The ultrasound-guided anterior trans-axillary approach to the infraclavicular brachial plexus block for postoperative analgesia of a fracture in the forearm: a case report
Okitolela Scotty Tambwe, Blaise Bayingana
Corresponding author: Okitolela Scotty Tambwe, Department of Anaesthesia, Charlotte Maxeke Johannesburg Academic Hospital, University of the Witwatersrand, Johannesburg, South Africa 
Received: 03 Feb 2026 - Accepted: 10 Feb 2026 - Published: 17 Feb 2026
Domain: Health emergencies
Keywords: UG-ATAXIC, analgesia, sensory block, infraclavicular brachial plexus, Case report
Funding: This work received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
©Okitolela Scotty Tambwe et al. PAMJ Clinical Medicine (ISSN: 2707-2797). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Okitolela Scotty Tambwe et al. The ultrasound-guided anterior trans-axillary approach to the infraclavicular brachial plexus block for postoperative analgesia of a fracture in the forearm: a case report. PAMJ Clinical Medicine. 2026;20:8. [doi: 10.11604/pamj-cm.2026.20.8.51438]
Available online at: https://www.clinical-medicine.panafrican-med-journal.com//content/article/20/8/full
Case report 
The ultrasound-guided anterior trans-axillary approach to the infraclavicular brachial plexus block for postoperative analgesia of a fracture in the forearm: a case report
The ultrasound-guided anterior trans-axillary approach to the infraclavicular brachial plexus block for postoperative analgesia of a fracture in the forearm: a case report
&Corresponding author
We are describing the ultrasound-guided trans-axillary approach to the infraclavicular block (UG-ATAXIC) as an innovative approach, through the anteromedial walls of the axillary region, to provide motor and sensory blocks for postoperative analgesia in surgical procedures involving the mid-humerus, elbow, the forearm, and hand. This approach is another variant and potential alternative to the existing and described approaches to the infraclavicular brachial plexus block.
The ultrasound-guided trans-axillary approach to the infraclavicular block (UG-ATAXIC) is, in fact, a 180° ultrasound probe rotation displaying a reverse view of the described coracoid approach aiming to improve visualisation and access to the brachial plexus at the level of the infraclavicular region. The UG-ATAXIC allows efficient block needle pass and manipulation to reach individually the three cords of the brachial plexus surrounding the axillary artery namely the medial, the lateral and posterior cords thereby optimising block coverage and effectiveness.
Patient´s information:this is a 28-year-old male, classified as ASA 2 and weighing approximately 75 kg, who presented for an open reduction and internal fixation (ORIF) of a left distal radial fracture. Patient sustained multiple gunshot wounds affecting the left forearm, scalp, and right infraorbital region and came with a GCS of 15/15. He reported no comorbidities, no allergies, nor prior surgical history. Patient was a bit anxious and had a history of occasional social alcohol use. This patient was admitted in hospital for two days from the time he sustained his multiple gunshot wounds, where appropriate investigations and internal referrals were arranged.
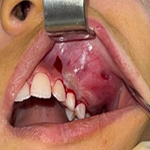
Clinical findings and assessments: clinical examination revealed no significant abnormalities or neurological deficits in the left upper limb. Patient had been nil by mouth for more than six hours and reported pain in the left upper limb, which was supported in a collar and cuff. The Airway assessment revealed some loose teeth and a moderately protruding but mildly swollen tongue. He also had a Mallampati grade 4 airway and slightly decreased inter-incisor distance, all indicators of a potentially difficult airway. A rapid sequence induction was planned to reduce aspiration risk and facilitate prompt airway management. After completing the airway evaluation and obtaining consent, patient was transferred to the operating theatre, where general anaesthesia with rapid sequence induction was performed without complication. The Cormack and Lehane laryngoscopy view was graded as 2.
