Esophageal motility disorders in systemic sclerosis
Sara Ghani, Ilham Serraj, Mouna Salihoun, Mohamed Acharki, Nawal Kabbaj
Corresponding author: Sara Ghani, EFD-Hepatogastroenterology Unit, Ibn Sina Hospital, Mohammed V University of Rabat, Rabat, Morocco 
Received: 22 Feb 2020 - Accepted: 05 Mar 2020 - Published: 13 Mar 2020
Domain: Gastroenterology
Keywords: Esophageal dysmotility, dysphagia, scleroderma, high-resolution manometry
©Sara Ghani et al. PAMJ Clinical Medicine (ISSN: 2707-2797). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Sara Ghani et al. Esophageal motility disorders in systemic sclerosis. PAMJ Clinical Medicine. 2020;2:108. [doi: 10.11604/pamj-cm.2020.2.108.21950]
Available online at: https://www.clinical-medicine.panafrican-med-journal.com//content/article/2/108/full
Esophageal motility disorders in systemic sclerosis
Sara Ghani1,&, Ilham Serraj1, Mouna Salihoun1, Mohamed Acharki1, Nawal Kabbaj1
1EFD-Hepatogastroenterology Unit, Ibn Sina Hospital, Mohammed V University of Rabat, Rabat, Morocco
&Corresponding author
Sara Ghani, EFD-Hepatogastroenterology Unit, Ibn Sina Hospital, Mohammed V University of Rabat, Rabat, Morocco
Systemic sclerosis is an autoimmune disease characterized by vasculopathy and tissue fibrosis. Esophageal disorders are often associated. The diagnosis is confirmed and characterized by high-resolution esophageal manometry (HRM). This study aims to describe the esophageal motility disorders found by high-resolution esophageal manometry, in patients followed for systemic sclerosis. An observational study carried out between April 2018 and January 2020, including 23 patients with systemic sclerosis according to EULAR/ACR 2013 criteria, referred for high-resolution esophageal manometry. We used the Chicago V3.0 classification to order esophageal motor disorders into two categories: major and minor disorders of peristalsis. Four parameters were analyzed: lower esophageal sphincter resting pressure (LES), distal latency (DL) and distal contractile integral (DCI) and integrated relaxation pressure (IRP). IRP was normal in all cases. The digestive symptoms were: gastroesophageal reflux in 10 cases (43.4%) and dysphagia in 6 cases (26.2%). Seven patients were asymptomatic (30.4%). HRM revealed a major disorder of esophageal peristalsis in 14 cases (60.9%), minor disorders in 4 patients (17.4%) and was normal in 5 cases (21.7%). There was; hypotonia of the lower esophageal sphincter (LES) with absent contractility in 8 cases (44.5%), only absence of contractility in 6 cases (33.3%), hypotonia of the lower esophageal sphincter (LES) with ineffective motility in 4 cases (22.2%). High-resolution esophageal manometry should be considered in all patients with systemic sclerosis even in the absence of digestive symptoms. In our series, motility disorders were present in 78.3% of cases.
Systemic sclerosis (SSc) is a rare autoimmune disease associated with vasculopathy and tissue fibrosis of unknown origin [1]. No specific prevalence data have been identified in the literature [2]. The digestive tract is most often involved. The common symptoms related to esophagus involvement are dysphagia and gastroesophageal reflux disease (GERD) [3]. Diagnosis and assessment are performed by high-resolution esophageal manometry (HRM). This study aims to describe the esophageal motility disorders classified by high-resolution esophageal manometry in patients followed for SSc.
An observational study carried out between April 2018 and January 2020, including 23 patients with SSc according to EULAR/ACR 2013 criteria, referred for high-resolution esophageal manometry. Upper endoscopy with esophagus biopsies were done in all patients with dysphagia. We use a probe with 36 sensors, MMS 9.5. According to the Chicago classification (v3.0), esophageal motor disorders have been classified as major and minor disorders of peristalsis. Four parameters were analyzed: lower esophageal sphincter resting pressure (LES), distal latency (DL) and distal contractile integral (DCI) and integrated relaxation pressure (IRP). IRP was normal in all cases. Ineffective motility syndrome was defined if ≥ 50% of swallows are ineffective with DCI < 450 mmHg.s.cm, and absent peristalsis was defined as normal LES relaxation and total absence of contractility DCI < 100 mmHg.s.cm. The data analysis was performed using Microsoft Excel.
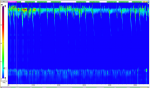
Among 200 high-resolution manometries performed during this period, 23 patients (11.5%) were included in the current study. The mean age was 50.6 years +/- 11.8. There were 21 women (91.3%) and 2 men (8.7%). The digestive symptoms were: GERD in 10 cases (43.4%) and dysphagia in 6 cases (26.2%). Seven patients (30.4%) were asymptomatic. HRM revealed a major disorder of esophageal peristalsis in 14 cases (60.9%), minor disorders in 4 patients (17.4%) and was normal in 5 cases (21.7%). The manometry results were absent peristalsis with hypotonia of the LES in 8 cases (44.5%) (called scleroderma esophagus), absent peristalsis in 6 cases (33.3%) and ineffective motility syndrome with hypotonia of the LES in 4 cases (22.2%) (Figure 1).
