Concomitant tuberculosis and sarcoidosis in a Nigerian woman: an important consideration in treatment failure: a case report
Omotola Oredipe, Sandra Kelechi Dede, Obianuju Beatrice Ozoh
Corresponding author: Omotola Oredipe, The Chest Clinic, Lagos, Nigeria 
Received: 29 May 2022 - Accepted: 04 Jul 2022 - Published: 06 Jul 2022
Domain: Infectious disease,Pulmonology
Keywords: Sarcoidosis, tuberculosis, case report
©Omotola Oredipe et al. PAMJ Clinical Medicine (ISSN: 2707-2797). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Omotola Oredipe et al. Concomitant tuberculosis and sarcoidosis in a Nigerian woman: an important consideration in treatment failure: a case report. PAMJ Clinical Medicine. 2022;9:23. [doi: 10.11604/pamj-cm.2022.9.23.35669]
Available online at: https://www.clinical-medicine.panafrican-med-journal.com//content/article/9/23/full
Case report 
Concomitant tuberculosis and sarcoidosis in a Nigerian woman: an important consideration in treatment failure: a case report
Concomitant tuberculosis and sarcoidosis in a Nigerian woman: an important consideration in treatment failure: case report
Omotola Oredipe1,&, Sandra Kelechi Dede1, ![]() Obianuju Beatrice Ozoh2
Obianuju Beatrice Ozoh2
&Corresponding author
Sarcoidosis and Tuberculosis are both inflammatory diseases that can affect more than one organ in the body. They both have a similar presentation in terms of symptomatology, histological and radiological findings, albeit different treatments making it important to differentiate between the two diseases. In this case report, we present the case of a 54-year-old African woman with symptoms of cough, shortness of breath and weight loss who was diagnosed as having pulmonary tuberculosis, however, her symptoms did not improve following treatment for Tuberculosis and she was referred for further assessment. Suspicion of sarcoidosis was raised after a finding of Erythema nodosum on physical examination and this was confirmed by elevated serum angiotensin converting enzyme levels and skin biopsy. She responded to high dose long term steroid therapy and Azathioprine. This case encourages physicians to be aware of the possibility of these disease entities occurring simultaneously.
Sarcoidosis is a multisystem inflammatory condition of unknown etiology characterized by non-caseating granulomas which can infiltrate any organ of the body but commonly affects the lungs, skin and eyes [1]. The incidence of sarcoidosis is estimated between 2.3 to 11 per 100,000 people per year. It affects people of all ages and races, but higher prevalence rates have been found among people 25 to 40 years old, women >50 years old, African-Americans and Caucasians of Scandinavian descent [2]. A Nigerian study by Nwosu et al. reported that 47.6% of interstitial lung disease cases in a tertiary hospital were due to sarcoidosis [3]. Tuberculosis, a chronic granulomatous disease, is a leading infectious cause of morbidity and mortality worldwide which also commonly affects the lungs but can also affect any organ [4]. Nigeria is the sixth-largest contributor to the global burden of Tuberculosis [5]. In 2020, the incidence of tuberculosis cases in Nigeria was 219 per 100,000 people [5]. Tuberculosis and sarcoidosis have similar clinical, histological and radiologic findings which underline a hypothesis about a possible link between both conditions [6]. Treatments of both conditions vary, making it imperative to accurately diagnose and treat both conditions independently. Although there are a few reports of concomitant sarcoidosis and tuberculosis globally [7], we are only aware of one such report from Nigeria, where both diseases are prevalent [8]. We report a case of sarcoidosis and tuberculosis occurring simultaneously in a Nigerian woman.
Patient information: a 54-year-old African female, non-smoker, non-alcoholic, non-hypertensive and non-diabetic. Her symptoms were productive cough, shortness of breath and weight loss. She had no history of contact with persons (family members, close workers) with similar symptoms and a history of tuberculosis treatment without improvement in her symptoms.
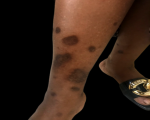
Clinical findings: the patient presented to our respiratory clinic with a history of productive cough, shortness of breath on moderate exertion and weight loss of 6 months duration. There was no history of fever or night sweats. In addition, she had dark plaques on her face and lower extremities Erythema nodosum. On chest examination; she had widespread crepitations.
