Prevalence of venous thromboembolism in patients hospitalized for tuberculosis at Yaoundé Jamot Hospital (Cameroon), 2010-2019: a cross-sectional study
Abdou Wouoliyou Nsounfon, Massongo Massongo, Alain Kuaban, Virginie Poka-Mayap, Marie Christine Ekongolo, Christelle Engananigne, Christian Belmond Takongue Djoum, Gabriel Arsène Zeh Mabiom, Gaëlle Tatiana Djapni Makougang, Eric Walter Pefura-Yone
Corresponding author: Abdou Wouoliyou Nsounfon, Department of Internal Medicine and Specialties, Faculty of Medicine and Biomedical Sciences, the University of Yaounde I, Yaounde, Cameroon 
Received: 09 Mar 2022 - Accepted: 11 Mar 2022 - Published: 11 Mar 2022
Domain: Infectious disease,Pulmonology
Keywords: Tuberculosis, pulmonary embolism, deep vein thrombosis, Cameroon
©Abdou Wouoliyou Nsounfon et al. PAMJ Clinical Medicine (ISSN: 2707-2797). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Abdou Wouoliyou Nsounfon et al. Prevalence of venous thromboembolism in patients hospitalized for tuberculosis at Yaoundé Jamot Hospital (Cameroon), 2010-2019: a cross-sectional study. PAMJ Clinical Medicine. 2022;8:38. [doi: 10.11604/pamj-cm.2022.8.38.34174]
Available online at: https://www.clinical-medicine.panafrican-med-journal.com//content/article/8/38/full
Research 
Prevalence of venous thromboembolism in patients hospitalized for tuberculosis at Yaoundé Jamot Hospital (Cameroon), 2010-2019: a cross-sectional study
Prevalence of venous thromboembolism in patients hospitalized for tuberculosis at Yaoundé Jamot Hospital (Cameroon), 2010-2019: a cross-sectional study
![]() Abdou Wouoliyou Nsounfon1,&,
Abdou Wouoliyou Nsounfon1,&, ![]() Massongo Massongo1,
Massongo Massongo1, ![]() Alain Kuaban1, Virginie Poka-Mayap1,2, Marie Christine Ekongolo1, Christelle Engananigne1, Christian Belmond Takongue Djoum1, Gabriel Arsène Zeh Mabiom1, Gaëlle Tatiana Djapni Makougang1, Eric Walter Pefura-Yone1,2
Alain Kuaban1, Virginie Poka-Mayap1,2, Marie Christine Ekongolo1, Christelle Engananigne1, Christian Belmond Takongue Djoum1, Gabriel Arsène Zeh Mabiom1, Gaëlle Tatiana Djapni Makougang1, Eric Walter Pefura-Yone1,2
&Corresponding author
Introduction: venous thromboembolic disease (VTE) can occur during tuberculosis (TB) through the hypercoagulability the latter generates. The association of these two diseases is poorly described in our setting. The objective of this study was to determine the prevalence of VTE in patients diagnosed with tuberculosis and describe the patients as well as the features of the diseases.
Methods: we conducted a retrospective study at the Yaounde Jamot Hospital. The records of all patients hospitalized for TB with VTE between January 2010 and May 2019 were included in the study. Clinical and paraclinical data were collected.
Results: of the 100% (n = 3872) patients hospitalized for TB, 31 had VTE, giving a prevalence (95% confidence interval) of 0.8% (0.5% - 1.1%). Of the 100% (n = 31) patients hospitalized for TB with VTE, 58.1% (n = 18) were males and the median [interquartile range (IQR)] age was 40 (33 - 56) years. Isolated deep vein thrombosis (DVT) was found in 77.4% (n = 24) of the patients, and 16.1% (n = 5) had isolated pulmonary embolism. HIV infection was found in 61.2% (n = 19) of the patients. Pulmonary location was the main site of the TB disease, comprising 48.4% (n =15) of the cases. Among the other known risk factors for VTE, immobility and history of VTE were respectively found in 51.6% (n = 16) and 12.9% (n = 4) of the patients.
