Intracranial cavernomas management and outcomes: cross-sectional study from 20 years of experience at Speciality Hospital, Rabat, Morocco
Mahjouba Boutarbouch, Nourou Dine Adeniran Bankole, Yasser Arkha, Adyl Melhaoui, Abdesamad El Ouahabi, Abdeslam El Khamlichi
Corresponding author: Nourou Dine Adeniran Bankole, Department of Neurosurgery, Speciality Hospital, Mohamed V University of Rabat, Rabat, Morocco 
Received: 06 Apr 2020 - Accepted: 06 Jun 2022 - Published: 08 Jun 2022
Domain: Neurosurgery, Vascular surgery
Keywords: Intracranial cavernomas, epilepsy secondary, intracranial hemorrhage
©Mahjouba Boutarbouch et al. PAMJ Clinical Medicine (ISSN: 2707-2797). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Mahjouba Boutarbouch et al. Intracranial cavernomas management and outcomes: cross-sectional study from 20 years of experience at Speciality Hospital, Rabat, Morocco. PAMJ Clinical Medicine. 2022;9:10. [doi: 10.11604/pamj-cm.2022.9.10.22686]
Available online at: https://www.clinical-medicine.panafrican-med-journal.com//content/article/9/10/full
Research 
Intracranial cavernomas management and outcomes: cross-sectional study from 20 years of experience at Speciality Hospital, Rabat, Morocco
Intracranial cavernomas management and outcomes: cross-sectional study from 20 years of experience at Speciality Hospital, Rabat, Morocco
Mahjouba Boutarbouch1,2, ![]() Nourou Dine Adeniran Bankole1,2,&, Yasser Arkha1,2, Adyl Melhaoui1,2, Abdesamad El Ouahabi1,2, Abdeslam El Khamlichi1,2
Nourou Dine Adeniran Bankole1,2,&, Yasser Arkha1,2, Adyl Melhaoui1,2, Abdesamad El Ouahabi1,2, Abdeslam El Khamlichi1,2
&Corresponding author
Introduction: cavernomas are benign vascular anomalies consisting of cavities where the blood circulates at low flow and low pressure. This paper aims to evaluate the management and outcomes of intracranial cavernoma.
Methods: this is a retrospective study, of patients managed from January 2000 to December 2020 for intracranial cavernoma in our department. The patients´ baseline demographic and cavernoma characteristics, as well as the management type and follow-up imaging, were recorded retrospectively.
Results: fifty-six intracranial cavernomas patients were managed during the study period, 11 were excluded (19.6%) because they have missing data. Forty-five patients (80.4%) were included in this analysis. Patients were 31 years old (median) (IQR: 03-64) at diagnosis, and 58% (n=26) were males. The delay between the onset of symptoms and the first consultation was 20 months (median) (IQR: 1 day-10 years). Epilepsy was the most common presenting clinical manifestation (47%; n=21) followed by a neurological deficit (27%; n=12) and intracranial hemorrhage (20%; n=9). Headache was less observed (6.6%; n=3). Sixty-four point four percent (64.4% (n=29) were operated on, and 6.6% (n=3) were treated with a radiosurgery Gamma Knife. Conservative attitude with clinical and neuroradiological monitoring was retained in 28.8% (n=13). The median follow-up in our series was 10 years (IQR: 3-18). The evolution was favorable in 82.7% (n=24) of 29 cases operated on patients including seizures free in 84.6% (n=11) of 13 seizures cases without drugs. The thirteen (13) patients that were managed conservatively had a favorable outcome in 85.7% (n=6) of 7 epilepsy cases with dual therapy control; recovering of the neurological deficit in 40% (n=2/5) of cases with a neurological deficit, the persistence of neurological deficit in 2 cases (40%), and 1 death (7.6%) for cavernomas revealed by intracranial hemorrhage. Globally the mRS was <2 in 38 patients (84.4%), was >2 in 6 cases (13.3%) and the mRS was 6 in one case (2.2%).
Conclusion: our study provides a multimodal treatment possibility that helps overcome the challenges in intracranial cavernomas management.
