Tumoral calcinosis in a Malawian teenager: case report and literature review
Ronald Chitatanga, Leonard Banza
Corresponding author: Ronald Chitatanga, Department of Pediatrics and Child Health, Queen Elizabeth Central Hospital, Blantyre, Malawi 
Received: 31 Aug 2021 - Accepted: 02 Sep 2021 - Published: 12 Nov 2021
Domain: General surgery,Orthopedic surgery
Keywords: Tumoral calcinosis, mutation, phosphates, subcutaneous tissue, case report
©Ronald Chitatanga et al. PAMJ Clinical Medicine (ISSN: 2707-2797). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Ronald Chitatanga et al. Tumoral calcinosis in a Malawian teenager: case report and literature review. PAMJ Clinical Medicine. 2021;7:11. [doi: 10.11604/pamj-cm.2021.7.11.31459]
Available online at: https://www.clinical-medicine.panafrican-med-journal.com//content/article/7/11/full
Tumoral calcinosis in a Malawian teenager: case report and literature review
&Corresponding author
Tumoral calcinosis is a rare and benign condition that is characterised by the deposition of calcium salts in the soft tissues near large joints. Although, it has an unclear aetiology, a pathogenesis-based classification has subdivided it into three types: primary normo-phosphataemic tumoral calcinosis, primary hyper-phosphataemic tumoral calcinosis, and secondary tumoral calcinosis, characterized by the presence of an underlying disorder. We report the case of a 16-year old female with a six-year history of bilateral greater trochanteric nodules that were producing a whitish discharge. She had no associated fever. On physical examination, her lower limbs revealed two irregular and non-tender nodules bilaterally located around the greater trochanteric region. The nodules had centrally located sinuses that drained a non-foul whitish discharge. She had normal range of motion around both hip joints. Her biochemical profile showed normal serum creatinine and calcium levels, however, with an elevated serum phosphorous level. An anterior-posterior pelvic radiograph revealed massive soft tissue calcifications over both greater trochanteric regions that spared the bones and joint spaces. A histological examination of the whitish discharge demonstrated a fibrous connective tissue with amorphous calcified material. The diagnosis of primary hyper-phosphataemic tumoral calcinosis was made. The patient made an uneventful recovery after subscribing to a low-calcium and phosphate diet coupled with the prescription of a daily phosphate-binding drug and surgical excision of the calcifications. This case report emphasizes the importance of considering tumoral calcinosis as a differential diagnosis for every patient presenting with a non-resolving spontaneously appearing nodule that produces a whitish discharge.
Tumoral calcinosis (TC) is a rare and benign condition that is characterised by the deposition of calcium salts, primarily consisting of hydroxyapatite crystals, in the soft tissues near large joints [1]. Since its first description in 1943 [2], this disease has less than 100 genetically confirmed cases reported in literature [3]. Additionally, due to the scarcity of cases and similar presentation to more common conditions, diagnosis is challenging. In this paper, we report a case of tumoral calcinosis of the lateral hip in a Malawian teenager. We present this case because TC is rare with the hyperphosphataemic type, additionally, being extremely rare [3].
Patient information
A previously healthy 16-year-old female, presented with a six-year history of non-regressing nodules, bilaterally located on both greater-trochanteric regions. The nodules both had sinuses that produced a continuous whitish discharge for the same period of time. Her nodules spontaneously appeared six years prior, with the right developing first and the left following suit in a month. They were painless and progressed in size for three months to approximately 5cm in diameter and then developed sinuses. There was no prior febrile illness or history of trauma to the affected areas, furthermore, she was able to walk and was in overall good health. She had no family history of similar diseases. She first presented to a health centre 3 months after symptom onset and upon assessment there, a diagnosis of bilateral greater trochanteric abscesses was made with a subsequent “incision and drainage” being performed. Clinicians noted the drainage of “pus” from both sides. A total of 5 “incision and drainage” procedures were performed in the six-year duration, with no improvement of symptoms and on each occasion clinicians noting to drain “pus”.
Clinical findings
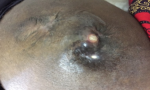
On assessment, she had pale conjunctiva with a BMI of 19.1kg/m². Her lower limbs revealed two irregular nodules bilaterally located around the greater trochanteric region. The nodules were 5cm in diameter and had centrally located sinuses. These sinuses (Figure 1) measured approximately 1cm in diameter and had surrounding hyper-pigmented skin. The discharge from either sinuses was whitish and non-foul smelling. The nodules were both non-tender and firm. She had normal range of motion around both hip joints. The lower limbs were normal looking and symmetrical with good neurovascular status. The rest of the systemic exam was non-remarkable.