Conclusion: venous thromboembolic disease is not a common complication of tuberculosis in our setting and occurs more in the form of deep vein thrombosis. Pulmonary location of tuberculosis and HIV infection are frequently found in these patients.
Tuberculosis (TB) remains a public health problem in developing countries, with significant morbidity and mortality [1]. It is associated with the occurrence of many complications, including venous thromboembolic disease (VTE) which is a collective term referring to deep vein thrombosis (DVT) and pulmonary embolism (PE). Venous thromboembolic disease can occur as a result of the chronic inflammatory state, and the hypercoagulability generated by TB [2,3], as well as the potential side effects of some anti-tuberculosis drugs [4]. The occurrence of VTE during TB significantly increases the risk of death, as shown by Dentan et al. in the United States of America [5]. They found an in-hospital mortality of 15% in patients who had both active TB and VTE, compared to 2.7% for isolated TB and 2.5% for isolated VTE [5]. The occurrence of VTE during TB probably remains under-diagnosed in our context because it is not actively searched for in routine clinical practice [6]. Indeed, Moran´s autopsy series in Virginia diagnosed pulmonary embolism in 24.3% of subjects who died from active TB [7], while VTE was only found in 1.5% - 3.4% of patients with TB [4,5]. Little is known on the association of these two diseases in an African setting [8]. This study aimed to determine the prevalence of VTE in patients with TB and describe their clinical, biological and radiologic characteristics in a tertiary health care facility in Cameroon.
Study design and setting: this retrospective descriptive study was carried out in a chest service at the Yaounde Jamot Hospital (YJH) from January 2010 to May 2019. Yaounde Jamot Hospital is the national referral centre for TB and respiratory diseases, located in Yaoundé, the capital city of Cameroon. In this hospital patients suspected to have DVT and pulmonary embolism by using clinical probability scores are asked to do a venous Doppler ultrasound and angiographic computed tomography (CT) scan to confirm the diagnosis.
Study population: all patients hospitalised for TB and who were diagnosed with VTE were included in the study. Patients who were hospitalized with a diagnosis other than TB were excluded. Those hospitalized with TB and in whom VTE was suspected but not confirmed were also excluded.
Data collection: the TB and hospitalisation registers were first consulted to identify patients who had been hospitalised during the study period. The files of these patients were then obtained from the archives in the various blocks of the service and analysed to identify those who had a confirmed diagnosis of deep vein thrombosis (DVT) and/or pulmonary embolism (PE) documented in the files. Data were retrieved from the medical files of these patients on the following: sex (male/female), age (in years), weight (in kilograms), height (in meters) and body mass index (BMI) calculated as the ratio:
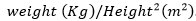
Obesity was defined by a BMI ≥ 30 kg/m2. Data were also retrieved on the delay (in weeks) between the onset of symptoms and diagnosis of TB, patient´s immobility, Human Immunodeficiency Virus (HIV) status, CD4 cell count (cells/mm3), full blood count and the radiologic (chest X-ray, venous doppler ultrasonography and angiographic chest CT scan) findings. The lung was divided into six zones for characterisation of the location and degree of lung involvement [9].
Statistical analysis: the data were processed and analysed using CSPRO 6.3 (United States Census Bureau, Washington, USA) and IBM SPSS Statistics 23.0 (IBM Corp., Armonk, New York, USA) software. Qualitative variables were summarised by using frequencies (percentage). Continuous quantitative variables were summarised by using the median and interquartile range.
Ethical considerations: administrative authorization to carry out the study was obtained from the authorities of the Yaoundé Jamot Hospital.
Study population and prevalence of VTE: of the 3872 patients hospitalized for TB during the study period, 31 had a proven VTE. Thus, the prevalence (95% confidence interval) of VTE was 0.8% (0.5% - 1.1%).
General characteristics of the study population: of the 100% (n = 31) patients hospitalized for TB with VTE, 58.1% (n = 18) were male and the median [interquartile range (IQR)] age was 40 (33 - 56) years. The median (IQR) body mass index (BMI) was 20.7 (18.6 - 24.3) kg/m2. HIV infection was found in 61.2% (n = 19) of patients, and their median (IQR) CD4 count was 222.5 (113 -342)/mm3. The median (IQR) haemoglobin, leukocyte, and platelet levels were respectively 9.8 (8.3 - 11.9) g/dL, 6.8 (3.9 - 8.7) x 109/L and 250 (144-351.5>) x 109/L (Table 1).
