Lupus-associated acute pancreatitis following initiation of glucocorticoid therapy: should corticosteroids be discontinued or kept? (case report)
Ismail Belefqih, Houda Bachir, Samah Tahri, Siham Hamaz, Habiba Alaoui, Khalid Serraj
Corresponding author: Ismail Belefqih, Internal Medicine, Faculty of Medicine and Pharmacy of Oujda, Oujda, Morocco 
Received: 07 May 2022 - Accepted: 28 Jun 2022 - Published: 30 Jun 2022
Domain: Internal medicine
Keywords: Lupus, acute pancreatitis, glucocorticoids, immunosuppressive therapy, case report
©Ismail Belefqih et al. PAMJ Clinical Medicine (ISSN: 2707-2797). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Ismail Belefqih et al. Lupus-associated acute pancreatitis following initiation of glucocorticoid therapy: should corticosteroids be discontinued or kept? (case report). PAMJ Clinical Medicine. 2022;9:18. [doi: 10.11604/pamj-cm.2022.9.18.35348]
Available online at: https://www.clinical-medicine.panafrican-med-journal.com//content/article/9/18/full
Case report 
Lupus-associated acute pancreatitis following initiation of glucocorticoid therapy: should corticosteroids be discontinued or kept? (case report)
Lupus-associated acute pancreatitis following initiation of glucocorticoid therapy: should corticosteroids be discontinued or kept? (case report)
Ismail Belefqih1,&, ![]() Houda Bachir1, Samah Tahri1, Siham Hamaz1, Habiba Alaoui1, Khalid Serraj1
Houda Bachir1, Samah Tahri1, Siham Hamaz1, Habiba Alaoui1, Khalid Serraj1
&Corresponding author
Systemic Lupus Erythematosus (SLE) is an autoimmune disease that can affect different organs and may have serious complications. Lupus-associated acute pancreatitis is one of its rare manifestations and can be fatal. Despite its severity, the rarity of this affection means there is still no consensus regarding the ultimate approach for management. Many cases have been reported and showed improvement using a variety of immunosuppressive drugs. Lupus pancreatitis remains a diagnosis of exclusion. We report the case of a 21-year-old patient who was admitted to the hospital for a newly diagnosed SLE, with skin, articular and hematological manifestations during the stay, the patient was put on glucocorticoid therapy, following which she reported epigastric pain, laboratory tests and computed tomography (CT) scan confirmed the diagnosis of necrotizing pancreatitis. The patient received a 3-days pulse of methylprednisolone in addition to supportive care, and improved within the second day and was discharged the week after.
There are few cases of lupus associated pancreatitis reported around the world. Many of these reports noticed the onset of this acute episode following an active disease or the initiation of an immunosuppressive therapy [1]. The disease is usually severe, and the outcome can be fatal. There is no consensus regarding the ultimate approach to management, although many reports relied on a variety of immunosuppressive therapy [2].
Patient information: we present the case of a 21-year-old woman, without any underlying comorbidities, who was admitted to the hospital for a generalized erythroderma and purpura associated with inflammatory polyarthralgia of the extremities and diffuse myalgia.
Clinical findings: initial physical examination found a hemodynamically, respiratory, and neurologically stable patient, with a facial erythema, purpuric lesions on the lower limbs and a discrete edema of lower limbs.
Diagnostic assessment: initial laboratory tests showed positive antinuclear antibodies (ANA) at a titer of 1:1280 (using FISH technique), positive anti-DNA antibodies, and low levels of C3 and C4 complements. The creatine phosphokinase (CPK) was elevated at 10-fold the normal range upper limit, transaminases levels were elevated, as was Gamma Glutamyl transferase level at 6 folds the normal range upper limit, while bilirubin and alkaline phosphatase levels were normal. The 24 hours urine proteinuria was positive at 0.8 gram. The complete blood count showed a mild thrombocytopenia at 130 000/mm3 and a normocytic normochromic anemia at 7 grams/dl with a positive direct Coombs Test; white blood cells level was normal at 5300 elements per microliter with a lymphopenia at 730 elements per microliter. Haptoglobin level was low, while bilirubin levels were within the normal range. The results are summarized in Table 1. A skin biopsy of a purpuric lesion revealed leukocytoclastic vasculitis. A renal biopsy revealed a class III lupus nephritis. The diagnosis of a systemic lupus erythematosus was established using the 2019 European League Against Rheumatism (EULAR)/American College of Rheumatology (ACR) classification for systemic lupus erythematosus.
Therapeutic interventions: the decision was to initiate treatment with hydroxychloroquine at a dose of 200�mg twice a day, and glucocorticoid therapy with prednisone at a dose of 1�mg/kg/day. Two days following the initiation of therapy, the patient complained of the acute onset of an epigastric pain without any particular radiation, associated with vomiting. Physical evaluation found a hemodynamically stable patient, with a cardiac frequency of 80 beats per minute, a normal breathing rate at 14 cycles per minute, and a normal temperature at 37.3°C. Abdominal examination found epigastric tenderness. Laboratory tests were ordered and showed an elevated serum lipase level at 46-fold the normal range upper limit at 3646 UI/L (normal range 8-78 UI/L), normal transaminases, triglyceride level, and calcium levels. The complete blood count showed a normal white blood cells count at 7000 elements /microL. A CT scan was performed 48 hours following the pain onset and showed a necrotizing pancreatitis classified according to Balthazar score (modified score at 4). Moreover, there were no gallstones or sludge (Figure 1). Due to the absence of systemic inflammatory response syndrome (SIRS) elements (tachycardia, fever, polypnea, elevated white blood cells), the diagnosis of a mild pancreatitis was established. The patient received supportive care, consisting of oral feeding cessation, intravenous hydration with normal saline solution, and analgesia with acetaminophen. As a specific therapy, the patient received a 3-day Methylprednisolone pulse therapy at a dose of 15 mg/kg/day.