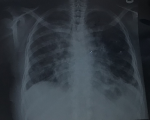
Timeline of current episode: May 2020: symptoms of cough, shortness of breath and weight loss started. July 2020: she presented to her primary care physician with the symptoms described above. She had a chest X-ray (Figure 1) and sputum microscopy, culture and sensitivity done at that visit. October 2020: skin biopsy done. November 2020: referred to our respiratory clinic due to worsening of her symptoms despite a negative sputum test for acid fast bacilli and treatment for pulmonary tuberculosis.
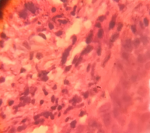
Diagnostic assessment: she had initially presented to her primary care physician with these symptoms three months earlier, where a chest X-ray (Figure 1) was done. The X-ray revealed hilar lymph nodes and widespread reticulonodular opacities in both lung fields. Her sputum was positive for acid-fast bacilli on microscopy. A diagnosis of pulmonary tuberculosis (TB) was made, and she commenced on the intensive phase of tuberculosis treatment with Rifampicin, Isoniazid, Pyrazinamide and Ethambol. At a follow-up visit three months later, her symptoms worsened despite a negative sputum test for acid-fast bacilli, which warranted referral to our center. On assessment, in addition to the persistent symptoms described above, we noticed dark plaques (Figure 2) on her extremities and face, which she reported had progressively worsened over a twelve-month period. A skin biopsy of the plaques was done which revealed lesions predominantly in the dermis composed of histiocytes forming granulomas alongside multinucleated giant cells and lymphocytes, entrapped skin adnexal structures and non-caseating necrosis in keeping with chronic granulomatous inflammation (Figure 3). This was highly suggestive of sarcoidosis. Serum Angiotensin Converting Enzyme (ACE) was elevated (200 U/L). Her lung function test showed severe restriction (Forced Vital Capacity (FVC): 38% of predicted, Forced Expiratory Volume in the first minute (FEV1): 39% of predicted).
Diagnosis: her symptoms and lack of improvement to tuberculosis treatment were suggestive of Sarcoidosis. Elevated Serum Angiotensin Converting Enzyme, skin biopsy result of non- caseating necrosis, severe restriction on pulmonary function testing confirmed the diagnosis of Sarcoidosis.
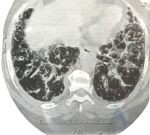
Therapeutic interventions: a daily dose of 40mg of prednisolone was prescribed in addition to her TB treatment. However, she was not adherent to the steroids. She re-presented at the clinic three months later in respiratory distress, her respiratory rate was 24 cycles per minute and her oxygen saturation was 89%. She had bi-basal crackles on chest auscultation, and her Erythrocyte Sedimentation Rate (ESR) was 42 mm in the first hour. A chest computed tomography (CT) scan showed extensive lung fibrosis, mediastinal lymphadenopathy and bilateral hilar lymphadenopathy in keeping with stage IV pulmonary sarcoidosis (Figure 4). She was given intravenous steroid initially and subsequently continued on oral steroids. She also applied Pimecrolimus cream to the skin lesions. Her symptoms began to improve, and the steroid dose was subsequently tailed down to 10mg daily and Azathioprine as well as inhaled steroids were also added to the treatment.
Follow-up and outcome of interventions: at her most recent follow-up visit, her symptoms improved remarkably. She has good exercise tolerance and serum ACE was normal (44U/L). Full blood count and ESR values were also within normal limits. However, her pulse rate was low (51 beats per minute). An electrocardiogram confirmed sinus bradycardia, which is suggestive of cardiac sarcoidosis (Figure 5). This prompted a decision to continue the oral steroid, and she has been referred to a cardiologist for review.
Patient perspective: “I am happy that I am now able to walk some distance without running out of breath and do most of my normal activities. I hope to keep getting better with treatment.”
Informed consent: the patient gave written informed consent and approval for her case to be published.
