Nose-blowing associated lamina papyracea fracture and orbital emphysema mimicking orbital cellulitis in an 11-year-old boy: a case report
Jonathan Timothy Oettlé
Corresponding author: Jonathan Timothy Oettlé, University of Cape Town, Department of Surgery, Division of Ophthalmology, Groote Schuur Hospital, Cape Town, South Africa 
Received: 30 Jul 2025 - Accepted: 08 Dec 2025 - Published: 11 Feb 2026
Domain: Infectious disease,Ophthalmology,Otolaryngology (ENT)
Keywords: Orbital emphysema, orbital cellulitis, nose blowing, paediatric, case report
Funding: This work received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
©Jonathan Timothy Oettlé et al. PAMJ Clinical Medicine (ISSN: 2707-2797). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Jonathan Timothy Oettlé et al. Nose-blowing associated lamina papyracea fracture and orbital emphysema mimicking orbital cellulitis in an 11-year-old boy: a case report. PAMJ Clinical Medicine. 2026;20:3. [doi: 10.11604/pamj-cm.2026.20.3.48812]
Available online at: https://www.clinical-medicine.panafrican-med-journal.com//content/article/20/3/full
Case report 
Nose-blowing associated lamina papyracea fracture and orbital emphysema mimicking orbital cellulitis in an 11-year-old boy: a case report
Nose-blowing associated lamina papyracea fracture and orbital emphysema mimicking orbital cellulitis in an 11-year-old boy: a case report
&Corresponding author
Air in the orbital space, known as orbital emphysema, is usually seen in the setting of trauma but may occur spontaneously when air is forced through a defect in the lamina papyracea. We describe an 11-year-old boy who presented with acute atraumatic periorbital swelling and was initially treated as having orbital cellulitis. Computed tomography imaging revealed a lamina papyracea fracture with orbital emphysema, and focused history-taking subsequently identified an episode of nose blowing as the cause. He was managed conservatively with full resolution. This case emphasises that orbital emphysema can occur in children without overt trauma and highlights the importance of a targeted history and early imaging to avoid misdiagnosis.
Lamina papyracea fractures with secondary orbital emphysema following nose blowing are uncommon but well-recognised phenomena [1]. Positive-pressure barotrauma within the paranasal sinuses can force air through a defect in the medial orbital wall, producing acute orbital signs that may resemble infection or inflammation [2]. The lamina papyracea is the thinnest and most fragile component of the orbital wall, making it particularly vulnerable to such pressure-related injury [3]. Forceful nose blowing can generate a sudden pressure gradient between the nasal cavity and orbit, resulting in fracture of the medial wall or orbital floor and subsequent insufflation of air into the orbit [4]. Although typically described in adults, these presentations can occur in children, in whom the clinical history may be less reliable and the condition easily mistaken for orbital cellulitis [2]. We report a case of an atraumatic lamina papyracea fracture from nose blowing, the second paediatric and first South African case reported.
Patient information: an 11-year-old boy presented to our tertiary-level paediatric ophthalmology clinic via the emergency department with a one-day history of a painful, swollen right eye. His caregiver reported a preceding upper respiratory tract infection with rhinorrhoea, and denied any history of trauma. The child had a history of allergic rhinitis and asthma, but was not receiving treatment. Previous sinusitis was noted, but there were no other significant medical, surgical, or family histories. He was born via normal vertex delivery at term, was up to date with immunisations, developmentally normal, and not allergic to any medications. On initial presentation, signs and symptoms closely resembled orbital cellulitis. Empirical treatment for orbital cellulitis was initiated pending clinical progression and imaging results.
Clinical findings: vital signs were within normal limits: respiratory rate 14/min, pulse 93 bpm, temperature 36.7°C, oxygen saturation 100%. He weighed 35.4 kg and was 148 cm tall. He was alert, with a Glasgow Coma Score of 15. Visual acuity was 6/18 in the right eye and 6/6 in the left eye (Snellen chart, 6 metres). Examination revealed marked periorbital swelling, 8 mm proptosis, chemosis, and a -1 limitation in abduction and depression, with associated pain on attempted abduction. There was no relative afferent pupillary defect. Anterior and posterior segment examinations were unremarkable in both eyes. The cup-to-disc ratio was 0.3 bilaterally, with no disc oedema or retinal folds in either eye. Intraocular pressure was raised to 29 mmHg in the right eye.