Timeline: this patient was admitted in hospital for two days from the time he sustained his multiple gunshot wounds, where appropriate investigations and internal referrals were arranged. In the ward, routine nursing care was ongoing, and the patient was kept nil per mouth as a standing order in preparation for his general anaesthesia the day after his injuries. He, thereafter, was brought into the operating theatre on the second day for further orthopaedic management of his left distal radial fracture.
Therapeutic intervention: right after the intubation, the left upper arm was abducted up to an angle of 90° to facilitate a lateral and considerable superficial displacement of the neurovascular bundle within the infraclavicular fossa away from the lung field and chest wall, aiming to reduce the risk of potential pulmonary complications. Then, the left axillary area was aseptically cleaned with 0.5% Chlorhexidine gluconate and allowed to dry completely. A sterile gel was applied to the anterior aspect of the axillary region, and a high-frequency linear ultrasound probe was utilised. The probe was positioned in a plane perpendicular to the anteromedial margin of the axillary region, superior to the infraclavicular fossa, with the probe marker directed toward the operator and oriented laterally. To optimise imaging, various ultrasound probe manoeuvres, including sliding, sweeping, tilting, and rotation, were employed. The operator was seated in the space between the left thoracic cage and the abducted left arm, while the ultrasound machine was placed in the space between the left side of the head and the abducted left arm, just above the shoulder, to ensure optimal ergonomics and visualisation.
Following sonographic identification of the anatomical structures within the infraclavicular fossa, including subcutaneous tissues, the pectoralis major and minor muscles, and the neurovascular bundles, an insulated 21-gauge, 100 mm Stimuplex®A needle was advanced using an in-plane approach under ultrasound guidance at angles up to 45° (Figure 1) and through the pectoralis muscles, targeting the space between the axillary vein and artery (Figure 2). Real-time visualisation of the needle shaft and tip was maintained, with initial advancement directed toward the medial cord of the brachial plexus. A 10 mL syringe containing 0.25% bupivacaine with adrenaline was attached and flushed. The first 5 mL of local anaesthetic was administered without resistance near the medial cord (Figure 2), and its spread was observed surrounding the medial cord and displacing cephalad the axillary. The injection effectively increased the distance between the artery and vein, facilitating needle repositioning and pass towards the posterior cord, where 10 mL of local anaesthetic was administered (Figure 3). Subsequently, the needle was redirected to reach and target the lateral cord (Figure 4), and the remaining 5 mL of local anaesthetic was deposited at this location, with satisfactory circumferential spread observed around the axillary artery. Throughout all needle insertions and repositioning, the assistant performed aspirations before each injection to minimise the risk of intraneural injection, vascular puncture, and systemic administration of the local anaesthetic. The intraoperative multimodal analgesic regimen of the patient included the following: Fentanyl 200 mcg IV administered during induction. Dexamethasone 8 mg IV given immediately after induction. Paracetamol infusion 1 g IV delivered following the regional block.
Further care and follow up: the surgical procedure lasted 75 minutes, with a total anaesthetic time estimated to be 135 minutes. A mid-forearm tourniquet was used, and vital signs remained stable throughout the anaesthesia period. Patient was extubated and then admitted to the post-anaesthetic care unit (PACU/Recovery room) for 15 minutes, during which the NRS score was recorded as 0, before being discharged back to the ward. Patient was monitored and followed up in the ward, and no additional analgesics were given for 12 hours postoperatively. The sensory block remained complete in the mid-arm, forearm, and hand during this period. The following VAS and NRS scores were recorded after the block: at 2 hours: NRS=0 (immediate postoperative period in the PACU); at 6 hours: NRS=0; VAS=0; at 12 hours: NRS=0; VAS=0.
Patient´s perspective: the patient was highly satisfied postoperatively because he was pain free for a long period of time after the surgery.
Informed consent: this case report was elaborated with the written consent of the patient, which can be provided upon request.