There are varying hypotheses to explain the concomitant occurrence of sarcoidosis and TB [9,10]. Although the exact etiology of sarcoidosis is unknown, studies have shown a link between TB infection and the development of sarcoidosis [1,11]. Serum samples from sarcoidosis patients have been found to contain antibodies to mycobacterial antigens such as Mycobacterium tuberculosis catalase-peroxidase (katG) and heat shock protein 70 [12]. A study in a Greek sarcoidosis population reported that 78% of tissues contained Mycobacterium TB DNA which was amplifiable [13]. These findings suggest that mycobacterial antigens in a susceptible host may trigger an immune response that leads to sarcoidosis. Other hypotheses have also suggested that TB may occur as a consequence of steroid-induced immunosuppression during treatment of sarcoidosis [12]. However, this hypothesis is refutable as in the case of our patient who had skin lesions prior to onset of the respiratory symptoms and in whom TB treatment was initially commenced.
Distinguishing between TB and sarcoidosis may prove a diagnostic challenge due to the clinical, radiologic and histologic similarities between the conditions [14]. Our patient was rightly diagnosed initially with pulmonary tuberculosis based on her clinical presentation and the presence of acid-fast bacilli in her sputum on Ziehl-Neelsen staining. However, an alternate diagnosis was suspected when her symptoms persisted despite TB treatment and sputum conversion. Concomitant diagnosis of sarcoidosis was then made based on spread of the skin lesions, CT scan findings, elevated serum ACE levels and a skin biopsy showing non-caseating granulomas. It is always pertinent to confirm the diagnosis of both conditions because a delay in treatment of either could lead to adverse outcomes. A case of acute respiratory distress has been reported in a patient with concomitant sarcoidosis and TB who was initially treated with only corticosteroids [15]. It has been suggested that in cases of severe concomitant disease, both anti-tuberculosis treatment and corticosteroid therapy could be started simultaneously [16]. In this present case, when the patient failed to take the prescribed treatment for sarcoidosis, her symptoms deteriorated and she developed respiratory distress that required oxygen supplementation.
This present case is also of interest because of the new-onset bradyarrhythmia which may suggest cardiac sarcoidosis. Autopsy findings among sarcoidosis patients show that up to 25% of them have cardiac granulomas, although only about 5% of them presented with clinical findings. Cardiac sarcoidosis develops as a result of granulomas in various locations in the heart, most commonly the left ventricular free wall, intraventricular septum and conducting system. It may present clinically as a cardiomyopathy, tachyarrhythmia or bradyarrhythmia. Cardiac magnetic resonance imaging (MRI) with gadolinium enhancement and positron emission tomography (PET) scanning are useful in diagnosis; however, endocardial biopsies are of low-diagnostic value because the location of cardiac granuloma is variable. Cardiac sarcoidosis may present with left ventricular dysfunction and sudden death. As such, electrophysiological evaluation to determine the risk of sustained arrhythmias should be conducted. Use of an electronic pacemaker may be warranted if there is complete heart block. In patients with ventricular fibrillation or tachycardia with severely reduced left ventricular ejection fraction, use of an automatic implantable cardioverter defibrillator is recommended [6].
We have presented an uncommon case of TB occurring simultaneously with sarcoidosis as evidenced by histologic, radiologic and bacteriologic findings. This highlights the need for physicians to be aware of the possibility of coexistence of sarcoidosis and TB, particularly in settings such as ours where both diseases are common. It is important for physicians to have an index of suspicion for concomitant disease in cases where the patient does not respond to initial treatment of either disease. Although cardiac sarcoidosis is uncommon, it is imperative that sarcoidosis patients undergo periodic electrophysiological assessments to detect and manage any underlying arrhythmias and reduce the risk of sudden cardiac death.
The authors declare no competing interests.
Patient management: OBO, SKD and OO; data collection: OO and SDK; manuscript drafting: OO and SKD; manuscript revision: OO, OOB and SDK. All authors approved the final version of the manuscript.