Timeline: the patient was admitted on August 7, 2024 via the eye clinic with a working diagnosis of orbital cellulitis. A CT scan was ordered, and an ENT consultation was requested. The following day, 8 August, review of the imaging revealed surgical emphysema and a lamina papyracea fracture. The patient improved with conservative management and was discharged on oral antibiotics on August 11, 2024, with outpatient follow-up arranged. At review on 23 August, there was complete resolution of swelling, vision had returned to baseline, and ocular motility was full and non-painful. A subsequent visit on October 18, 2024 confirmed that these findings remained stable. On December 11, 2024, the patient re-presented with mild periorbital swelling. A repeat CT scan was arranged, and on January 17, 2025, the uncontrasted scan demonstrated no abnormal findings. At a final follow-up on January 22, 2025, the swelling had fully resolved, and the patient was discharged with advice to return if symptoms recurred (Table 1).
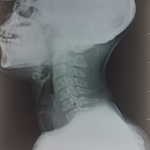
Diagnostic assessment: a CT scan on admission revealed a lamina papyracea fracture with associated orbital emphysema (Figure 1). Blood tests, conducted as part of the work-up for suspected orbital cellulitis, were unremarkable (Table 2). A repeat CT scan performed several months later showed complete resolution. There were no specific diagnostic challenges.
Diagnosis: the initial diagnosis of orbital cellulitis was called into question based on the results of the CT scan, which showed significant orbital emphysema communicating with the ethmoid sinus. On further questioning, a careful history revealed that periorbital swelling was sudden and immediately preceded by an unwitnessed episode of nose blowing in the school bathroom.
Therapeutic intervention: intravenous ceftriaxone (30 mg/kg once daily) and intravenous metronidazole (7 mg/kg every 8 hours) were initiated on admission. On day 5, IV antibiotics were switched to oral co-amoxiclav (30 mg/kg twice daily) for a total 10-day course. Nasal decongestants were prescribed, and the family was advised to avoid further nose blowing.
Follow up and outcome of interventions: visual acuity returned to baseline within two weeks. The abduction deficit, proptosis, chemosis, and pain resolved. Figure 2 shows the progression of periorbital swelling. The patient re-presented on December 11, 2024 with intermittent swelling. Examination revealed a 4 mm proptosis with full extraocular motility. A CT scan on January 17, 2025 showed complete resolution. At follow-up on January 22, 2025, proptosis had resolved, ocular motility was normal, and visual acuity was 6/6 in both eyes. There were no concerns regarding adherence or tolerability. No adverse or unanticipated events occurred. The family was advised to return if new symptoms developed.
Patient perspective: “I was very happy with the treatment my son received, and he got better quickly” - MM, his father.
Informed consent and ethics clearance: written informed consent was obtained from the patient's caregiver, and ethical clearance to conduct the study was obtained from the Human Resource Ethics Committee at the University of Cape Town, with HREC Ref: 225/2025.
Orbital fractures secondary to nose blowing are rare, with the first case described by Oluwole and White in 1996 in an elderly patient. To date, 29 cases have been reported in the English-language literature, excluding those with preceding trauma or incidental findings such as osteomas [4]. The medial wall, orbital floor, and inferomedial wall are the thinnest components of the orbit and therefore most susceptible to barotrauma-related injury. All published cases of orbital fracture following nose blowing have involved the medial or inferior orbital wall [1,4], consistent with the anatomical vulnerability of these regions.
