Locally advanced groin neurofibrosarcoma misdiagnosed twice as inguinal hernia: a case report
Axel Stephane Nwaha Makon, Frantz Epoupa, Owon Abessolo, Agbor Orock Tanyi, Paul Tolefac, Leon Ndongo Onana, Jean Cedric Fouda, Mbouché Landry Oriole, Pierre Joseph Fouda, Fru III Angwafor, Maurice Aurelien Sosso
Corresponding author: Axel Stephane Nwaha Makon, Department of Surgery and Subspecialties, Faculty of Medicine and Biomedical Sciences, University of Yaoundé 1, Yaoundé, Cameroon 
Received: 19 Jun 2022 - Accepted: 13 Aug 2022 - Published: 22 Aug 2022
Domain: Surgical oncology
Keywords: Neurofibrosarcoma, inguinal hernia, tumour, case report
©Axel Stephane Nwaha Makon et al. PAMJ Clinical Medicine (ISSN: 2707-2797). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Axel Stephane Nwaha Makon et al. Locally advanced groin neurofibrosarcoma misdiagnosed twice as inguinal hernia: a case report. PAMJ Clinical Medicine. 2022;9:41. [doi: 10.11604/pamj-cm.2022.9.41.35976]
Available online at: https://www.clinical-medicine.panafrican-med-journal.com//content/article/9/41/full
Case report 
Locally advanced groin neurofibrosarcoma misdiagnosed twice as inguinal hernia: a case report
Locally advanced groin neurofibrosarcoma misdiagnosed twice as inguinal hernia: a case report
Axel Stephane Nwaha Makon1,2,&, ![]() Frantz Guy Epoupa Ngalle1, Owon Abessolo1,3,
Frantz Guy Epoupa Ngalle1, Owon Abessolo1,3, ![]() Agbor Tanyi Orock1, Paul Tolefac1, Leon Ndongo Onana1,
Agbor Tanyi Orock1, Paul Tolefac1, Leon Ndongo Onana1, ![]() Jean Cedric Fouda1,3,
Jean Cedric Fouda1,3, ![]() Mbouché Landry Oriole1, Pierre Joseph Fouda1,3, Fru III Angwafor1, Maurice Aurelien Sosso1
Mbouché Landry Oriole1, Pierre Joseph Fouda1,3, Fru III Angwafor1, Maurice Aurelien Sosso1
&Corresponding author
Neurofibrosarcoma is a rare malignant, aggressive peripheral nerve sheet tumour. It presents diagnostic challenges as it is difficult to be distinguished from other tumours. It may present in all body regions. The authors report a case of a 26-year-old male who presented with recurrent inguinal mass following repair of an inguinal hernia. He was diagnosed with a malignant neurofibrosarcoma and multidisciplinary team (MDT) reviews done by the hospital oncology MDT declared the patient was not eligible for chemotherapy. The patient had tumour excision, and he died 3 months later. Inguinal masses may mimic an inguinal hernia. Traditional characteristics of an inguinal hernia should be sought for in all inguinal masses and a high index of suspicion be maintained.
Neurofibrosarcoma is a peripheral nerve sheet malignant tumour affecting the peripheral nerves. The real incidence and prevalence of these rare tumours is unknown worldwide with current studies estimating it to account for about 3-5% of all soft tissue sarcomas [1,2]. This tumour is very aggressive with a high metastatic and recurrence potential [3]. This tumour originates from the peripheral nerves and occurs mainly in the limbs, head and neck, and spine. Neurofibrosarcoma has a variety of histologic subtypes. Due to the diversity of histologic types, these tumours have a high histologic similarity to other benign and malignant soft tissue tumours. Due to the lack of specific diagnostic criteria, pathologic diagnosis is extremely difficult, since these tumours should be differentiated from other sarcomas according to the site of tumour occurrence and morphologic characteristics, which can be determined using immunohistochemical staining [2]. The incidence of neurofibrosarcoma peaks in individuals between 20 and 50 years of age, with a median age of 44 years [4]. The aetiology of these tumours remains unclear. However, studies have shown that there might be related to neurofibromatosis. The clinical manifestations are primarily enlarged masses, accompanied by pain, compression symptoms, and motor and sensory dysfunction [5]. Following an extensive literature search, very few cases of neurofibrosarcoma have been reported from Africa and no case from Cameroon.
