Symptomatic prostatic utricle cyst: a case report
Ait Ouali Rachid, Aarab Mouaad, Mortaji Adnane, Lakmichi Mohamed Amine, Dahami Zakaria, Moudouni Mohamed Said, Sarf Ismail
Corresponding author: Ait Ouali Rachid, Department of Urology, Kidney Transplantation and Mini Invasive Surgery, CHU Mohammed VI, Marrakesh, Morocco 
Received: 04 Dec 2021 - Accepted: 21 Jan 2022 - Published: 26 Jan 2022
Domain: Urology
Keywords: Cyst, prostatic utricle, adolescent, external genitalia, case report
©Ait Ouali Rachid et al. PAMJ Clinical Medicine (ISSN: 2707-2797). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Ait Ouali Rachid et al. Symptomatic prostatic utricle cyst: a case report. PAMJ Clinical Medicine. 2022;8:18. [doi: 10.11604/pamj-cm.2022.8.18.32689]
Available online at: https://www.clinical-medicine.panafrican-med-journal.com//content/article/8/18/full
Symptomatic prostatic utricle cyst: a case report
![]() Ait Ouali Rachid1,&,
Ait Ouali Rachid1,&, ![]() Aarab Mouaad1, Mortaji Adnane1, Lakmichi Mohamed Amine1, Dahami Zakaria1, Moudouni Mohamed Said1, Sarf Ismail1
Aarab Mouaad1, Mortaji Adnane1, Lakmichi Mohamed Amine1, Dahami Zakaria1, Moudouni Mohamed Said1, Sarf Ismail1
&Corresponding author
The prostatic utricle is a remnant of the Müllerian ducts and can be the site of a cyst that is usually asymptomatic and most often associated with hypospadias or other external genitalia anomalies. We report a rare case of a symptomatic prostatic utricle cyst revealed by lower urinary tract signs evolving since 3 months in a 19-year-old adolescent with cerebral palsy, without external genital anomalies. The diagnosis was confirmed by pelvic MRI, and the treatment consisted of transrectal ultrasound-guided aspiration with good clinical evolution.
Prostatic utricle cyst is a rare cystic lesion of the prostatic midline, most often it is associated with urogenital tract abnormalities, it may be diagnosed incidentally during an imaging workup, or revealed by lower urinary tract symptoms, pelvic pain infertility or hemo-spermia. We report a rare case of a large cyst of the prostatic utricle without hypospadias or external genitalia abnormalities drained by transrectal echo-guided evacuation. The purpose of this case is due to its rarity due and to its symptomatic nature and absence of external genitalia abnormalities.
Patient information: the case we report is a 19-year old male patient, how suffer from spastic cerebral palsy due to neonatal suffering at term, who consulted for spontaneous pelvic pain associated with dysuria and mictional burning evolving since 3 months, without any other clinical signs for instead haematuria, haemospermia, fever or perineal pain.
Clinical findings: on physical examination we noted external genitalia without abnormalities with a urethral meatus in apical position, both testicles were in a normal position intrascrotally. The digital rectal examination revealed a median, firm, evenly contoured prostatic mass that was slightly painful.
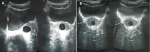
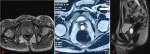
Diagnosis approach: a biological check-up was carried out which came back without any particularities, it included a cytobacteriological examination of the urine, a renal function, and hydatid serology given the endemic context of hydatid cyst in our country. The patient underwent a reno-vesico-prostatic ultrasound (Figure 1) which revealed a thin-walled, anechogenic cystic lesion with posterior enhancement measuring 2.1 x 1.4 cm. The ultrasound was complemented by a pelvic MRI (Figure 2) which revealed a normal-sized prostate with a median cystic lesion, measuring 2.3 x 1.6 cm, thin-walled, with fluid content in T1 hyposignal, T2 hypersignal, without restriction diffusion, in contact with the rectal wall and the prostatic urethra without communicating pertussis, the vesicles seminales were normal suggesting a dysembryoplastic cyst of the utricle.
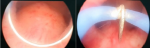
Therapeutic interventions: the medical care consisted initially of exploratory urethrocystoscopy (Figure 3), which revealed a slight swelling of the urethra protruding into the urethral lumen, then in a second phase the cyst was located by endorectal ultrasound (Figure 4) which showed that the location of the cyst was closer to the rectal wall than to the prostatic urethra, which is why we opted for a transrectal ultrasound-guided evacuation puncture, with collection of the liquid for biochemical and cytological study and search for spermatozoon.