Clinical and morphological characteristics of tuberculosis: pulmonary localization was the main site of TB with 48.4% (n = 15) of cases. The median delay (IQR) for the diagnosis of TB was 5.5 (4 - 14) weeks. On the chest X-ray, infiltrates were the most frequently observed pulmonary lesions with 72.4% (n = 21) of cases, and the median (IQR) number of affected zones was 4 (2 - 6). Lesions and the number of affected lung zones are summarized in Table 2.
Characteristics of venous thromboembolic disease: in trying to describe the factors known to increase the risk of VTE, we identified immobility and a history of VTE, which were respectively found in 51.6 % (n=16) and 12.9% (n = 4) of patients. In 54.8% (n = 17) of the patients, the diagnosis of VTE was made after they had started anti-TB treatment, with a median delay (IQR) of 13 (7 - 38) days. Twenty-four (77.4%) patients had isolated deep vein thrombosis (DVT) and 5 (16.1%) patients had isolated pulmonary embolism. Extensive DVT was found in 45% (n = 9) of cases (Table 3). Deep vein thrombosis was more frequent in patients with pulmonary tuberculosis, as seen in 58.3% (n=14) of cases, while pulmonary embolism was found to occur more in those with both pulmonary and extrapulmonary tuberculosis in 80% (n=4) of cases (Table 4).
Outcome: among the 31 TB patients with VTE, 3 died during hospitalisation, resulting in an in-hospital mortality rate of 9.7% (n=3) (Table 1).
The purpose of this retrospective study was to determine the prevalence of VTE in patients admitted for tuberculosis (TB) and to describe their characteristics. The prevalence of VTE during TB was 0.8% (n=31), presenting as isolated and bilateral DVT in 77.4% (n=24) and 34.6% (n=9) of the cases respectively. The diagnosis of VTE was made more after the initiation of anti-tuberculosis treatment, and the main known risk factor for VTE was immobility. Pulmonary location of TB and HIV infection were frequently found in these patients. The in-hospital mortality rate was 9.7% (n=3). The occurrence of VTE is not uncommon in TB. Indeed, in their study, Dentan et al. [5] found that patients with TB had an increased risk of VTE (OR = 1.55; 95% CI= 1.23 - 1.97; p <0.001) and this is close to the risk observed in patients with neoplastic diseases (OR = 1.62) as observed by Alikhan R et al. in their study [10]. The prevalence of VTE in patients known to have TB varies across studies. The prevalence (0.8%) found in our study is close to the 0.7% found by Shitrit et al. [11]. It is, however, lower than that found in most studies from high-income countries, with a range of 1.5 - 3.4% [4,5]. These differences in prevalence could be explained by the financial constraints patients face in our setting, thereby limiting the realisation of the required imaging investigations needed for diagnosis. The absence of specific symptoms of DVT and pulmonary embolism in patients affected by pulmonary involvement of TB could also limit the active search for VTE by caregivers. Several mechanisms have been proposed to possibly explain the development of VTE in patients with active TB. TB induces inflammatory processes that can affect all elements of the Virchow triad, and these phenomena may in part explain the increased risk of thromboembolic events in patients with TB. Indeed, it has been shown that TB causes a state of hypercoagulability, which could be due to haematological disturbances such as increased plasma fibrinogen and factor VIII, as well as thrombocytosis and increased platelet aggregation [2,3]. In addition, some authors have demonstrated high titres of antiphospholipid antibodies in patients with TB [12]. The return of all these haematological parameters to a normal level during treatment of TB is a good indicator of disease control [12]. Venous stasis can be due to local compression of the veins by enlarged lymph nodes or immobilization, partly linked to severe respiratory impairment. Endothelial lesions can be induced by Mycobacterium tuberculosis itself, but also by rifampicin-based regimens used to treat TB [4]. All these mechanisms make TB to be considered as a disease that significantly increases the risk for the occurrence of VTE.