Patient and observation: the authors report a case of a 26-year-old male who presented with recurrent right inguinal mass following surgical repair of a right inguinal hernia. He does not report any family history of cancers or genetically predisposed illness. He was diagnosed with a malignant neurofibrosarcoma, and he died 3 months later following tumour resection. This case has been reported in accordance with the CARE guidelines [6].
Case presentation: mr X is a 26-year-old male transferred by his primary care physician (PCP) in March 2021 from a district hospital to our tertiary hospital at Douala Laquinitinie Hospital (DLH) for evaluation and management of a right recurrent ulcerating groin mass. The patient reports that the swollen dates back about 10 months prior to presentation with an inguinal swollen diagnosed initially as right inguinal hernia for which a hernia repair was done by his primary care physician. One month following the inguinal hernia repair, he presented with a larger recurrence of the inguinal mass, prompting a second surgical exploration by the same health care provider. His PCP reports that during the second exploration there was a large necrotic tumour which a biopsy was taken for histopathology and the results came out suggestive of chronic inflammation. Following the 2nd surgical exploration, the mass increased rapidly in size, extending from the groin to the anterolateral abdominal wall and the left hemi-scrotum. The mass was ulcerative, constantly secreting yellowish offensive fluids. This prompted transferred to our tertiary centre at DLH.
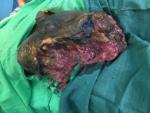
Clinical findings: on arrival and upon physical examination, the patient was cachectic and ill looking, with satisfactory vital signs. There was a giant ulcerative and fungating mass in the right groin extending to the right hemi-scrotum which measures about 30x20x10�cm as shown in the Figure 1.
Diagnostic assessment: the differential diagnosis at entry included testicular tumour and Fournier´s gangrene. The following investigations were requested MRI of the mass and the pelvis, complete blood count (CBC), clotting profile, blood group and Rhesus factor, urea and serum creatinine, lactate dehydrogenese (LDH), alpha fetoprotein (AFP). Magnetic resonance imaging (MRI), AFP and LDH were not done due to financial constraints. The results of biological investigations were as follows: haemglobin of 5g/dl, white cell count of 33000 cells/mm3. Clotting profile and renal functions were normal.
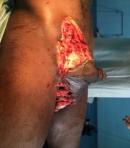
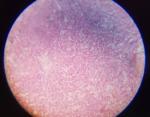
Therapeutic intervention: the immediate management consisted of blood transfusion, fluid and electrolytes correction and antibiotics. A pre-anestheic consultation was done in preparation for excision of the tumour. Surgery was done and consisted of excision of the mass as shown in Figure 2. Histopathology results after surgery were confirmatory of poorly differentiated locally advanced neurofibrosarcma with the margin of resections R2 as shown in Figure 3. Multidisciplinary team (MDT) review was done during the hospital oncology MDT, and he was declared not to be eligible for chemotherapy.
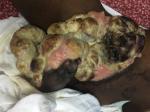
Follow-up and outcome: the postoperative treatment consisted of iterative blood transfusions, multimodal analgesics, antibiotics and local wound care. A month after surgery, the tumour has grown more than it was at initial presentation, as shown in Figure 4. He died three months following surgery.
There is paucity of literature in the epidemiology as well as the presentation and management of malignant neurofibrosarcoma. Here we report a young man with advanced metastatic neurofibrosarcoma of the groin, managed initially as inguinal hernia. The tumour was diagnosed following its second recurrence, presumed to be the second repair of inguinal hernia. Hernia is a common surgical disease, and cases of metastatic carcinoma in inguinal hernias have occasionally been reported [7,8]. Neurofribrosarcoma may occur in three different contexts; associated with neurofibromatosis in about 50% of cases, sporadic in about 40% of cases, as a consequence of previous radiation in about 10% of cases [9]. The index case was not diagnosed of neurofibromatosis, didn�t have features of this disease at presentation and had never been exposed to radiation, and as such the tumour was most likely to be sporadic. Neurofibrosarcoma lacks specific clinical and imaging characteristics, making the diagnosis difficult [3]. These tumours, though can occur everywhere in the body, if they occur in the inguinal region they may present sometimes like an inguinal mass [8], making diagnosis and differentiation difficult from inguinal hernia especially by inexperience hands. Hernia is readily distinguished from inguinal masses by by its characteristics of reducibility, cough impulse and reproducibility. Most classical neurofibrosarcomas consist of tightly arranged spindle cells, which are often densely distributed around blood vessels in loose or mucoid areas; these spindle cells grow diffusely in rich intercellular areas that are interlaced with cell-sparse areas. The cytoplasm is lightly eosinophilic or dichroic [3]. The nuclei are darkly stained, irregular, and contain obvious mitotic figures. Approximately 1/3 of neurofibrosarcoma are composed of large cells with obvious pleomorphism and common multinucleated giant cells [3]. Due to the lack of morphologic specificity of tumour cells, it is difficult to distinguish them solely by microscopic features. Therefore, further diagnosis requires a combination of immunohistochemical staining and microscopy [5]. In one large series, a total of 159 patients with neurofibrosarcoma were enrolled in the study. The ratio of male to female was 1.04 to 1. The median age was 40 (range: 5-76) years at the time of diagnosis. The 3- and 5-year overall survival rates were 50.0% and 43.0%, respectively. The median follow-up period was 31.0 (range: 2.0-199.0) months [9]. This is consistent with our index reported case.