Figure 1: chest X-ray showing bilateral enlarged hilar lymph nodes and patchy reticulonodular opacities
Figure 2: cutaneous lesions on lower extremities
Figure 3: biopsy showing histiocytes forming granulomas alongside multinucleated giant cells and lymphocytes
Figure 4: chest computed tomography scan showing bilateral ground glass opacities with fibrosis and traction bronchiectasis
Figure 5: electrocardiogram of the patient showing bradycardia suggestive of cardiac sarcoidosis
- Iannuzzi MC, Rybicki BA, Teirstein AS. Sarcoidosis. N Engl J Med. 2007;357(21):2153-2165. PubMed
- Sève P, Pacheco Y, Durupt F, Jamilloux Y, Gerfaud-Valentin M, Isaac S et al. Sarcoidosis: a clinical overview from symptoms to diagnosis. Cells. 2021;10(4):766. Google Scholar
- Nwosu NI, Uduma V, Nlewedim P, Ukwaja KN, Onyedum C, Chukwuka C. Profile of interstitial lung disease at the University of Nigeria Teaching Hospital Enugu, Nigeria. Enugu. 2020. Google Scholar
- Agyeman AA, Ofori-Asenso R. Tuberculosis: an overview. J Public Health Emerg. 2017;1:7-7 Google Scholar
- World Health Organization. Global tuberculosis report 2020. Accessed June 19, 2022.
- Brownell I, Ramírez-Valle F, Sanchez M, Prystowsky S. Evidence for mycobacteria in sarcoidosis. Am J Respir Cell Mol Biol. 2011;45(5):899-905. PubMed | Google Scholar
- Pedroso A, Ferreira I, Chikura T. Tuberculosis and sarcoidosis overlap: a clinical challenge from diagnosis to treatment. Cureus. 2020 Nov 23;12(11):e11662. PubMed | Google Scholar
- Oluboyo P, Awotedu AA, Banach L. Concomitant sarcoidosis in a patient with tuberculosis: first report of association in Africa. The Central African Journal of Medicine. 2005;51(11-12):123-5. PubMed | Google Scholar
- Papaetis GS, Pefanis A, Solomon S, Tsangarakis I, Orphanidou D, Achimastos A. Asymptomatic stage I sarcoidosis complicated by pulmonary tuberculosis: a case report. J Med Case Reports. 2008 Jul 7;2:226. PubMed | Google Scholar
- Cho HS, Kim SJ, Yoo JY. Sarcoidosis during treatment of pulmonary tuberculosis: a rare case report and review of the literature. J Int Med Res. 2021 Apr;49(4):3000605211001632. PubMed | Google Scholar
- Gupta D, Agarwal R, Aggarwal AN, Jindal SK. Sarcoidosis and tuberculosis: the same disease with different manifestations or similar manifestations of different disorders. Current Opinion in Pulmonary Medicine. 2012;18(5):506-516. PubMed | Google Scholar
- Mandal SK, Ghosh S, Mondal SS, Chatterjee S. Coexistence of pulmonary tuberculosis and sarcoidosis: a diagnostic dilemma. Case Reports. 2014(dec19 1);bcr2014206016-bcr2014206016. PubMed | Google Scholar
- Gazouli M, Ikonomopoulos J, Trigidou R, Foteinou M, Kittas C, Gorgoulis V. Assessment of mycobacterial, propionibacterial, and human herpes virus 8 DNA in tssues of greek patients with sarcoidosis. J Clin Microbiol. 2012;40(8):3060-3063. PubMed | Google Scholar
- Agrawal R, Kee AR, Ang L, Tun Hang Y, Gupta V, Kon OM et al. Tuberculosis or sarcoidosis: opposite ends of the same disease spectrum. Tuberculosis. 2016;98:21-26. PubMed | Google Scholar
- Vadala R, Bhat MNM, Rabindrarajan E, Ramakrishnan N. Concomitant presentation of sarcoidosis and pulmonary tuberculosis with ARDS: a diagnostic dilemma and therapeutic challenge. Indian Journal of Tuberculosis. 2019;66(2):314-317. PubMed | Google Scholar
- Mise K, Goic-Barisic I, Puizina-Ivic N, Barisic I, Tonkic M, Peric I. A rare case of pulmonary tuberculosis with simultaneous pulmonary and skin sarcoidosis: a case report. Cases Journal. 2010 Jan 13;3:24. PubMed | Google Scholar