Thyroid psychosis in a young male: an unusual presentation of Graves' disease (a case report)
Herta Babasoronoung Kankpeyeng, Davidson Iroko, Eugene Dordoye, Narkwor Narteh, Yaw Asante Awuku
Corresponding author: Herta Babasoronoung Kankpeyeng, Department of Medicine, Ho Teaching Hospital, Ho, Ghana 
Received: 07 Apr 2021 - Accepted: 06 Jun 2022 - Published: 08 Jun 2022
Domain: Internal medicine
Keywords: Thyroid, psychosis, male, Graves' disease, case report
©Herta Babasoronoung Kankpeyeng et al. PAMJ Clinical Medicine (ISSN: 2707-2797). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Herta Babasoronoung Kankpeyeng et al. Thyroid psychosis in a young male: an unusual presentation of Graves' disease (a case report). PAMJ Clinical Medicine. 2022;9:9. [doi: 10.11604/pamj-cm.2022.9.9.29242]
Available online at: https://www.clinical-medicine.panafrican-med-journal.com//content/article/9/9/full
Case report 
Thyroid psychosis in a young male: an unusual presentation of Graves' disease (a case report)
Thyroid psychosis in a young male: an unusual presentation of Graves' disease (a case report)
![]() Herta Babasoronoung Kankpeyeng1,&,
Herta Babasoronoung Kankpeyeng1,&, ![]() Davidson Iroko1,2,
Davidson Iroko1,2, ![]() Eugene Dordoye1,3, Narkwor Narteh4, Yaw Asante Awuku1,5
Eugene Dordoye1,3, Narkwor Narteh4, Yaw Asante Awuku1,5
&Corresponding author
Thyroid psychosis is a rare presentation of hyperthyroidism and, like other thyroid disorders, is uncommon among males. It can be life-threatening if prompt diagnosis and treatment are delayed. We report a case of thyroid psychosis in a young male who presented with: insomnia, talking to self with delusions of persecution, and excessive sweating. He was initially misdiagnosed with a psychiatric disorder. There was no improvement on treatment until a diagnosis of hyperthyroidism was made and managed accordingly. As demonstrated in this report, thyrotoxicosis presenting with psychosis, especially in males, can be missed at presentation. This report seeks to create awareness of the disease and how it can mimic psychiatric disorders.
Thyrotoxicosis is the clinical manifestation of increased levels of thyroid hormones in the body. Patients commonly show symptoms of sympathetic activation, gastrointestinal, cardiovascular and eye signs (especially in Graves´ disease). Graves´ disease which is the commonest cause of hyperthyroidism is an autoimmune disorder in which autoantibodies stimulate thyroid-stimulating hormone receptors, leading to increased thyroid hormones [1]. This condition is associated with more marked clinical symptoms compared to other causes. Psychosis is an extreme manifestation of thyrotoxicosis. Though rare, it can be life-threatening if medical treatment is delayed [2]. We report a case of thyroid psychosis in a young male who was initially misdiagnosed with manic episode of a bipolar affective disorder.
Patient information: a 26-year-old male with an unremarkable medical history, presented to the Ho Teaching Hospital emergency room as a referral from the psychiatric department (was being managed for a manic episode of a bipolar affective disorder to exclude hyperthyroidism) with complaints of insomnia, excessive sweating and reports of abnormal behavior (talking to self with delusions of persecution) of 4 months´ duration. These were associated with polyphagia, weight loss, heat intolerance, palpitations and headaches. He had no family history of psychiatric disease and was unemployed. Prior to the presentation, he had visited a few clinics and was being managed for a psychiatric disorder on an outpatient basis. However, no improvement was noticed in his symptoms despite being on treatment with olanzapine and carbamazepine.
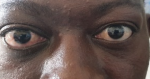
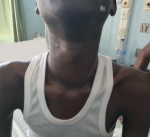
Clinical findings: on examination, the patient was moderately wasted and had a diffuse anterior neck swelling (moved with swallowing with well-defined edges, non-tender, and no differential warmth), bilateral exophthalmos (Figure 1, Figure 2) and fine tremors. He was tachycardic (125 beats per minute), his temperature was 37.2 degrees celsius, respiratory rate was 24 cycles per minute, and he recorded blood pressure of 120/70 mmHg. He was noticed to be in an elated mood, exhibiting over-familiarity and laughing factitiously. There were disturbances in behavior, speech and thought in his mental state exam. He was talking excessively, although he maintained eye contact and his speech was occasionally irrelevant and incoherent with an increased volume and rate. His thought form was consistent with flight of ideas, and his content revealed delusions of paranoia and persecution.
Diagnostic assessment: an electrocardiogram revealed sinus tachycardia and a thyroid ultrasound showed a diffuse hyper vascular thyroid. Thyroid function tests (Thyroid-stimulating hormone (TSH), free thyroxine (FT4), free triiodothyronine (FT3)), TSH Receptor antibodies (TSHR-Ab) and thyroglobulin antibodies tests were conducted and results are shown in Table 1. A diagnosis of thyroid psychosis in a patient with Graves´ disease was made and a treatment plan instituted.