Follow-up and outcome of interventions: the post-surgery period was marked by the disappearance of pain, discharge from the hospital at D1, and no cyst was detected at the control ultrasound.
Patient consent: written informed consent was obtained from the patients' mother for publication for this case report.
The prostatic utricle is a vestigial cavity, opening at the top of the verumontanum, located between the termination of the two ejaculatory ducts, at the posterior border of the prostatic urethra. It becomes pathological when it is dilated. This dilatation is most often congenital, and is referred to as congenital hypertrophy of the prostatic utricle (enlarged prostatic utricle). It derives from an anomaly in the involution of the caudal end of the Müllerian apparatus, due to a deficiency in the anti-Müllerian hormone [1].
The incidence of prostatic utricle cysts is rare, around 1% in neonates, 4% in adults [2], and 11-14% in association with penile hypospadias, penoscrotal hypospadias, cryptorchidism or with patient with congenital anomalies of urogenital development, and up to 50% in association with perineal hypospadias [3]. While it is 10 to 25% in association with renal agenesis or dysgenesis [4]. The cyst of the utricle can be revealed by signs of the lower urinary tract, obstructive or irritative, pelvic pain such as in our patient, haemospermia, epididymitis, urethral discharge, infertility or asymptomatic discovery, particularly if it is small. Urinary tract infections, sometimes recurrent, or stone formation. Malignant degeneration has been reported in 3% of prostatic utricle cysts, with a peak incidence in the 4th decade of life [5]. Sometimes a well-bounded cystic mass is palpable on rectal examination.
After suspicion of the diagnosis based on clinical elements, transrectal, retropubic or perineal ultrasonography is the paraclinical examination are the first choice. It allows to objective a pelvic mass of cystic appearance, intraprostatic and median, well delimited in relation to the neighbouring organs such as the prostate and the urethra [6], small cysts may be undetectable by ultrasonography.
Although ultrasonography is the first-line examination, MRI allows multiplanar acquisition for a better precision of the dimensions of the cyst, to localize it in\to the adjacent structures, in particular the rectum, bladder, and seminal vesicles, as well as its communication or not with the prostatic urethra, and shows a median, thin-walled cystic mass with T2-weighted hypersignal and T1-weighted hyposignal [7]. In case of an intracystic hemorrhagic component, the cyst appears in T1 and T2 hypersignal. Urethroscopy, performed in the first phase in case of endoscopic resection of the cyst, allows visualization the orifice of the utricle at the top of the verumontanum. Retrograde urethrography: allows to differentiate a cyst of the prostatic utricle from other prostatic and periprostatic cysts by specifying its location and communication with the prostatic urethra. This examination is not routinely recommended because of the presence of other simple, non-invasive, painless examinations, and the impossibility of filling the utricle with contrast fluid if the cyst is not communicating or the utricular opening is so narrow and slit-like [8].
The differential diagnosis must always be considered, in particular a seminal vesicle cyst, urethral cyst, bladder diverticulum and most importantly Müllerian duct cysts. These cysts of the Müllerian duct are the most difficult to distinguish from the cyst of the utricle from the embryological, clinical and radiological point of view, because both are median intra-prostatic cysts with absence of sperm cells in their content. Some authors suggest that the Müllerian duct cyst originates from the mesoderm, while the prostatic utricle cysts originate from the endoderm [5]. Müllerian duct cysts are usually not communicating with the prostatic urethra. They are round in form and are frequently encountered in adults (20-40 years) with normal external genitalia. While prostatic utricle cysts are tubular or vesicular in shape and are most commonly observed in pediatric and adolescent patients (<20 years of age) with hypospadias, cryptorchidism and sexual dysplasia are usually in communication with the prostatic urethra [9].
Surgical management of a prostatic utricle cyst is not systematic; only patients who are symptomatic should be treated, as small cysts can be simply monitored. There are several therapeutic methods available, ranging from transperineal or transrectal puncture-aspiration to conventional surgery, and these different methods can be used in a combined manner.
While there are multiple techniques, they have not been well codified. Endoscopic dilatation of the orifice of the utricle, followed by catheterization and aspiration of its contents with or without sclerotherapy, and transurethral resection of the anterior wall of the cyst are two less invasive techniques; they make it possible to avoid the complications of surgery, especially infertility and impotency, but they present a high risk of recurrence [10]. Transurethral resection of the prostatic utricle cyst can be performed using the Holmium laser with reliable and effective results [11].
