Carpal tunnel syndrome secondary to extrapulmonary tuberculosis: a case report
Sergio Candido Ekekang Ncogo Nsegue, Mohamed Benchakroun, Kamal El Mokhtari, Noel Mamfoumbi, Hajar El Agouri, Salim Bouabid
Corresponding author: Sergio Candido Ekekang Ncogo Nsegue, Department of Traumatology and Orthopedic Surgery Mohammed V Military University Hospital Rabat, Morocco 
Received: 27 Jan 2022 - Accepted: 04 Apr 2022 - Published: 06 May 2022
Domain: Infectious disease, Orthopedic surgery
Keywords: Carpal tunnel syndrome, extrapulmonary tuberculosis, tenosynovitis, tuberculosis, case report
©Sergio Candido Ekekang Ncogo Nsegue et al. PAMJ Clinical Medicine (ISSN: 2707-2797). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Sergio Candido Ekekang Ncogo Nsegue et al. Carpal tunnel syndrome secondary to extrapulmonary tuberculosis: a case report. PAMJ Clinical Medicine. 2022;9:2. [doi: 10.11604/pamj-cm.2022.9.2.33477]
Available online at: https://www.clinical-medicine.panafrican-med-journal.com//content/article/9/2/full
Carpal tunnel syndrome secondary to extrapulmonary tuberculosis: a case report
![]() Sergio Candido Ekekang Ncogo Nsegue1,&, Mohamed Benchakroun1, Kamal El Mokhtari1, Noel Mamfoumbi1,
Sergio Candido Ekekang Ncogo Nsegue1,&, Mohamed Benchakroun1, Kamal El Mokhtari1, Noel Mamfoumbi1, ![]() Hajar El Agouri2, Salim Bouabid1
Hajar El Agouri2, Salim Bouabid1
&Corresponding author
In this article, we present a rare case of carpal tunnel syndrome secondary to flexor tenosynovitis from M. tuberculosis. This condition should be considered in the differential diagnosis of carpal tunnel syndrome and mass lesions of the wrist as early diagnosis and appropriate treatment for M. tuberculosis infection is important to restore hand function, in patients with late diagnosis poor functional outcome can occur. The patient should receive a combination of carpal tunnel release, flexor tenosynovectomy, and appropriate antibiotics which should yield complete resolution of symptoms. Here we present a case report which was diagnosed and treated successfully at our center.
Although rare in developed countries, tuberculosis is one of the most feared diseases in underdeveloped and developing countries where it constitutes a real public health problem. Skeletal involvement is unusual and occurs in 10%-15% of TB patients [1]. The possibility of upper-extremity involvement, especially in hand, is very rare. Its unusual presentations such as tuberculous tenosynovitis of the hand are often unrecognized and are associated with diagnostic and therapeutic delay, especially since formal histological evidence may sometimes be lacking. Carpal tunnel syndrome due to tuberculous tenosynovitis in the hand is a rare condition that requires early diagnosis and treatment to prevent complications that lead to poor functional outcomes of the hand [2].
Patient information: a 30-year-old male who worked as a butcher presented to us complaining of occasional mild left hand numbness for 2 years, recently progressing to severe pain and weakness. The patient had no significant past medical or surgical history. There was no history of trauma although the patient recalled to have sustained superficial cuts to his left hand occasionally due to his work during the past few years. The patient did not report having any fever, night sweats, cough or weight loss, and the patient had no contact with anyone with tuberculosis recently.
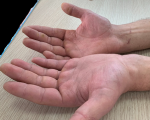
Clinical findings: on physical examination, there was numbness of the left index, middle, and ring fingers and diffuse swelling over the entire left palm and distal volar wrist that extended about 6cm proximally (Figure 1). There was a positive Tinel and Phalen tests at the wrist.
Timeline of current episode: the symptoms began 2�years before consulting our center with occasional mild left-hand numbness and later slowly developed into severe pain and weakness of the hand with a swelling of the volar wrist that appeared about 1.5 years after symptoms began.