Follow-up and outcome of interventions: the evolution was marked by the disappearance of pain and oral diet initiation at day 2 of the pulse. Serum lipase level returned to normal on the 5th day and the patient was discharged the week after on prednisone 1 mg/kg a day and hydroxychloroquine 200 mg twice a day. A CT scan performed 7 weeks after the acute pancreatitis episode showed the resolution of necrosis (Figure 2). Following the resolution of necrosis, mycophenolate therapy was initiated for the lupus nephritis.
Informed consent: the patient provided a clear and well-informed written consent for the publication of the case.
Lupus associated pancreatitis is a rare but possibly fatal manifestation of SLE. Reports showed an incidence varying from 0.4 to 1.1 cases per 1000 lupus patients [3]. The pathogenesis remains unclear; but vascular damage is considered as the main plausible mechanism [4]. Histological studies of pancreas on autopsies revealed mainly vascular lesions; thrombosis and vasculitis [2]. The main risk factor appears to be an active disease [1]; Initiation of an immunosuppressive drug (e.g. glucocorticoids; azathioprine) also appear to play a role [4]. The most frequent clinical sign is abdominal pain, which was reported in 88% of patients [3]. The diagnosis of the acute pancreatitis is then based on elevated serum pancreatic enzymes and imaging depicting an abnormal pancreas (CT scan). Lupus pancreatitis remains a diagnosis of exclusion, and thus, ruling out main causes of acute pancreatitis, including gallstone disease, ethanol consumption, hypertriglyceridemia, and hypercalcemia, is necessary. Mortality rates have been reported as high as 45 percent [4], which is higher than in non-lupus pancreatitis. Complications are the same as non-lupus pancreatitis; represented by respiratory failure, pleural effusion, acute renal failure and circulatory shock [5]. Recurrent episodes of pancreatitis have been reported [5]. In our case; the acute pancreatitis occurred 2 days after initiation of glucocorticoid therapy on an active disease. Even though glucocorticoids might trigger an acute pancreatitis, as was demonstrated in animal experimentation [1]; studies have shown that keeping them may be useful in reducing mortality [5]. Overall, reported cases of acute pancreatitis in lupus occurred within 3 weeks following initiation of a glucocorticoid therapy, but approaches on management have been different in these studies as some discontinued the drug while others kept or even increased the dose. Other immunosuppressive therapies may be added, including azathioprine and cyclophosphamide, and severe cases could benefit from immunoglobulin therapy or plasmapheresis [2].
Lupus associated pancreatitis is a rare but potentially fatal complication of SLE. An active disease appears to be the main precipitating factor. Although glucocorticoid therapy may play a role in its occurrence; its continuation might be beneficial, as was demonstrated in our case. While other immunosuppressive therapies have been reported to be beneficial in reducing symptoms and mortality overall; there is still no clear consensus regarding the optimal approach to specific therapy. As glucocorticoid therapy is a main component in the management of SLE, clinicians should keep in mind that acute pancreatitis following the initiation of this therapy might not constitute a contraindication in itself.
The authors declare no competing interests.
Patient management: Ismail Belefqih, Houda Bachir, Samah Tahri, Khalid Serraj. Manuscript revision: Houda Bachir, Samah Tahri, Habiba Alaoui, Khalid Serraj. All the authors have read and agreed to the final manuscript.
Table 1: summary of the results of initial laboratory finding
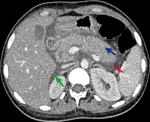
Figure 1: initial abdomen CT scan depicts a swollen homogeneously enhanced pancreatic gland (blue arrow) with fat stranding (red arrow) and poorly defined fluid collections (green arrow) in the peripancreatic and retroperitoneal spaces (Balthazard grade E with CTSI 4)
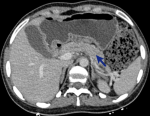
Figure 2: follow-up CT scan 7 weeks later shows significant resolution of fluid and fat stranding and normalization of the pancreatic parenchyma (blue arrow)
- Dwivedi P, Kumar RR, Dhooria A, Adarsh MB, Malhotra S, Kakkar N et al. Corticosteroid-associated lupus pancreatitis: a case series and systematic review of the literature. Lupus. 2019;28(6):731-739. PubMed | Google Scholar
- Nesher G, Breuer GS, Temprano K, Moore TL, Dahan D, Baer A et al. Lupus-associated pancreatitis. Seminars in Arthritis and Rheumatism. 2006;35(4):260-267. PubMed | Google Scholar
- Breuer GS, Baer A, Dahan D, Nesher G. Lupus-associated pancreatitis. Autoimmunity Reviews. 2006;5(5):314-318. PubMed | Google Scholar
- Makol A, Petri M. Pancreatitis in systemic lupus erythematosus: frequency and associated factors-a review of the Hopkins Lupus Cohort. The Journal of Rheumatology. 2010 Feb;37(2):341-5. PubMed | Google Scholar
- Favarato MH. Lupus-associated pancreatitis: clinical aspects. Journal of Rheumatic Diseases and Treatment. 2015. Google Scholar