Cavernomas are benign vascular anomalies consisting of cavities where blood flows at low flow and low pressure. The diagnosis is possible at all ages in both sexes and is frequently seen in young adults [1,2]. The knowledge of this pathology is quite recent. They made a big difference in the mid-1980s with advances in magnetic resonance brain imaging that allowed for the non-invasive diagnosis of cavernomas. However, their mechanism of appearance remained misunderstood [3]. Virchow described the first case of cavernoma in 1863. The current nomenclature is based on descriptions made by Russell and Rubinstein as well as McCormick. Cavernomas are observed either outside of any familial context (sporadic forms) or as part of an autosomal dominant disease with variable penetrance (familial form) [4,5]. Classically they are revealed by clinical manifestations such as epilepsy, neurological deficit, intracranial hemorrhage, and headache. MRI provides a positive diagnosis of cavernoma. Surgery is the treatment of choice for symptomatic cavernomas and consists of total excision of the lesion [4,5]. The neurosurgeon must however determine the modalities of adequate therapeutic management of intracranial cavernomas according to their clinical manifestations, their location, their sizes, their numbers, and the age of the patient. We aimed to evaluate the management and outcomes of intracranial cavernoma after 20 years of experience at our institution.
Study design and setting: a retrospective single institutional review of patient data was done at a Neurosurgery Department of Neurosurgery, Speciality Hospital, Rabat, Morocco between 2000 and 2020.
Study population: between January 2000 and December 2020, patients diagnosed, managed, and followed up for intracranial cavernoma with clinical and imaging follow-up were screened for inclusion. Included patients were managed surgically or conservatively or with radiosurgery, and clinical imaging follow-up >2 years. Patients without intracranial cavernomas and intracranial cavernoma patients lost to follow-up, or with missing data were excluded.
Data collection: sociodemographic data (i.e, age, gender), date of diagnosis, clinical data (presenting signs and symptoms), radiological data (location of intracranial cavernoma, presence of hematoma), treatment modality, outcomes, and clinical and imaging follow-up were extracted retrospectively from the health information system. The outcome was to evaluate the management of intracranial cavernoma and the outcomes in our institution regarding the type of localization and the discovery mode after 20 years of practice.
Operational definition of terms: intracranial cavernoma characteristics were recorded from pre-and post-treatment CT-scan and MRI imaging. Intracranial cavernomas were presented on CT-scan as spontaneous hyperdensity with hypodensity surrounded by the hyperdensity. A typical aspect of MRI cavernoma semiology was a heterogeneous central zone (association of hyper and hypo signals called pepper and salt) surrounded by a halo of hypo signals with a hyper signal in T1 and T2. The lesional center had a homogeneous hyper signal on the T1 and T2 weighted sequences. Antiepileptic treatment was established in patients with seizures of any type. Corticosteroids had a place to fight against perilesional edema. The analgesics were used in stages either alone or in combination with NSAIDs in case of pain. Anticoagulant prophylaxis was systematically instituted in our patients who had a neurological deficit. Lesionectomy surgery was indicated in symptomatic patients (hemorrhagic or non-hemorrhagic) who have supra-tentorial cavernomas that are surgically cortico-subcortical and usually bulky with a mass effect or accompanied by a hematoma that facilitates their access. For infra-tentorial cavernomas, the surgical indication is encouraged in cavernomas that are flush with the surface, making them easy to access after visualization of the tractography or bulky having bled. Joint meeting staff between the neurosurgery department and radiosurgery Gamma Knife was performed case by case to retain conservative management or radiosurgery Gama knife treatment, these patients were being treated at the National Center for Rehabilitation and Neurosciences in Morocco - Gamma Knife Perfexion Radiosurgery Unit - after having been hospitalized in our department. In the case of hydrocephalus, a ventriculoperitoneal VP-shunt was performed in an emergency.
Statistical analysis: we recorded the data in Excel spreadsheets (Microsoft, WA, USA) and analyzed them in SPSS v. 26 (IBM, NY, USA). Gender, mode of discovery (i.e., symptomatic as headache, epilepsy, hemorrhagic, neurological disorders), and type of treatment (conservative management, medical treatment, surgical, radiosurgery) were coded as categorical variables whereas age, the follow-up time, were coded as continuous variables. The distribution of categorical variables was described with frequencies and percentages, whereas continuous variables were described as means and standard deviation (SD) or median (IQR) as per their distribution.
Ethical considerations: ethics approval and consent to participate: only projects, questions of a general nature or relating to a trial, experiment, or biomedical study relating to human beings are examined. Ethics Committee for Biomedical Research of Mohammed V University, Rabat, Morocco. It was not required in this type of study (CERB).