Venous thromboembolic disease can occur at any time during the course TB [5,13]. In our study, the diagnosis of VTE was made in 54.8% of patients after they had started anti-tuberculosis treatment. This observation is similar to that found in many studies [4,11]. Several hypotheses have been put forward on the occurrence of thromboembolic complications during the treatment of TB, among which the action of rifampicin is strongly incriminated [4]. Studies have demonstrated a possible association between DVT and the use of rifampicin, with a relative risk of occurrence of DVT of 4.74 in these patients [4]. VTE seems to develop frequently during the first month of treatment, especially in patients with prolonged hospitalisation [11]. Twenty-four patients (77%) in our study had isolated deep vein thrombosis and this is consistent with the results of Shitrit et al. in 2012 [11]. Of these, 14 (58.3%) had pulmonary TB, while only 1 (20%) of the 5 patients with isolated pulmonary embolism, had isolated pulmonary TB. These results could suggest that there is no link between the type of VTE and the location of TB in our setting, unlike what was previously found by Dental et al. [5].Thus, all forms of VTE could be associated with all forms of TB, and from this we can hypothesize that the role of systemic hypercoagulability is more important than that of local venous compression in the pathogenesis of VTE in patients with TB. In this study, pulmonary embolism was more frequent in extensive TB (0.0% in extrapulmonary TB, 6.7% in pulmonary TB, and 40% in pulmonary plus extra-pulmonary TB), while the association of DVT plus PE was only found in patients having pulmonary + extrapulmonary TB. This supports the importance of inflammation (thus systemic hypercoagulability) over solely local injuries. The in-hospital mortality rate was 9.7% in our study. This result, even though being lower than what was reported by Dentan et al. [5], still appears quite high. The occurrence of VTE during active TB marks an evolutionary turning point because it increases the risk of death in these patients. Indeed, Dentan et al. in observed that the in-hospital mortality of patients with both active TB and VTE was 15%, and this was significantly higher than that of patients with isolated TB (2.7%) or isolated VTE (2.5%) (P<0.001) [5]. The main limitation of this retrospective study was that of missing data, which is expected to occur in all retrospective study designs. Furthermore, it is very likely that the prevalence of VTE could be underestimated in this setting, due to underdiagnosis. This could be explained by the fact that some patients suspected to have VTE could not do the required investigations to confirm the diagnosis of VTE because of financial constraints and the fact that the Yaoundé Jamot Hospital doesn´t have CT scan. Nevertheless, this study as the first of its kind in our setting provides an overview of VTE during TB locally. More research can be done to have information on the risk factors for VTE that are "specific" to this population. Such information might contribute to better understand the occurrence of VTE in this clinical setting, and potentially help in the prevention of VTE.
VTE is an associated comorbid condition found in patients admitted for TB in our setting and most commonly presents in the form of DVT which is extensive. Pulmonary location of TB and HIV infection are frequently found in these patients. As such patients with active TB should always be screened for VTE, particularly when other thromboembolic risk factors are present. More research is needed to determine the real association between TB and VTE in our setting.
What is known about this topic
- The prevalence of venous thromboembolic disease in patients with tuberculosis in settings other than Cameroon;
- The established risk factors of venous thromboembolic disease in other diseases;
- To the best of our knowledge no evidence exists on the relationship between tuberculosis and venous thromboembolic disease in Cameroon.
What this study adds
- The rates of venous thromboembolic disease in patients admitted with active tuberculosis in a major centre for the management of tuberculosis in Cameroon is not negligible;
- Pulmonary location of tuberculosis and HIV infection are frequently found when venous thromboembolic disease occurs in patients who have tuberculosis.
The authors declare no competing interests.
Conception and study design: AWN, MM, VPM, AK and EWPY. Data collection: AWN, AK, MCE, CE, CBTD, GAZM and GTDM. Data analysis and interpretation: AWN, MM, VPM, AK and EWPY. Manuscript drafting: AWN. Manuscript revision: AWN, MM, VPM, AK and EWPY. Guarantor of the study: EWPY. All the authors have read and agreed to the final manuscript.