Diagnostic assessment
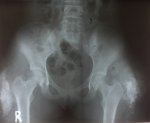
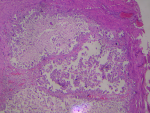
Her Full Blood Count (FBC) revealed; a normal white Blood Cell Count (WBC) of 8,490 cells/μl, a slightly reduced Red Blood-Cell count (RBC) of 3,930,000 cells/μl and a microcytic anaemia of 8.5g/dL. Additional renal function tests (Table 1) showed; a normal serum calcium of 8.9mg/dl, a high Serum phosphorous of 10.5mg/dl and a normal creatinine of 0.7mg/dl. Anterior-Posterior (AP) pelvic radiograph (Figure 2) revealed massive soft tissue calcifications over both greater trochanteric regions. The bones and joint spaces in these areas were spared. Computer Tomography services were not utilized as a result of financial limitations. Histological examination (Figure 3) of the discharge taken from the right sinus showed a fibrous connective tissue with amorphous calcified material boarded by a florid proliferation of macrophages and multinucleated, osteoclast-like giant cells.
Diagnosis
Factoring in the patient history, clinical assessment and diagnostic assessment, the final diagnosis of primary hyper-phosphataemic tumoral calcinosis of the greater-trochanteric region was made. Other differential diagnosis considered were neoplastic diseases such as osteosarcoma and hyper-phosphataemia as a result of chronic kidney failure.
Therapeutic interventions
Her medical management included restricting the consumption of high calcium and phosphate food. She was also prescribed oral Calcium carbonate 250mg to be taken 2 times (with meals) per day for two months. She underwent a successful excision surgery after completing a three-month course of oral haematinics (Ferrous sulphate 200mg twice a day for three months). Her preference of a three-month course of haematinics instead of a whole blood transfusion was because of religious beliefs.
Follow-up and outcome of interventions
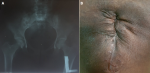
The patient made an uneventful recovery post-operatively and clinical follow-up over the next six months was unremarkable. Repeat AP pelvic radiograph (Figure 4) showed complete resolution of calcifications.
Patient perspective
The patient described life, in the six years preceding her final diagnosis of tumoral calcinosis, as hopeless because her life and school progress was mostly affected. She was in and out of hospital with no improvement. After her ultimate recovery, she is now fully attending school with no problems and is now a more confident person. The treatment she received did not give her any long-term side effects or disabilities. She is glad to be fully recovered.
Informed consent
The patient provided informed consent for all treatments given, both medical and surgical, and additionally to publish this case report.
TC falls under a group of disorders called Calcinosis cutis [1] which is a descriptive term for the deposition of insoluble calcium salts in the cutaneous and subcutaneous tissue [4]. Calcinosis cutis is classified based on the aetiology of calcium deposition and the subtypes are: dystrophic, metastatic, idiopathic, iatrogenic, and calciphylaxis [4]. Tumoral calcinosis falls under idiopathic calcinosis cutis which is a subtype where the occurrence of calcium deposition takes place in the absence of any tissue damage or metabolic disorder [4].
General characteristics of the calcified nodules are; a large sized, juxta-articular located, progressive enlargement with a tendency to recur after surgical removal and the ability to encase adjacent normal structures [1]. Common locations of the calcifications are the hip, elbow, scapula, foot, leg, knee, and hand, with the hip (greater trochanteric bursa) being the most common one [5]. Symmetrical and bilateral involvement is commonly seen [1]. Although there is no sex predilection, patients most frequently affected have been those of African descent who are typically in their first two decades of life [5]. Our patient is an African teenager who had lesions on the hip.
The pathogenesis of TC remains uncertain, however, a classification was formulated by Smack et al. [6] after a review of cases. It subdivides tumoral calcinosis into three types: primary normo-phosphataemic tumoral calcinosis, primary hyper-phosphataemic tumoral calcinosis, and secondary tumoral calcinosis, characterized by the presence of an underlying disorder, usually chronic renal failure. The present case fits into the primary hyper-phosphataemic type which is characterised by normo-calcemia and hyper-phosphataemia [3]. Genetic predisposition is a feature of this type of TC where hyper-phosphataemia arises due to reduced urinary phosphate excretion caused by recessive genetic mutations that cause the inactivation of a phosphoturic hormone [3,4].