Demographic, clinical, and paraclinical findings: during the study period, 56 intracranial cavernomas patients were managed during the study period, 11 were excluded (19.6%) because they have missing data. Forty-five patients (80.4%) were included in this analysis. They had 31 years old (median) (IQR: 03- 64) at diagnosis, and 58% were males. Intracranial cavernomas were common in the age group between 20-40 years (58%, n=26) in our series. The delays between the onset of symptoms and the first consultation were 20 months (median) (IQR: 1 day-10 years). Epilepsy was the most common presenting clinical manifestation (47%; n=21) followed by a neurological deficit (27%; n=12) and intracranial hemorrhage (20%; n=9). Headache was less observed (6.6%; n=3) (Table 1). Intracavernomatous calcification was observed in 37.7% (n=17). In our series, the diagnosis was strongly suggested in all patients using MRI, the median long size in the axial plane of the cavernoma was 28 mm (IQR: 13- 46). Sixty-four (64) cavernomas were located in our 45 patients, they were mostly located in the supratentorial level (62.5%; n=40). They were unique in 72% (n=46) and multiple in 28% (n=18) of cases (Table 1).
Treatment: the antiepileptic drugs used were sodium valproate 25 mg/kg/day, carbamazepine 600 up to 1200 mg/day, and phenobarbital 150 mg/day but they are less and less used because of their side effects. Surgical excision was performed in 64.4% (n=29), 4.4% (n=2) benefited from the evacuation of hematoma without cavernoma resection because they were deep in the brainstem, 2.2% (n=1) benefited from the ventriculoperitoneal shunt for hydrocephalus secondary to brainstem cavernoma with intracranial hemorrhage, and 6.6% (n=3 ) were treated with a radiosurgery Gamma Knife, they were one deep cavernomas case that was not surgically accessible, one multiple cavernomas cases, and one cavernomas of the frail elderly case. The median dose received was 15 gray (IQR: 13-18). Conservative attitude with clinical and neuroradiological monitoring, follow-up was retained in 28.8% (n=13), it was the epileptic form in 7 patients, the form with neurological deficit in 5 patients, and the hemorrhagic form in 1 patient. Two patients among the 13 patients had refused excision surgery despite his indication (Table 2).
Anatomopathology: an anatomopathological study was performed on 26 patients (57.7%) of the cases and confirmed the cavernomatous nature in 21 patients (80.8%) of cases and was in favor of hematoma in 3 patients (11.5%) cases and was inconclusive in 2 patients (7.7%) of cases.
Outcome and follow-up: the evolution was favorable in 82.7% of 29 cases (n=24) operated patients including seizures free in 84.6% (n=11) of 13 seizure cases without drugs. The thirteen (13) patients that were managed conservatively had a favorable outcome in 85.7% (n=6) of 7 epilepsy cases with dual therapy control; recovering of the neurological deficit in 40% (n=2/5) of cases with a neurological deficit, the persistence of neurological deficit in 2 cases (40%), and 1 death (7.6%) for cavernomas revealed by intracranial hemorrhage. Globally, the mRS was <2 in 38 patients (84.4%), was >2 in 6 cases (13.3%) and the mRS was 6 in one case (2.2%).
In this study, we show the multimodal attitude for intracranial cavernoma management, depending on the localization, the unique or multiple types of cavernoma, and the discovery mode. Epilepsy was the most common presenting clinical manifestation (47%) followed by a neurological deficit (27%) and intracranial hemorrhage (20%). Adequate surgical approach for surgical management, conservative management, medical treatment, and radiosurgery were the main attitude in our center, followed by shunts in associated acute hydrocephalus cases. Globally The mRS was <2 in 38 patients (84.4%), was >2 in 6 cases and the mRS was 6 in one patient who died. Usually, the average age found for intracranial cavernomas is between 35 and 40 years [6,7]. The pediatric forms represent 25% of the cases with two peaks of preferences, a peak during the first year of life and a second between 12 and 16 years of age [8]. The average age in our series was 31 years with a predominant age range between 20 to 40 years (58%). The lucky discovery of cavernomas is rare; he could often be recognized before their break by signs related to cortical irritation or neurological deficit signs by compression, in our series epilepsy is the most common clinical manifestation indicative of the presence of intracranial cavernoma and this result is comparable to results after the literature review [9,10]. Thus, the incidental discovery of cavernomas remains rare. Approximately 70% of the cavernomas are supratentorial with predominantly subcortical and development around the Rolando furrow [11], we found 63.5% supratentorial in our series. The temporal lobe is another preferential site of cavernomas. The basal ganglia and the third ventricle are sometimes affected and are associated with hydrocephalus in case of ventricular involvement. At the subtemporal level, the protuberance is most often affected and the cerebellum rarely [11], the localization at the level of the brainstem represents 79% of infratentorial localizations in our series.