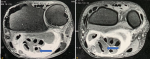
Diagnostic assessment: plain radiographs of the hand and thorax were normal except for increased soft tissue opacity over the left wrist, with no calcification or osseous abnormality. Laboratory findings were within normal limits (blood cell counts, erythrocyte sedimentation rate, C-reactive protein, antinuclear antibodies, rheumatoid factor, anti-SS-A, anti-DNA, anti-HIV, anti-HVC, VDRL, TSH, and T4). Pre-operative chest X-ray was normal. Electromyography and nerve conduction studies confirmed the clinical diagnosis of CTS. A distal motor latency of >4.5 ms and a sensory latency of >3.5 ms were consistent with carpal tunnel syndrome (CTS) diagnosis. MRI was ordered to help elucidate the hand and forearm swelling, and showed soft tissue swelling and diffuse synovitis within the carpal canal, thickening of the bursa and a deep cystic lesion measuring 15�mm, producing a mild mass effect on the tendons and median nerve (Figure 2).
Diagnosis: all the above clinical and imaging results confirmed the diagnosis of carpal tunnel syndrome and wrist tenosynovitis within the carpal canal.
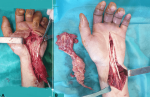
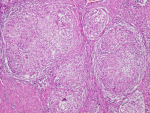
Therapeutic interventions: using regional anesthesia, carpal tunnel was released by volar approach in the wrist with extension into the forearm and palm. After opening the flexors' retinaculum, we encountered multiple false membranes along the flexor tendons and the compressed median nerve. The synovium within the carpal tunnel was grossly thickened and adherent to the median nerve and flexor tendons. The median nerve was compressed, and the epineurium was thickened (Figure 3). After careful dissection and taking care of the neurovascular structures, radical excision of the synovial sheath of tendons was done, the median nerve was released. The excised specimen measured 12.5x7.5x3cm and showed an irregular surface. The histological examination of the specimen revealed hyperplasia of the synovial lining epithelium. The underlying tissue exhibited the typical granulomatous reaction associated with tuberculosis infection, with numerous granulomas of various size, caseating and non-caseating, containing epithelioid and giant cells, as well as a chronic inflammatory infiltrate (Figure 4,Figure 5). These features are consistent with the clinical diagnosis of tuberculous tenosynovitis. The patient was treated with isoniazid, rifampicin, pyrazinamide, and streptomycin for 2 months then with rifampicin and isoniazid for 10 months.
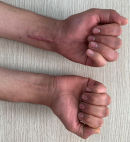
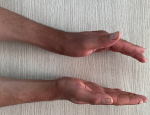
Follow-up and outcome of interventions: a culture of the specimen was performed and was positive for tubercle bacilli. Finger movements were encouraged from day 2. Early postoperative complications such as bleeding, hematoma, wound dehiscence, and infection were not observed. At the last follow-up appointment, anterior wrist swelling and sensory disturbance had disappeared, with no clinical sign of recurrence. At 6 months follow up the patient had full active and passive painless motion of the wrist and fingers (Figure 6,Figure 7).
Patient perspective: “It has been a year after surgery and I have regained a confortable and painless wrist and hand that allows me to do my job in a more efficient way”.
Informed consent: the patient gave informed written consent about the publication of this article.
Infection caused by Mycobacterium tuberculosis in developing countries and the third world is a major health problem. In musculoskeletal system, spinal vertebra involvement usually occurs in 30%-50%. Soft-tissue involvement is rare. Tuberculosis-induced CTS is rare. Tenosynovitis due to M. tuberculosis is reported to be <1% of the cases [2,3]. The largest case series of flexor tenosynovitis from Mycobacterium tuberculosis with median nerve involvement published so far reported 12 cases followed up for 10 years [4]. Tuberculous tenosynovitis is caused due to hematogenous spread from a primary focus of infection or by direct inoculation from adjacent infected tissue [5], in our case direct inoculation is probably the cause as the patient is a butcher. The disease may be associated with several factors, including older age, male gender, profession, low income, poor nutrition, history of or exposure to TB, immunosuppression, alcohol abuse, permanence in endemic areas and corticosteroid infiltration [6].