Plain radiographs, which are often diagnostic, show a lobulated calcific mass within soft tissues, which is typically cystic, has a bursal distribution and usually affects extensor surfaces [5]. Axial Computer Tomography (CT) better delineates the mass. Finally, histopathologic examination reveals, epithelioid elements and multinucleated giant cells surrounding calcium granules [5]. Despite not showing any evidence of familial predisposition, the clinical features, biochemical profile, radiological and histological findings, displayed by the patient, all supported the diagnosis of TC. Spontaneous regression of TC does not occur regardless of being a benign condition [1]. Treatment centres on the initiation of a phosphate restricted diet and the daily intake of a phosphate binding drug, typically aluminium hydroxide [7]. Additionally, the option of using Acetazolamide has been successfully demonstrated for TC resistant to the phosphate deprivation treatment [8]. Our patient was on Calcium Carbonate, another effective phosphate binding drug, which however predisposes people episodes of hypercalcaemia if used in high doses in the long term [9]. Surgical excision of the calcification is paramount to treating the symptoms and reducing recurrence rates [10]. However, even with holistic treatment, recurrences have been reported.
This case emphasizes the fact that tumoral calcinosis, however rare, should be included in the differential diagnosis of a subcutaneous lump adjacent to a joint, especially in an African patient in their first two decades of life. Additionally, because the patient presented as a classic patient with an abscess requiring Incision and drainage, the presentation compels medical practitioners to thoroughly assess seemingly classical-presenting conditions, in order to avoid misdiagnosing disease.
The authors declare no competing interests.
Both authors were involved in the direct patient care of the patient. RC wrote the first draft of the case report and LB assisted in its revision. Both authors have read and approved the final version of the case report.
Table 1: renal function tests
Figure 1: sinus on the left greater trochanteric region
Figure 2: AP pelvic radiograph taken before surgical excision
Figure 3: histological photomicrograph of the discharge from the sinus showing a fibrous connective tissue with amorphous calcified material boarded by macrophages and osteoclast-like giant cells
Figure 4: clinical follow-up after treatment: (A) AP pelvic radiograph; (B) healing surgical scar after excision
The authors acknowledge the assistance of Dr. Maurice Mulenga, a Pathologist working at Kamuzu Central Hospital, for performing the histopathological examination of the patients� specimen.
- Alam A, Sree Ram M, Manrai K, Bhardwaj R. Tumoral Calcinosis. Medical Journal Armed Forces India. 2007 Apr 1;63(2):180-1. PubMed | Google Scholar
- Inclan A, Leon P, Camejo MG. Tumoral calcinosis. Journal of the American Medical Association. 1943 Feb 13;121(7):490-5. Google Scholar
- Vivek Tiwari, Farah Zahra. Hyperphosphatemic Tumoral Calcinosis. 2021. Accessed 2021 Aug 31.
- Kristen H Fernandez, Dana S Ward. Calcinosis cutis: etiology and patient evaluation . 2021. Accessed 2021 Aug 31.
- Olsen KM, Chew FS. Tumoral Calcinosis: Pearls, Polemics, and Alternative Possibilities. RadioGraphics. 2006 May 1;26(3):871-8. PubMed | Google Scholar
- Smack DP, Norton SA, Fitzpatrick JE. Proposal for a Pathogenesis-Based Classification of Tumoral Calcinosis. International Journal of Dermatology. 1996;35(4):265-71. PubMed | Google Scholar
- Mozaffarian G, Lafferty F, Pearson O. Treatment of tumoral calcinosis with phosphorus deprivation. Annals of Internal Medicine. 1972 Nov;77(5):741-5. PubMed | Google Scholar
- Yamaguchi T, Sugimoto T, Imai Y, Fujita T, Chihara K. Successful Treatment of hyperphosphatemic tumoral calcinosis with long-term acetazolamide. Bone. 11995 Apr;16(4 Suppl):247S-250S. PubMed | Google Scholar
- Malberti F, Surian M, Poggio F, Minoia C, Salvadeo A. Efficacy and safety of long-term treatment with calcium carbonate as a phosphate binder. American Journal of Kidney Diseases. 1988 Dec;12(6):487-91. PubMed | Google Scholar
- Mendelson BC, Linscheid RL, Dobyns JH, Muller SA. Surgical treatment of calcinosis cutis in the upper extremity. J Hand Surg Am. 1977 Jul;2(4):318-24. PubMed | Google Scholar