Incidence and symptoms of esophageal disorders in patients followed for SSc: esophageal disorders are the most frequent during sclerosis. Its incidence is estimated to be between 40% and 80%, even in asymptomatic patients. The patients usually report 2 types of symptoms; GERD and dysphagia [4]. Several studies have shown a strong correlation between severe esophageal dysfunction and extensive skin disease in patients followed for SSc [3].
Diagnosis
High-resolution manometry (HRM): HRM is the gold standard for diagnosing and assessing esophageal dysfunction. It measures the pressure of the whole esophagus and of the LES. The Chicago classification is used to interpret the manometric results and to facilitate the classification of esophageal motility disorders. Typical manometry findings are absence contractility, ineffective esophageal motility and/or hypotonia of LES, it found up to 75%-80% [4]. Ogliari et al. showed in their study, that 56% of the patients had absent contractility, 10% had infective esophageal motility and 26% had normal motility on HRM [5]. Asymptomatic patients with aperistalsis or ineffective motor syndrome will be more likely to develop esophageal symptoms [6].
Endoscopy: upper endoscopy is performed before HRM to identify the causes of dysphagia and the complications of GERD, such as esophagitis, esophageal stenosis, Barrett´s esophagus and to take a biopsy [4].
Treatment: there is no specific treatment available for esophageal motility disorders. In general, the treatment of symptomatic patients is based first on lifestyle modifications. For GERD, proton-pomp inhibitors (PPIs) are the gold standard. Previous studies showed that PPI alone was not effective and the addition of domperidone and/or alginic acid seems necessary to have a good response [7]. For refractory GERD, no specific therapies are available [4]. Patients with abnormal motility, several molecules have been studied; such as buspirone (a serotonin receptor agonist), pyridostigmine (an acetylcholinesterase inhibitor) and bethanechol (parasympathomimetic choline carbamate), with a short-term effect. Currently, no specific prokinetic treatment has been proven to be effective in patients with esophageal dysmotility [6].
High-resolution esophageal manometry should be considered in all patients with systemic sclerosis even in the absence of digestive symptoms. In our series, motility disorders were present in 78.3% of cases and 60.9% of them were classified as major disorders of peristalsis according to Chicago classification V3.0.
What is known about this topic
- The digestive tract is mostly involved in systemic sclerosis;
- The esophageal symptoms are GERD and dysphagia;
- The is no specific treatment.
What this study adds
- High-resolution esophageal manometry should be performed in all patients followed for systemic sclerosis even in the absence of symptoms;
- The frequency of scleroderma esophagus in asymptomatic patients.
The authors declare no competing interests.
All the authors have read and agreed to the final manuscript.
Figure 1: HRM showing absent peristalsis with hypotonia of the LES (scleroderma esophagus)
- Pattanaik D, Brown M, Postlethwaite BC, Postlethwaite AE. Pathogenesis of systemic sclerosis. Front Immunol. 2015 Jun 8;6:272. PubMed | Google Scholar
- Bergamasco A, Hartmann N, Wallace L, Verpillat P. Epidemiology of systemic sclerosis and systemic sclerosis-associated interstitial lung disease. CLEP. 2019 Apr;11:257-73. PubMed | Google Scholar
- Kimmel JN, Carlson DA, Hinchcliff M, Carns MA, Aren KA, Lee J et al. The association between systemic sclerosis disease manifestations and esophageal high-resolution manometry parameters. Neurogastroenterol Motil. 2016 Aug;28(8):1157-65. PubMed | Google Scholar
- Denaxas K, Ladas SD, Karamanolis GP. Evaluation and management of esophageal manifestations in systemic sclerosis. Ann Gastroenterol. 2018;31(2):165-170. PubMed | Google Scholar
- Ogliari C, Piazza O Sed N, Vecchi M. High resolution manometry in scleroderma patients. Clinical Gastroenterology and Hepatology. 2017 Oct;15(10):1640-1. PubMed | Google Scholar
- Leandri C, Guillaumot M-A, Dohan A, Leconte M, Coriat R, Chaussade S et al. Le syndrome de motricité œsophagienne inefficace. La Presse Médicale. 2019 Sep;48(9):897-903. PubMed | Google Scholar
- Foocharoen C, Chunlertrith K, Mairiang P, Mahakkanukrauh A, Suwannaroj S, Namvijit S et al. Effectiveness of add-on therapy with domperidone vs alginic acid in proton pump inhibitor partial response gastro-oesophageal reflux disease in systemic sclerosis: randomized placebo-controlled trial. Rheumatology. 2017 Feb;56(2) :214-22. PubMed | Google Scholar