Neurofibrosarcomas are very aggressive peripheral nerve sheets tumours that present diagnostic as well as therapeutic challenges. There have variable localisations and clinical presentations. Their clinical presentation in the groin may mimic inguinal hernia. A high index of suspicion is therefore needed in the evaluation of all patients with groin masses to rule out all other causes which may not be related to hernia.
The authors declare no competing interests.
ASNM and PT conceived the manuscript; MLO, OA, LNO, JCF, FE, PJF, FA and MAS corrected the draft manuscript. All authors read and approved the final manuscript.
Figure 1: ulcerating and fungating groin mass at presentation following two repeated inguinal explorations by the primary care physician
Figure 2: showing groin after complete excision of the mass at Douala Laquintinie Hospital
Figure 3: cytology showing cells suggestive of neurofibrosarcoma
Figure 4: recurrence of the groin mass a month after excision at Douala Laquintinie Hospital
- do Amaral TL, Valiati R, de Andrade BAB, Rumayor Piña A, Torres SR, Romañach MJ et al. Malignant peripheral nerve sheath tumor of the lower labial mucosa: case report and literature review. Oral Surg Oral Med Oral Pathol Oral Radiol. 2016 Aug 1;122(2):e64-8. PubMed | Google Scholar
- Liu M, Liu S, Zhan J, Chen W, Yang P, Zhou H. Mixed malignant peripheral nerve sheath tumor in the inguinal region: a case report. Int J Clin Exp Pathol. 2020 Feb 1;13(2):261-5. PubMed | Google Scholar
- Du P, Zhu J, Zhang ZD, He C, Ye MY, Liu YX et al. Recurrent epithelioid malignant peripheral nerve sheath tumor with neurofibromatosis type 1: a case report and literature review. Oncol Lett. 2019 Sep;18(3):3072-80. PubMed | Google Scholar
- Jiwani S, Gokden M, Lindberg M, Ali S, Jeffus S. Fine-needle aspiration cytology of epithelioid malignant peripheral nerve sheath tumor: a case report and review of the literature. Diagn Cytopathol. 2016;44(3):226-31. PubMed | Google Scholar
- Durbin AD, Ki DH, He S, Look AT. Malignant Peripheral Nerve Sheath Tumors. Adv Exp Med Biol. 2016;916:495-530. PubMed | Google Scholar
- The EQUATOR Network. The CARE guidelines. consensus-based clinical case reporting guideline development. Accessed Dec 13, 2018.
- Qin R, Zhang Q, Weng J, Pu Y. Incidental finding of a malignant tumour in an inguinal hernia sac. Contemp Oncol. 2014;18(2):130-3. PubMed | Google Scholar
- Li F, Tian R, Yin C, Dai X, Wang H, Xu N et al. Liposarcoma of the spermatic cord mimicking a left inguinal hernia: a case report and literature review. World J Surg Oncol. 2013 Jan 25;11:18. PubMed | Google Scholar
- Yuan Z, Xu L, Zhao Z, Xu S, Zhang X, Liu T et al. Clinicopathological features and prognosis of malignant peripheral nerve sheath tumor: a retrospective study of 159 cases from 1999 to 2016. Oncotarget. 2017 Jul 4;8(62):104785-95. PubMed | Google Scholar