Nowadays, the therapeutic management of cavernomas is controversial. However, depending on the location, the surgical treatment remains superior to other therapeutic methods regardless of the number (single, multiple) [11,12]. The surgical indication in the treatment of cavernoma depends on the presentation in single or multiple forms, the localization in the superficial or deep zone, supratentorial or infratentorial, and the fact that it is symptomatic or incidental discovery. Among the 29 patients operated on, there were 26 cases of resection surgery including 25 cases (86.2%) of total excision (Figure 1, Figure 2) and one case of partial resection of a large temporal cavernoma in our series. Supratentorial lobar cavernomas that do not involve basal ganglia, ventricles, or calyces account for 86% of all locations. They can be located in the superficial zone, cortico-cortical, or in the radiata corona up to 5 cm deep [13]. Cavernomas located near language areas, rolandic and visual areas will pose particular problems of indication and surgical technique. Functional MRI distinguishes whether the cavernoma is located within or adjacent to the eloquent area, whether neuroplasticity has changed the usual anatomy-functional correlations, and whether the so-called non-eloquent areas are actually [14]. A good analysis of the images will make it possible to perform a surgical approach, and surgical excision is facilitated even if the lesion is located in an eloquent zone. In the case of a location at the bottom of a groove, the latter able to be expended by cortical atrophy in the neighborhood, which will lead to recommending a transulcal approach when it is possible [15].
The three main deep locations are the thalamus, the head of the nucleus caudate, and the lenticular nucleus. The localization at the level of the internal capsule and insula is considered deep localization [16]. Cavernomas of the head of the caudate nucleus able to be approached by interhemispheric and trans-callous, according to the technique described by the team Spetzler, the resection of the cavernoma by microsurgical technique is, in the majority of cases, achievable after a simple break-up of the ependyma without significant parenchymal opening [17]. Cavernomas of insular localization, when they are symptomatic or large volume, particularly in young subjects, seem could be operated on with low morbidity [18]. Brainstem Cavernomas benefited from advances in imaging; techniques microsurgical, neuronavigation and treatment experiences nowadays. The pons is the most frequent location (50 to 55%) followed by the mesencephalic or thalamo-peduncular region (approximately 35%) whereas bulbar sites are rarer (about 15%) [19]. A history of familial cavernomatosis was been found in almost 14% of patients with cavernoma of the brainstem [20]. In the evaluation of surgical risk, careful analysis of imaging is essential. In the evaluation of surgical risk, careful analysis of imaging is essential. Indeed, progress in the knowledge of anatomy compared to the fundamental anatomy and the use of the neuronavigation are key factors contributing to the improvement results of the surgical treatment [20]. In our series, we did not use neuronavigation because we did not have it yet in our department during the study period. The highly functional character of the stated structures and their difficult accesses inspire in first analyzing the therapeutic abstention for this kind of cavernomas. However, some authors believe that the risk of major neurological problems in case of bleeding, in eminently functional, justifies a preventive operative indication of the risk of hemorrhagic [21]. This is the case of localizations in the body callous, an affordable location as described above, or localizations flush or exophytic brainstem. Besides, the surgical management of multiple cavernomas does not differ in any way from that of the unique lesions. It must take into account the age and general condition of patients, clinical symptomatology, and localization of cavernomas [22]. In our series, we treat one case with stereotaxic radiosurgery. Radiosurgery for cavernomas treatment is considered a good alternative or an adjunct to surgery in a number of small brain lesions [23,24]. This radiosurgical method is being proposed for patients who do not seem to be able to benefit from open surgery and especially when the cavernoma sits in the middle pit because of important problems of hemostasis encountered in this localization [24].