The UGATAXIC approach involves a 180° clockwise or anti-clockwise rotation of the ultrasound probe in the same plane relative to the described coracoid approach, with a needle insertion through the anteromedial aspect of the axillary region. Our finding indicates that, when abducting the arm at least 90� from the thoracic cage, the UG-ATAXIC approach offers clear visualisation of anatomical structures within the infraclavicular fossa. The abduction of the arm allows a reduction of the depth of the brachial plexus as demonstrated by Ruiz et al. [1] and, in this case, has allowed optimal needle angulations without posing challenges, as in the classic approach, of limited area between the clavicle and the ultrasound probe requiring steep angulation of the needle at the point of insertion as postulated by Scanaill et al. [2]. Because the UG-ATAXIC may provide better needle angulation, it can allow multiple needle redirections aiming to individually target each cord of the brachial plexus around the axillary artery and expedite the onset of action, facilitate adequate block coverage and thus, enhancing the overall effectiveness.
In that regard, Aytuluk et al. [3] demonstrated that when using the medial approach to the infraclavicular brachial plexus block and when comparing a single versus triple injections, there was no need for additional block in the triple injections group although the success rate did not differ. Finally, we acknowledge that anatomical variations may be encountered when performing this block in adults or paediatric populations as well as technical difficulties in obese patients, where the use of Ultrasound guidance is effective in identifying and overcoming those challenges. A study by Mian et al. [4] concluded that despite those variations, equivalently successful infraclavicular block could be potentially obtained while reducing the incidence of intravascular injections.
The UG-ATAXIC appears to be a reliable method to achieve effective postoperative analgesia in procedures involving areas distal to the mid-humerus, including the elbow, the forearm, and the hand. This report is limited to a single patient, thus comprehensive training and appropriate supervision are essential to minimise the risk of complications. Further studies are required to assess the efficacy, the effectiveness and reliability of the UG-ATAXIC compared to the other described ultrasound guided infraclavicular blocks.
The authors declare no competing interests.
Okitolela Scotty Tambwe: Regional block procedure, data collection, manuscript and case report writings. Blaise Bayingana: supervision and manuscript review. All the authors have read and aprroved the final version of this manuscript.
We would like to express our sincere gratitude to the whole Anaesthetic Nursing staff of Charlotte Maxeke Johannesburg Academic Hospital (South Africa), to the Second Year Medical Intern, Dr. Lebogang Gwangwa, on rotation in the department of anaesthesia (July 2025), for assisting with intraoperative documentations; thus, all of them helped to advance knowledge.
Figure 1: A) operator´s hands; B) ultrasound probe; C) needle insertion on the antero-medial aspect of the axillary region; D) sterile gel
Figure 2: A) needle directed towards the medial cord; B) axillary vein, C) medial cord, D) axillary artery; E) pectoralis major muscle; F) pectoralis minor muscle
Figure 3: A) needle directed towards the posterior cord; B) axillary vein; C) axillary Artery, D) posterior cord
Figure 4: A) needle directed towards the lateral cord; B) axillary vein; C) axillary artery; D) lateral cord
- Ruíz A, Sala X, Bargalló X, Hurtado P, Arguis MJ, Carrera A. The influence of arm abduction on the anatomic relations of infraclavicular brachial plexus: an ultrasound study. Anesth Analg. 2009 Jan;108(1):364-6. PubMed | Google Scholar
- Resources.wfsahq. Ultrasound-Guided Infraclavicular Brachial Plexus Block. Accessed on Feb 3,2026.
- Aytuluk HG, Colak T. The need for supplemental blocks in single versus triple injections in infraclavicular brachial plexus blocks with a medial approach: a clinical and anatomic study. Braz J Anesthesiol. 2020 Jan-Feb;70(1):28-35. PubMed | Google Scholar
- Mian A, Chaudhry I, Huang R, Rizk E, Tubbs RS, Loukas M. Brachial plexus anaesthesia: a review of the relevant anatomy, complications, and anatomical variations. Clinical Anatomy. 2014 Mar; 27(2):210-21. PubMed | Google Scholar