The progression of disease is slow and insidious. Initially, the symptoms are minimal. There is mild swelling around the wrist initially, which involves the adjacent areas over few months to years. Most patients come very late for medical advice after the development of pain, discomfort or median nerve compression symptoms [7] and restrictions of movement of fingers or wrists. Local signs of inflammations are very minor [8] even though synovial inflammation is present at various stages [5]. These types of swelling have a large category of differential diagnoses like pyogenic tenosynovitis, fungal infection, rheumatoid arthritis, gouty arthritis, infected ganglion, foreign body reaction granuloma, pigmented villonodular synovitis, sarcoidosis, brucellosis, systemic lupus erythematosus, etc [9,10]. Early diagnosis and appropriate treatment for M. tuberculosis infection that could go up to 14�months therapy [11,12] is important to restore the performance, in patients with late diagnosis poor functional outcome can occur [2], thus a mild tender and painful swelling in the anterior wrist should raise suspicion of TB in patients with clinical symptoms of CTS. The vast majority of patients test positive for tuberculin, while chest X-rays are normal in 50% of cases [13]. Ultrasound and magnetic resonance imaging may be useful to evaluate lesion extension and severity, with visualization of synovial thickening and relatively small effusions.
Given the clinical symptoms of CTS and after confirmation of nerve suffering on the electromyography, a carpal tunnel release should be done in order to release pressure on the median nerve. If the surgeon encounters extensive synovitis with adhesion to other structures during surgery then TB should be suspected, and direct smear, culture, and histologic examination of the specimens should be requested. This synovial inflammation has three stages [5]: 1) Stage 1 (hygromatous): increased synovial exudates inside the sheath is found. 2) Stage 2 (serofibrinous): caseous debris and fibrous tissue replace the exudates (rice and melon seed bodies). 3) Stage 3 (fungoid): extensive caseation and sinus formation with bone and joint involvement. Similar to what happens in other sites, local effusions may test negative for AFS bacilli and specific culture may take 8 weeks to reveal bacilli. In the present case, M. tuberculosis culture was positive after 3 weeks, indicating high bacilli loads. Typical histopathology shows caseous granulomas surrounded by epithelioid histiocytes and multinucleate giant cells associated to the presence of bacilli. However, in a study on arthritis from TB by Garrido and coworkers, 12% of the patients presented no granulomas and, among the remainder, 27% had non-caseous granulomas [14]. The postoperative use of anti-TB drugs is suggested in accordance with culture and sensitivity results [3]. The medical treatment of patients with negative smear test results should start after positive histopathology reports because the delay in culture and sensitivity results may delay the treatment by about 6 weeks [3]. Treatment by isoniazid, rifampicin, pyrazinamide, and streptomycin for 2 months should be completely performed; and the treatment should be also continued by rifampicin and isoniazid for 10-14 months [12,13]. The mentioned therapy was very successful in our patient.
Carpal tunnel syndrome can be secondary to many etiologies, and flexor tenosynovitis due to M. Tuberculosis should be a differential diagnosis to the physician, especially in places where tuberculosis is endemic. Early diagnosis and treatment is essential for a complete recovery of symptoms. In our case, a complete flexor synovectomy and carpal tunnel release followed by anti TB drugs was very successful in our patient.
The authors declare no competing interests.
Data collection: SCENN, KEM and MB. Written manuscript: SCEN and MB. Conception, Interpretation and Intellectual content: HEA and NM. Intellectual content of critical importance and article review: SB. All authors read and approved the final manuscript.