Due to the potential risks associated with interventional treatment, there have been several studies on the effectiveness of medical management of CMs, allowing lesions to progress naturally and only alleviating the clinical symptoms. Fernández et al. reported that surgical treatment of patients with no refractory epilepsy did not significantly decrease the risk of future seizures when compared with conservative management. They observed 17 patients who received medical management for 5 years and 12 of them (70.6%) remained seizure-free [25]. Garrett and Spetzler studied 14 patients who managed conservatively and found that 50% of them improved or remained at their baseline, 29% became worse, and 7% died, while 14% did not complete the study [26]. While some positive findings on conservative management were reported, there are important limitations to these studies because researchers retrospectively studied patients who did not receive surgical treatment for various reasons, for example, because they maintained good control of their epilepsy, because of the location of cavernoma, or simply because they declined surgery [27]. In our series, patients that were managed conservatively had a favorable outcome in 85.7% (n=6) of 7 epilepsy cases with dual therapy control; recovering of the neurological deficit in 40% (n=2/5) of cases with a neurological deficit. This study is a retrospective study, it was difficult to achieve good imaging follow-up in our entire patient due to the lack of means in our center which is located in a low middle-income country. But the clinical follow-up was possible to evaluate properly the clinical improvement of the patient. Besides this study highlight the multimodality possibility to overcome the challenges of cavernoma management.
Surgical excision of cavernoma is the treatment of choice as much as possible when it is symptomatic. With the help of the intraoperative neuronavigation techniques, diffusion-tensor, neurosurgeons can resect deep-seated lesions in eloquent areas of the brain with minimal new neurological deficits and low mortality and morbidity rates. Radiosurgery offers an alternative that, without replacing excision surgery, remains promising. The prognosis depends on the clinical state of the patient at the time of diagnosis and the seat of the malformation.
What is known about this topic
- Cavernomas revealed by epilepsy, hemorrhage, headache, deficit neurologic;
- Treatment could be conservative, or surgical in Africa.
What this study adds
- Nowadays in Africa, only a few centers have radiosurgery or good equipment to manage surgically intracranial cavernoma;
- This study highlights multimodal management of intracranial cavernomas and challenges encountered with management guidelines.
The authors declare no competing interests.
Mahjouba Boutarbouch: conceptualization, methodology, data curation, writing - original draft, supervision, reviewing. Nourou Dine Adeniran Bankole: writing - original draft, methodology, data analysis, reviewing and editing, Adyl Melhaoui, and Yasser Arkha: validation, review-and editing, Abdessamad El Ouahabi, and Abdeslam El Khamlichi: Supervision, validation, review-and editing. All the authors have read and agreed to the final manuscript.
Table 1: patients characteristics summary
Table 2: multimodal management summary
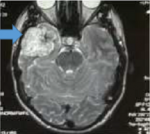
Figure 1: preoperative MRI T2 axial view of right side temporal cavernoma
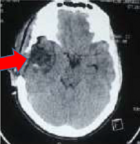
Figure 2: CT scan postoperative showing total removal of temporal
- Kivelev J, Niemel� M, Kivisaari R, Hernesniemi J. Intraventricular cerebral cavernomas: a series of 12 patients and review of the literature. J Neurosurg. 2010;112(1):140-9. PubMed | Google Scholar
- Maraire JN, Awad IA. Intracranial cavernous malformations: lesion behavior and management strategies. Neurosurgery. 1995;37(4):591-605. PubMed | Google Scholar
- Aiba T, Tanaka R, Koike T, Kameyama S, Takeda N, Komata T. Natural history of intracranial cavernous malformations. J Neurosurg. 1995;83(1):56-59. PubMed | Google Scholar
- Baqué jean. Cavernomes du système nerveux central: à propos de 25 cas et revue de la littérature. Thèse médicale n�117, Université de Nice. 2000.
- Houtteville JP. Les cavernomes du système nerveux central: historique et évolution des idées. Neurochirurgie. 2007;53(2):117-121. Google Scholar
- Del Curling O Jr, Kelly DL Jr, Elster AD, Craven TE. An analysis of the natural history of cavernous angiomas. J Neurosurg. 1991;75(5):702-8. Google Scholar
- Kondziolka D, Lunsford LD, Kestle JR. Natural history of cranial cavernous malformations. Journal of Neurosurgery. 1995;83(5):820-824. PubMed | Google Scholar
- Herter T, Brandt M, Szüwart U. Cavernous hemangiomas in children. Childs Nerv Syst. 1988;4(3):123-127. PubMed | Google Scholar
- Brunereau L, Labauge P, Tournier-Lasserve E, Laberge S, Levy C, Houtteville JP. Familial form of intracranial cavernous angioma: MR imaging findings in 51 families. Radiology. 2000;214(1):209-16. PubMed | Google Scholar
- Houtteville JP. Les cavernomes intracrâniens. Neurochirurgie. 1989;35(2):73-131.