Robot-assisted or unassisted laparoscopic excision of the cyst is possible but requires an experienced operator, it reduces the risk of damaging the retrobladder space and the surrounding tissues, it also allows better visibility and decreases the time needed for recovery. The classic method proposes several approaches; the transvesical or transtrigonal abdominal method allows a very good exposure of the prostatic region and an easier surgical procedure, reducing the risk of damage to the ureters and ducts of inference as well as the risk of postoperative incontinence [12]. The extra bladder abdominal approach is technically difficult with a risk of altering the surrounding structures, and transperineal excision is also less used.
The cyst of the prostatic utricle in adolescents that is not associated with an abnormality of the external genitalia, cryptorchidism or renal agenesis constitutes an entity rarely reported in the literature. Most often it is revealed by urogenital signs, ultrasound guidance and pelvic MRI confirm the diagnosis. The treatment should be as conservative as possible and less invasive.
The authors declare no competing interests.
All authors were involved in the management of the patient. RA wrote the first version of the clinical case and ZD approved the final version. All the authors have read and agreed to the final manuscript.
Figure 1: suprapubic ultrasound: A) sagittal; B) transverse sections showing a medioprostatic cystic lesion
Figure 2: pelvic magnetic resonance imaging (MRI) of the patient: A,B) with axial; and C) sagittal sections showing a median prostatic cyst, without obvious communication with the prostatic urethra measuring 2.3 cm in long axis, in hyposignal T1 (yellow arrow) and hypersignal T2 (red arrows)
Figure 3: endoscopic appearance of the prostatic utricle
Figure 4: A) transrectal ultrasound location of the prostatic cyst; B) aspiration puncture
- Gevenois PA, Van Sinoy ML, Sintzoff Jr SA, Stallenberg B, Salmon I, Van Regemorter G. Cysts of the prostate and seminal vesicles MR imaging findings in 11 cases. AJR Am J Roentgenol. 1990 Nov;155(5):1021-4. PubMed | Google Scholar
- Desautel MG, Stock J, Hanna MK. Mullerian duct remnants: surgical management and fertility issues. J Urol. 1999 Sep;162(3 Pt 2):1008-13; discussion 1014 PubMed | Google Scholar
- Coppens L, Bonnet P, Andrianne R, DE Leval J. Adult Mullerian duct or utricle cyst: clinical significance and therapeutic management of 65 cases. J Urol. 2002 Apr;167(4):1740-4. PubMed | Google Scholar
- Momin YA, Dhende NP, Ghodke BA, Ansari SA, D'Costa GF, Mahajan VR. An abnormally large prostatic utricle cyst associated with unilateral renal agenesis. Urol Ann. 2013 Apr;5(2):129-31. PubMed | Google Scholar
- Schuhrke TD, Kaplan GW. Prostatic utricle cysts (Müllerian duct cysts). J Urol. 1978;119(6):765-767. PubMed | Google Scholar
- Hester AG, Kogan SJ. The prostatic utricle: an under-recognized condition resulting in significant morbidity in boys with both hypospadias and normal external genitalia. J Pediatr Urol. 2017;13(5):492.e1-492.e5. PubMed | Google Scholar
- Mayersak JS. Urogenital sinus-ejaculatory duct cyst: a case report with a proposed clinical classification and review of the literature. J Urol. 1989;142(5):1330-1332. PubMed | Google Scholar
- Kojima Y, Hayashi Y, Maruyama T, Sasaki S, Kohri K. Comparison between ultrasonography and retrograde urethrography for detection of prostatic utricle associated with hypospadias. Urology. 2001;57(6):1151-1155. PubMed | Google Scholar
- Lazarus J, Maison POM, Howlett J. Prostatic utricle cyst presenting with recurrent urethral discharge in the newborn: a case report. Pediatric Urology Case Reports. 2017;4(6):383-6. Google Scholar
- Luo JH, Chen W, Sun JJ, Xie D, Mo JC, Zhou L, Lu J. Laparoscopic management of Müllerian duct remnants: four case reports and review of the literature. J Androl. 2008;29(6):638-42. PubMed | Google Scholar
- Sávio LF, Carrasquillo RJ, Dubin JM, Shah H, Ramasamy R. Transurethral ablation of a prostatic utricle cyst with the use of a holmium laser. Fertil Steril. 2018;110(7):1410-1411. PubMed | Google Scholar
- Fontaine E, Jardin A. Anomalies des organes génitaux internes masculins et retentissement sur la fertilité. Prog Urol. 2001; 11:729-732.