Reported clinical features vary, but a review of the first 18 cases by Komro et al. demonstrated pain in 7/18, reduced vision in 2/18, elevated intraocular pressure in 1/18, and restricted extraocular motility in 2/18 [1]. Our patient demonstrated all four features; the first reported case with this full spectrum of findings. Recognised risk factors include previous trauma or surgery, mucosal inflammation (such as sinusitis or rhinitis), smoking, older age, and episodes of forceful nose blowing [1-4]. In our case, the only identifiable risk factor was a history of sinusitis, with no prior trauma, surgical history, smoking exposure, or unusually forceful nose blowing.
The average age of affected patients in the literature is 45.2 years [1]. Only one paediatric case-a similarly aged 11-year-old girl-has been previously reported, and she too was initially misdiagnosed with orbital cellulitis [2]. Our patient is the second paediatric and first South African case described. It is also the first reported case without a predisposing lesion to show documented recurrence: 4 mm of proptosis was noted on follow-up examination on 11th December, which had resolved by the time repeat CT imaging was performed in January. A single prior recurrence has been described in a patient with a frontal sinus osteoma requiring surgical excision [5].
The initial presentation strongly suggested orbital cellulitis secondary to sinusitis, a common and potentially life-threatening condition in our setting. Given the risk of morbidity from delayed treatment of orbital cellulitis, empirical intravenous antibiotics and urgent imaging were appropriate. This case highlights the importance of thorough history-taking and early imaging-particularly CT-in situations where symptoms are atypical, the mechanism is unclear, or the clinical course does not fit the expected pattern for infection.
Strengths of this case include a cooperative patient and family, early access to imaging, and the prompt initiation of intravenous antibiotics in the context of diagnostic uncertainty. Limitations include the initial misdiagnosis due to incomplete early history and the lack of routine access to MRI, resulting in reliance on CT imaging and its associated radiation exposure.
This case describes an 11-year-old boy who developed orbital emphysema from a lamina papyracea fracture following forceful nose blowing, initially misdiagnosed as orbital cellulitis. It highlights that non-traumatic orbital emphysema can occur in children and may closely mimic infectious orbital disease, leading to incorrect treatment if not recognised. Careful history-taking and early imaging are essential when clinical features are atypical, and clinicians should remain aware of barotrauma-related orbital injuries as a possible, though uncommon, mimic of infection.
The authors declare no competing interests.
Patient management: Jonathan Timothy Oettlé. Data collection: Jonathan Timothy Oettlé. Manuscript drafting: Jonathan Timothy Oettlé. Manuscript revision: Jonathan Timothy Oettlé. The author have read and approved the final version of this manuscript.
Table 1: timeline of events
Table 2: blood results
Figure 1: computerised tomography scans of the orbit legend: axial (A) and coronal (B) images demonstrate a defect in the lamina papyracea (arrows) with air communication between the orbit and ethmoid sinuses
Figure 2: facial photographs legend: progression of orbital swelling: day 1 (A), day 3 (B), day 4 (C) and at 5 months (D)
- Komro JJ, Williams PJ, Lin DJ. Orbital defect and emphysema after nose blowing: a case report and literature review. Cureus. 2022 Dec 26;14(12):e32958. PubMed | Google Scholar
- Aubin-Lemay C, Acar P, Alnaif N, Alamri A, Azzi AJ, Cugno S. Orbital subcutaneous emphysema in a child. J Craniofac Surg. 2013 May;24(3):703-7. PubMed | Google Scholar
- Shin JW, Lim JS, Yoo G, Byeon JH. An analysis of pure blowout fractures and associated ocular symptoms. J Craniofac Surg. 2013 May;24(3):703-7. PubMed | Google Scholar
- Salar S, Edafe. A case report and systematic review of periorbital emphysema following nose blowing or sneezing. The Annals of The Royal College of Surgeons of England. 2025 Apr 21;107(4):295-9. PubMed | Google Scholar
- Jack LS, Smith TL, Ng JD. Frontal sinus osteoma presenting with orbital emphysema. Ophthalmic Plast Reconstr Surg. 2009 Mar-Apr;25(2):155-7. PubMed | Google Scholar