Refractory grade III atopic dermatitis of the extremities in a post-menopausal female
Aditi Satish Telrandhe, Anita Santoshrao Wanjari
Corresponding author: Anita Santoshrao Wanjari, Department of Rasashastra Evam Bhaishajya Kalpana, Mahatma Gandhi Ayurveda Collage Hospital and Research Center, Datta Meghe Institute of Higher Education and Research Salod (H) Wardha, Maharashtra, India 
Received: 08 Oct 2025 - Accepted: 06 Feb 2026 - Published: 25 Mar 2026
Domain: Dermatology
Keywords: Atopic dermatitis, chronic eczema, post-menopausal female
Funding: This work received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
©Aditi Satish Telrandhe et al. PAMJ Clinical Medicine (ISSN: 2707-2797). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Aditi Satish Telrandhe et al. Refractory grade III atopic dermatitis of the extremities in a post-menopausal female. PAMJ Clinical Medicine. 2026;20:17. [doi: 10.11604/pamj-cm.2026.20.17.49691]
Available online at: https://www.clinical-medicine.panafrican-med-journal.com//content/article/20/17/full
Images in clinical medicine 
Refractory grade III atopic dermatitis of the extremities in a post-menopausal female
Refractory grade III atopic dermatitis of the extremities in a post-menopausal female
&Corresponding author
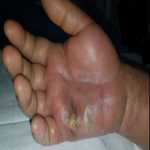
A 50-year-old post-menopausal female presented to the Dermatology Outpatient Clinic with a three-year history of intensely pruritic, erythematous, and scaly plaques symmetrically involving the left ankle joint and right foot. The lesions were associated with severe nocturnal pruritus, leading to scratching, excoriation, and occasional bleeding. The condition worsened during cold weather, after consumption of spicy or acidic foods, and during emotional stress. She had a history of prior treatment with topical corticosteroids, which provided only temporary relief with recurrence within one month of discontinuation. On examination, multiple well-defined erythematous plaques with scaling, crusting, and excoriation were noted, along with areas of post-inflammatory hyperpigmentation. Based on the clinical presentation and severity, the case was graded as EASI Grade III (severe). A final diagnosis of chronic eczema (atopic dermatitis) was established. Severe eczema requires an individualized management approach focusing on skin barrier restoration and inflammation control. In the present case, the patient was managed with a combination of systemic and topical therapy. She was prescribed a super-bioavailable formulation of itraconazole 130 mg once daily for two weeks, along with cetirizine 10 mg at bedtime for symptomatic relief of pruritus, while a gastro-resistant pantoprazole tablet was co-administered once daily during the treatment period for gastric protection. Topically, Topisal-MF 3% ointment was applied twice daily to reduce inflammation and scaling, and Emax ointment twice daily to restore skin hydration and barrier function. The patient was advised to avoid triggering factors and maintain proper skin care. On follow-up after two weeks, significant improvement in itching, erythema and scaling was observed.
Figure 1: A,B) itchy, erythematous, scaly lesions near left ankle joint; C) itchy, erythematous, scaly lesions on right foot