Therapeutic intervention: a multidisciplinary approach involving medical, psychiatric and ophthalmology departments was key to treatment success. Patient was admitted, and pharmacological therapy started with oral Carbimazole 20�mg 12 hourly, oral propranolol 40�mg 8 hourly, intravenous hydrocortisone (200�mg stat, 100�mg 8 hourly for 3 days) and amlodipine 10�mg daily (started on day 3 following persistently recorded high blood pressures). The dosages were tapered down according to clinical response. On the sixth day of admission, the patient recorded a temperature spike of 38°C. He was screened and treated for malaria following a positive rapid diagnostic test for malaria. After one week of instituting treatment, patient´s psychosis had resolved and there was a marked improvement in other symptoms.
Follow-up and outcomes: patient was discharged home with a scheduled review with repeat thyroid function and full blood count tests on an outpatient basis. Two months into his treatment, the patient reported resolution of most symptoms except exophthalmos which appeared to have worsened. The laboratory findings on follow-up are seen in Table 1. Oral prednisolone (starting at 40�mg daily) was added to his treatment and was slowly tapered off following an improvement in eye signs. He is currently on a maintenance dose of 5�mg daily Carbimazole and doing well.
Patient perspective: "I am happy I can sleep at night like everyone else now. My mother used to worry a lot about me, but she is happy now. I am happy she brought me to the hospital for treatment because I feel much better, and I am grateful to everyone who played a role to get me back to being myself".
Informed consent: written informed consent was obtained from the patient for the publication of this case report, including photographs taken. A copy of the written consent is available for review by the Editor-In-Chief of the journal.
There are few reports of thyrotoxicosis and its life-threatening complication of thyroid psychosis occurring in young males between 20 and 40 years, like in our patient. Current statistics of Graves´ disease show up to 88% of affected patients are females [3]. Studies in Ghana and Nigeria have shown similar results, with 83.5% and 86% of patients being female respectively [4,5]. Many patients improved with the introduction of drug therapy with only a few requiring more advanced treatment options [6]. In the case of our patient, his response to medical treatment was prompt with no complications. There are reports of patients who required plasmapheresis as part of management because no improvement was observed with drug therapy [7]. The use of steroids in Graves´ ophthalmopathy is controversial, although some literature shows good response to eye signs [8,9]. In the context of our patient, his response was remarkable. This case is peculiar and worth reporting, since most reported cases of thyroid psychosis in the literature occur in females, with only a few documented male cases. Furthermore, it creates awareness of the incidence of thyrotoxicosis among men and therefore heightens our index of clinical suspicion when dealing with male patients who may have similar symptoms or may have been misdiagnosed as having psychiatric disorders.
Thyrotoxicosis presenting with psychosis can mimic psychiatric disorders and pose a diagnostic challenge to clinicians. Male patients presenting with thyrotoxicosis are uncommon, but a high index of suspicion will be required to make a diagnosis.
The authors declare no competing interests.
Patient management: DI, ED, HBK, NN and YAA. Data collection: HBK. Manuscript drafting: HBK. Manuscript revision: DI, HBK and YAA. All authors read and approved the final version of the manuscript.
We acknowledge the contribution of staff of the Department of Medicine at Ho Teaching Hospital.
Table 1: thyroid function profile of patient at diagnosis and follow-up
Figure 1: bilateral exophthalmos
Figure 2: diffuse anterior neck swelling
- Kumar P, Clark M. Kumar and Clark´s Clinical Medicine - 9th edition, London. Elsevier. 2016.
- Sarlis NJ, Gourgiotis L. Thyroid emergencies. Rev Endocr Metab Disord. 2003;4(2):129-136. PubMed | Google Scholar
- Medscape. How does the prevalence of Grave's disease vary by sex? 2020. Accessed April 17, 2021.
- Sarfo-Kantanka O, Sarfo FS, Ansah EO, Kyei I. Grave's disease in central Ghana: clinical characteristics and associated factors. Clin Med Insights Endocrinol Diabetes. 2018;11:1-7. PubMed | Google Scholar
- Okafor EN, Ugonabo MC, Chukwukelu EE, Okonkwo IN, Ezigbo E, Odurukwe O. Prevalence and pattern of thyroid disorders among patients attending University of Nigeria Teaching Hospital, Enugu, Southeastern Nigeria. Niger Med J. 2019; 60(2):62-67. PubMed | Google Scholar
- Ross DS, Burch HB, Cooper DS, Greenlee MC, Laurberg P, Maia AL et al. 2016 American thyroid association guidelines for diagnosis and management of hyperthyroidism and other causes of thyrotoxicosis. Thyroid. 2016; 26(10):1343-1421. PubMed | Google Scholar
- Desai D, Zahedpour AS, Reddy N, Epstein E, Tabatabaie V. Thyroid storm presenting as psychosis. J Investig Med High Impact Case Reports. 2018;6:0-4. PubMed | Google Scholar
- Penta L, Muzi G, Cofini M, Leonardi A, Lanciotti L, Esposito S. Corticosteroids in moderate-to-severe Graves´ ophthalmopathy: oral or intravenous therapy? Int J Environ Res Public Heal. 2019;16(1):155. PubMed | Google Scholar
- Yang DD, Gonzalez MO, Durairaj VD. Medical management of thyroid eye disease. Saudi J Ophthalmol. 2011;25(1):3-13. PubMed | Google Scholar