- Mahla K, Rizk T, Fischer C, Belliard H, Vallée B, Fischer G. Intracranial cavernoma. Surgical results of 47 cases. Neurochirurgie. 1999 Nov;45(4):286-92. PubMed | Google Scholar
- Brühlmann Y, de Tribolet N, Berney J. Intracerebral cavernous angiomas. Neurochirurgie. 1985;31(4):271-9. Google Scholar
- Jabre A, Patel A. Transulcal microsurgical approach for subcortical small brain lesions: technical note. Neurosurgical Focus. 2006;65(3):312- 3. PubMed | Google Scholar
- Khouri S, Lacerda Leal P, Guarnieri J, Borha A, Gadan B, Emery E et al. Traitement chirurgical des cavernomes corticaux et souscorticaux. Principes généraux et série personnelle de 20 cas opérés entre 2000 et 2006. Neurochirurgie. 2007 Jun;53(2-3 Pt 2):163-7. PubMed | Google Scholar
- Jannin P, Seigneuret E, Morandi X, Fleig OJ, Riffaud L, Le Goualher G et al. Sulcal identification and neuronavigation in supratentorial cavernoma surgery. Neurochirurgie. 2000;46(6):534-9. PubMed | Google Scholar
- Sousa AA. Cavernomes profonds (corps calleux, intraventriculaires, ganglions de la base, insulaires) et du tronc cérébral. Expérience d´une série brésilienne. Neurochirurgie, 2007;53(3):182-191. Google Scholar
- Tirakotai W, Sure U, Benes L, Krischek B, Bien S, Bertalanffy H. Image-guided transsylvian, transinsular approach for insular cavernous angiomas. Neurosurgery. 2003;53(6):1299-1305. PubMed | Google Scholar
- Kupersmith MJ, Kalish H, Epstein F, Yu G, Berenstein A, Woo H et al. Natural history of brainstem cavernous malformations. Neurosurgery. 2001;48(1):47-53. PubMed | Google Scholar
- Kyoshima K, Kobayashi S, Gibo H, Kuroyanagi T. A study of safe entry zones via the floor of the fourth ventricle for brain-stem lesions. Report of three cases. J Neurosurg. 1993; 78(6):987-993. PubMed | Google Scholar
- Samii M, Eghbal R, Carvalho GA, Matthies C. Surgical management of brainstem cavernomas. J Neurosurg. 2001;95(5):825-832. PubMed | Google Scholar
- Nannucci S, Pescini F, Poggesi A, Ciolli L, Patrosso MC, Marocchi A et al. Familial cerebral cavernous malformation: report of a further Italian family. Neurol Sci. 2009;30(2):143-147. PubMed | Google Scholar
- Tindall RS, Krikpatrick JB, Sklar F. Multiple small cavernous angiomas of the brain with increased intracranial pressure. Ann Neurol. 1978;4(4):376-378. PubMed | Google Scholar
- Khalil T, Lemaire JJ, Chazal J, Verrelle P. Role of radiosurgery in the management of intracranial cavernomas. Review of the literature. Neurochirurgie. 2007 Jun;53(2-3 Pt 2):238-42. PubMed | Google Scholar
- García-Muñoz L, Velasco-Campos F, Lujan-Castilla P, Enriquez-Barrera M, Cervantes-Martínez A, Carrillo-Ruiz J. La radiochirurgie dans le traitement des cavernomes. Expérience de 17 lésions traitées chez 15 patients. Neurochirurgie, 2007;53(3): 243-250. PubMed | Google Scholar
- Fernández S, Miró J, Falip M, Coello A, Plans G, Castañer S, Acebes JJ. Surgical versus conservative treatment in patients with cerebral cavernomas and non refractory epilepsy. Seizure. 2012;21(10):785-788. PubMed | Google Scholar
- Bozinov O, Hatano T, Sarnthein J, Burkhardt JK, Bertalanffy H. Current clinical management of brainstem cavernomas. Swiss Med Wkly. 2010;140:w13120. PubMed | Google Scholar
- Mouchtouris N, Chalouhi N, Chitale A, Starke RM, Tjoumakaris SI, Rosenwasser RH et al. Management of cerebral cavernous malformations: from diagnosis to treatment. Scientific World Journal. 2015; 2015:808314. PubMed | Google Scholar