Table 1: clinical and biological characteristics of hospitalized patients for tuberculosis who developed a venous thromboembolic disease
Table 2: radiographic presentation of pulmonary involvement of tuberculosis in patients hospitalized for tuberculosis who presented with venous thromboembolic disease
Table 3: characteristics of venous thromboembolic disease in the patients hospitalized for tuberculosis and who presented with venous thromboembolic disease
Table 4: distribution of tuberculosis locations according to venous thromboembolic disease type in the patients hospitalized for tuberculosis and who presented with venous thromboembolic disease
- WHO. Global tuberculosis report: 2016. Genève: Word Health Organization. 2016. Google Scholar
- Turken O, Kunter E, Sezer M, Solmazgul E, Cerrahoglu K, Bozkanat E et al. Hemostatic changes in active pulmonary tuberculosis. Int J Tuberc Lung Dis Off J Int Union Tuberc Lung Dis. 2002;6(10):927-3. PubMed | Google Scholar
- Robson SC, White NW, Aronson I, Woollgar R, Goodman H, Jacobs P. Acute-phase response and the hypercoagulable state in pulmonary tuberculosis. Br J Haematol. 1996;93(4):943-9. PubMed | Google Scholar
- White NW. Venous thrombosis and rifampicin. Lancet Lond Engl. 1989 Aug 19;2(8660):434-5. PubMed | Google Scholar
- Dentan C, Epaulard O, Seynaeve D, Genty C, Bosson JL. Active tuberculosis and venous thromboembolism: association according to international classification of diseases, ninth revision hospital discharge diagnosis codes. Clin Infect Dis Off Publ Infect Dis Soc Am. 2014;58(4):495-501. PubMed | Google Scholar
- Njonnou SRS, Nganou-Ngnindjo CN, Hamadou B, Jemea B, Jingi AM, Boombhi J et al. Epidemiology of venous thrombo-embolic disease in Yaounde: a cross-sectional study in sub-Saharan Africa. World J Cardiovasc Dis, Scientific Research Publishing; 2019;9(5):360-9. Google Scholar
- Moran TJ. Autopsy incidence of pulmonary embolism in tuberculosis. Dis Chest. 1950;18(2):171-3. PubMed | Google Scholar
- Ekukwe NC, Bain LE, Jingi AM, Sylvia K, Mintom P, Menanga A. Bilateral pulmonary embolism in a patient with pulmonary tuberculosis: a rare association in Yaoundé, Cameroon. Pan Afr Med J. 2014;17(262). PubMed | Google Scholar
- Chuchottaworn C, Thanachartwet V, Sangsayunh P, Than TZM, Sahassananda D, Surabotsophon M et al. Risk factors for multidrug-resistant tuberculosis among patients with pulmonary tuberculosis at the central chest Institute of Thailand. PLOS ONE. Public Library of Science; 2015;10(10):e0139986. PubMed | Google Scholar
- Alikhan R, Cohen AT, Combe S, Samama MM, Desjardins L, Eldor A et al. Risk factors for venous thromboembolism in hospitalized patients with acute medical illness: analysis of the MEDENOX Study. Arch Intern Med. 2004;164(9):963-8. PubMed | Google Scholar
- Shitrit D, Fox L, Preiss R, Raz M, Mtvitzuk A. Incidence of venous thromboembolism in 700 patients with acute tuberculosis. Harefuah. 2012;151(4):208-10, 254. PubMed | Google Scholar
- Suárez Ortega S, Artiles Vizcaíno J, Balda Aguirre I, Melado Sánchez P, Arkuch Saade ME, Ayala Galán E et al. Tuberculosis as risk factor for venous thrombosis. An Med Interna Madr Spain 1984. 1993;10(8):398-400. PubMed | Google Scholar
- Gupta A, Mrigpuri P, Faye A, Bandyopadhyay D, Singla R. Pulmonary tuberculosis - an emerging risk factor for venous thromboembolism: a case series and review of literature. Lung India Off Organ Indian Chest Soc. 2017;34(1):65-9. PubMed | Google Scholar




