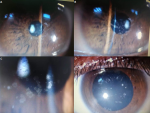
Schnyder corneal dystrophy
Kamelia Rifai, Lalla Ouafa Cherkaoui
Corresponding author: Kamelia Rifai, Department A of Ophthalmology, Mohammed V University Souissi, Rabat, Morocco 
Received: 26 Jan 2022 - Accepted: 11 Mar 2022 - Published: 14 Mar 2022
Domain: Ophthalmology
Keywords: Anterior stroma, cornea, dyslipidemia, schnyder dystrophy
©Kamelia Rifai et al. PAMJ Clinical Medicine (ISSN: 2707-2797). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Kamelia Rifai et al. Schnyder corneal dystrophy. PAMJ Clinical Medicine. 2022;8:39. [doi: 10.11604/pamj-cm.2022.8.39.33488]
Available online at: https://www.clinical-medicine.panafrican-med-journal.com//content/article/8/39/full
Schnyder corneal dystrophy
&Corresponding author
We present the case of a 45-year-old African male patient, who presented to the ophthalmic consultation for decreased bilateral visual acuity and complaints of blurred vision for 5 years. The ophthalmological examination included a measure of visual acuity using Snellen´s distance vision chart. We did a complete and bilateral biomicroscopic examination of the anterior and the posterior segments. The clinical examination found a reduced visual acuity to counting fingers in the right eye and 2/10 in the left eye. Intraocular pressure was normal in both eyes. Slit lamp examination revealed corneal arcus or a disk-like lesion and polychromatic crystalline depositions in both eyes in the subepithelial and the anterior 1/3 of the stroma. The mild onset of arcus lipoides was seen, but the Midperipheral stromal haze was absent. Central corneal thickness results were 513 μm in the right eye and 509 μm in the left eye. A diagnosis of Schnyder corneal dystrophy was based on clinical presentation and the coexistence of dyslipidemia of the patient. Schnyder corneal dystrophy (SCD) is a rare, autosomal dominant, anterior stromal dystrophy described as progressive bilateral corneal opacification due to abnormal accumulation of cholesterol and phospholipids in the cornea. Schnyder corneal dystrophy with different presentations may actually be misdiagnosed. Early diagnosis would help to rule out other potentially sight threatening or treatable conditions like infectious keratitis or drug toxicity. Schnyder corneal dystrophy should be discerned from other lipid keratopathies. Ophthalmologists should keep SCD in mind and its associated systemic findings that need to be estimated and managed duly.
Figure 1: fundus image of the left eye revealing a large papillary excavation partially occupied by glial tissue, partially masking the retinal vessels which spread radially over its entire circumference. Some are uninhabited suggesting a congenital malformation of the head optic nerve