound and the absence of bleeding 10 min after incision of the tunica albuginea, the orchiectomy is the appropriate attitude [17]. A recent study recommends a second look exploration after 48 hours in order to assess post-operative viability and rectify treatment [18]. Orchidopexy is indicated when the testicle is available. Otherwise, orchidectomy is the treatment of choice in front of non-available testis. Which suggested in the most cases, in particular in adult patients [15]. Orchidopexy of the ipsilateral testis is indicated by the majority of authors [8]. Justify as the congenital malformation of tunica vaginalis responsible for the torsion is usually bilateral [19]. Meanwhile, the risk of torsion of the other testis is small [16]. In our case, an ipsilateral orchidopexy is planned in a few weeks. And the torsion risk was explained to the patient and his family.
The torsion of cryptorchid testicle is an unusual emergency that may be misdiagnosed especially among the pediatric population, when the undescended testicle is not yet known. Analyzing its consequences, early cure of undescended testis is recommended, to avoid the increase risk of torsion. Meanwhile the examination of external genital organs in front of inguinal pain must be considered by physician. Finding an empty hemiscrotum must make the physician think of torsion of an undescended testis. The recourse to radiologic investigation should not be systematic and never delays the surgical exploration.
The authors declare no competing interests.
All the authors have read and agreed to the final manuscript.
Figure 1: inguinal area with a visible mass
Figure 2: ultrasound with no Doppler flow
Figure 3: positive whirlpool sign
Figure 4: surgical exploration: necrotic testis
- Naouar S, Braiek S, El Kamel R. Testicular torsion in undescended testis: a persistent challenge. Asian Journal of Urology. 2017;4(2):111-115. PubMed | Google Scholar
- McDowall J, Adam A, Gerber L, Enyuma COA, Aigbodion SJ, Buchanan S et al. The ultrasonographic "whirlpool sign" in testicular torsion: valuable tool or waste of valuable time? a systematic review and meta-analysis. Emerg Radiol. 2018;25(3):281-292. PubMed | Google Scholar
- Chan IH, Wong KK. Common urological problems in children: inguinoscrotal pathologies. Hong Kong Med J. 2017;23(3):272-81. PubMed | Google Scholar
- Carvalho FF, Talati I, Krill A. Intravaginal torsion of undescended testes. BMJ Case Rep. 2019 Nov 26;12(11):e231244. PubMed | Google Scholar
- Sijstermans K, Hack WW, Meijer RW, van der Voort-Doedens LM. The frequency of undescended testis from birth to adulthood: a review. Int J Androl. 2008 Feb;31(1):1-11. PubMed | Google Scholar
- Mowad JJ, Konvolinka CW. Torsion of undescended testis. Urology. 1978;12(5):567-8. PubMed | Google Scholar
- Candocia FJ, Sack-Solomon K. An infant with testicular torsion in the inguinal canal. Pediatr Radiol. 2003;33(10):722-4. PubMed | Google Scholar
- Schultz KE, Walker J. Testicular torsion in undescended testes. Ann Emerg Med. 1984;13(7):567-9. PubMed | Google Scholar
- Zilberman D, Inbar Y, Heyman Z, Shinhar D, Bilik R, Avigad I et al. Torsion of the cryptorchid testis can it be salvaged. J Urol. 2006;175(6):2287-9. PubMed | Google Scholar
- Nöske HD, Kraus SW, Altinkilic BM, Weidner W. Historical milestones regarding torsion of the scrotal organs. J Urol. 1998;159(1):13-6. PubMed | Google Scholar
- Williamson RC. Torsion of the testis and allied conditions. Br J Surg. 1976;63(6):465-76. PubMed | Google Scholar
- Moore CP, Marr JK, Huang CJ. Cryptorchid testicular torsion. Pediatr Emerg Care. 2011;27(2):121-3. PubMed | Google Scholar
- Malik MIK, Abbas J, Sabri S, Michael G, Ellenbogen S. Torsion of undescended abdominal testicle in a 16-year-old and its management. BMJ Case Rep. 2020 Jan 29;13(1):e232179. PubMed | Google Scholar
- Slijper N, Sukhotnik I, Toubi A, Mogilner J. Critical validation of ultrasound Doppler in the diagnosis of torsion of undescended testis. Isr Med Assoc J. 2007;9(2):99-101. PubMed | Google Scholar
- Geng JH, Huang CN. Torsion of undescended testis: clinical, imaging, and surgical findings. Urological Science. 2014;25(1):31-34. Google Scholar
- Ahmad SN, Chowdri NA, Parray FQ, Wani RA. Torsion of undescended testis. The Indian Journal of Surgery. 2006;68:106-7. Google Scholar
- Cimador M, DiPace MR, Castagnetti M, DeGrazia E. Predictors of testicular viability in testicular torsion. J Pediatr Urol. 2007;3(5):387-90. PubMed | Google Scholar
- Rouzrokh M, Mirshemirani A, Khaleghnejad-Tabari A. Outcomes of second look exploration in testicular torsion of children. Iranian Journal of Pediatrics. 2015;25(4):e528-e528. PubMed | Google Scholar
- Mishriki SF, Winkle DC, Frank JD. Fixation of a single testis: always, sometimes or never. Br J Urol. 1992;69(3):311-3. PubMed | Google Scholar