Figure 1: preoperative hand appearance showing diffuse swelling over the entire left palm and distal volar wrist
Figure 2: A,B) MRI of the hand in axial section T1 sequence without fatsat: hyper signal thickening of the sheaths of all the flexor tendons of the hand (blue arrows)
Figure 3: A,B) intraoperative hand appearance showing thickened synovium and false membrane
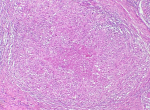
Figure 4: photomicrograph of a histopathological section of the synovium shows multiple granulomas containing epithelioid histiocytes and multinucleated giant cells (Hematoxylin and eosin stain, original magnification x100)
Figure 5: photomicrograph shows a caseating granuloma surrounded by epithelioid histiocytes and multinucleated giant cells (Hematoxylin and eosin stain; original magnification x200)
Figure 6: full active and painless motion of the fingers at 6 months follow up
Figure 7: dissapearance of anterior wrist swelling on follow up
- Elmi A, Tabrizi A, Tolouei FM. Skeletal tuberculosis presenting as a small cystic lesion in the medial femoral condyle. Arch Bone Jt Surg. 2013 Dec;1(2):112-5. PubMed | Google Scholar
- Marques VB, Vieira HP, Alcantara AC, Braga FN, Rocha FA, Medeiros MC. Tenosynovitis and carpal tunnel syndrome from Mycobacterium tuberculosis - a rare manifestation of extrapulmonary tuberculosis. Acta Reumatol Port. 2010;35(1):82-4. PubMed | Google Scholar
- Suso S, Peidro L, Ramon R. Tuberculous synovitis with “rice bodies” presenting as carpal tunnel syndrome. J Hand Surg Am. 1988 Jul;13(4):574-6. PubMed | Google Scholar
- Hassanpour ES, Gousheh J. Mycobacterium tuberculosis - induced carpal tunnel syndrome: management and follow-up evaluation. J Hand Surg. 2006 Apr;31(4):575-9. PubMed | Google Scholar
- Hooker RP, Eberts TJ, Strickland JA. Primary inoculation tuberculosis. J Hand Surg Am. 1979 May;4(3):270-3. PubMed | Google Scholar
- Albornoz MA, Mezgarzedeh M, Neumann CH. Granulomatous tenosynovitis: a rare musculoskeletal manifestation of tuberculosis. Clin Rheumatol. 1998;17(2):166-9. PubMed | Google Scholar
- Altaf W, Attarde D, Sancheti P. Tubercular compound palmar ganglion presenting as a severe carpal tunnel syndrome- a case report. J Clin Orthop Trauma. 2020 Oct;11(Suppl 5):S889-S891. PubMed | Google Scholar
- Baidoo PK, Baddoo D, Ocloo A, Agbley D, Lartey S, Baddoo NA. Tuberculous tenosynovitis of the flexor tendons of the wrist: a case report. BMC Res Notes. 2018 Apr 10;11(1):238. PubMed | Google Scholar
- Walker UA, Gutfleisch J, Peter HH. Case number 23: tuberculous tenosynovitis. Ann Rheum Dis. 2002 May;61(5):384. PubMed | Google Scholar
- Woon CY, Phoon ES, Lee JY, Puhaindran ME, Peng YP, Teoh LC. Rice bodies, millet seeds, and melon seeds in tuberculous tenosynovitis of the hand and wrist. Ann Plast Surg. 2011 Jun;66(6):610-7. PubMed | Google Scholar
- Janier M, Gheorghiu M, Cohen P, Mazas F, Duroux P. Carpal tunnel syndrome due to Mycobacterium bovis BCG (author´s transl). Sem Hop. 1982 Apr 22;58(16):977-9. PubMed | Google Scholar
- Kotwal PP, Khan SA. Tuberculosis of the hand: clinical presentation and functional outcome in 32 patients. J Bone Joint Surg Br. 2009 Aug;91(8):1054-7. PubMed | Google Scholar
- Hoffman GS, Sentochnik DE. Mycobacterial and fungal infections. In: Kelly WN, Harris ED, Ruddy S et al. editors. Textbook of rheumatology. Philadelphia: WB Saunders. 1989:1586-1591.
- Garrido G, Gomez-Reino JJ, Fern�ndez-Dapica P, Palenque E, Prieto S. Review of peripheral tuberculous arthritis. Semin Arthritis Rheum. 1988 Nov;18(2):142-9. PubMed | Google Scholar